Fleur-de-Lis Abdominoplasty for Excess Skin After Massive Weight Loss
Significant weight loss — whether achieved through bariatric surgery or sustained lifestyle change — can result in excess abdominal skin that does not retract.
Many patients describe:
- Hanging or folded skin in the lower abdomen
- Loose skin that gathers and bunches in the center of the abdomen
- Persistent skin redundancy despite stable weight
- Hygiene difficulties beneath skin folds
- Discomfort with movement or exercise
In some individuals, the pattern of skin laxity is both vertical and horizontal. In these cases, a standard tummy tuck (abdominoplasty) may not adequately address the degree of central abdominal excess.
A Fleur-de-Lis abdominoplasty is a surgical procedure designed to remove excess skin in two directions. It is typically considered in patients who have experienced massive weight loss and have complex abdominal laxity.
This procedure is performed in hospital under general anaesthesia and requires comprehensive assessment prior to surgery.
Who This Procedure Is Designed For
A Fleur-de-Lis abdominoplasty may be considered for patients who:
- Have lost a substantial amount of weight
- Have maintained a stable weight for an appropriate period
- Have excess skin both above and below the umbilicus
- Have both vertical and horizontal excess abdominal skin
- Have skin folds causing irritation or hygiene concerns
- Are medically fit for major surgery
This operation is generally not appropriate for:
- Patients seeking minor contour refinement
- Patients whose primary concern is localised fat rather than excess skin
- Individuals planning further significant weight loss
Selection of the appropriate procedure depends on the pattern of skin redundancy, abdominal wall integrity, and overall health status.
As a Specialist General Surgeon with over 15 years of experience in post-weight-loss body contouring, Dr Bernard Beldholm assesses each patient individually to determine whether a Fleur-de-Lis procedure — or an alternative approach — is most appropriate.
What Is a Fleur-de-Lis Abdominoplasty?
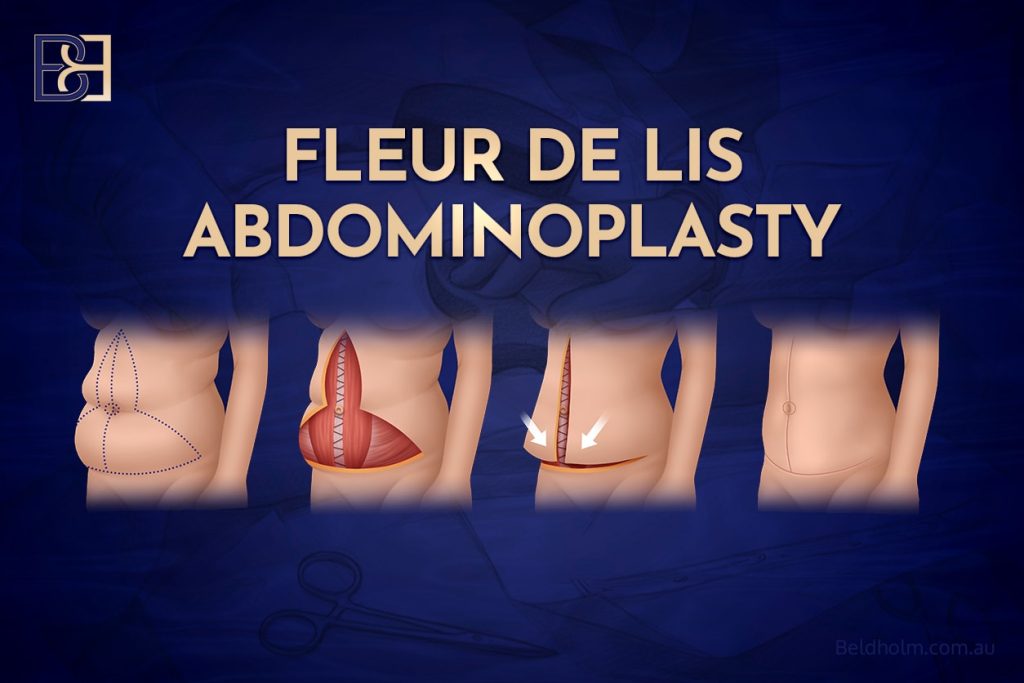
A Fleur-de-Lis abdominoplasty is an extended form of abdominal skin removal designed to address both horizontal and vertical excess skin.
