Male Chest Surgery Post-Weight Loss: Understanding Upper Body Lift (Torsoplasty)
Upper and Circumferential Torsoplasty (upper body lift) surgery in men is a highly effective procedure that removes excess skin and fat from the arms, chest, back, and abdomen. This procedure is especially beneficial for individuals who have undergone significant weight loss and are left with loose, excess skin that can cause discomfort and limit mobility. Dr Bernard Beldholm, a specialist surgeon focused on post-weight-loss body contouring, offers an upper body lift (Torsoplasty) as part of his comprehensive approach to post-weight-loss body contouring in men.
Male chest surgery post-weight loss is increasingly requested by men who have achieved significant weight loss but are left with loose skin, excess skin and fat, and a feminised chest contour. For most patients, the anterior chest is one of the most confronting areas after weight loss, despite major health benefits.
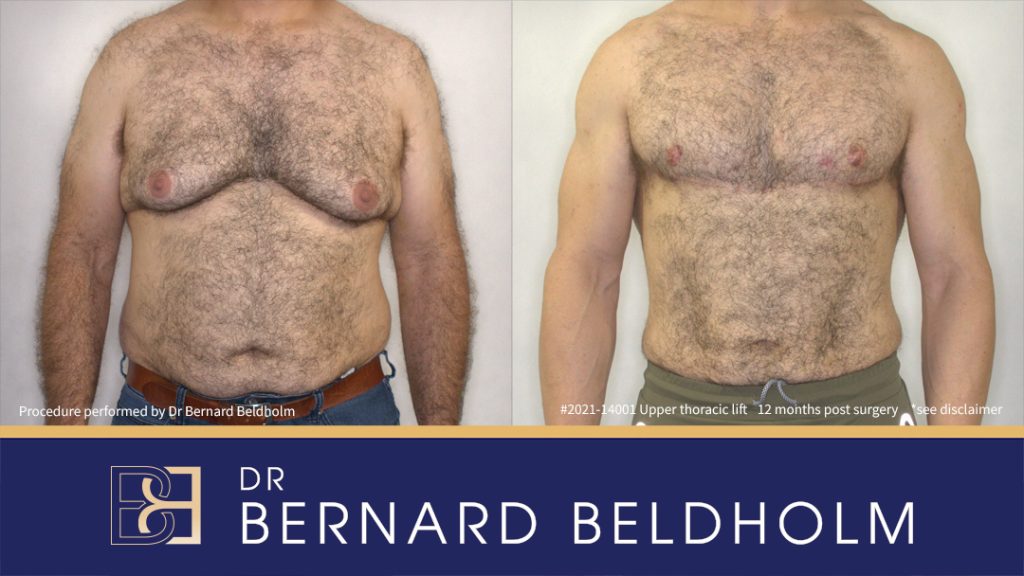
Disclaimer: Operation performed by Dr Bernard Beldholm. Adult content, surgery has risks; individual results vary, seek 2nd opinion. Please see the full disclaimer.
Why the Male Chest Changes After Weight Loss
In males who have lost significant weight, there is a notable overlap with gynaecomastia (development of breast tissue in males). Many men who gain a significant amount of weight develop pseudo-gynaecomastia, a condition where excess fat accumulates in the chest area, making it look like gynaecomastia. Weight gain itself can lead to actual breast tissue development. Therefore, the management of male chest post-weight loss shares considerable overlap with that of male gynaecomastia, requiring a careful, tailored approach to the removal of excess skin and breast tissue.
