This article focuses exclusively on recovery after male chest surgery following significant weight loss, specifically recovering from male chest surgery post weight loss with the upper torsoplasty (upper body lift). The surgical reasons, indications, and decision-making are covered in a separate article. Here, the aim is to clearly explain how recovery varies depending on the type of surgery performed, what to expect as normal during recovery, and how to prepare effectively.
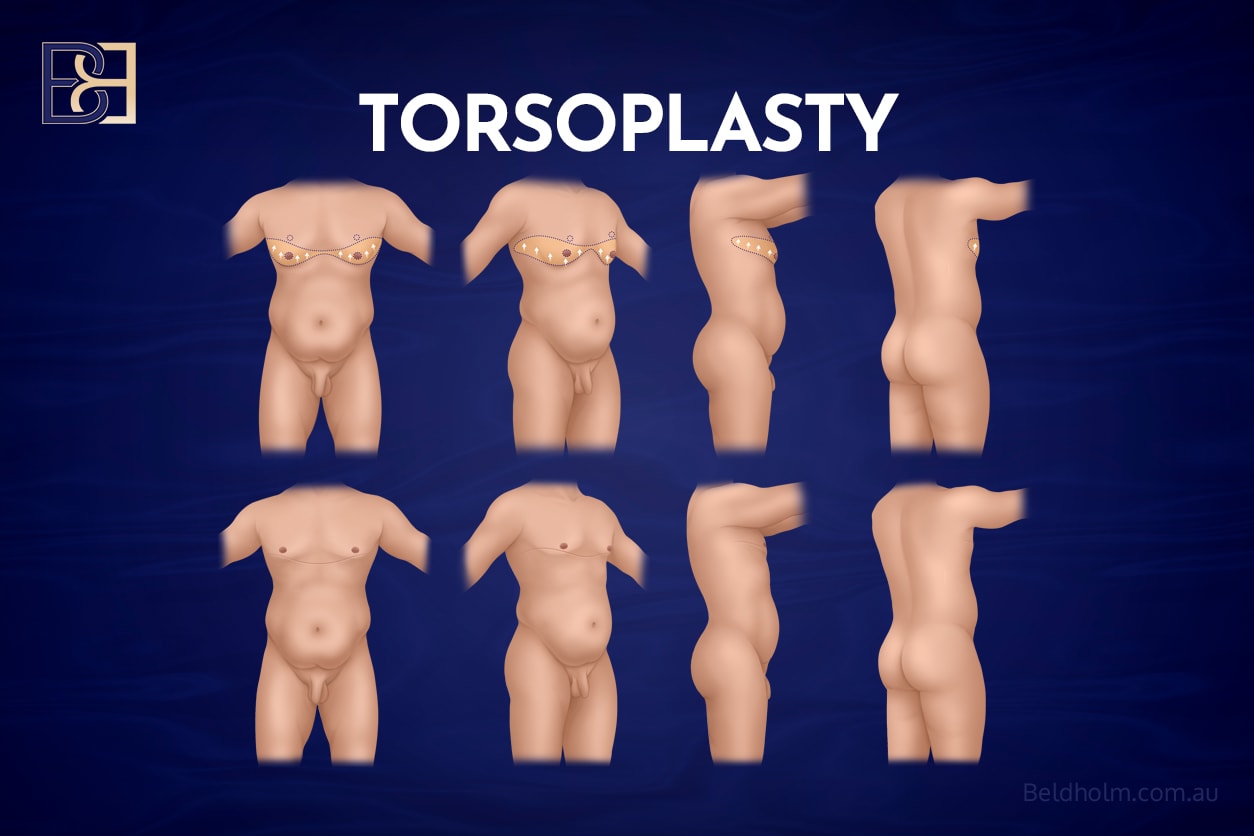
Recovery after male chest surgery post-weight loss is not one-size-fits-all. In my practice, recovery typically falls into three distinct categories, depending on the surgical approach:
- Anterior torsoplasty (upper body lift/body lift)
- Circumferential upper body lift (360° body lift, lipectomy, upper circumferential torsoplasty)
- Upper body lift (upper torsoplasty) with VASER liposuction (suction-assisted lipectomy)
Each has a different recovery profile, level of discomfort, and return-to-activity timeline.
