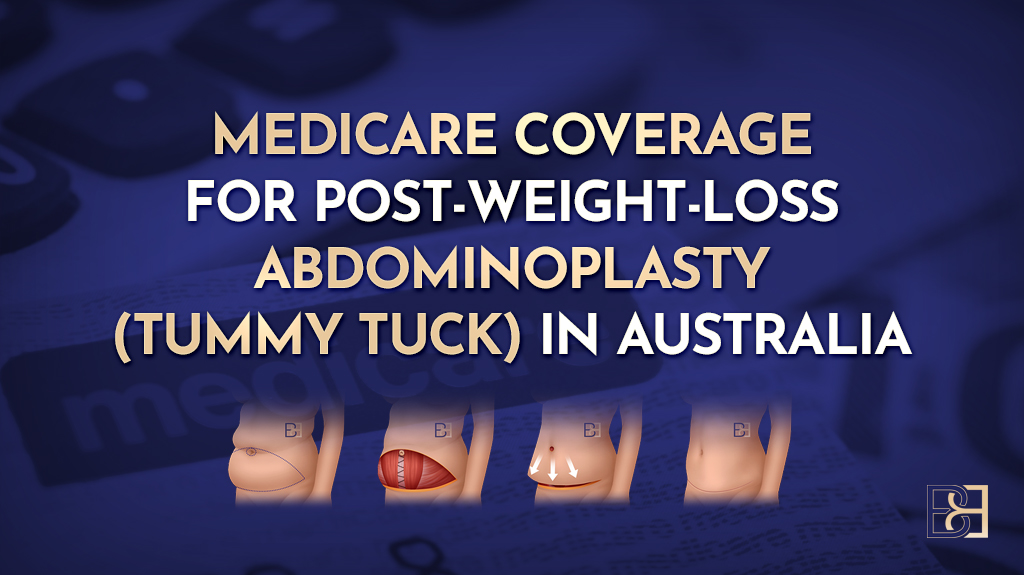
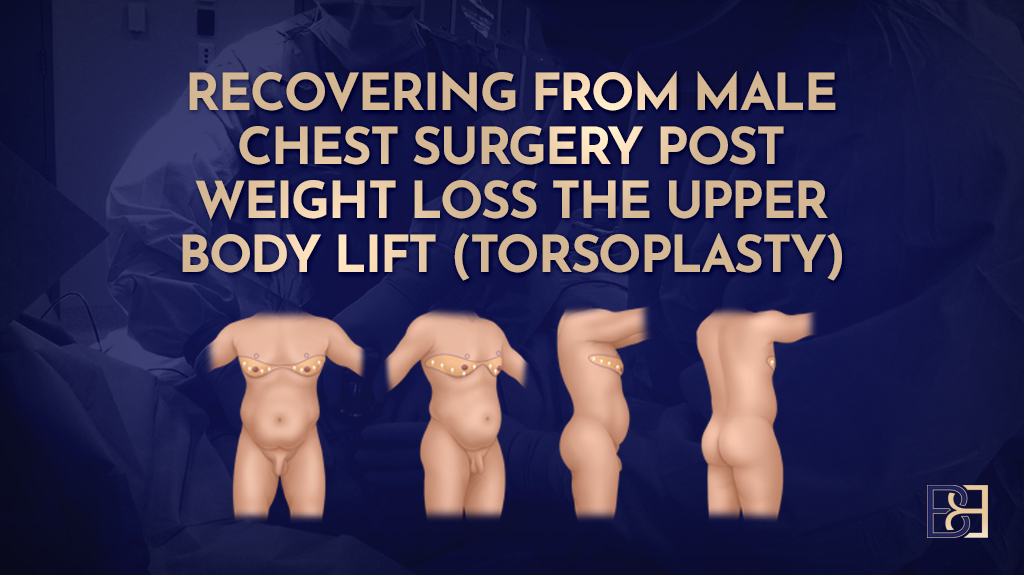
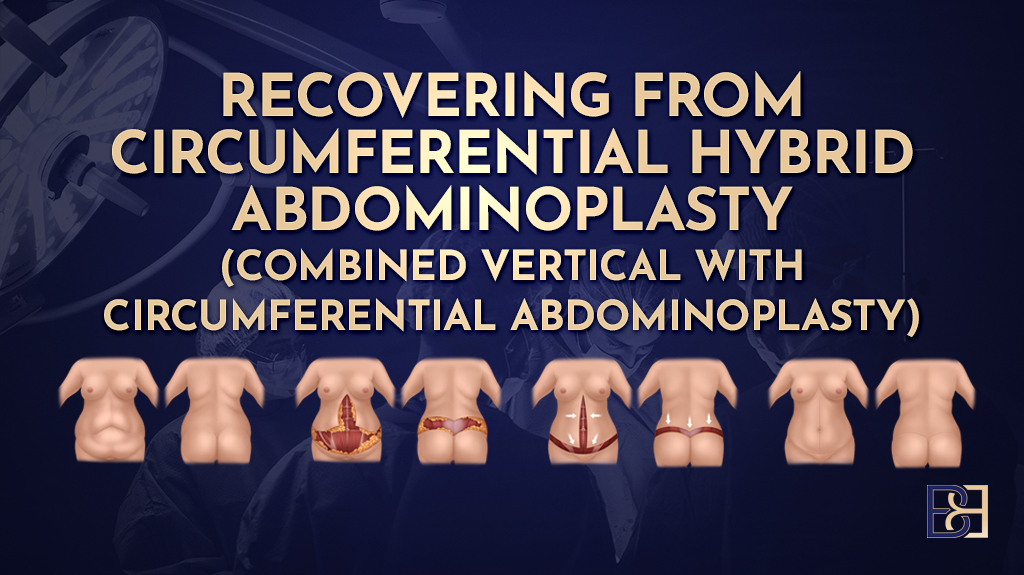
Dual vector abdominoplasty is an advanced form of abdominoplasty surgery designed for patients who have experienced significant weight loss. It combines principles of the Fleur-de-Lis abdominoplasty with an additional upper abdominal skin excision, allowing excess skin to be addressed in multiple directions, including the upper abdomen and lower chest region.