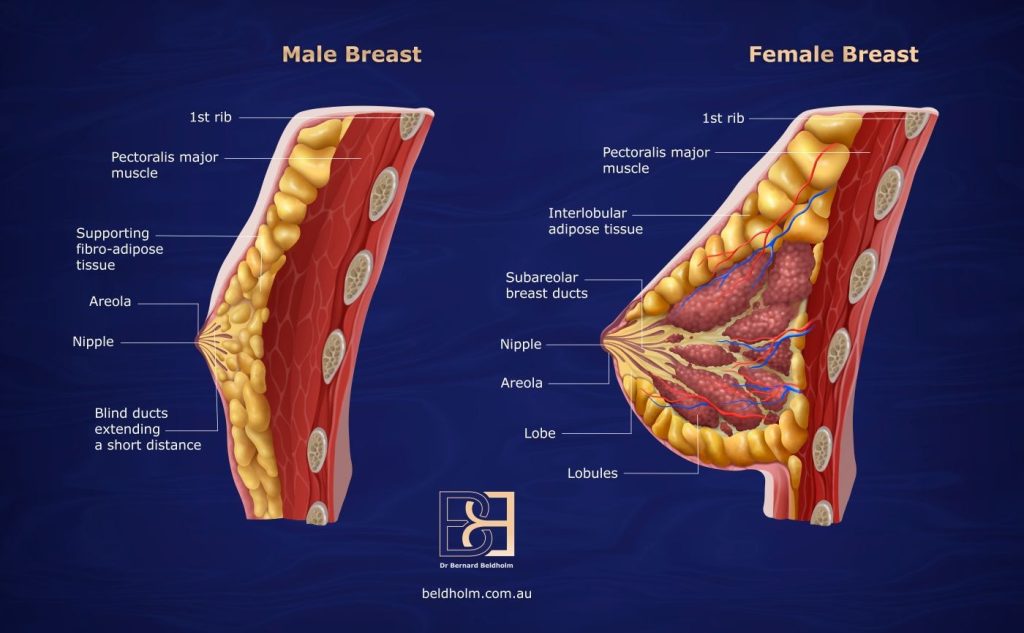
After massive or extreme weight loss, the chest skin often loses its ability to retract. This leads to loose skin, excess tissue, and visible skin folds. While weight loss reduces excess body weight and extra fat, it does not reliably tighten skin, particularly in men who have undergone bariatric surgery or have carried excess body weight for many years.
Common concerns include:
- Loose chest skin and lax skin
- Excess skin and fat hanging over the chest
- Low or downward-facing nipples
- Rashes, irritation, and hygiene problems in skin folds
- Difficulty wearing fitted clothing or going shirtless
For most patients, these issues persist even at a stable weight.
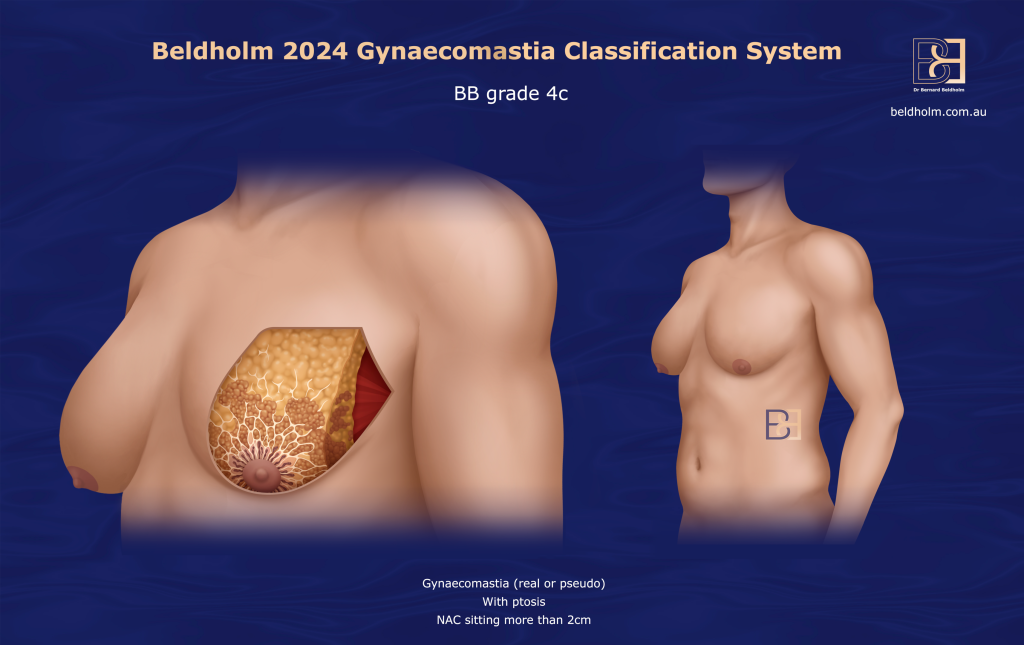
Gynaecomastia, Pseudogynaecomastia, and Post-Weight Loss Chest Deformity
Post-weight loss chest deformity differs from standard gynaecomastia. While gynaecomastia involves glandular tissue, post-weight loss deformity is usually driven by excess skin, loose skin, and residual fat.