Unlike a standard abdominoplasty, which removes excess tissue primarily from the lower abdomen using a horizontal incision, a Fleur-de-Lis procedure involves:
- A horizontal lower abdominal incision (similar to a standard tummy tuck)
- An additional vertical midline incision
- Removal of excess skin in two directions
- Repositioning of the umbilicus (belly button)
- Repair of the abdominal wall if indicated
The vertical component allows removal of horizontal excess skin of the central abdomen that cannot be adequately tightened with a horizontal excision alone.
This pattern of excision is most commonly required in patients following massive weight loss, where the abdominal skin envelope has stretched and then deflated, leaving redundancy in more than one direction.
The procedure is performed in hospital under general anaesthesia. The extent of skin removal, abdominal wall repair, and any additional procedures are determined following detailed clinical assessment.
How a Fleur-de-Lis Differs from a Standard Abdominoplasty
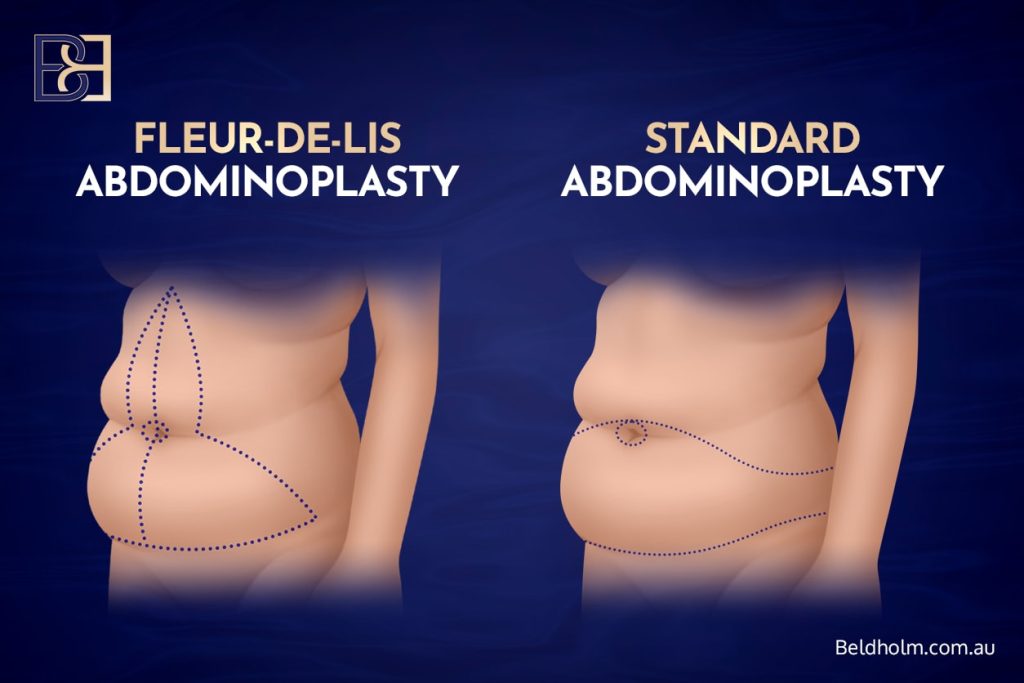
A standard abdominoplasty is designed primarily to treat vertical excess skin of the abdomen. Through a low transverse incision, excess lower abdominal skin is removed and the remaining tissue is tightened downward. This approach is appropriate when skin redundancy is mainly in a vertical direction, even if it extends above and below the umbilicus.
Both a standard abdominoplasty and a Fleur-de-Lis procedure typically include trimming and lifting of the mons pubis area. After significant weight loss, the mons region often becomes lax or descends. Elevation and reduction of this area may be performed as part of abdominal contour surgery to restore proportion and reduce overhang.