General Principles of Recovery After Male Chest Surgery
Regardless of the surgical technique used, there are shared recovery principles across all forms of upper body lift (torsoplasty) surgery:
- Swelling and tightness are expected
- Fatigue is common during the early recovery period
- Compression garments are essential
- Recovery progresses over weeks, not days
- Follow-up appointments are critical
Patients who have experienced significant weight loss often exhibit reduced skin elasticity, areas of skin laxity, excess skin folds, and altered lymphatic drainage, which can influence healing after body contouring surgery. These factors influence the healing process and must be respected.
In addition to activity modification, dressing management and nipple–areola complex (NAC) care are key components of recovery and require careful attention.
Dressing Management After Upper Body Lift (Torsoplasty) Surgery
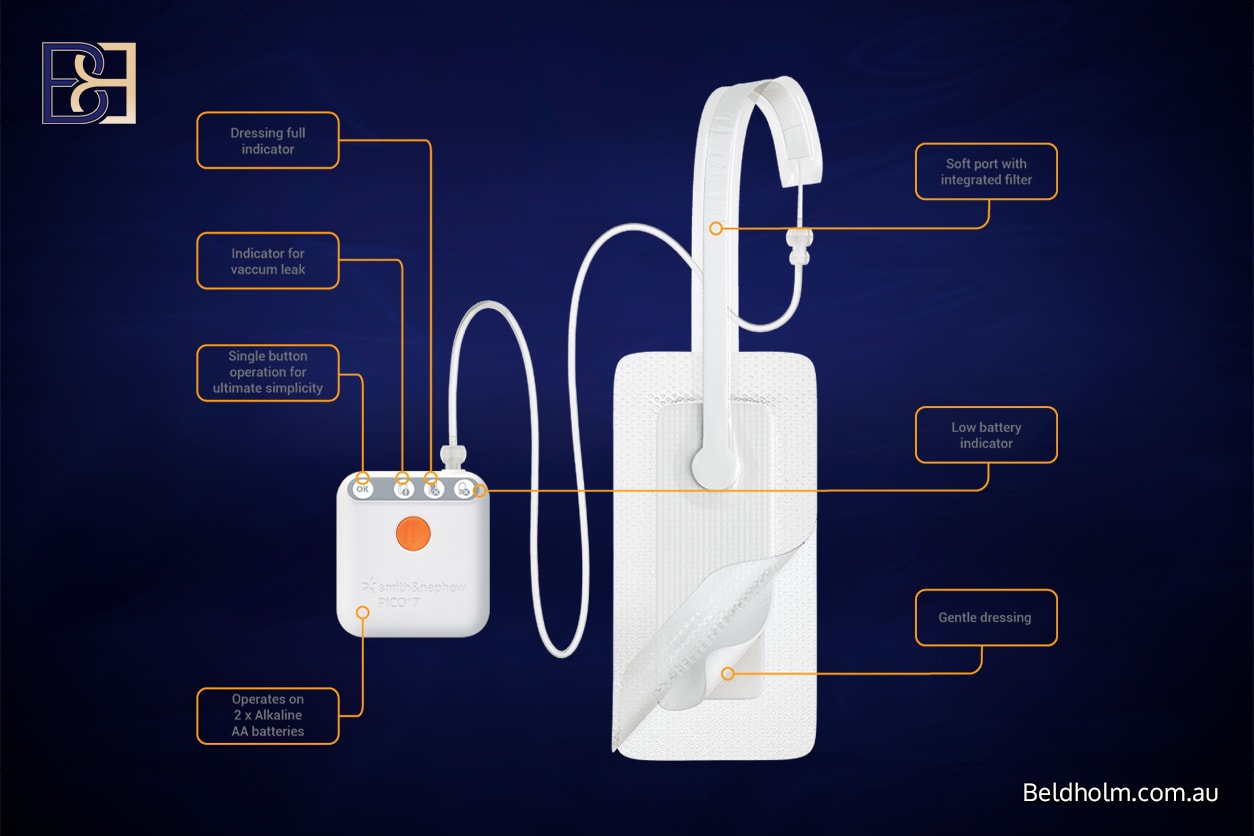
Dressing management varies depending on the extent of surgery and whether an anterior or circumferential approach was used.
