Brachioplasty, also known as arm lift surgery or brachioplasty arm lift surgery, is a surgical procedure designed to remove excess skin and, in some cases, excess fat from the upper arms. This type of surgery is most commonly performed after significant weight loss, including after bariatric surgery, after pregnancy, or due to age-related changes in skin elasticity.
Although brachioplasty surgery is effective at reducing excess skin, it is a major surgical procedure and therefore carries risks. Understanding the full range of complications from brachioplasty is essential for patients considering an arm lift (brachioplasty). Complications may range from minor issues, such as delayed healing, to more serious medical complications that require medical intervention or revision surgery.
This article provides an in-depth, evidence-based discussion of brachioplasty complications, including their incidence, mechanisms, and management. It is intended to support informed decision-making and help patients develop realistic expectations about arm lift (brachioplasty) surgery and the recovery process.
Overview of Complication Rates in Brachioplasty (Arm Lift) Surgery
Brachioplasty (arm lift) surgery is associated with higher reported complication rates than many smaller cosmetic procedures. This largely depends on the length of the incision, the amount of excess skin and fat removed, and the involvement of underlying tissues, such as lymphatic channels and superficial nerves.
Across multiple studies, the overall complication rate for arm lift (brachioplasty) surgery ranges from 20–40%, with most complications classified as minor and resolving with appropriate postoperative care instructions [1–3]. Patients undergoing brachioplasty after significant weight loss or bariatric surgery consistently demonstrate a higher risk of complications compared with patients undergoing arm lift (brachioplasty) surgery for mild skin laxity alone [1,2].
Importantly, major complications such as blood clots, deep vein thrombosis, lung complications, or the need for blood transfusion are rare when brachioplasty surgery is performed by an experienced specialist surgeon with appropriate patient selection and preventive measures in place.
Early Post‑Operative Complications
Bleeding and Haematoma
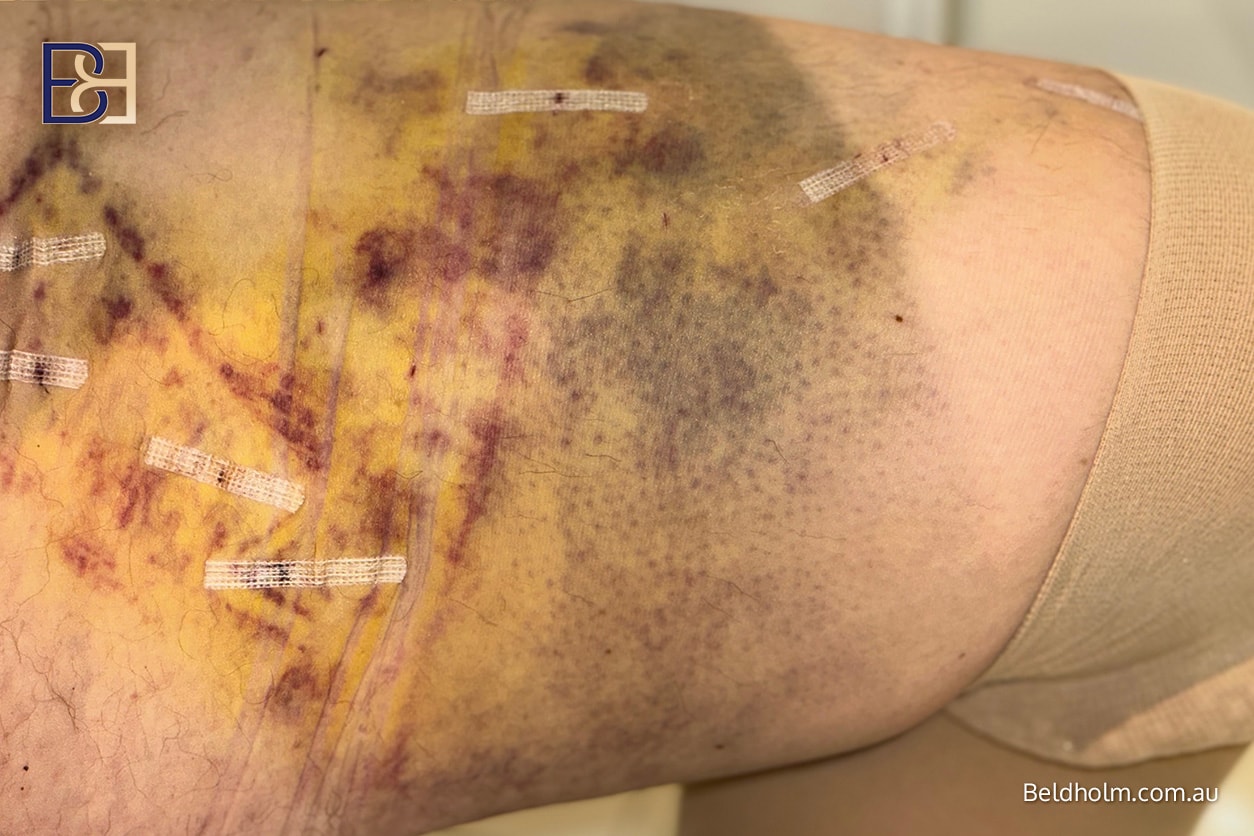
Incidence: approximately 1–5% [1,4]
Bleeding following brachioplasty may occur in the immediate post‑operative period or within the first 24–48 hours. When blood collects beneath the skin, it forms a haematoma, which can place pressure on surrounding tissues and compromise wound healing.
