Drainless lipo-abdominoplasty is a modern abdominoplasty technique that does not require surgical drains. This technique combines liposuction and abdominoplasty to achieve impeccable results. Lipo-abdominoplasty reduces or eliminates the need for drains by employing liposuction to dissect tissues which minimises seroma formation.
In my 15 years of service, many of my tummy tuck patients would have chosen a drainless abdominoplasty over an abdominoplasty with drains if given a choice. Abdominoplasty is the most sought-after cosmetic surgery in Australia, and with the increased demand, specialist surgeons like myself have developed alternative, more efficient operation techniques like drainless lipo-abdominoplasty.

Book your appointment online now
This modern approach combines the benefits of liposuction and tummy tuck surgery to remove excess fat and tighten the abdominal muscles without the need for surgical drains. It is important to note that this operation technique is not suitable for all patients. Patients who have undergone significant weight loss may not be suitable candidates due to excessive loose skin. Post-pregnancy patients with a moderate amount of subcutaneous fat, with or without muscle separation, are usually the best candidates for this surgery.
What Is an Abdominoplasty (Tummy Tuck) Drain?
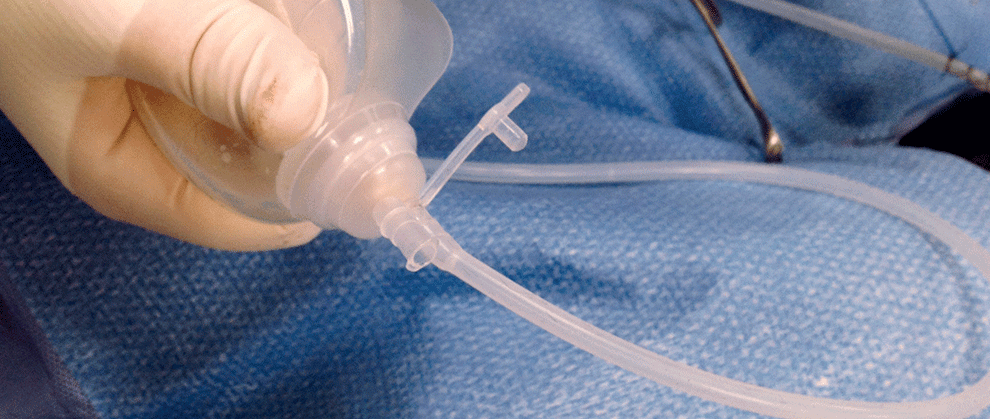
According to a study published by National Library of Medicine, “[s]uction drains are appliances used to collect blood, pus, or body fluids. They are active drains that maintain a negative pressure gradient. The collection reservoir of an active drain collects fluid by exchanging negative pressure, and the drain may become ineffective if the vacuum is lost.”
During an abdominoplasty surgery, I dissect abdominal tissues, leaving spaces that could easily fill up with bodily fluid. To control fluid buildup, I make small incision cuts close to the surgical site and insert small drainage tubes, which I connect to drainage bags. Most patients prefer abdominoplasty without the use of drains due to their discomfort and inconvenience.
When Drains Are Used for an Abdominoplasty
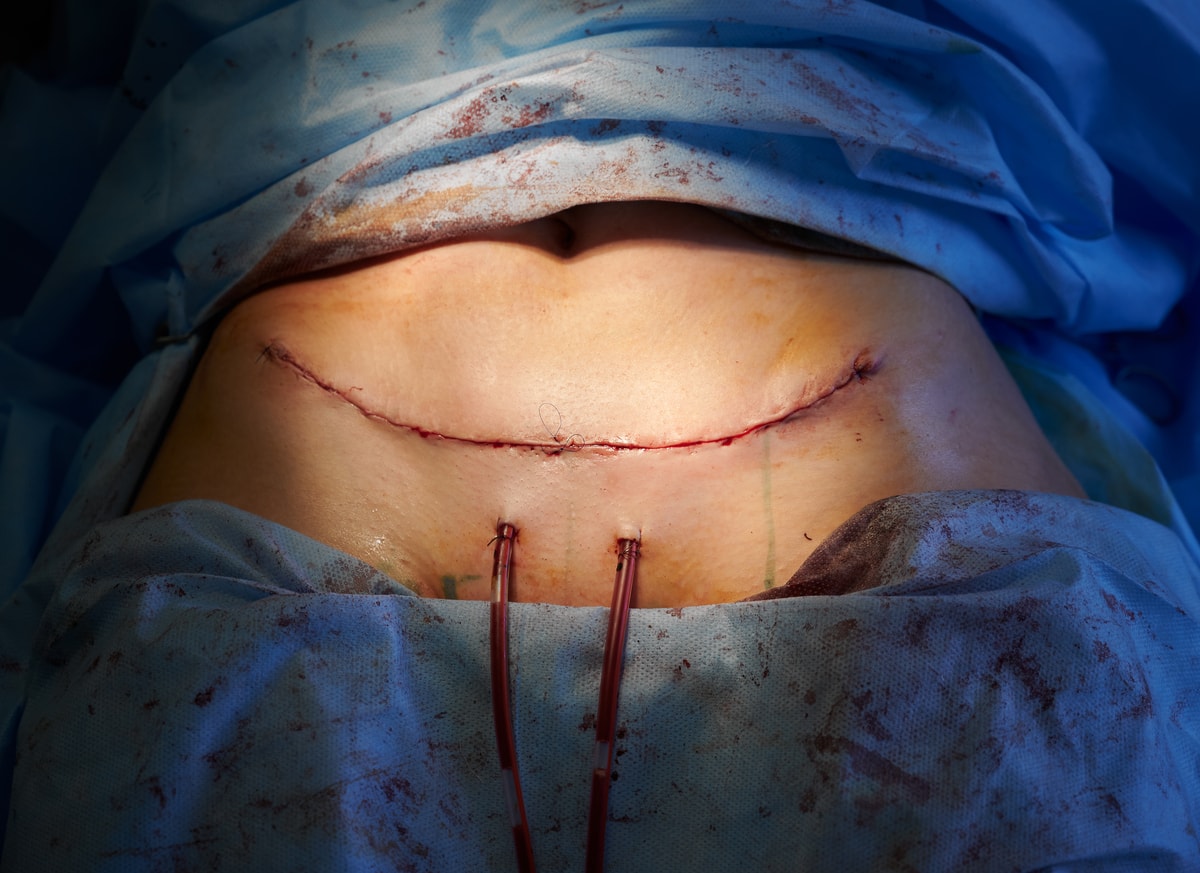
I use drains for major surgeries where the risk of fluid buildup is high due to the extent of tissue manipulation. Here are two scenarios when I use drains after a tummy tuck:
FDL Surgery
Fleur-de-Lis is an invasive tummy tuck surgery that requires both vertical and horizontal incisions to remove the excess skin. Since it targets a large abdomen area, extensive tissue manipulation increases the risk of seroma formation. I will therefore use drains to monitor and manage any fluid accumulation which can cause swelling, discomfort, and increase the risk of infection.
Extended Abdominoplasty
Extended abdominoplasty targets loose skin on your abdomen, flanks, and lower back. The large amounts of skin resection cause fluid buildup, so I insert drains near your incision site to manage the fluid accumulation.
When Are Drains Not Used?
Post-pregnancy
I will not normally use drains for post-pregnancy patients and for less extensive surgeries like mini or standard abdominoplasty, as these procedures are less likely to cause fluid buildup.
Mini Tummy Tuck
Additionally, I do not use drains for less complex procedures like mini abdominoplasty.
Download our short guide: “11 Important abdominoplasty techniques that you need to know about”
Why Drains Are Falling Out of Favour
- There is little to no evidence that drains lower the chance of seroma development.
- Drains are cumbersome, interfering with normal activities such as showering and sleeping **.
- Patients tend to experience longer hospital stays.
- There is an increased risk of infection.
- Drains increase the risk of pain, irritation, swelling, and discomfort and extend the recovery period.

The “Drainless” VASER Lipo-Abdominoplasty Method
The “drainless” method offers a modern alternative to traditional tummy tuck surgeries, focusing on a less invasive approach while achieving similar aesthetic results. This procedure involves a combination of VASER liposuction, removal of excess skin, and repair of diastasis recti.
VASER liposuction uses ultrasound energy to break apart fat cells and loosen them from the surrounding tissue, allowing for a more precise and controlled removal of fat deposits. This helps to better target abdominal contours, minimise the amount of surgical intervention, reduce the need for extensive dissection, reduce the risk of complications, and promote a smooth recovery.