- PICO negative pressure dressings are routinely used on the anterior chest area following anterior torsoplasty (upper body lift) surgery
- PICO dressings are designed to support wound healing, manage fluid, and reduce the risk of wound complications
- In most cases, PICO dressings are left in place for approximately 7 days
- Occasionally, if a PICO dressing is not functioning as intended or loses its seal, it may need to be changed earlier
For patients undergoing a circumferential upper body lift (torsoplasty), additional dressings are required:
- Comfeel dressings are commonly used on the side and back incisions
- These dressings protect the surgical wounds and support healing in areas subject to movement and tension
- Comfeel dressings are reviewed and changed during follow-up appointments at my Lorn clinic
Patients should avoid removing or disturbing dressings unless specifically instructed to do so. Showering instructions are individualised and explained before discharge. Keeping dressings clean, dry, and intact supports proper wound healing and reduces complications.
Managing the Nipple–Areola Complex (NAC) Graft
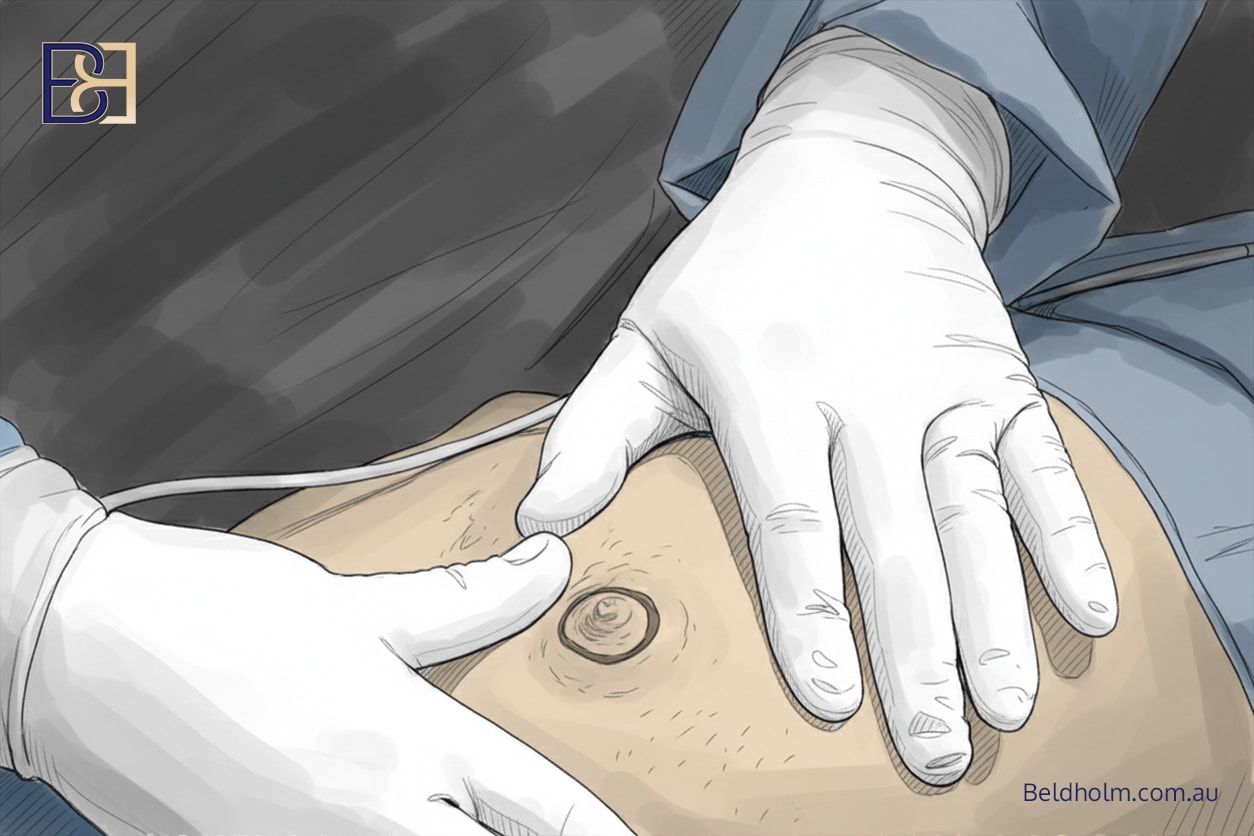
In male upper body torsoplasty surgery following weight loss, a free nipple–areola graft is used.