- Gynaecomastia: glandular breast tissue
- Pseudogynaecomastia: excess fat
- Post-weight loss chest deformity: excess skin, skin laxity, and excess tissue
Treating post-weight loss patients using limited gynaecomastia techniques often leads to poor contour and persistent lax skin.
What Is Upper Torsoplasty (Body Lift) Surgery for Men After Significant Weight Loss?
When considering upper torsoplasty (upper chest lipectomy, body lift) in men, several important factors should be considered. This surgery is designed to treat the unique challenges men face after significant weight loss, particularly in the chest and upper body. One of the key aspects of upper torsoplasty is treating the anterior chest, which often requires a similar approach to that used in the management of gynaecomastia (male breast tissue development).
For many men, pseudo-gynaecomastia (excess fat in the chest) may also be present. Post-weight loss, this fat often leads to a female-like chest appearance. The goal is to excise both the breast tissue (if needed) and excess skin, repositioning the nipple to achieve a masculine-looking chest.
In addition to the chest area, the back and sides can also be treated as part of a circumferential torsoplasty. This comprehensive procedure not only lifts and tightens the chest but also treats the back and side of the chest. The patient is typically turned during surgery to allow Dr Beldholm to focus on these areas from both the front and the back.
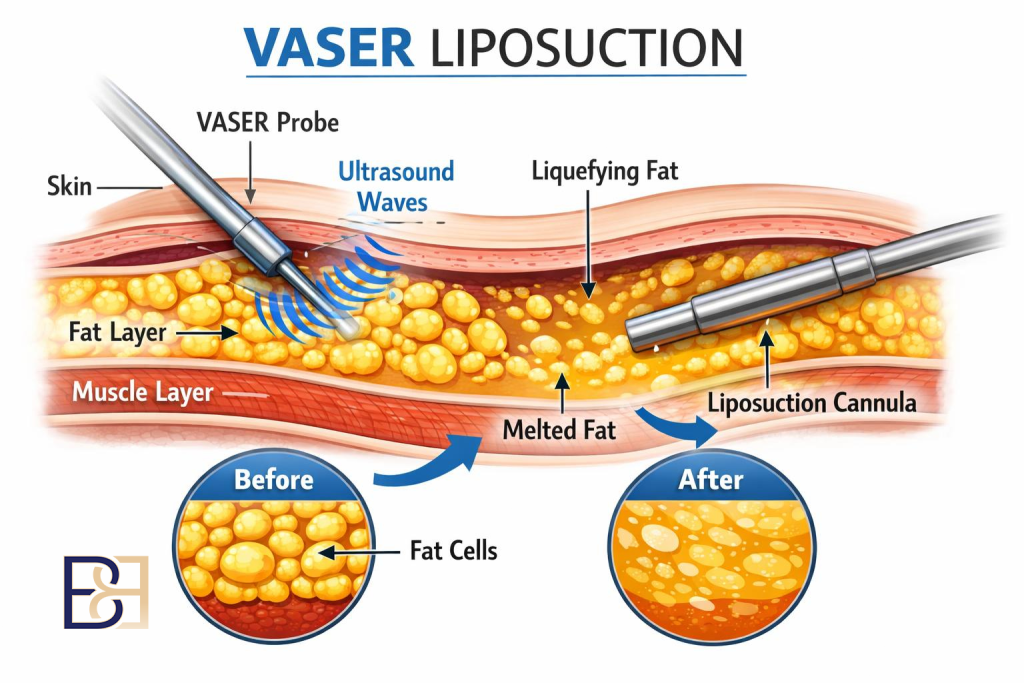
VASER Liposuction (Suction-assisted Ultrasonic Liposuction)
Although many post-weight-loss patients achieve their ideal BMI and maintain a stable weight, some may still have excess fat deposits that don’t respond to diet or exercise. In these cases, suction-assisted lipectomy with VASER technology may be an essential component of the surgery. This allows fat to be removed from areas such as the chest, back, or abdomen. Dr Beldholm prefers using suction-assisted lipectomy with VASER technology, a technique that utilises ultrasound energy to remove fat.