Risk factors include elevated blood pressure, early excessive arm movement, anticoagulant medications, and combined procedures that prolong operative time.
Small haematomas may resolve with observation and compression. Larger or expanding haematomas typically require surgical evacuation to reduce the risk of infection and wound breakdown.
Infection
Incidence: approximately 2–4% [1,3,5]
Surgical site infection after brachioplasty is uncommon but clinically significant when it occurs. Most infections are superficial and present within the first two weeks after surgery.
Patients may notice increasing redness, warmth, pain, or discharge from the incision, sometimes accompanied by fever. Risk factors include smoking, diabetes, obesity, prolonged operative time, and wound tension, particularly in the axillary region.
Treatment usually involves oral antibiotics and local wound care. Deeper infections may require intravenous antibiotics or surgical drainage. Early intervention is critical to prevent delayed healing and poor scar outcomes.
Wound Breakdown, Poor Wound Healing, and Delayed Healing
Incidence: approximately 10–25%, higher in patients after significant weight loss [1,2]
Poor and delayed wound healing are among the most frequently reported complications of brachioplasty (arm lift). These issues are most commonly seen near the axilla, where tension, moisture, and arm movement place stress on the incision site.
Risk factors include smoking, impaired skin elasticity, diabetes, nutritional deficiencies, and excessive early arm movement or heavy lifting. Poor wound healing may present as scabbing, wound separation, or slow closure of the incision.
Most cases are managed conservatively with wound care, dressings, and activity modification. While frustrating, these minor complications usually resolve without the need for revision surgery.
Seroma and Fluid Accumulation
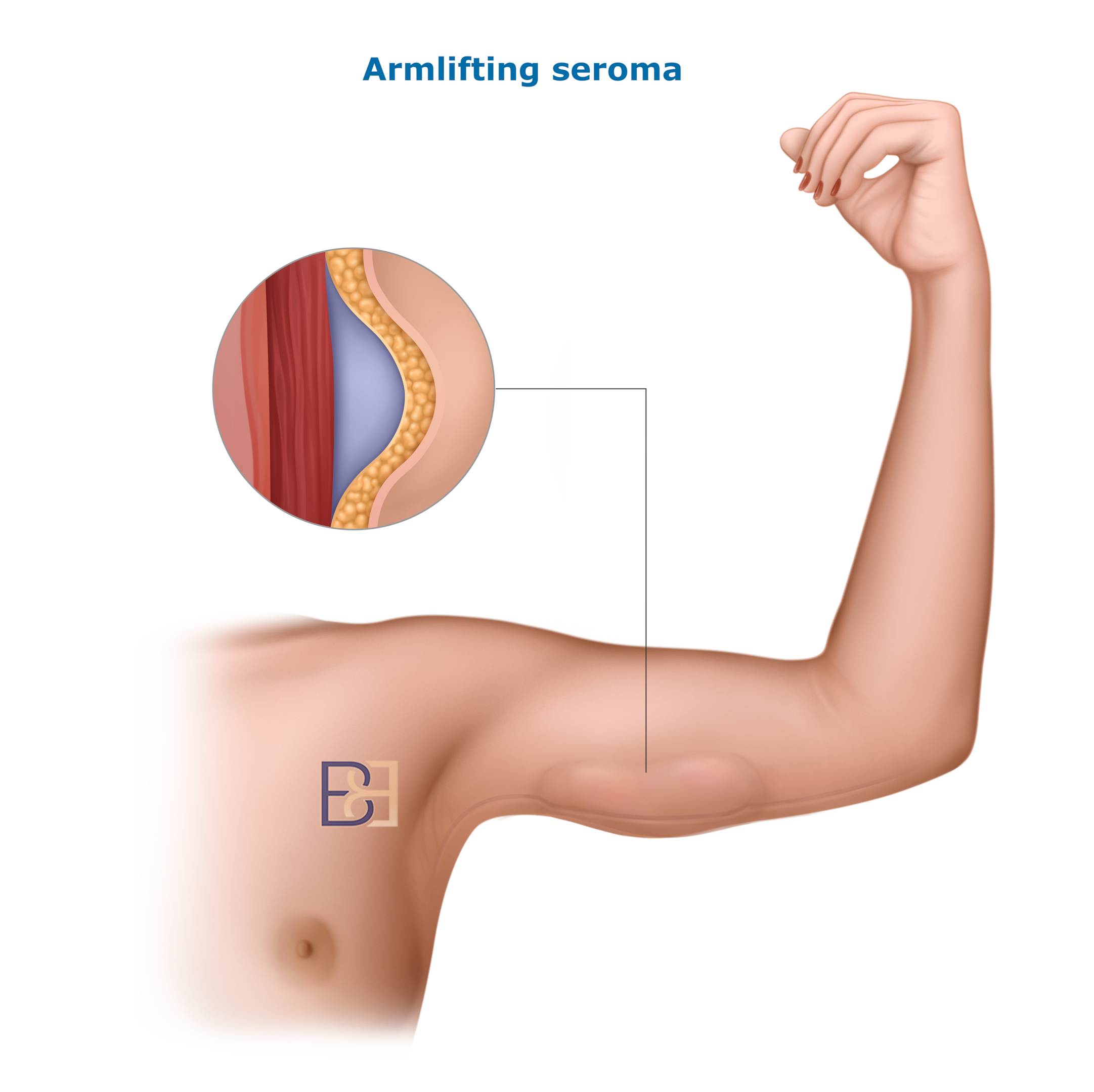
Incidence: approximately 5–15% [1,3,6]
A seroma is a fluid accumulation beneath the skin at the surgical site and is a common complication of brachioplasty (arm lift) surgery. Fluid accumulation occurs due to the disruption of lymphatic channels and the creation of a potential space after excess skin and fat are removed.