- The NAC graft is secured with a bolster dressing, which is attached to the surrounding skin using surgical clips
- The purpose of the bolster is to apply gentle, even pressure to the graft, which supports graft survival and healing
- The bolster dressing is intentionally left undisturbed during the early healing phase
- The bolster and surgical clips are usually removed around day 10 after surgery during a clinic visit
Temporary changes in colour, sensation, or firmness of the nipple–areola complex are expected during early healing.
Patients are advised:
- Not to tamper with the bolster or surgical clips
- To avoid pressure, stretching, or tension across the chest
- To follow all dressing, compression, and activity instructions carefully
Successful NAC graft healing depends on maintaining pressure, minimising movement, preserving blood supply, and close follow-up. My team monitors NAC graft healing closely throughout the recovery period.
Recovery After Upper Body Lift (Torsoplasty)

Recovery after an upper body lift (torsoplasty) follows the same core principles for all patients, regardless of whether the procedure is performed as an anterior torsoplasty, a circumferential upper body lift (torsoplasty), or combined with VASER liposuction (Suction-assisted lipectomy). What differs is the extent of surgery, which can influence discomfort, swelling, drain duration, and the overall recovery timeline.
In every procedure, Dr Beldholm excises excess skin, fat, and tissue, including breast tissue. The incision is strategically positioned along the inferior border of the pectoralis major muscle to reduce visible scarring and promote optimal healing. Furthermore, free nipple–areola complex (NAC) grafts are utilised in all male upper body torsoplasty surgeries, carefully repositioned to restore the nipple to its anatomically correct location on the male chest.
Hospital Stay – What to Expect Immediately After Surgery
Book your appointment online now