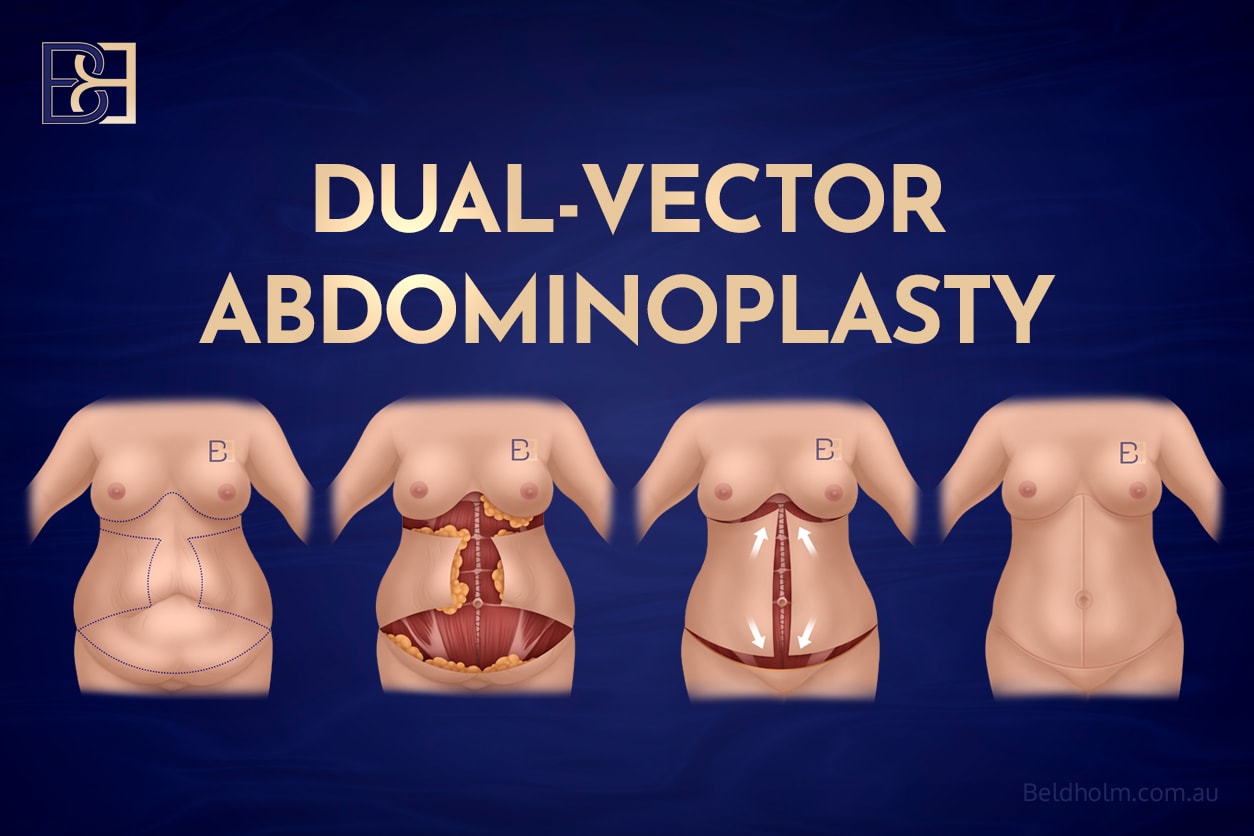
Because this is a complex reconstructive operation involving multiple incisions and extensive tissue mobilisation, the complication profile is similar to other post-weight-loss body contouring surgeries, particularly Fleur-de-Lis abdominoplasty. However, due to the additional incision and increased wound surface area, some complications may occur more frequently than in standard tummy tuck (abdominoplasty) procedures.