Patients may notice swelling, a soft or fluctuant area, or asymmetry between the upper arms. Seromas may develop during the early recovery period or several weeks after surgery, even in patients who wear compression garments as instructed.
Management usually involves drainage procedures, most commonly needle aspiration performed in the clinic. Some patients require repeated aspirations. Persistent seromas may require prolonged compression garments or, rarely, further medical intervention.
Book your appointment online now
Sensory and Nerve‑Related Complications

Temporary Sensory Changes
Incidence: reported in up to 70% of patients early post‑operatively [2,4]
Temporary numbness, tingling, or altered sensation along the inner or posterior arm is expected after brachioplasty. This occurs due to stretching or division of small cutaneous nerves during skin excision.
In most patients, sensation gradually returns over several months as nerve fibres regenerate. This process can take 6–12 months or longer.
Persistent Sensory Loss and Nerve Damage
Incidence: approximately 5–10% [1,2]
Nerve damage resulting in long-term sensory change is an acknowledged risk of brachioplasty surgery. The medial antebrachial cutaneous nerve is the most commonly affected nerve, as it supplies skin sensation to the inner arm and lies close to typical brachioplasty incisions.
Patients may experience persistent numbness, altered skin sensation, or reduced sensitivity along the inner arm. While this rarely affects arm function, it can be noticeable.
There is no reliable surgical correction for permanent sensory loss. Management focuses on reassurance, education, and setting realistic expectations regarding surgical outcomes.
Neuropathic Pain and Neuroma Formation
Incidence: less than 2% [2,6]
Rarely, injured nerves may form neuromas, leading to localised burning or shooting pain. Symptoms are often triggered by touch or pressure.
Management may include neuropathic pain medication, local steroid injections, or surgical excision in selected cases. Fortunately, this complication is uncommon.