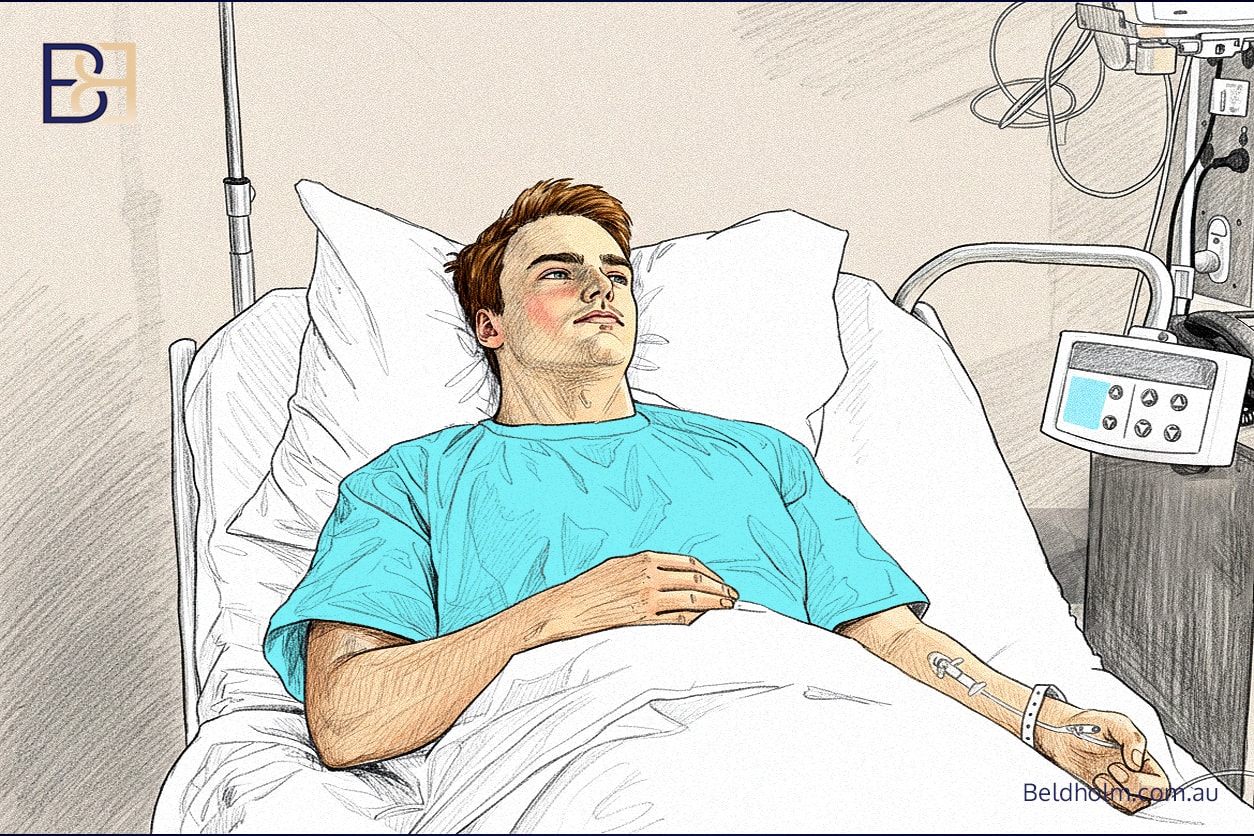
After your upper body lift (torsoplasty) surgery, you will wake up in the recovery unit at Maitland Private Hospital. This is a closely monitored area where the nursing team, your anaesthetist, and I ensure you are stable and comfortable before transfer to the ward.
Most patients can expect the following when they wake up:
- An indwelling urinary catheter (IDC) to monitor urine output, particularly important after longer surgeries
- Surgical drains to reduce fluid accumulation
- A patient-controlled analgesia (PCA) pump for pain relief in the early phase
- PICO negative pressure dressings on the anterior chest
- Comfeel dressings on the side and back incisions if a circumferential upper body lift has been performed
- Your compression garment is already in place
Both Dr Beldholm and your anaesthetist will review you in recovery before you are transferred to the ward.
The First Night in Hospital
For most patients, the first night is the most challenging. Sleep can be difficult due to:
- Background ward noise
- Post-operative pain and tightness
- Limited movement due to drains, PCA, IDC, and dressings
This is normal and expected, particularly after longer procedures.
Day 1 After Surgery
I review all patients on the morning of day 1 after surgery.
Day 1 can still be challenging. Patients who have undergone circumferential surgery or significant liposuction often experience:
- Higher pain levels
- Increased swelling
- Occasional blood pressure fluctuations
Patients who have had anterior torsoplasty alone often find day 1 slightly more manageable, although discomfort and fatigue are still common.
The primary goal for day 1 is mobilisation:
- Sitting out of bed
- Standing with assistance
- Taking short walks with nursing support
Early mobilisation is critical to:
- Reduce the risk of blood clots
- Improve circulation
- Support the overall recovery process
Progress is gradual, and support is provided at every step.