Understanding these potential complications is an essential part of informed consent and surgical planning.
Why Complications Are More Common After Post-Weight-Loss Abdominoplasty
Patients seeking dual vector abdominoplasty are often very different from those undergoing standard abdominoplasty. Following massive weight loss, the skin, fat tissue, and underlying structures have usually undergone prolonged stretching, changes in blood supply, and loss of elasticity.
Several recognised risk factors contribute to higher complication rates in post-weight-loss abdominoplasty, including:
- Large amounts of excess skin
- Reduced skin quality and elasticity
- Altered blood supply to the abdominal skin
- Nutritional deficiencies following bariatric surgery
- Previous abdominal operations
- Longer operative times
- Multiple incision lines under tension
For these reasons, dual vector abdominoplasty is best considered a form of reconstructive surgery, rather than a simple cosmetic procedure.
Most Common Complications After Dual Vector Abdominoplasty
Wound Breakdown and Wound-Related Complications
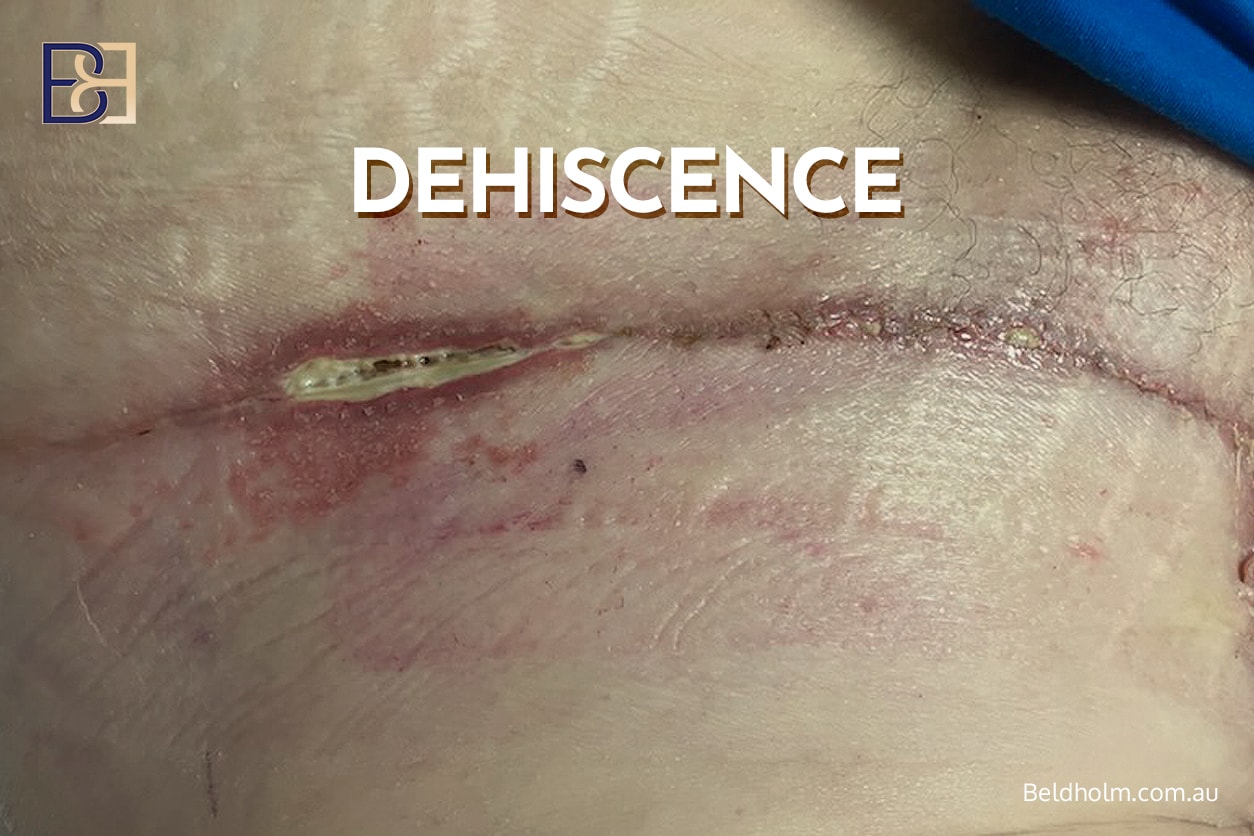
Wound breakdown is the most common complication after dual-vector abdominoplasty. This is consistent with findings from the aesthetic plastic surgery and reconstructive surgery literature on Fleur-de-Lis and post-weight-loss abdominoplasty procedures.
Wound-related complications may include:
- Delayed wound healing
- Small areas of wound separation
- Breakdown at incision junctions
- Localised skin loss
These issues most commonly occur:
- Where vertical and horizontal incisions intersect
- Along the upper abdominal incision
- Around the belly button
The underlying cause is usually reduced blood supply to the skin combined with tension across the wound during healing. In most cases, wound breakdown represents a minor complication and can be managed with careful wound care, dressings, and close follow-up. In some situations, surgical debridement or delayed primary closure may be required.