Surgical Options Explained
There is no single approach to brachioplasty that suits every patient. The type of arm lift (brachioplasty) procedure recommended depends on the amount of skin and fat, the distribution of excess tissue, and overall health.
Liposuction (suction-assisted lipectomy)
Liposuction can remove excess fat, but does not treat lax skin. In post-weight-loss patients, liposuction alone may worsen loose skin by removing underlying support while leaving stretched skin behind. For this reason, liposuction is rarely used as a standalone solution in men after massive weight loss and is more commonly used as an adjunct to excisional surgery.
Pedicled Nipple Techniques
Pedicled techniques aim to preserve nipple sensation by keeping the nipple–areola complex attached to the underlying tissue. While this may be appropriate in selected patients with mild skin excess, these techniques often leave excess tissue and bulk in post-weight-loss men. In Dr Beldholm’s experience, pedicled techniques frequently produce a rounded or breast-like appearance and may fail to adequately correct significant ptosis or loose skin.
Chest Lipectomy With Free Nipple Grafting
For most patients with significant weight loss, Dr Beldholm recommends chest lipectomy (male mastectomy) with free nipple–areola grafts. This surgical excision removes excess skin and fat, repositions the nipple, and creates a flatter chest with a horizontal scar placed along the lower border of the pectoralis major muscle.
This approach prioritises chest shape, long-term durability, and a masculine contour over nipple sensation, which is often already reduced in this patient group.
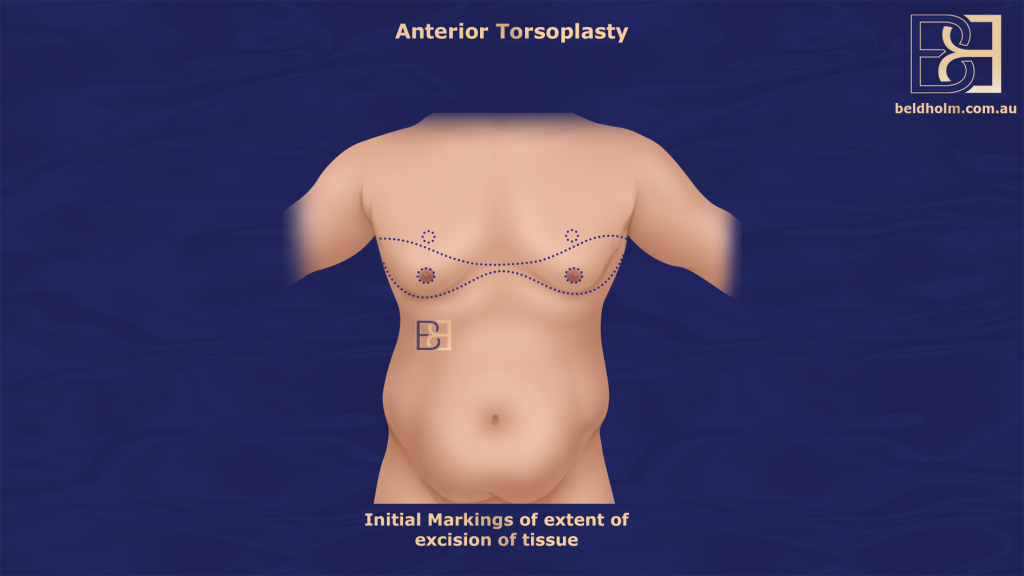
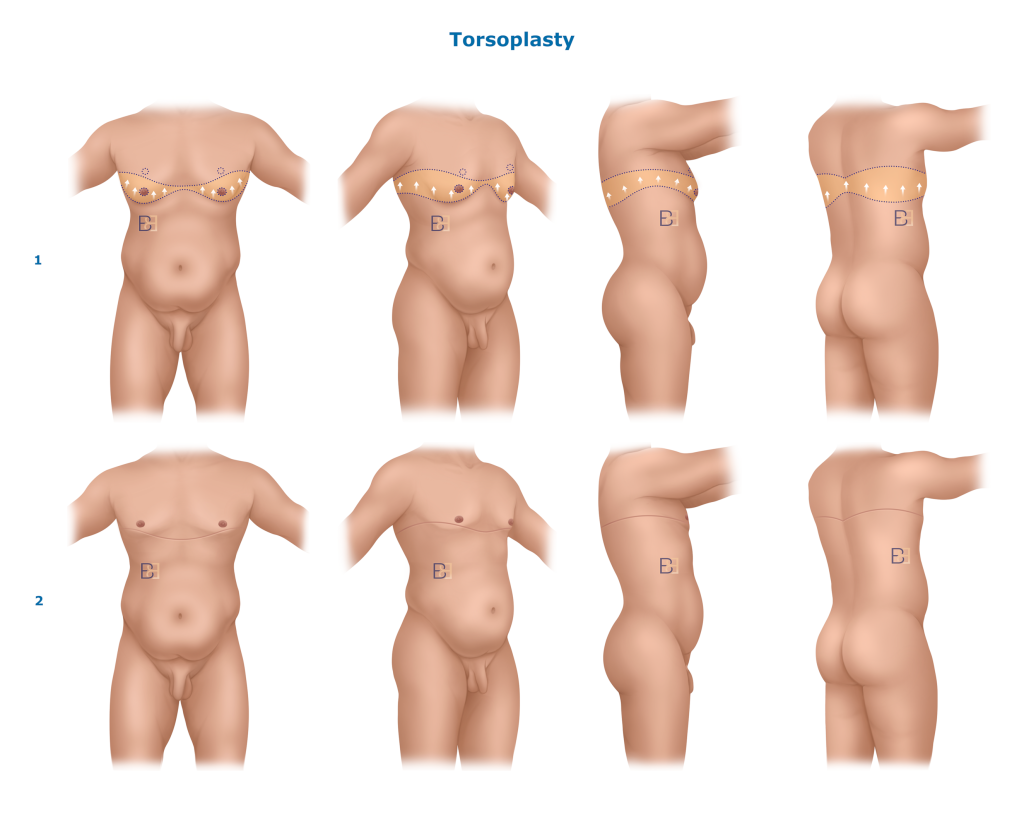
Anterior Torsoplasty (Anterior chest lipectomy, or male mastectomy)
Anterior torsoplasty treats excess skin and fat across the entire front of the upper torso. In addition to the chest itself, this technique targets loose skin extending toward the upper abdomen and lateral chest wall. By removing a wide segment of redundant skin, this approach helps create a flatter, tighter upper body contour while maintaining scars in anatomically appropriate locations.