Pain, Tightness, and Fatigue
- Tightness across the chest is expected for all patients
- Patients who undergo circumferential surgery often experience additional tightness through the sides and upper back
- Fatigue is common and may last longer when a larger surface area is treated
- Discomfort is usually most noticeable in the first 1–2 weeks and gradually resolves
Drains
- Surgical drains are routinely used
- Patients undergoing circumferential surgery often require more drains or longer drain duration
- Drains are typically removed within 5–10 days, depending on output
Compression Garments

- Compression garments are essential for all upper body lift (torsoplasty) patients
- Worn continuously for six to eight weeks
- Circumferential surgery and VASER liposuction (suction-assisted lipectomy) may require longer or more extensive compression coverage
Activity Restrictions
- Walking is encouraged from day one as part of the recovery process to reduce swelling and lower the risk of blood clots
- No heavy lifting or strenuous upper body activity for at least 6 weeks
- Circumferential surgery requires additional care with twisting and reaching movements
- Return to desk-based work is commonly possible around weeks 3–4, depending on recovery progress
When VASER Liposuction (suction-assisted lipectomy) Is Added
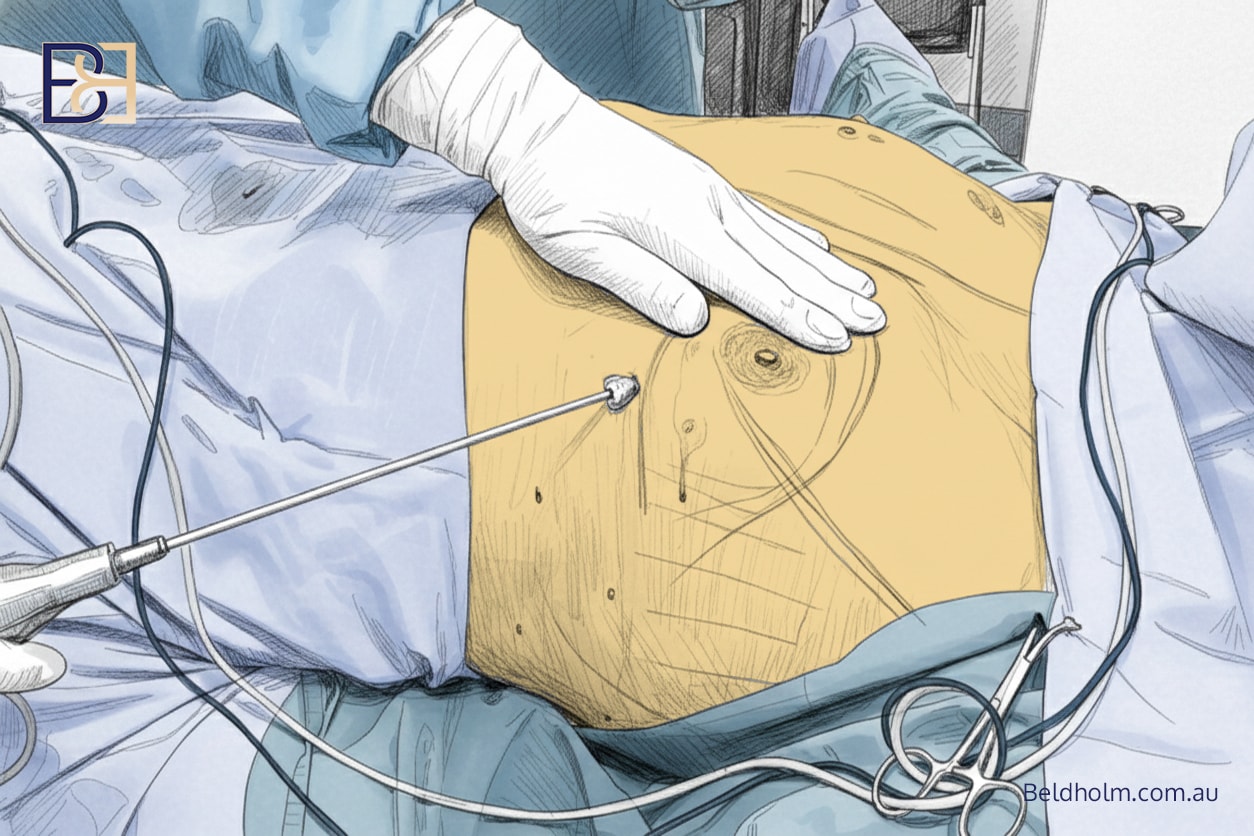
When VASER liposuction (suction-assisted lipectomy) is combined with an upper body lift (torsoplasty):
- Swelling and bruising are usually more pronounced
- Treated areas may feel firm or tender during early healing
- Compression is particularly important to help reduce swelling
- Final contour may take longer to settle, often 3–6 months
Expected Recovery Timeline (General Guide)
The following timeline is a general guide to help patients understand how recovery typically progresses after an upper body lift (torsoplasty). Individual recovery will vary depending on the extent of surgery, overall health, and whether circumferential surgery or significant liposuction has been performed.
Weeks 0–2: Immediate Post-Operative Phase
This is the most intensive phase of recovery.