However, after massive weight loss, many patients develop excess skin in two dimensions:
- Vertical excess (skin that hangs downward)
- Horizontal excess (skin that is excessive across the width of the abdomen)
A standard tummy tuck (abdominoplasty) can effectively address vertical excess, including improvement of the lower abdomen and mons region, but it does not directly remove significant horizontal redundancy. When horizontal excess is present, tightening in a downward direction alone may leave residual central bunching or persistent width of the abdominal skin envelope.
A Fleur-de-Lis abdominoplasty adds a vertical midline excision to the standard transverse incision. This allows removal of both vertical and horizontal excess skin, reducing abdominal width as well as length, while also addressing the lower abdominal and mons laxity.
Selection between these procedures depends on the pattern of skin redundancy, abdominal wall integrity, scar tolerance, and overall medical suitability. A detailed clinical examination is required to determine the most appropriate surgical approach.
Limitations of a Fleur-de-Lis Abdominoplasty
While a Fleur-de-Lis abdominoplasty can address both vertical and horizontal excess skin of the abdomen, it does not correct all patterns of post-weight-loss tissue laxity.
Understanding these limitations is important when selecting the most appropriate procedure.
Upper Abdomen and Lower Chest Laxity
A Fleur-de-Lis procedure primarily reshapes the central abdomen. It may not adequately tighten significant excess skin of the upper abdomen near the lower ribs or the lower chest region.
In patients with pronounced upper abdominal redundancy, tightening in both vertical and horizontal directions may still leave residual laxity higher on the torso. In selected cases, an alternative approach such as a dual vector abdominoplasty may be considered following clinical assessment.
Flanks and Lower Back
A Fleur-de-Lis abdominoplasty is an anterior abdominal procedure. It does not directly address excess skin of the flanks, lateral torso, or lower back.
Where tissue redundancy extends circumferentially around the body — which is common after massive weight loss — a circumferential approach such as a belt lipectomy or hybrid body lift (circumferential hybrid abdominopalsty) may be more appropriate.
Scar Considerations
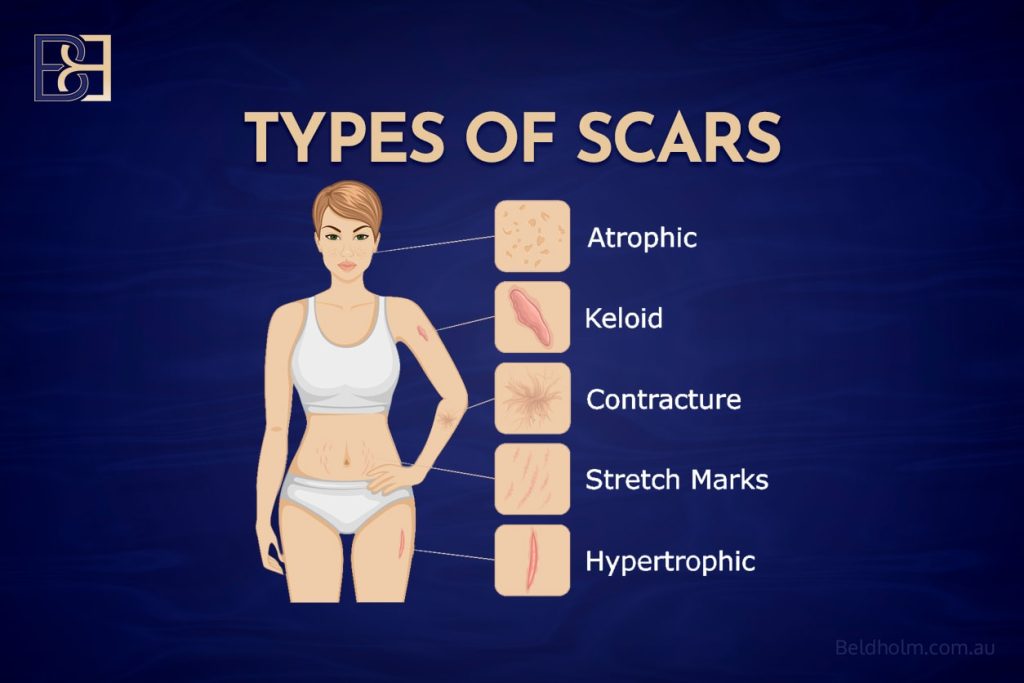
A Fleur-de-Lis procedure results in both a horizontal lower abdominal scar and a vertical midline scar. The vertical scar is permanent and visible on the central abdomen. Patients must weigh the trade-off between improved contour and the presence of additional scarring.