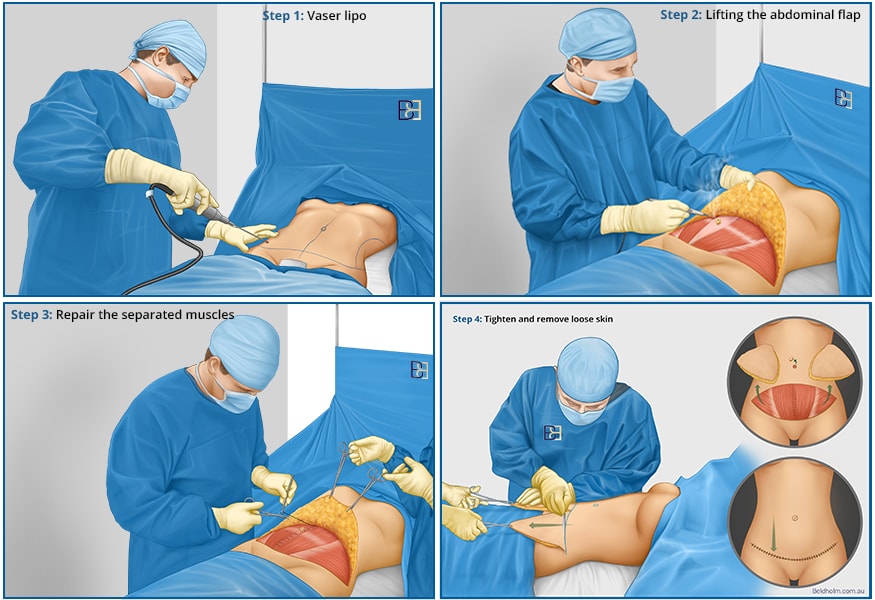
Benefits of This Method
Various benefits make the drainless method popular among post pregnancy patients, including:
- Drainless. Drains are often used in traditional abdominoplasty procedures to remove excess fluid and blood, but they can be ** for the patient and increase the risk of infection. The body is able to naturally reabsorb the excess fluid, reducing the need for drains and ** the overall patient experience.
- **. Drains cause discomfort and irritation. The use of tumescent fluid and the ** suction technique helps reduce discomfort and reduce swelling during the tummy tuck procedure.
- Pain relief. Additionally, the anaesthetic properties of tumescent fluid provide pain relief for the first day of recovery, making the initial stage of healing more ** for you.
- Easier recovery. Traditional tummy tuck surgeries that involve the use of drains require consistent care and monitoring. However, the drainless method ** the recovery process.
Drainless VASER Lipo-Abdominoplasty
Below is an overview of the steps I follow during drainless VASER lipo-abdominoplasty, a modern method for eliminating drains for lipo-abdominoplasty:
Preoperative Prep
Upon arrival at the hospital, I will ** your last-minute concerns in the anaesthesia bay. I will then make incisional markings on your body while you’re still standing. I recommend wearing your preferred choice of underwear or swimsuit bottoms to help guide me as I create your incisional markings so I can best disguise your scars.

The anaesthetist will greet you and give you premedications. Once in the operation room, they will administer general anaesthesia until you are fully asleep.
Liposuction
The initial step in the surgical procedure is to perform liposuction. First, access holes will be made in your abdomen, and a wetting solution will be injected to aid in the ** removal of fat and provide pain relief for 12 hours after the abdominoplasty. The wetting solution contains a local anesthetic and adrenaline. Next, the VASER probe will break down the fat cells, followed by the liposuction cannula removing the liquefied fat.

Lower abdominal incision and elevation of the skin
During the next step, I will make an incision in the lower abdomen as well as around the umbilicus. Then, I will separate the skin from the underlying tissue.
Repair Diastasis Recti
The rectus abdominis muscles, which provide core strength, tend to separate during pregnancy or from massive weight loss, causing a belly bulge. To repair diastasis recti during a tummy tuck surgery, I bring the ab muscles together using barbed permanent sutures.