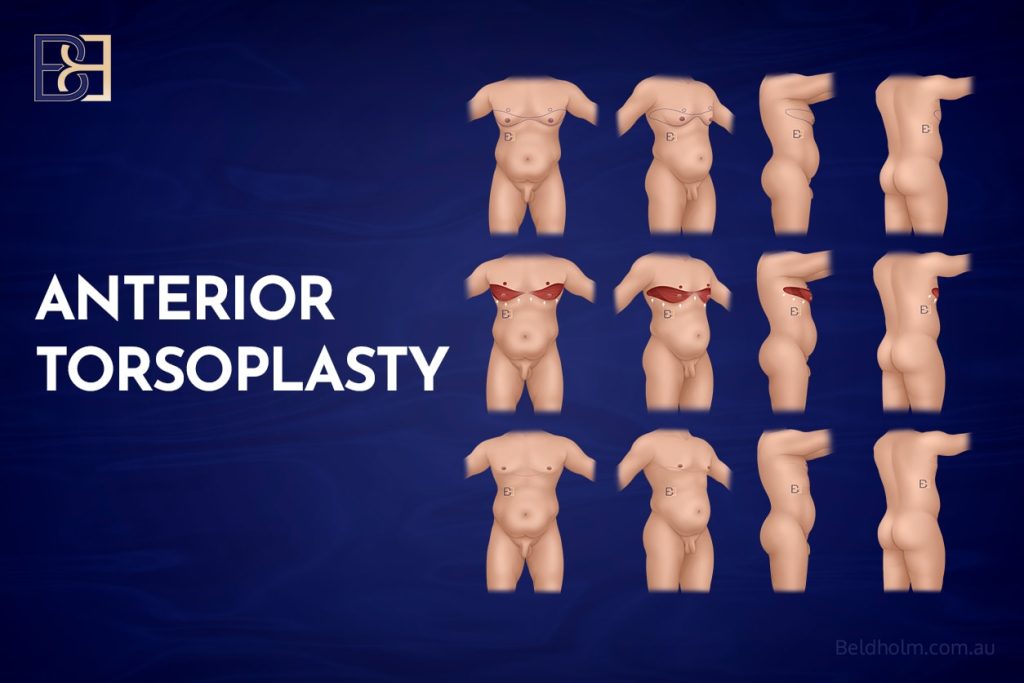
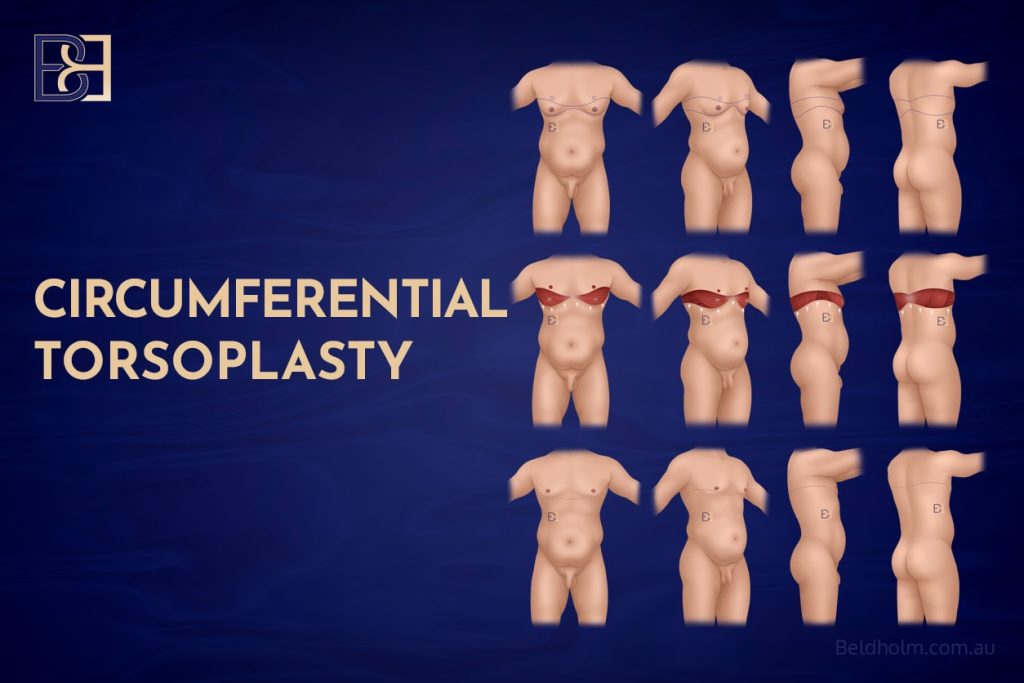
Circumferential Torsoplasty
Circumferential torsoplasty is a more extensive surgical option designed for men with widespread loose skin involving the chest, sides of the torso, and upper back. In these patients, treating the anterior chest alone can leave residual laxity and imbalance.
Circumferential torsoplasty involves excision of excess skin and fat around the entire upper torso, often combined with chest lipectomy, upper back lift, and underarm tightening. This approach is commonly recommended for patients classified as Grade BB 4c, in whom skin laxity is severe and circumferentially distributed. The goal is to achieve a balanced, masculine contour of the entire upper body rather than focusing on the anterior chest in isolation.
