Gynaecomastia (Male Breast Reduction) Surgery with Dr Bernard Beldholm
A Specialist Surgeon assessment for men with enlarged breast tissue, drawing on a grading and treatment framework developed over 15+ years of clinical practice.
For most men in BB Grades 1 to 3, gynaecomastia surgery is performed as a day procedure at Maitland Private Hospital. The right operation depends on whether the enlargement is glandular, fatty, or both, and on whether there is associated skin laxity. Each patient is assessed individually at consultation, and a GP referral is required before booking.
Results vary. All surgery carries risks. Consultation required to determine suitability.
My Approach to Gynaecomastia Surgery
Over more than 15 years treating men with enlarged breast tissue, I work to four clinical principles.
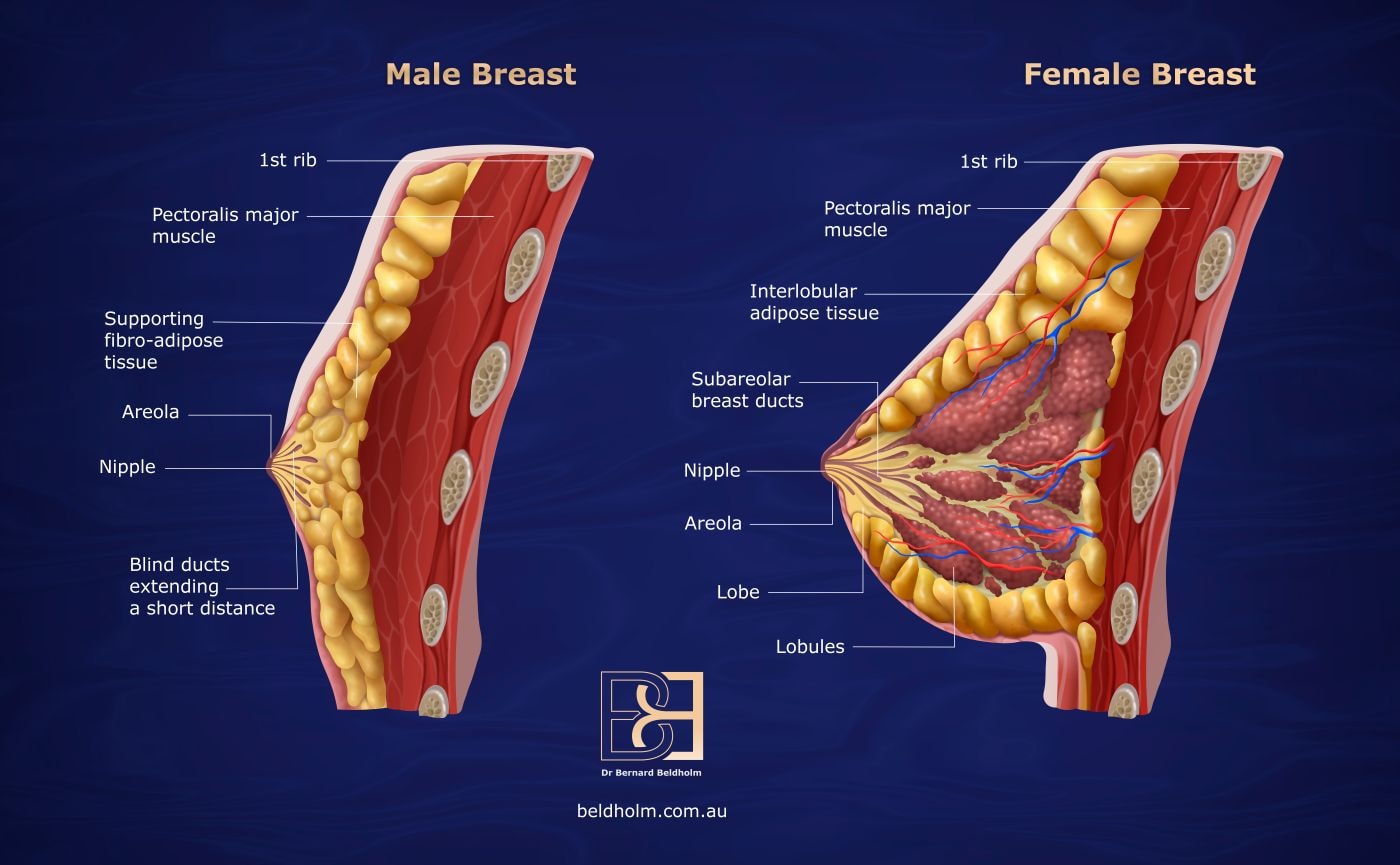
1. Distinguish real gynaecomastia from pseudo-gynaecomastia