Lymphatic Complications
Prolonged Arm Swelling
Incidence: approximately 5–10% [1,3]
Persistent swelling beyond the expected recovery period reflects temporary lymphatic disruption. It typically returns gradually with time, compression garments, and arm elevation.
Lymphoedema
Incidence: less than 1% [1,6]
True chronic lymphoedema following brachioplasty is rare but recognised. It presents as persistent, non‑resolving swelling and heaviness of the arm.
Management involves long‑term compression therapy and referral to a lymphoedema specialist. Prevention through meticulous surgical technique is critical.
Scarring‑Related Complications
Widened or Prominent Scars
Incidence: approximately 10–30% [1,2]
Scarring after brachioplasty is inevitable due to the length of the incision. Some patients develop widened or more visible scars due to skin quality, tension, or individual healing tendencies.
The appearance of scars typically continues to change for 12–18 months.
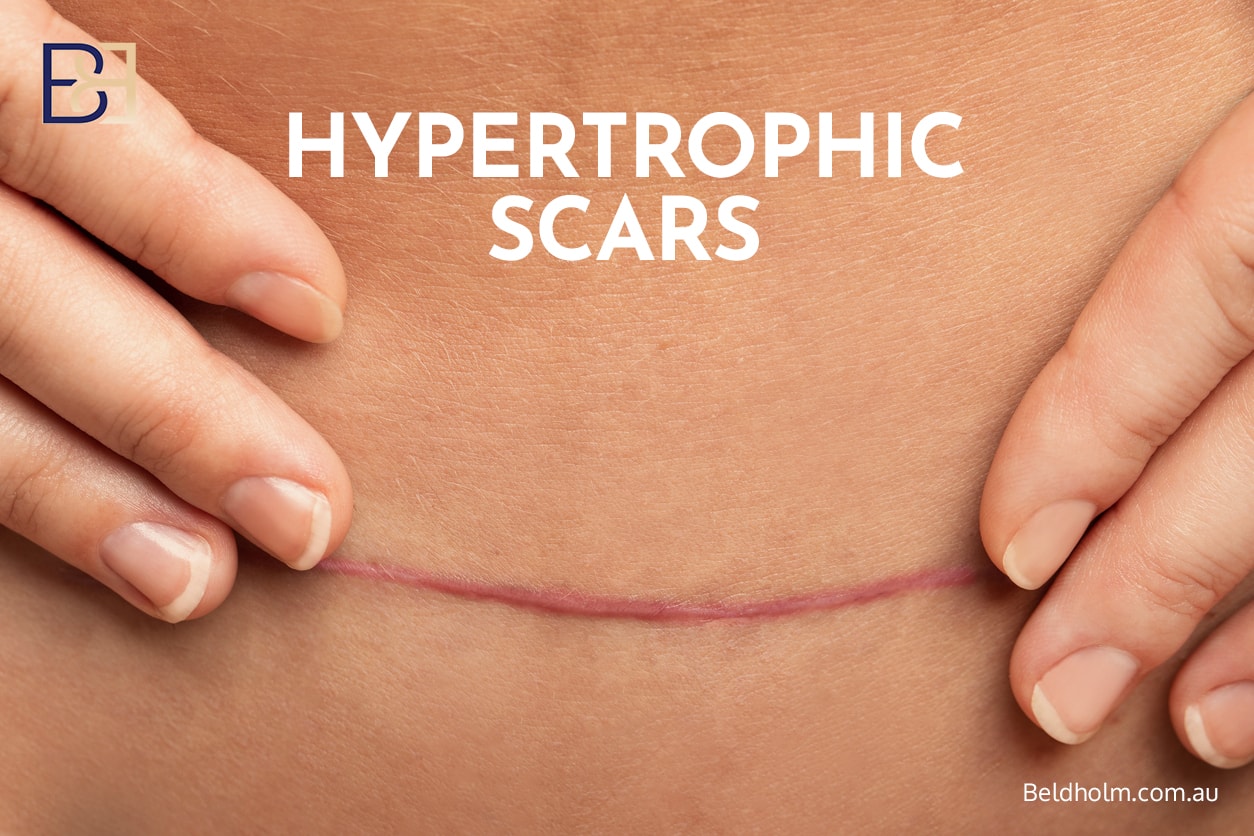
Hypertrophic Scarring
Incidence: approximately 5–15% [3,5]
Hypertrophic scars are raised and firm but remain within the incision borders. They are more common in areas of high tension.