Book your appointment online now
The Surgical Procedure and Hospital Stay
Upper body lift surgery (upper torsoplasty) requires general anaesthesia and typically involves a hospital stay of one to two nights. The procedure involves making incisions either on the anterior chest for an anterior torsoplasty or extending along the chest and back from the sides to the midline of the back for a circumferential torsoplasty. This approach allows for the comprehensive removal of excess skin and tissue. Surgery duration generally ranges from three to six hours, depending on the complexity and number of combined procedures. During the operation, the patient is repositioned to provide the surgeon with optimal access to both the anterior and posterior aspects of the upper body.
Recovery and Healing Process After Upper and Circumferential Torsoplasty Surgery with Dr Bernard Beldholm
The recovery process following upper torsoplasty surgery is carefully managed by Dr Bernard Beldholm to optimise healing. Here’s an outline of the recovery routine under his expert care:

In-Hospital Care
Patients typically stay in the hospital for 1 to 2 days after surgery. During this time, Dr Beldholm and his team closely monitor the patient’s recovery, providing pain medication and antibiotics to manage discomfort and prevent infection. Drains are placed to manage fluid buildup and are typically removed during a follow-up visit one or two days later.
The First Two Weeks: An Intense Recovery Period

The first two weeks are crucial, and patients are seen frequently during this period. Follow-up visits with Dr Beldholm and his dedicated nurse are scheduled to ensure everything is healing as expected. During this time, patients should have the opportunity to communicate directly with Dr Beldholm’s office, and any questions can be answered promptly.
For patients travelling from outside the area, it’s essential to remain near the surgical centre for at least 10 days for proper care and allow for the NAC grafts to be managed. Ideally, patients should stay for two weeks. Dr Beldholm works closely with local GPs for travelling patients, and Zoom consultations can be arranged to ensure continuous monitoring and support.
Dr Beldholm uses specialised dressings and devices to optimise recovery:

- Healite Therapy: Dr Beldholm uses Healite, a therapeutic light device for healing and reduce inflammation during the early stages of recovery.
- PICO Dressings: These are applied to support incision healing and reduce swelling. They are removed on day 7 following surgery.
- Nipple-Areolar Complex (NAC) Grafts: A pressure dressing with clips is applied to support the NAC grafts and maintain their position. This pressure dressing is typically removed on day 10.
Ongoing Follow-Up
After the initial two weeks, the routine follow-up schedule is as follows:
- 1 month
- 3 months
- 6 months
- 12 months
During these follow-up visits, Dr. Beldholm can monitor the healing process and confirm that the patient is progressing well toward optimal outcomes.
Important Considerations

During the first month, patients are required to wear a compression garment continuously to support healing and reduce swelling. Dr Beldholm carefully monitors patients during follow-ups to ensure there are no complications and that the recovery is progressing well.
Patients are also advised to avoid strenuous physical activity and heavy lifting for 6-8 weeks to prevent complications, such as delayed wound healing or seroma formation.