Procedure selection is based on anatomical pattern, skin quality, medical fitness, and patient priorities. A detailed consultation is required to determine whether a Fleur-de-Lis procedure or an alternative approach is more suitable.
What May Be Addressed During the Same Operation
In addition to removal of excess skin, a Fleur-de-Lis abdominoplasty may involve treatment of the underlying abdominal wall and surrounding tissues. The exact components of surgery are determined following clinical assessment.
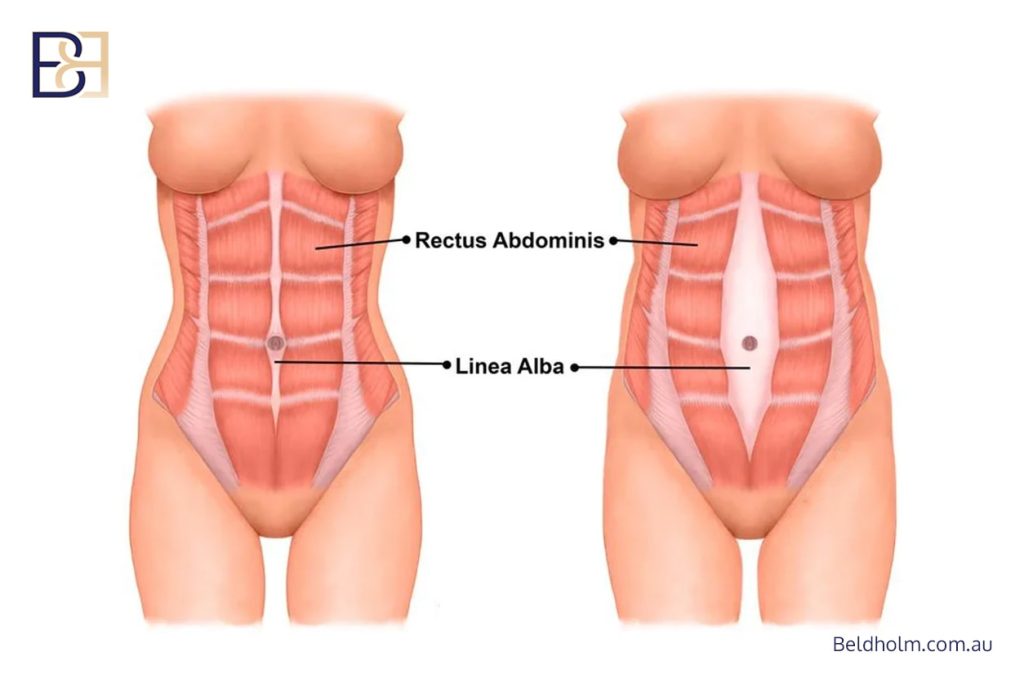
Repair of Diastasis Recti
Following pregnancy or significant weight change, separation of the rectus muscles (diastasis recti) may be present. This can contribute to abdominal wall weakness, bulging, and reduced core support.
Where appropriate, rectus muscle repair (plication) may be performed at the time of surgery to restore midline support and improve abdominal wall contour.