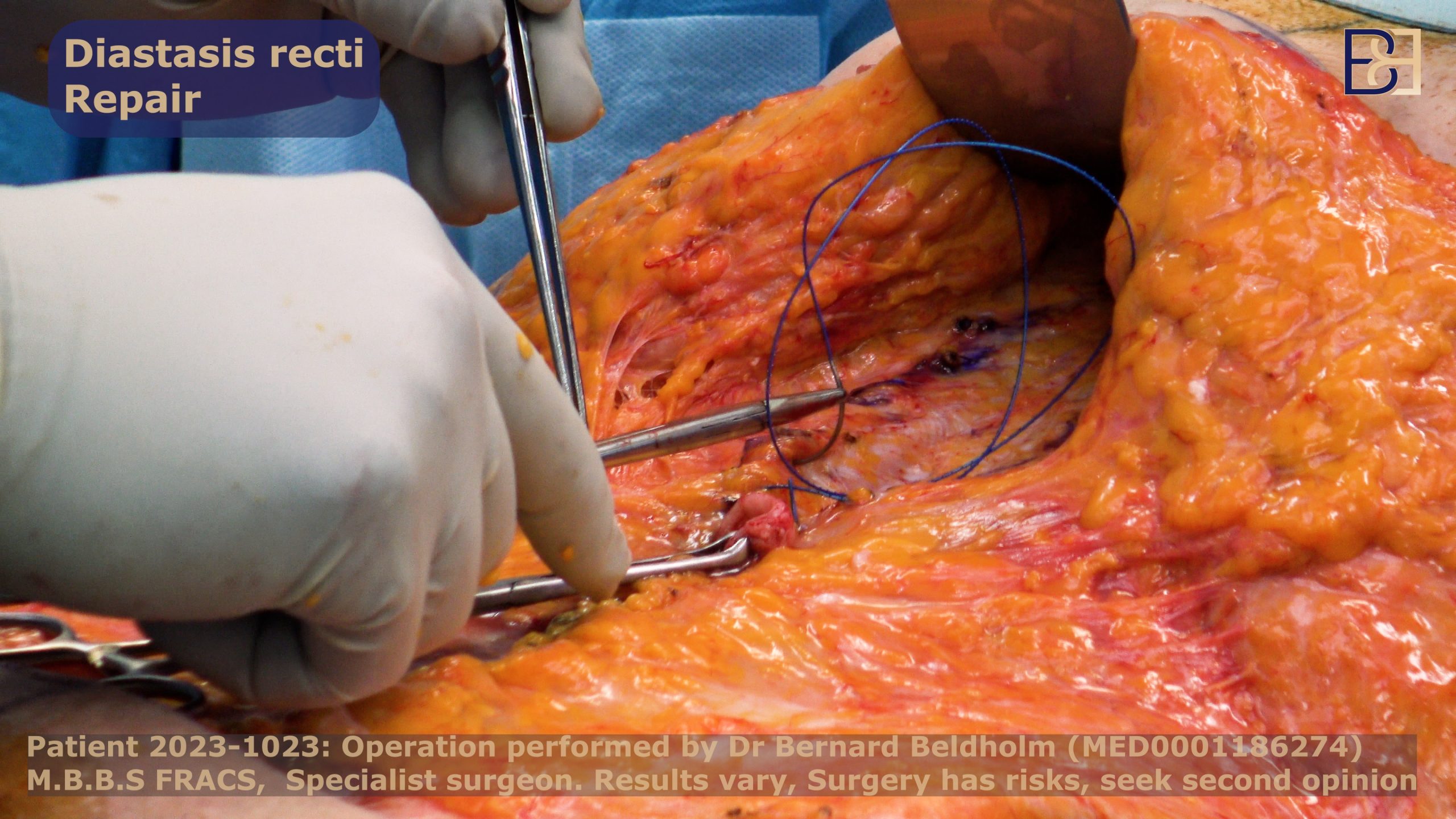
Removing excess skin in abdominoplasty
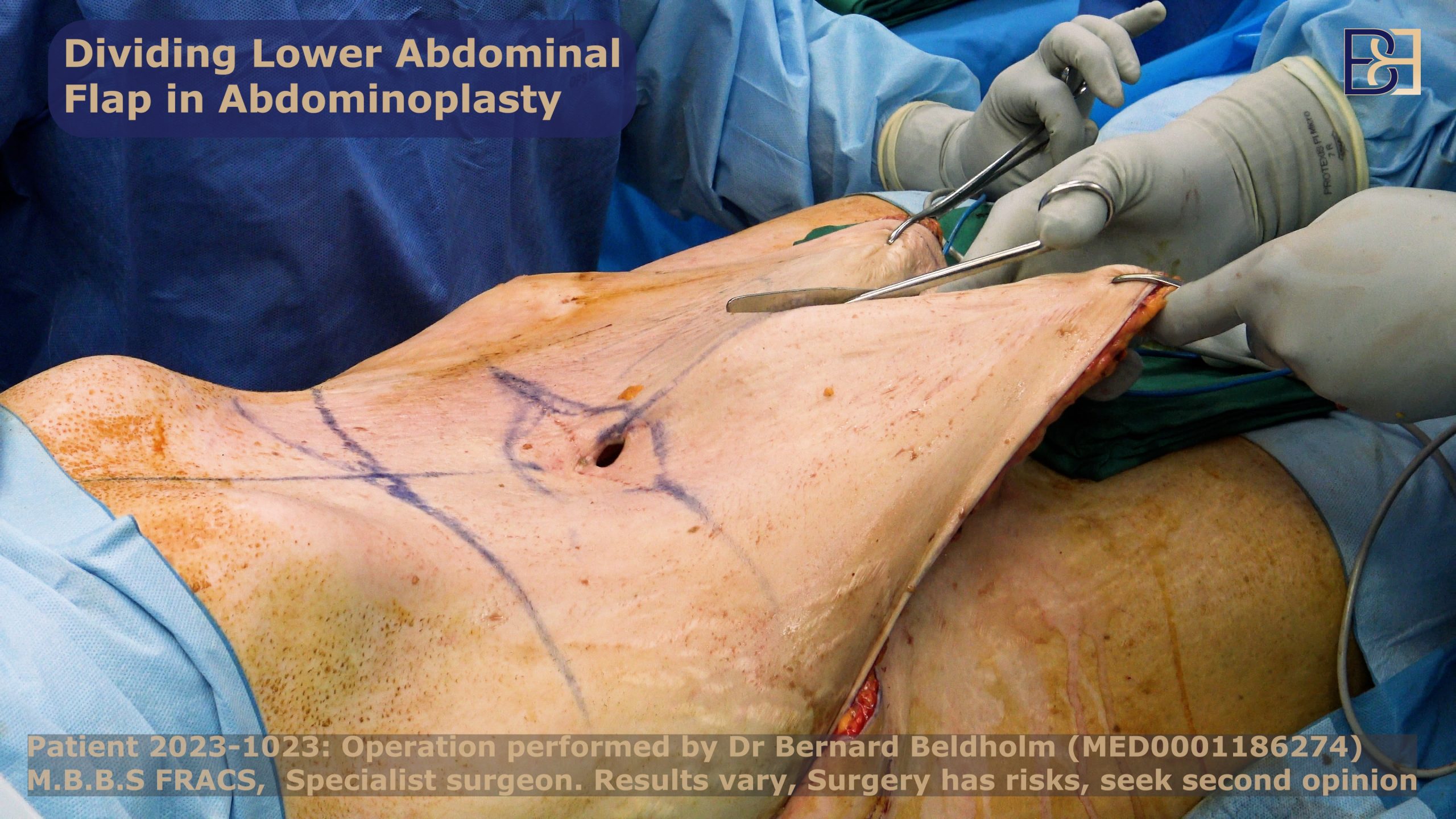
After I tighten your abdominal muscles, a substantial amount of loose skin will be left hanging. During the last dissection, I will adjust the operating table to bend slightly so that I can close your skin under ** tension. As I progressively close the lower abdominal area I use plication sutures as well as tissue glue to eliminate any dead space. This helps minimise the chance of a seroma.
Reposition Belly Button
The umbilical position is marked. The skin is then incised, and the umbilical stalk is pulled through.
Remove Lower Abdominal Skin
After repositioning the belly button, I will remove the excess skin.
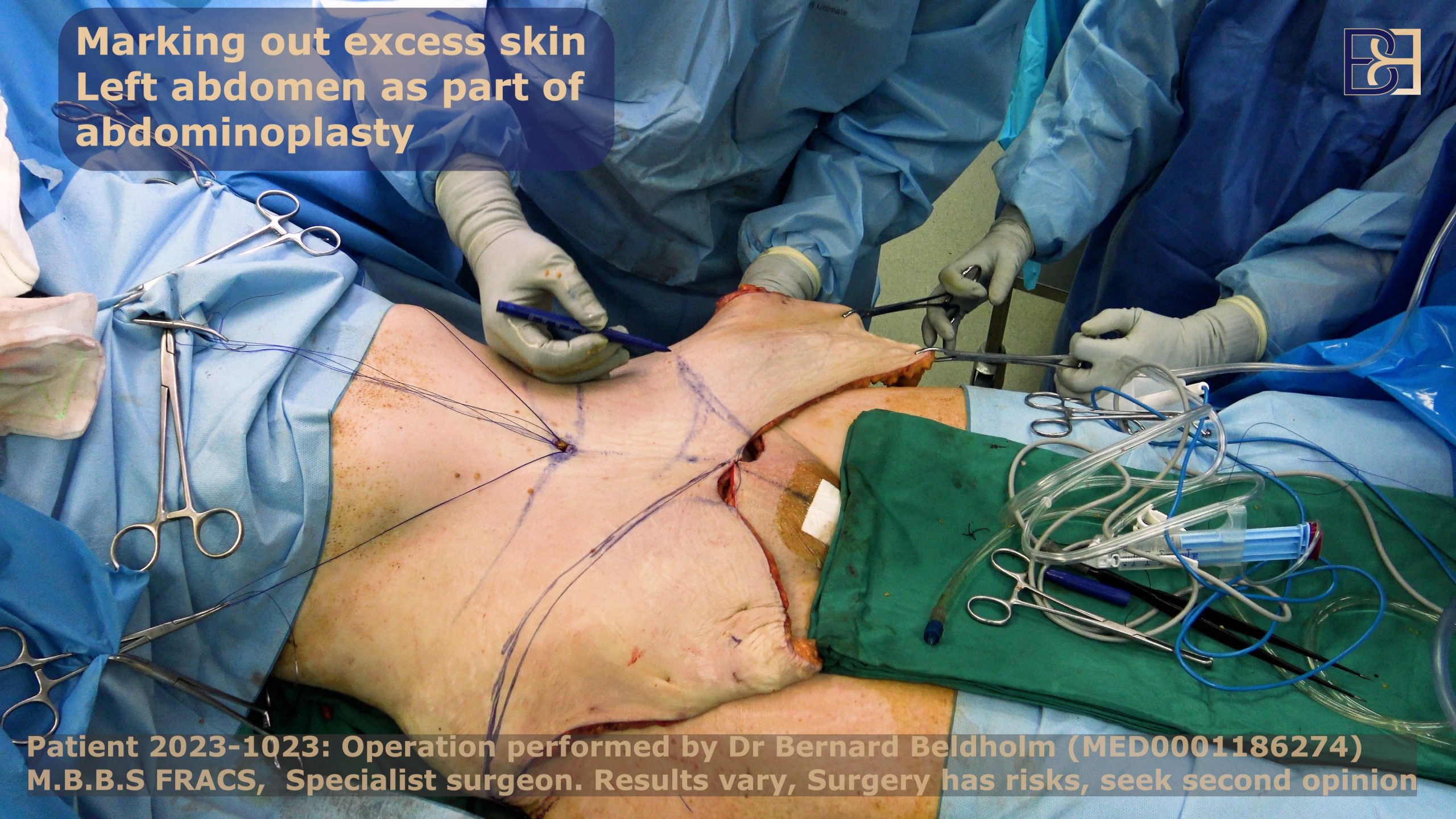
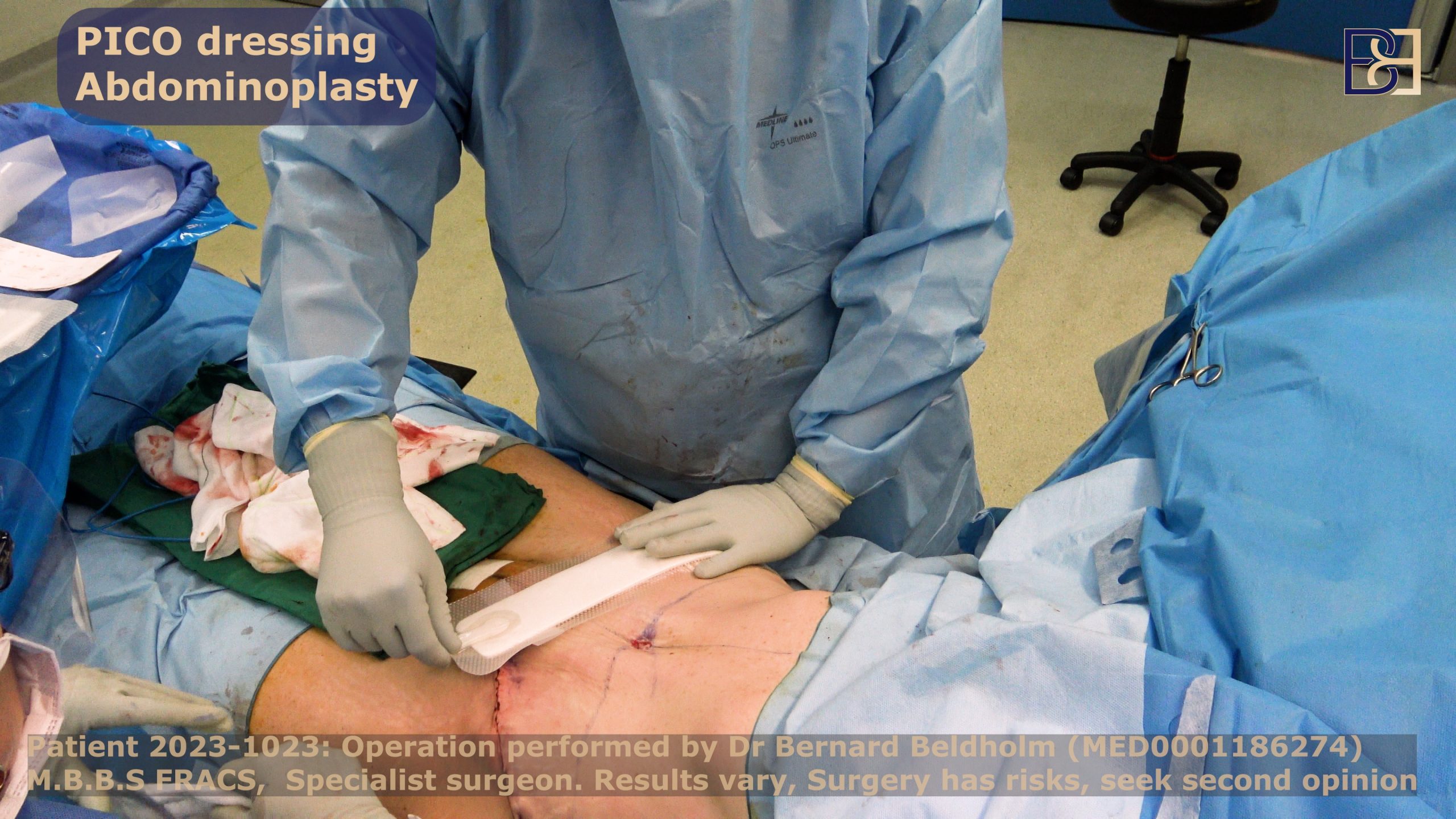
Finalising the Surgery
Lastly, I will use absorbable sutures to close the skin, which can withstand significant tension while ** aesthetic outcomes. PICO dressings are also applied.
Surgical Drains Overview

Surgical drains, which are small tubes placed in your body to remove the excess lymphatic fluid and blood, are used to reduce the risk of seroma formation and promote healing. If I do use tummy tuck drains, the following tips will ensure a smooth recovery.