Potential Risks and Complications of Upper and Circumferential Torsoplasty
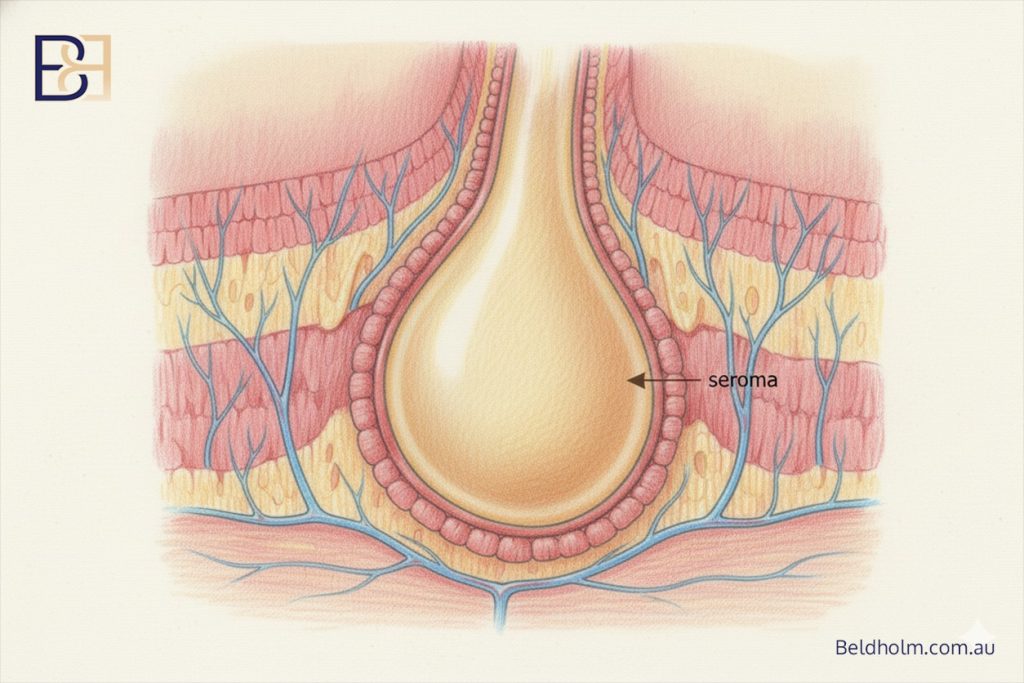
Upper and Circumferential Torsoplasty surgery, like any surgical procedure, carries significant risks and complications that may arise during or after surgery. These can include infection, scarring, blood clots, wound healing issues, and seroma formation (accumulation of fluid under the skin). Patients should monitor their bodies for signs of complications and seek medical advice if any concerns arise. see below link to more comprehensive article about complications from torsoplasty.
Dr Beldholm’s Final Thoughts on Upper and Circumferential Torsoplasty Surgery

Upper and circumferential torsoplasty may be an appropriate surgical option for selected patients who have experienced significant weight loss and continue to have excess skin and residual adipose tissue affecting the upper torso. In these individuals, the procedure is primarily considered to treat ongoing physical and functional concerns rather than cosmetic change alone.
In male patients, upper and circumferential torsoplasty can form part of a broader surgical strategy to manage redundant tissue involving the chest, upper abdomen, lateral chest wall, back, and flanks. Following major weight loss, conditions such as gynaecomastia or pseudogynecomastia are commonly encountered and require careful clinical assessment. Classification systems may help guide treatment planning based on the type, distribution, and severity of the remaining tissue.
This procedure is typically considered when excess skin extends beyond the anterior chest and involves multiple regions of the upper torso. Where clinically appropriate, suction-assisted liposuction techniques, including technologies such as VASER (vibration amplification of sound energy at resonance), may be used selectively to assist with fat reduction. In patients with significant skin laxity, liposuction (suction-assisted lipectomy) alone is usually insufficient and is therefore combined with excisional techniques.
The clinical indications for upper and circumferential torsoplasty often relate to functional issues. Patients may experience recurrent skin irritation, hygiene difficulties, discomfort, or limitations in movement due to excess skin folds. In these cases, surgical intervention aims to reduce these concerns. As with all body contouring procedures, outcomes vary between individuals and should be discussed in detail during consultation, including potential risks, scarring, recovery expectations, and alternative treatment options.
References
- Gusenoff JA, Coon D, Rubin JP. Pseudogynaecomastia after massive weight loss. Plast Reconstr Surg. 2008;122(5):1301–1308.
- Ziegler UE, Lorenz U, Daigeler A, et al. Modified treatment algorithm for pseudogynaecomastia. Ann Plast Surg. 2018;81(3):290–294.
- Stoff A, Velasco-Laguardia FJ, Richter DF. Central pedicled breast reduction technique in male patients after massive weight loss. Obes Surg. 2012;22:445–451.
- Rohrich RJ, Ha RY, Kenkel JM, Adams WP. Classification and management of gynaecomastia. Plast Reconstr Surg. 2003;111(2):909–923.
- Hurwitz DJ. Boomerang upper body lift after massive weight loss. Plast Reconstr Surg. 2004;114(7):1674–1683.