Infection
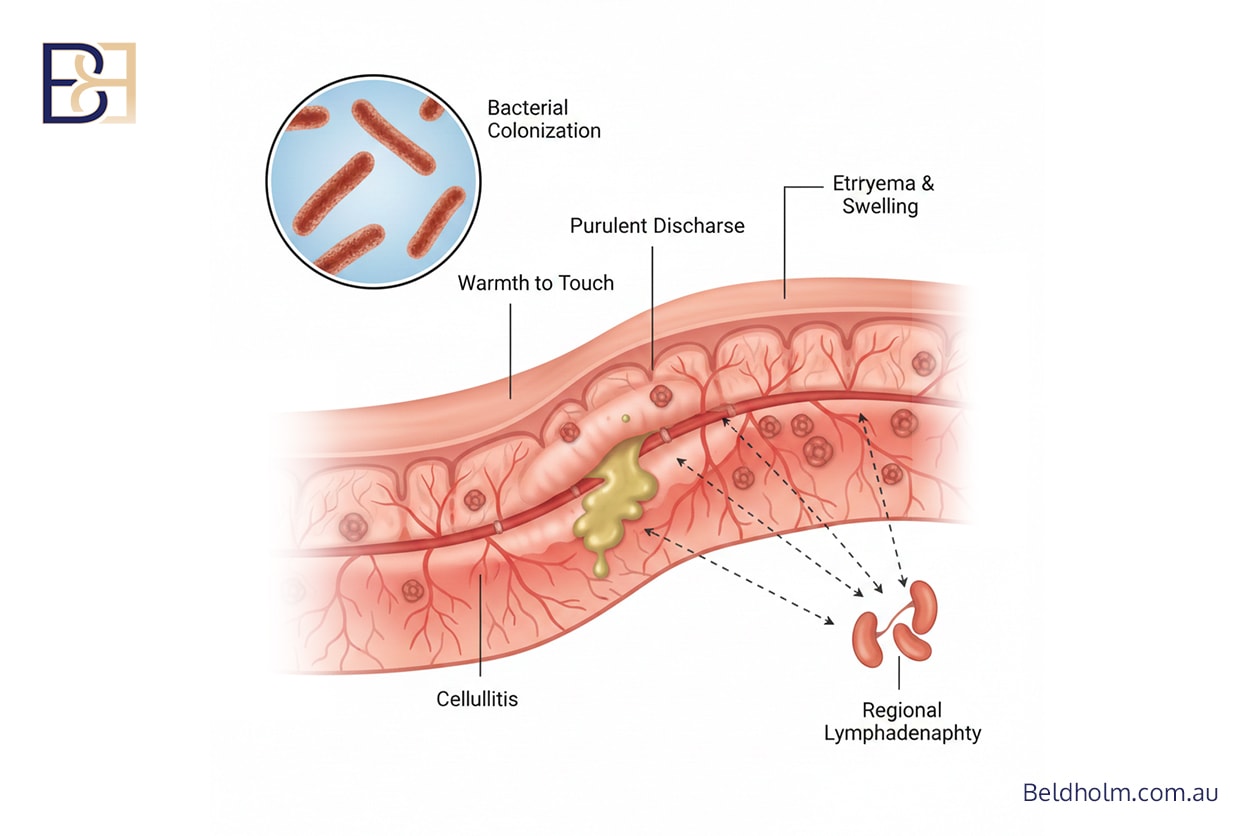
Infection is a recognised risk following abdominoplasty surgery, particularly when large skin flaps and multiple incisions are involved. Infections may be superficial or deeper and can present with redness, swelling, pain, discharge, or fever.
Risk factors for infection include:
- Prolonged healing
- Seroma formation
- Reduced blood flow to the skin
- Underlying medical conditions
Most infections are treated successfully with antibiotics and local wound care. Serious complications such as deep infection or sepsis are rare but possible and require urgent medical assessment.