Management includes silicone therapy, steroid injections, and sometimes laser treatment.
Keloid Scarring
Incidence: less than 5%, higher in genetically predisposed individuals [5]
Keloid scars extend beyond the original incision and can be symptomatic. Patients with a known history of keloids should be counselled carefully before surgery.
Aesthetic and Functional Complications
Residual Excess Skin or Recurrent Laxity
Incidence: approximately 10–20% in massive weight loss patients [1,2]
Residual or recurrent loose skin may occur due to conservative resection or poor skin elasticity. Revision surgery may be considered once healing is complete.
Asymmetry
Incidence: approximately 5–10% [3]
Minor asymmetry is common during early recovery and often resolves as swelling resolves. Persistent asymmetry may require revision surgery.
Restricted Arm or Shoulder Movement
Incidence: less than 5% [4]
Tight scars or prolonged guarding can temporarily restrict movement. Physiotherapy and gradual stretching usually treat function. Permanent restriction is rare.
General Surgical Risks
Venous Thromboembolism (DVT and Pulmonary Embolism)
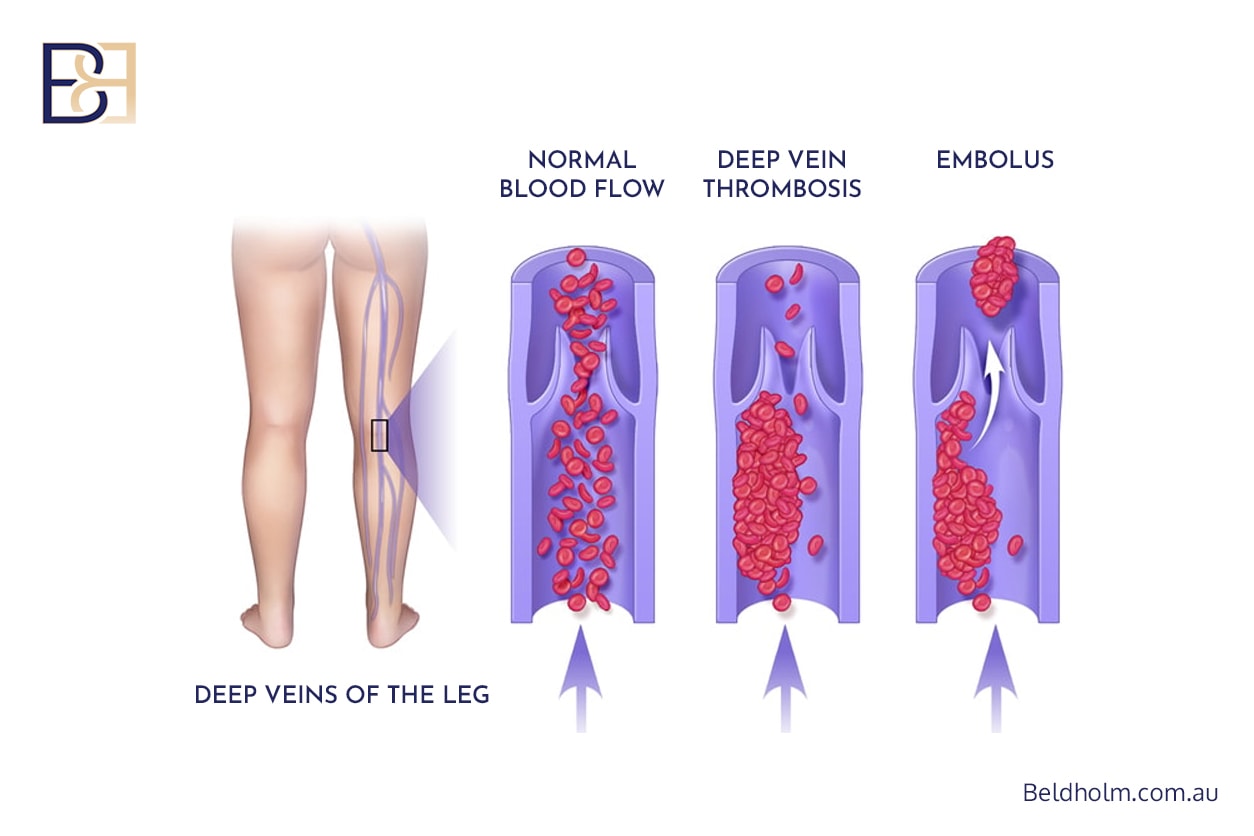
Incidence: less than 1% [4]
Although uncommon in isolated brachioplasty, the risk increases with prolonged surgery, combined procedures, obesity, and limited mobility. Early mobilisation is essential.