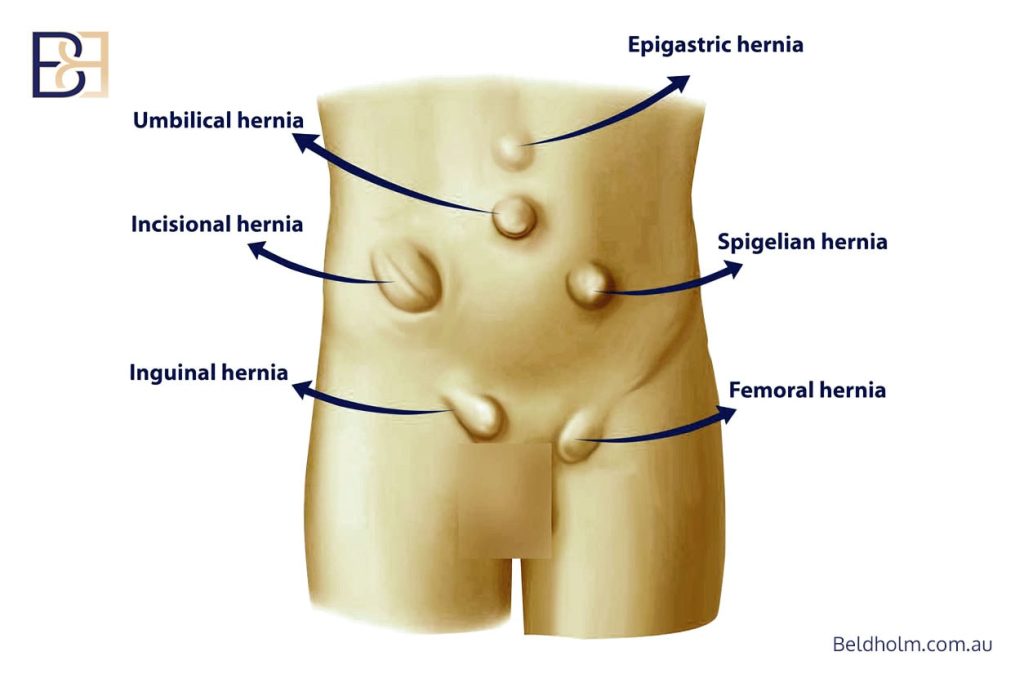
Book Online NowHernia Assessment and Repair
Post-weight-loss patients may have umbilical, ventral, or incisional hernias. These may be identified during examination or imaging.
Where a hernia is present, repair may be performed at the same operation. Depending on the size and location of the defect, mesh reinforcement may be required.
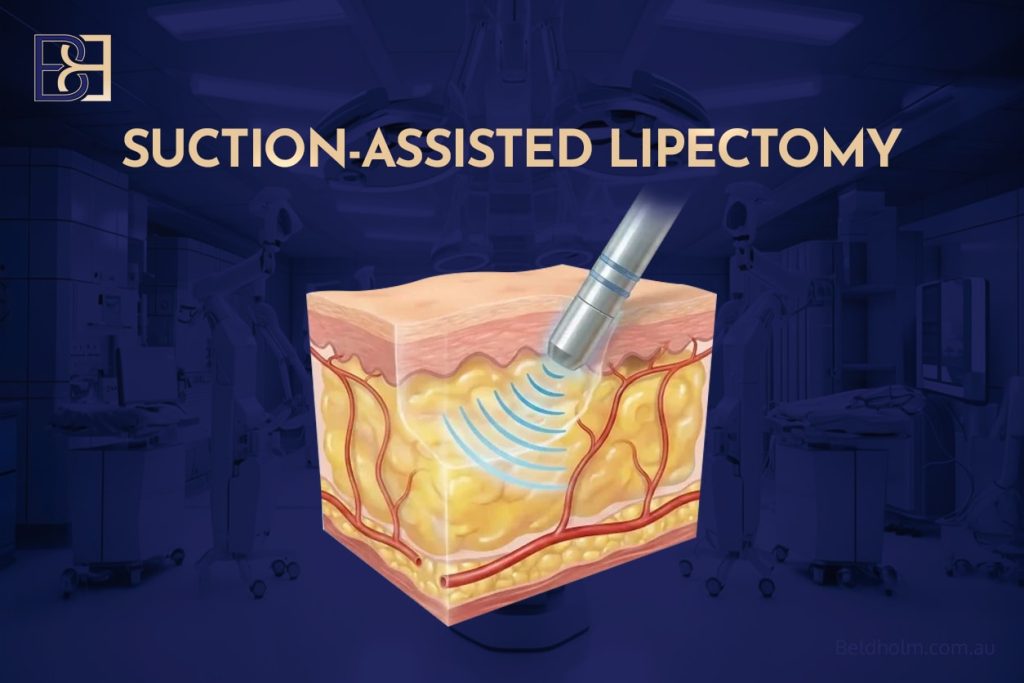
Selective Liposuction (suction assisted lipectomy)
In selected cases, liposuction (suction-assisted lipectomy) may be performed to improve contour transition zones or reduce residual fat deposits. Liposuction (suction-assisted lipectomy) does not remove excess skin and is not a substitute for excisional surgery.