Seroma Formation
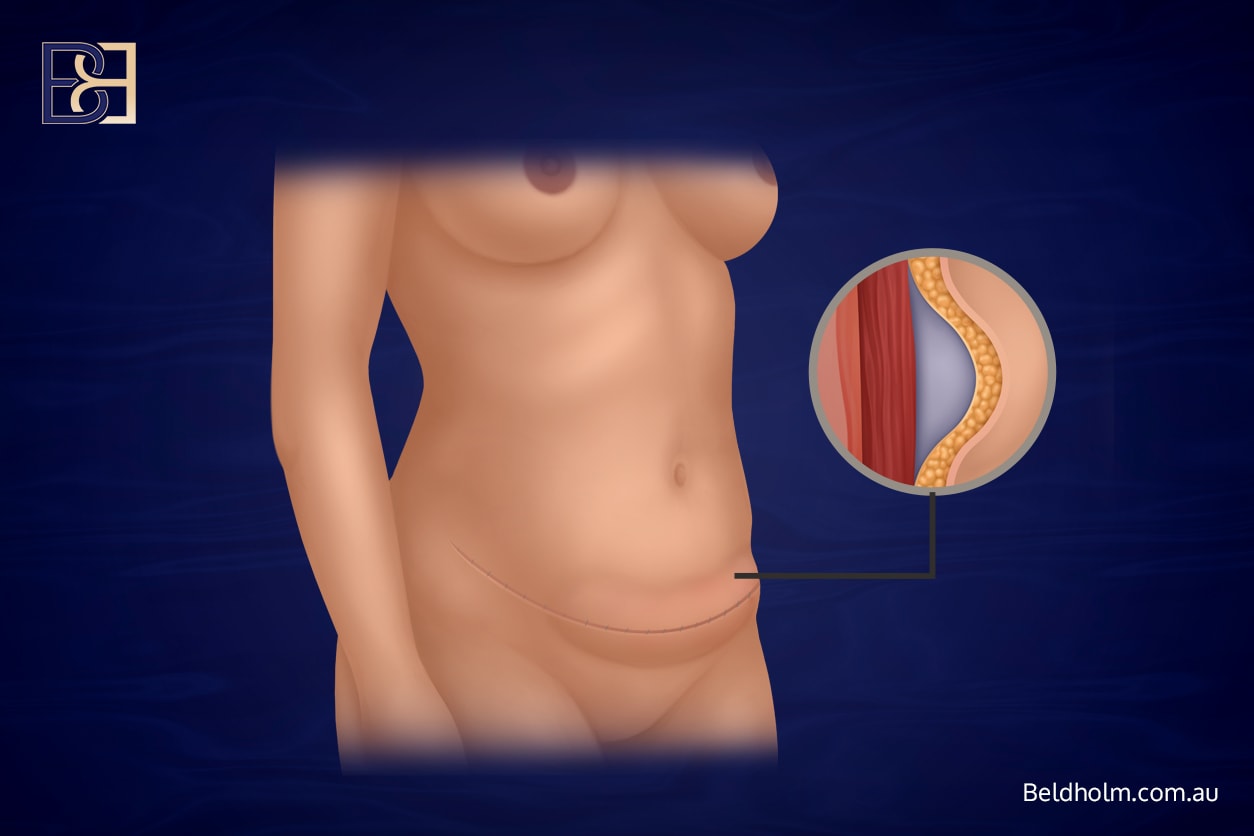
Seroma formation is one of the most frequent complications after dual vector abdominoplasty and Fleur-de-Lis abdominoplasty.
A seroma is a collection of clear fluid that accumulates beneath the skin after surgery. It occurs because lymphatic channels are disrupted during the procedure and a large potential space exists between the skin and the abdominal wall.
Seroma formation may present as:
- Localised swelling
- A fluid-like sensation
- Increased abdominal fullness
Management depends on severity and may include:
- Observation
- Surgical drainage
- Needle aspiration
- Compression garments
Most cases resolve over time, but persistent seromas may require repeated drainage or, in rare cases, further surgery.
Skin Necrosis and Blood Supply Issues

Skin necrosis refers to the loss of skin due to inadequate blood supply. This complication is more common in post-weight-loss abdominoplasty patients and in procedures with multiple incision lines.
Risk factors include:
- Smoking history
- Diabetes
- Poor nutritional status
- Previous abdominal surgery
Small areas of skin necrosis are usually managed conservatively with dressings and wound care. Larger areas may require surgical debridement and prolonged healing.