Anaesthetic‑Related Complications

Complications related to general anaesthesia are uncommon but include nausea, vomiting, allergic reactions, and cardiopulmonary events. These risks are assessed individually by the anaesthetic team.
Revision Surgery
Incidence: approximately 5–15% [1,2]
Revision surgery may be required to treat problematic scarring, persistent seroma, residual skin, or asymmetry. Revision is typically delayed by 6–12 months after the initial operation.
Reducing the Risk of Complications and Supporting Recovery
While brachioplasty (arm lift) surgery carries risks, several preventive measures can reduce the risk of complications and support recovery.
Key strategies include:
- Choosing an appropriately qualified specialist surgeon with experience in arm lift (brachioplasty) surgery
- Disclosing your full medical history during consultation
- Achieving and maintaining a stable weight prior to surgery
- Adopting a healthy lifestyle, including a balanced diet and adequate protein intake
- Stopping smoking and nicotine use well before surgery, as nicotine can impede healing
- Carefully following all post-operative care instructions
- Wearing and continuing to wear compression garments as advised
- Avoiding strenuous exercise and heavy lifting during the early recovery period
- Attending all scheduled follow-up appointments
These measures help reduce complications related to wound healing, fluid accumulation, and general surgical risks, thereby supporting a smoother healing process.
Frequently Asked Questions About Brachioplasty Complications

What is the most common complication of brachioplasty (arm lift) surgery?
The most common complications of brachioplasty are minor wound-healing issues, including delayed healing and small wound separations, particularly near the axilla. These are reported in up to 25% of patients, especially after significant weight loss or bariatric surgery. Most resolve with appropriate wound care and do not require further surgery.
How risky is arm lift (brachioplasty) surgery?
Arm lift (brachioplasty) surgery is considered lower risk when performed by a qualified specialist surgeon, but it does carry risks like any surgical procedure. Published studies report overall complication rates of 20–40%, with most classified as minor complications. Major complications such as blood clots, deep vein thrombosis, or lung complications are rare, occurring in less than 1% of cases.
What is the most common nerve injury in brachioplasty?
The most commonly affected nerve in brachioplasty arm lift surgery is the medial antebrachial cutaneous nerve, which supplies skin sensation to the inner arm. Injury may lead to numbness or altered skin sensation, which is usually temporary but can occasionally persist.
What unusual symptoms should prompt medical review after brachioplasty surgery?
Patients should contact their specialist surgeon promptly if they experience unusual symptoms such as increasing redness, severe pain, rapidly increasing swelling, fever, fluid accumulation, or signs of infection at the incision site. Early medical intervention improves surgical outcomes and reduces the risk of major complications.
Final Thoughts

Brachioplasty is an effective procedure for selected patients, but it carries a recognised spectrum of complications. Most complications are minor and manageable, particularly when identified early and treated appropriately. Patients considering brachioplasty should weigh these risks carefully and understand that outcomes and recovery experiences vary.
References
- Aly AS, Soliman S, Cram AE, et al. Brachioplasty in the massive weight loss patient. Clin Plast Surg. 2008;35(1):141‑147.
- Hurwitz DJ, Holland SW. The L brachioplasty: an innovative approach to excess tissue of the upper arm, axilla and lateral chest. Plast Reconstr Surg. 2006;117(2):403‑411.
- Hurwitz DJ. Brachioplasty. Clin Plast Surg. 2014;41(4):745‑751.
- Shermak MA, Chang D, Magnuson TH, et al. An outcomes analysis of patients undergoing body contouring surgery after massive weight loss. Plast Reconstr Surg. 2006;118(4):1026‑1031.
- Rubin JP, Michaels J. Correction of arm ptosis with medial bicipital scar. In: Strauch B, Herman C, eds. Encyclopedia of Body Sculpting After Massive Weight Loss. New York: Thieme; 2010.
- Aly AS. Complications of brachioplasty in the post–weight loss patient. Aesthetic Surg J. 2006;26(1):76‑84.