The decision to include liposuction (suction-assisted lipectomy) is based on tissue thickness, vascular safety, and overall operative planning.
Risks and Potential Complications
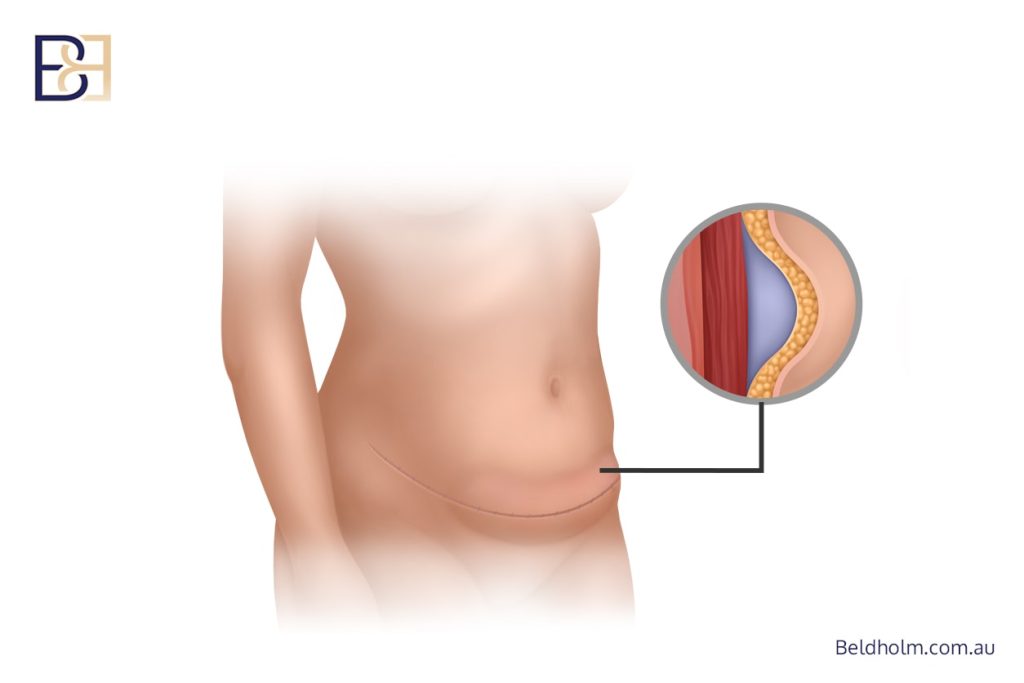
A Fleur-de-Lis abdominoplasty is a major surgical procedure performed under general anaesthesia. As with all surgery, risks are present and must be carefully considered.
Potential complications include:
- Bleeding or haematoma
- Infection
- Seroma (fluid collection)
- Delayed wound healing
- Wound separation
- Prominent or unfavourable scarring
- Skin or fat necrosis
- Altered sensation of the abdominal wall
- Venous thromboembolism (blood clots)
- Anaesthetic risks
Patients who have undergone massive weight loss may have higher rates of wound healing complications due to skin quality, nutritional factors, and previous medical history.
The presence of a vertical midline incision increases the overall scar burden and may increase the risk of delayed healing along the central closure line.
Careful pre-operative assessment, optimisation of medical conditions, smoking cessation, and appropriate post-operative care are important in reducing surgical risk.
All risks, alternatives, and expected recovery considerations are discussed in detail during consultation prior to proceeding with surgery.
Recovery After Fleur-de-Lis Abdominoplasty

Recovery following a Fleur-de-Lis abdominoplasty depends on the extent of skin removal, whether diastasis repair or hernia repair is performed, and individual healing factors.