Bleeding and Haematoma
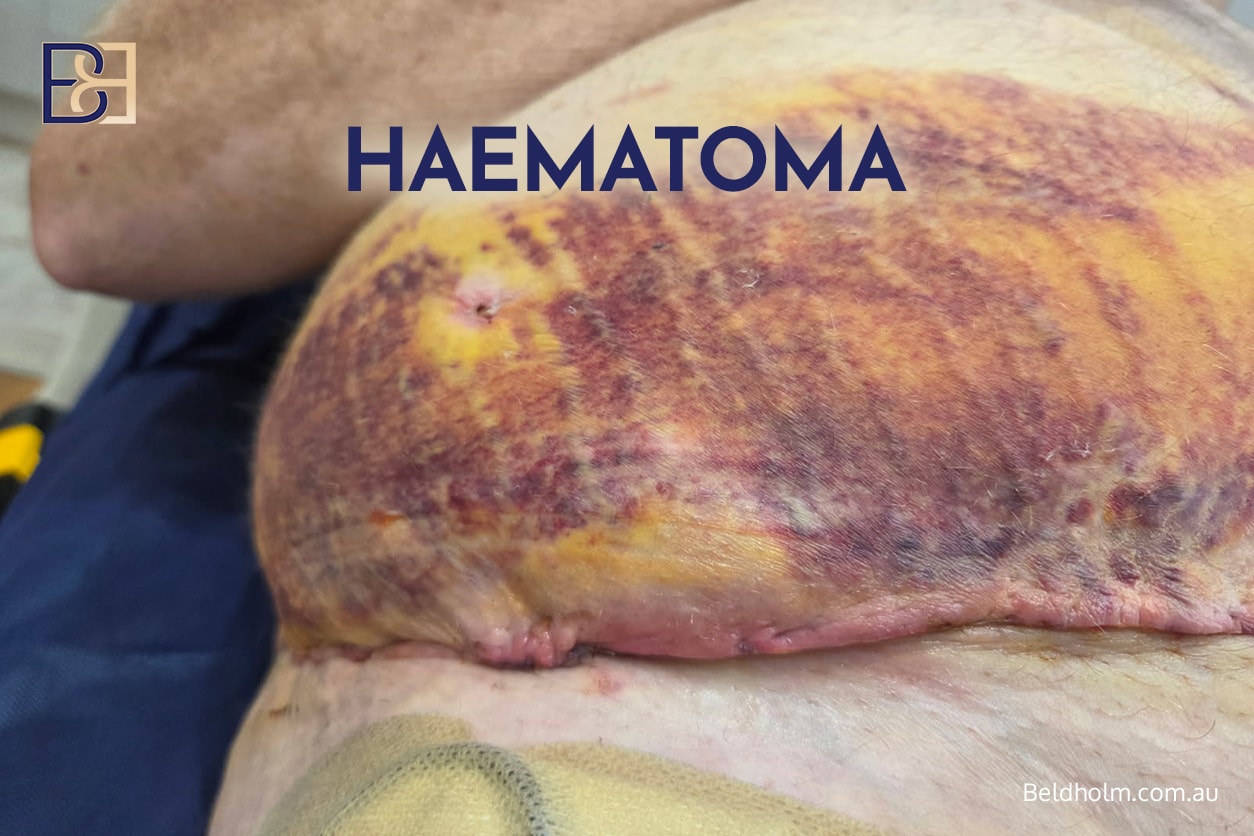
Bleeding during or after surgery can result in a haematoma, which is a collection of blood beneath the skin. This may cause swelling, discomfort, and an increased risk of infection.
Most haematomas are identified early and managed promptly. Return to the theatre is uncommon but may be required in cases of significant bleeding.
Scarring and Abnormal Scar Formation
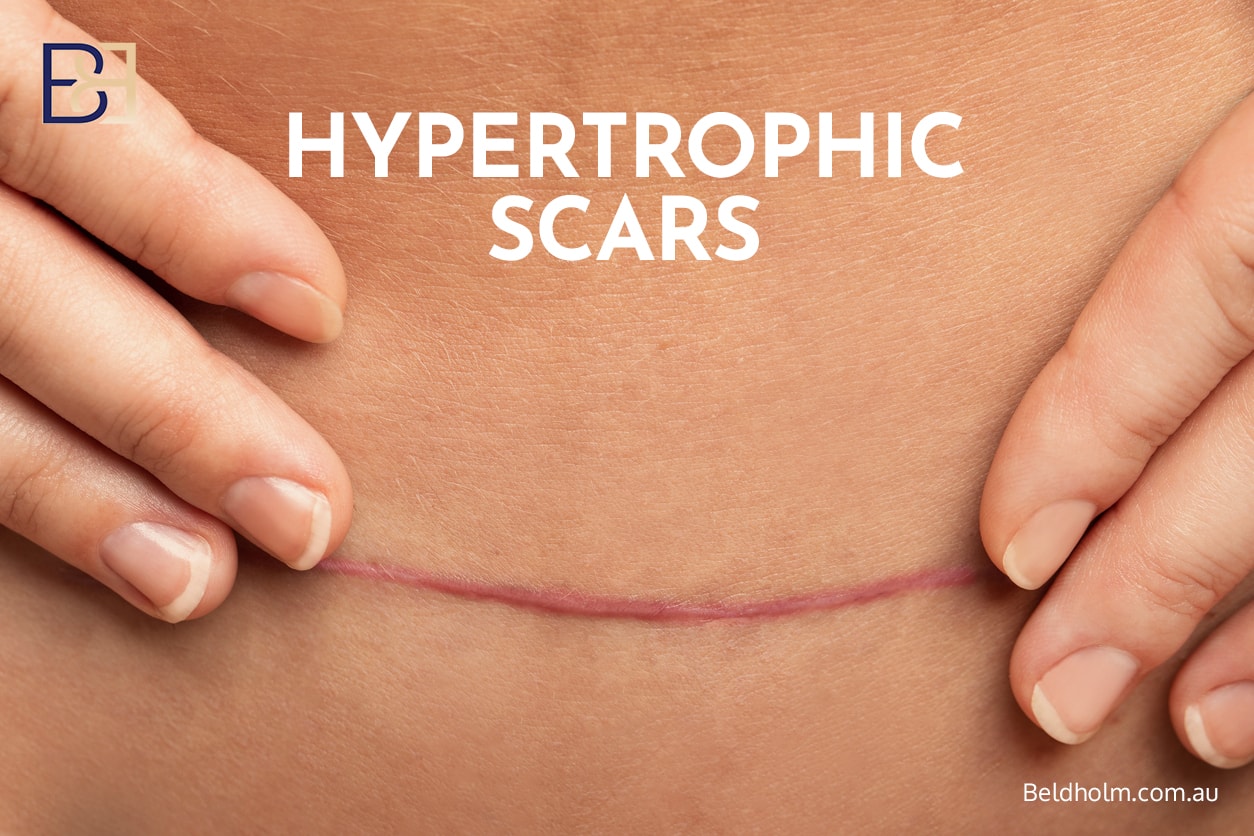
All abdominoplasty procedures result in permanent scars. Dual vector abdominoplasty involves more extensive scarring than standard tummy tuck (Abdominoplasty) procedures, including:
- A lower abdominal scar
- A vertical midline scar
- An upper abdominal or inframammary scar