- Significant swelling, tightness, and bruising are expected
- Fatigue is common, and energy levels are low
- NAC grafts are in their protection phase with bolster dressings in place
- Drains, dressings, compression garments, and limited mobility are all part of daily recovery
- Pain is most noticeable during this period, but is actively managed
- Drains and bolster dressings have usually been removed
The focus during this phase is rest, wound protection, pain control, and early mobilisation.
Weeks 3–6: Early Functional Recovery
During this phase, most patients notice a steady return to function.
- Swelling begins to reduce, though it is still present
- Comfort and mobility gradually return to baseline
- Patients become more independent with daily activities
- Ongoing scar and NAC graft monitoring continues
Many patients can return to desk-based work during this period, depending on their recovery progress.
Weeks 6–12: Progressive Return to Normal Activity
This phase marks the transition back toward normal routines.
- Tightness continues to ease
- Activity levels can increase gradually under guidance
- Compression garments may be discontinued as advised
- Light exercise may be introduced
Although patients feel significantly better, tissues are still healing and require care.
Beyond 3 Months: Ongoing Healing and Scar Maturation
Healing continues well beyond the early recovery period.
- Residual swelling slowly resolves
- Scars soften and fade over time
- Final contour continues to evolve
Scar maturation and tissue settling can take many months, and patience remains important throughout this phase.
Follow-Up Appointments at My Lorn Clinic

Follow-up care is a core part of recovery after upper body lift (torsoplasty) surgery and is deliberately structured to support healing, reassurance, and early identification of issues. Recovery does not end when you leave the hospital.
In my practice, the first two weeks after surgery are the most intensive phase of follow-up. During this period, patients are typically reviewed two to three times per week by my nursing team and me at my Lorn clinic. This level of follow-up reflects the complexity of recovery after male upper body torsoplasty and the importance of close monitoring during early healing.
During these early visits, we focus on:
- Assessing overall recovery and pain control
- Monitoring blood pressure, swelling, and fluid shifts
- Reviewing drains, dressings, and compression garments
- Assessing NAC graft viability and healing
- Supporting early mobilisation
In the first week after surgery, reviews are particularly important. PICO dressings are checked to ensure they are functioning correctly and may be changed earlier than day 7 if required. Drain output is monitored closely, and early issues can be treated before they escalate.
Around day 7 to day 10, patients are reviewed again. This is usually when:
- PICO dressings are removed from the anterior chest
- The NAC bolster and surgical clips are removed
- Drain output is reassessed, and drains are often removed if appropriate
The first two weeks are focused on wound healing, graft take, swelling management, and adjustment of compression garments. This period sets the foundation for long-term healing and scar quality.
After this intensive phase, follow-up continues at gradually increasing intervals over the following weeks and months. These later reviews focus on scar maturation, ongoing swelling or firmness, progression of activity levels, and longer-term recovery milestones.
Patients are encouraged to contact the clinic at any stage if something does not feel right. Early review is always preferred over waiting, and follow-up is an active part of care rather than a formality.
Managing Risks During Recovery
All surgical procedures carry risk. During recovery, we actively work to reduce:
- Blood clots through early mobilisation
- Wound infection through monitoring and wound care
- Fluid collections with drains and compression
Prompt communication with the clinic is essential if concerns arise.
Long-Term Recovery and Expectations

Final results from upper body lift surgery (torsoplasty), a major surgical procedure following significant weight loss, take time and progress throughout the recovery period. Swelling resolves gradually, scars mature over many months, and the body continues to adapt.
Maintaining a stable weight and a healthy lifestyle supports long-term results after body lift (torsoplasty) and body contouring surgery, particularly following major weight loss. Future weight changes can affect the remaining skin and overall body shape.
Dr Bernard Beldholm’s Final Thoughts

Recovery after male chest surgery post-weight loss depends heavily on the type of surgery performed. Anterior torsoplasty, circumferential Torsoplasty (body lift) surgery, and the addition of VASER liposuction (Suction-assisted lipectomy each come with different recovery demands.
My role is not only to perform the surgery, but to guide patients through recovery at Maitland Private Hospital and ongoing care at my Lorn clinic, ensuring clarity and realistic expectations at every stage.