Dr Bernard Beldholm performs this procedure at Maitland Private Hospital under general anaesthesia.
Hospital Stay at Maitland Private Hospital
Patients are typically admitted on the day of surgery. Most patients stay 2–4 days in hospital, depending on surgical complexity, pain control, mobility, and medical status.
During the inpatient stay:
- Surgical drains are routinely used to reduce fluid accumulation
- Intravenous fluids and antibiotics are administered as required
- Early assisted mobilisation is encouraged
- Compression garments are fitted
Patients are discharged once pain is controlled, mobility is safe, and drain output is appropriate.
First Two Weeks After Surgery

In the early recovery phase, patients can expect:
- Abdominal tightness and swelling
- Bruising
- Temporary numbness of the abdominal wall
- A slightly flexed walking posture initially
Drains remain in place until output reduces to an appropriate level. Dr Beldholm generally considers removal once drainage is less than 20 mL over a 24-hour period. Timing varies between patients and depends on overall fluid production and wound healing.
Compression garments are worn full-time for approximately 4 weeks following surgery. After this period, they are typically continued for a further 2 weeks on a part-time basis. Garments support the abdominal wall, reduce swelling, and assist with contour stabilisation during early healing.
Activity Restrictions

Light walking is encouraged from the early post-operative period to reduce the risk of venous thromboembolism.
However:
- Heavy lifting is restricted for approximately 6 weeks
- Core strengthening and strenuous exercise are avoided during early healing
- Driving is resumed once patients are comfortable and no longer taking strong analgesia
Return to work depends on the occupation. Sedentary roles may resume earlier than physically demanding work.
Follow-Up Schedule

Post-operative follow-up is conducted through Dr Beldholm’s rooms. Patients are reviewed regularly to:
- Monitor wound healing
- Remove drains when appropriate
- Assess for early complications
- Provide scar management guidance
Long-term follow-up allows monitoring of scar maturation and abdominal wall integrity.
Scar Maturation
Both the horizontal lower abdominal scar and the vertical midline scar are permanent. Initially, scars may appear firm, raised, and red. Over time, they typically soften and fade, although visibility varies between individuals.
Individual recovery timelines vary. Detailed written post-operative instructions are provided prior to discharge from Maitland Private Hospital.
Consultation and Surgical Planning
A Fleur-de-Lis abdominoplasty is major surgery and requires comprehensive assessment before proceeding.
Referral and Initial Assessment
A valid GP referral is required to arrange consultation.
During the consultation, Dr Bernard Beldholm — Specialist General Surgeon — conducts a detailed assessment including:
- Review of weight loss history (including bariatric surgery if applicable)
- Confirmation of weight stability
- Assessment of skin pattern (vertical and horizontal excess)
- Examination of the abdominal wall for diastasis or hernia
- Review of medical history, medications, and previous operations
Nutritional status, smoking history, and overall medical fitness are carefully evaluated, particularly in post-bariatric patients.
Determining the Appropriate Procedure
Not all patients with excess skin require a Fleur-de-Lis procedure. Surgical planning is based on:
- The direction and degree of skin redundancy
- Presence of circumferential laxity
- Upper abdominal involvement
- Abdominal wall integrity
- Scar tolerance
Where appropriate, alternative procedures such as a standard abdominoplasty, dual vector abdominoplasty, or circumferential body lift may be discussed.
Informed Consent and Risk Discussion

All potential risks, benefits, limitations, and alternatives are discussed in detail prior to surgery. Patients are encouraged to seek a second opinion before proceeding.
A clear understanding of expected scarring, recovery time, and complication risk is essential before making a decision.
Pre-Operative Preparation

Prior to surgery, patients may be required to:
- Maintain a stable weight
- Cease smoking
- Optimise medical conditions
- Complete relevant investigations
Surgery is scheduled at Maitland Private Hospital once all pre-operative requirements have been satisfied.
Each operative plan is individualised. The goal is to select the most appropriate procedure based on anatomical findings and overall patient safety.