Some patients may develop:
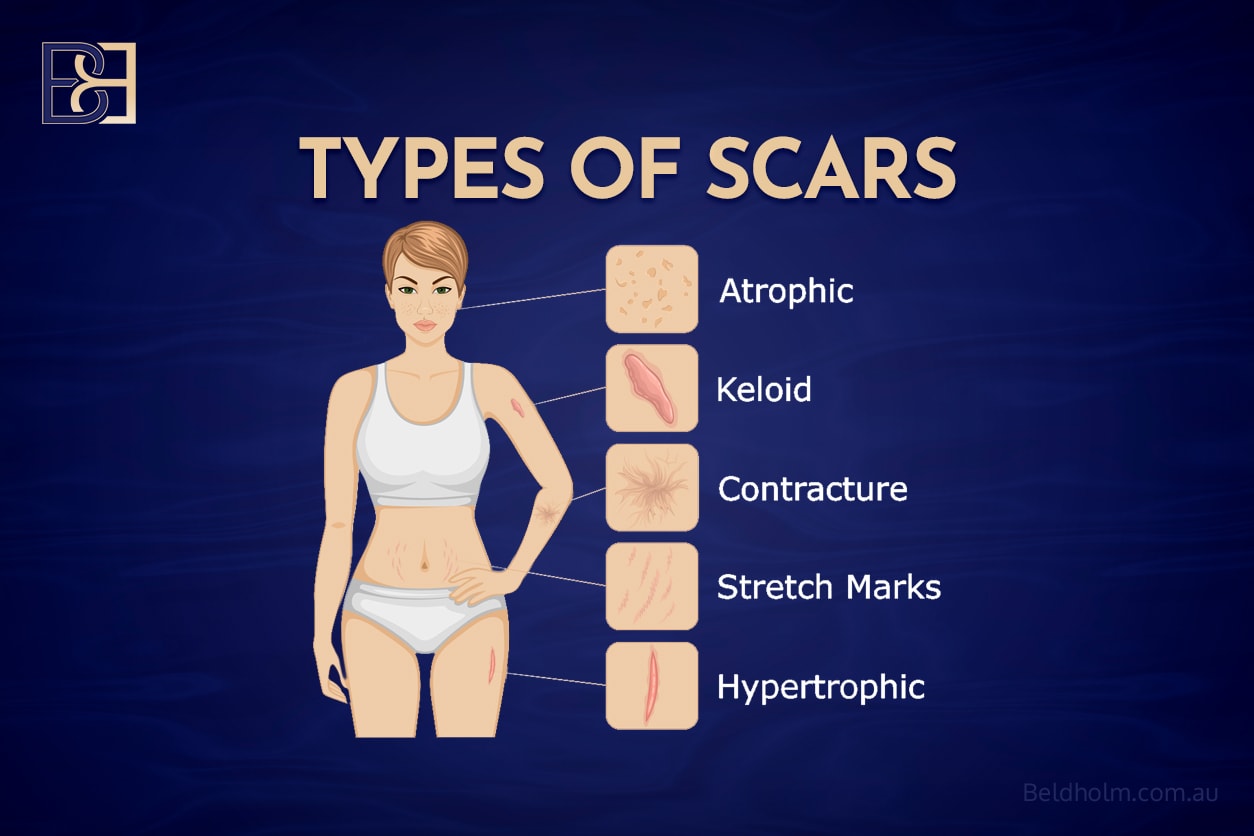
- Thickened scars
- Hypertrophic scars
- Keloid formation
Scar appearance is influenced by skin type, genetics, wound tension, and individual healing response. While scar management strategies can help, scars cannot be completely eliminated.
Changes in Sensation and Nerve-Related Issues
Book your appointment online now
Temporary numbness of the abdominal skin is common following abdominoplasty and usually resolve over several months. This occurs due to disruption of small sensory nerves during surgery.
Permanent changes in sensation are less common but can occur, particularly after extensive procedures involving large areas of skin removal.