The two conditions can look similar from the outside but require different operations. Real gynaecomastia involves firm glandular tissue that does not respond to weight loss or exercise. Treatment requires surgical removal of the gland through subcutaneous mastectomy, on its own for smaller cases and commonly combined with VASER liposuction where fat is also present. Pseudo-gynaecomastia is fatty tissue alone, without glandular enlargement, and may be addressed with VASER liposuction on its own. Telling the two apart is the first step at consultation.
2. Match the operation to the presentation
The procedure depends on what is found at examination: the type of enlargement (glandular, fatty, or both) and the presence of any associated skin laxity. To make this decision systematic, I developed the Beldholm 2024 Gynaecomastia Grading System, which sets out eight grades from BB 1 through BB 4c with a recommended operation for each. The principle is straightforward: the procedure follows the pattern, not the reverse.
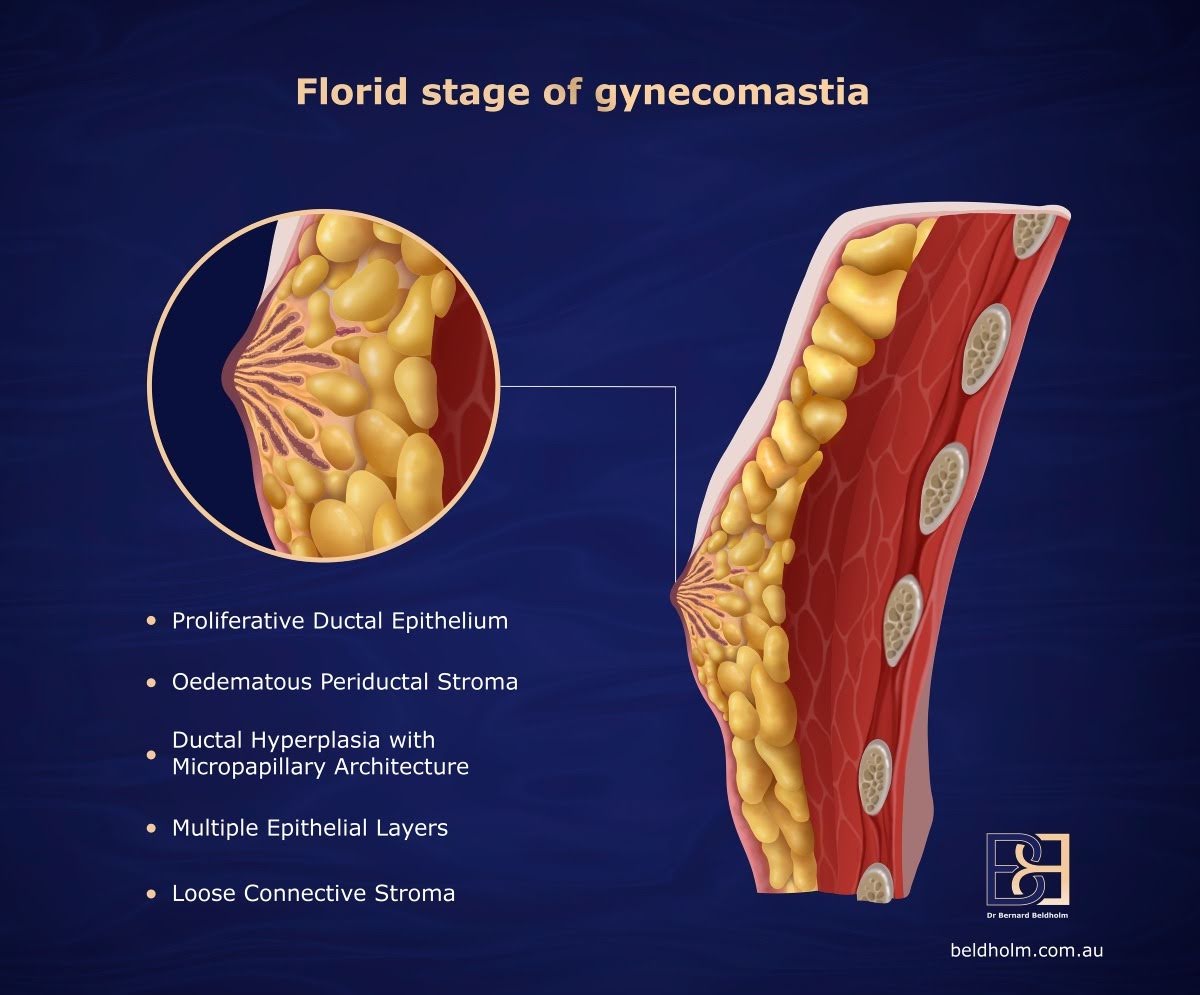
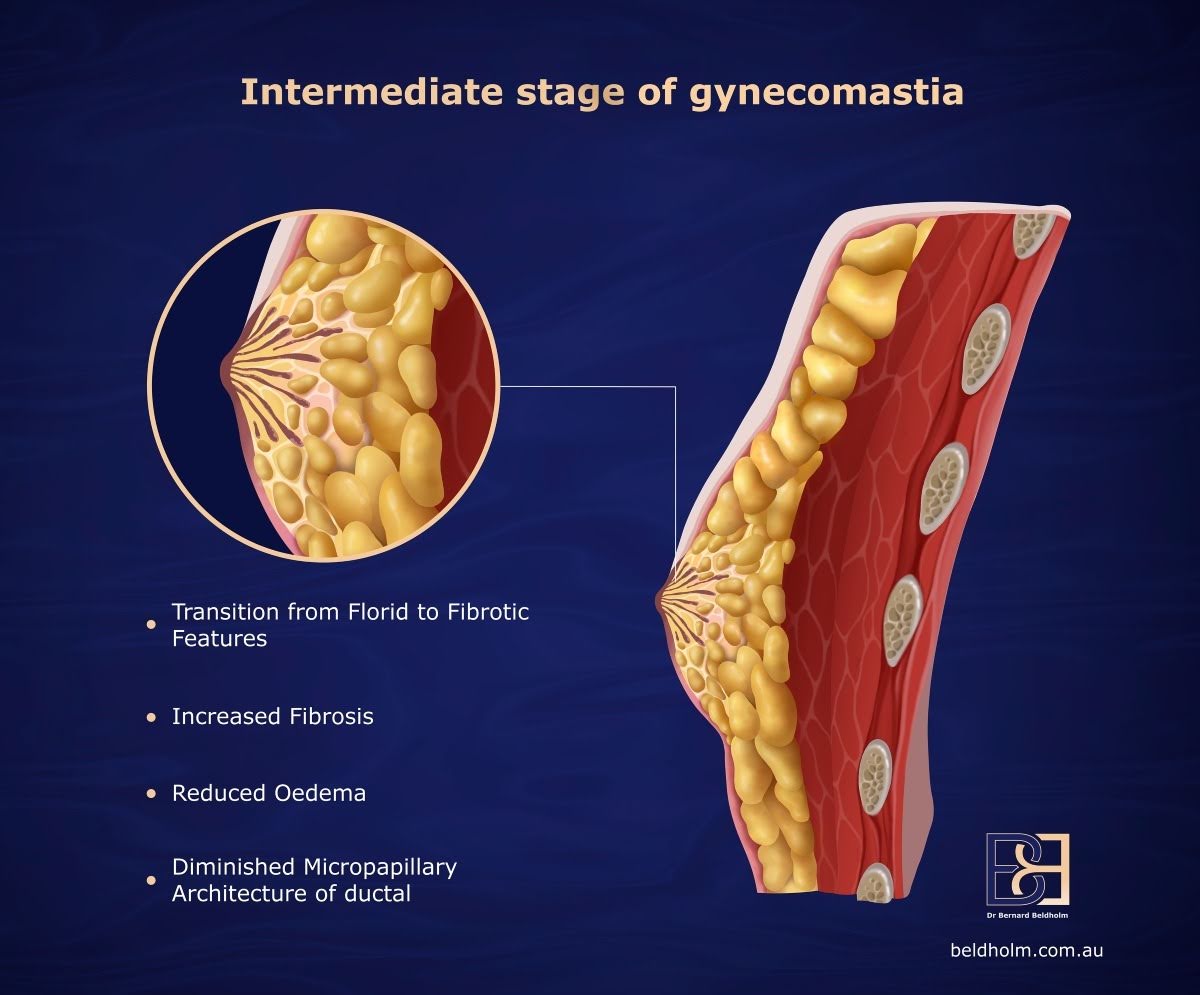
3. One operation where possible
For most men in BB Grades 1 to 3, surgery is performed as a day procedure under general anaesthetic. A combined approach addresses both glandular and fatty components in a single operation where indicated, using gland excision and VASER suction-assisted lipectomy together.
4. VASER suction-assisted lipectomy as adjunct
VASER uses ultrasonic energy to break down fat before it is suctioned out, with the aim of targeted removal while minimising trauma to surrounding tissues. When fat forms part of the presentation, VASER is used as an adjunct to gland excision. When the presentation is purely fatty (pseudo-gynaecomastia), it is the standalone operation.
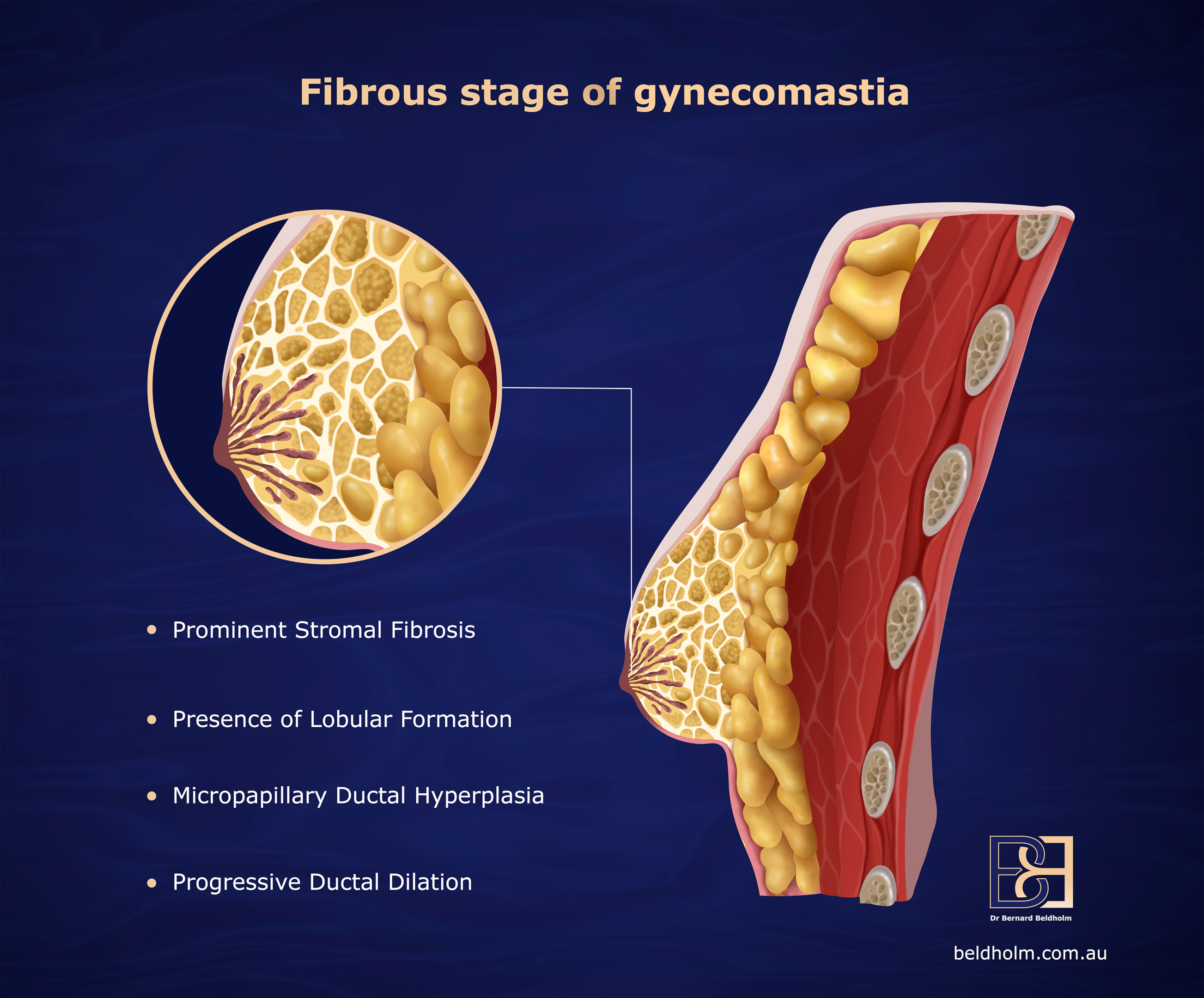
Two Questions to Consider Before Booking a Consultation
Gynaecomastia surgery is a personal decision and there is no rush to proceed before you feel ready. The two questions below can help you think through where you are in that decision.