- After Care: After your lipo-abdominoplasty surgery, I will give you guidelines on how to change your drains, record the drain amount and colour, and take careful showers or sponge baths. It is important to monitor how much fluid collection you get a day. The tummy tuck drain collected in the bags is an indicator of your progression, you must take care of your drainage site and the post-surgical drain belts to prevent infection and promote healing.
- Drain Removal: I will assess when it is time to remove your drain tube by considering the amount of drainage and your recovery progress.
NOTE: Do not attempt to remove the tummy tuck drains yourself. Only me or my nurse should do so.
Dr. Beldholm’s Method for Eliminating Drains
During lipo-abdominoplasty surgery, I use the following techniques to reduce the need for post-surgical drains:
Use of Liposuction to Limit Dissection
By targeting specific areas with excess fat, liposuction reduces the need for extensive tissue dissection. My preferred technique for “discontinuous” dissection is to use VASER liposuction. This preserves blood flow and minimizes the “dead space” that occurs with extensive elevation of the abdominal flap. Seromas do happen; however, the rate is similar or lower compared to using drains.
Current literature by NCBI suggests that “[i]n a vast majority of patients undergoing abdominoplasty with liposuction, insertion of drains is unnecessary. Avoidance of tummy tuck drains was not found to be associated with seroma formation or wound-related complications.”
Progressive Tension Sutures
I use progressive sutures after surgery to ensure that the wound is closed evenly and minimise the risk of the wound reopening. Progressive sutures secure the repaired tissues and reduce the likelihood of seroma formation. These sutures are efficient because they are absorbable, meaning they break down in the body over time.
Recovery Process
The recovery process for every patient is different. After your surgery, it is up to you to ensure that you take care of your incision or drain sites to avoid delayed healing.
- Showering with drains: If I place drains in your incisional site, you will only be able to have limited showers until I remove the tummy tuck drains. You should always pat the incision site dry to avoid causing friction and irritating your skin, which could cause infection. Please follow my guidelines on how and when to shower ** for optimal healing.
- Back to Work: How soon you return to work depends on the physical demands of your job and your healing progress. Ideally, on average, it takes 2 to 6 weeks before it’s ** to return to work. This will depend on a number of factors including, wound healing rate, type of surgical procedure, nature of work among others.
For a mini abdominoplasty, patients can typically return to most normal activities within 2 weeks after surgery. For full tummy tucks, you’ll need at least 2 weeks to return to sedentary jobs. Extended and Fleur-de-lis abdominoplasties have a slightly longer recovery, with most of my patients returning to work in 3 weeks. The most extensive procedure, a belt lipectomy, has a 4-week recovery timeline. It’s important to note that revision abdominoplasty surgeries often take longer than initial procedures, as the previous scar tissue can be more painful and require additional healing time.