Belly Button and Abdominal Wall Complications
The belly button is repositioned during most abdominoplasty procedures. Possible complications include delayed healing, infection, or partial loss of the belly button. These issues are uncommon and usually manageable with appropriate treatment.
Repair of the underlying muscles of the abdominal wall may result in temporary tightness or discomfort. In rare cases, muscle repair failure can occur.
Serious Complications: Blood Clots and Pulmonary Embolism
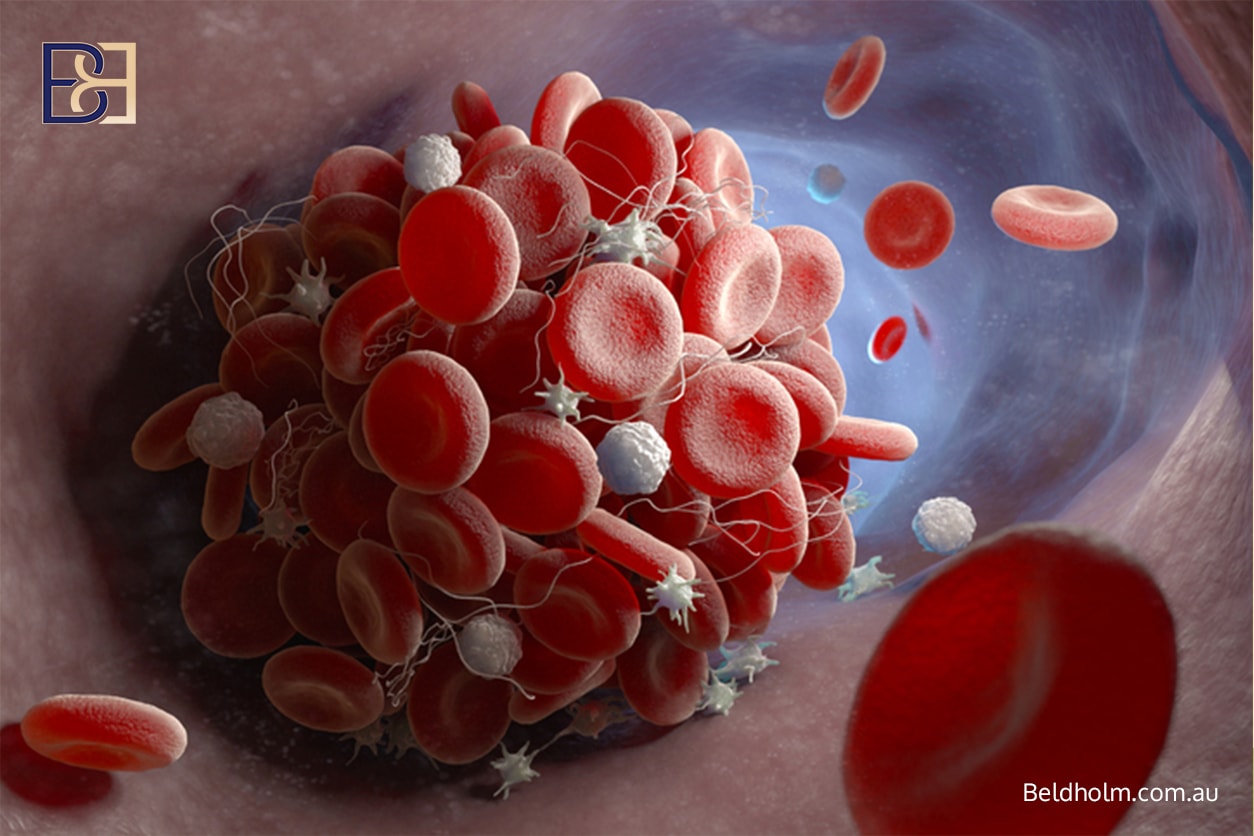
Although uncommon, serious complications such as deep vein thrombosis and pulmonary embolism are recognised risks following major surgery.
Risk reduction strategies include:
- Careful pre-operative assessment
- Early mobilisation after surgery
- Mechanical compression devices
Patients are advised to seek urgent medical attention if they experience symptoms such as leg swelling, chest pain, or shortness of breath.
Can Complications Occur Long After Surgery?
Most complications occur during the early healing phase. However, rare cases of late complications such as chronic seroma, scar-related problems, or abdominal wall weakness have been reported.
Long-term follow-up with the treating surgeon and ongoing involvement of the patient’s GP are important.
How Are Complications Managed?
The management of complications depends on their nature and severity. Many complications can be managed without additional surgery, while others may require further procedures or prolonged wound care.
Early recognition and prompt treatment are key factors in reducing the impact of complications.
Final Considerations

Dual vector abdominoplasty can treat excess skin that cannot be effectively treated with traditional abdominoplasty techniques. However, it is a major operation with higher complication rates than standard cosmetic procedures.
A detailed consultation, thorough review of medical history, and realistic expectations are essential. Patients must understand that complications are a recognised part of surgery and that healing can be prolonged following post-weight-loss body contouring.