To learn more about abdominoplasty recovery timelines, check out my article, Dr. Beldholm Gets Down to Business: Comprehensive Guide for Returning to Work After Abdominoplasty Surgery.
- Exercise: You should always start slowly and build up your resistance. Exercise is a crucial part of the recovery journey since it promotes blood circulation, speeding up the recovery. If you remain immobile after your lipo-abdominoplasty surgery, you risk the formation of blood clots.
- Sleeping: Avoid sleeping on your stomach or surgical site because it may slow healing. Most patients find it ** to sleep at an elevated angle with the support of pillows since it alleviates swelling.
- Compression Garments: Compression garments will be essential in your post-surgical journey. They provide support and **, reduce swelling, and ** blood circulation. I will explain how long you should wear these garments for optimal results.
Are Drains Painful?
Most patients complain they are ** since drains pull around the insertion site. If possible I opt for the drainless lipo-abdominoplasty surgery, which does not require drains to make the post-abdominoplasty journey ** and easier to manage.
Risks Of Drainless Tummy Tuck
Drainless lipo-abdominoplasty has risks and complications similar to other abdominoplasty techniques. The following are some common risks:
- Infection: If you do not handle the incisional site properly, your wound is at risk of developing infection, which may cause skin or tissue necrosis.
- Scarring: The incision I make during surgery matures to form a scar. I always place the scar where it will be inconspicuous, but the final scar visibility depends on your healing process and how well you care for your wound.
- Delayed healing: When you do strenuous activities before your incision site is properly healed, you risk reopening your wound, which could require a corrective procedure. Underlying health issues could also delay your healing process.

Dr. Beldolm’s Final Thoughts: ** Patient Outcomes
Abdominoplasty has evolved to provide better aesthetic results and an easier post-abdominoplasty journey. By using the drainless lipo-abdominoplasty technique, I can reduce post-operative complications such as seromas. There are many ways of performing an abdominoplasty surgery, but this one has continuously proven its effectiveness by limiting tissue dissection, preserving blood flow, and enabling a smooth recovery for my patients. As your specialist general surgeon in Australia, I aim to bring your abdominoplasty goals to life while prioritising your health and **.
There is so much to discuss before you plan your surgery, so I invite you to book a consultation with me so that I can enlighten you further.
Book your appointment online now
References
- Ramesh, B. A., Evans, J. T., & BK, J. (2023). Suction Drains. In StatPearls. StatPearls Publishing.
- Durai, R., Mownah, A., & Ng, P. C. (2009). Use of tummy tuck drains in surgery: a review. Journal of perioperative practice, 19(6), 180–186.
- Isaac, K. V., Lista, F., McIsaac, M. P., & Ahmad, J. (2017). Drainless abdominoplasty using barbed progressive tension sutures. Aesthetic Surgery Journal, 37(4), 428–429.
- Ramesh, B. A., Evans, J. T., & BK, J. (2023). Suction Drains. In StatPearls. StatPearls Publishing.
- Shauly, O., Goel, P., & Gould, D. J. (2022). Painless, Drainless Lipoabdominoplasty: A Retrospective Study of Pain Following Lipoabdominoplasty Utilising Liposomal Bupivacaine and a Modified Enhanced Recovery After Surgery Protocol. Aesthetic Surgery Journal. Open Forum, 4.
- Brauman, D., van der Hulst, R. R. W. J., & van der Lei, B. (2018). Liposuction Assisted Abdominoplasty: An Enhanced Abdominoplasty Technique. Plastic and reconstructive surgery. Global open, 6(9), e1940.
- Xia, Y., Zhao, J., & Cao, D. S. (2019). Safety of Lipoabdominoplasty Versus Abdominoplasty: A Systematic Review and Meta-analysis. Aesthetic plastic surgery, 43(1), 167–174.
- Pollock, T., & Pollock, H. (2004). Progressive tension sutures in abdominoplasty. Clinics in plastic surgery, 31(4), 583–vi.
- Valença-Filipe, R., Martins, A., Silva, Á., Vásconez, L. O., Amarante, J., & Costa-Ferreira, A. (2014). Dissection Technique for Abdominoplasty: A Prospective Study on Scalpel versus Diathermocoagulation (Coagulation Mode). Plastic and Reconstructive Surgery Global Open, 3(1).
- Patronella C. K. (2022). Progressive Tension Sutures Eliminate the Need for Drains in Body Contouring Surgery. Aesthetic surgery journal, 42(3), NP191–NP192.
- Khan, F. A. A., & Fatima, M. (2021). Abdominoplasty without Drains or Progressive Tension Suturing. Aesthetic plastic surgery, 45(4), 1660–1666.