Is this real gynaecomastia, or pseudo-gynaecomastia?
The two conditions can look the same to the patient but are addressed by different operations. Real gynaecomastia involves firm, rubbery glandular tissue beneath the nipple. It will not respond to weight loss, exercise, or supplements. Pseudo-gynaecomastia is fatty tissue alone, and will sometimes reduce with sustained weight loss.
Distinguishing the two requires a clinical examination. The GP is the appropriate first step and can usually make the distinction during a physical examination. An ultrasound may be requested if there is uncertainty. Patients who have already lost weight without seeing a meaningful change in their chest are likely to have a glandular component that surgery is needed to address.
Is now the right time for surgery?
Three factors are worth considering before scheduling a consultation.
Weight stability. Gynaecomastia surgery is performed once patient weight is stable. Significant weight loss after surgery can leave residual skin laxity that may then require a second operation. If active weight loss is still underway, deferring surgery until weight has been stable for at least six months is generally advised.
Active anabolic steroid use. Anabolic steroids and certain medications can cause or worsen gynaecomastia. Patients who are still using these substances are usually advised to stop, as continued use after surgery can lead to recurrence of the condition. The duration of cessation before surgery is discussed at consultation.
Age. Gynaecomastia during adolescence often resolves on its own as the hormonal changes of puberty settle. For adult men, gynaecomastia that has been present for years rarely resolves without surgical treatment. Surgery is generally considered only once the condition has been stable for at least 12 months and conservative measures have not produced sufficient change.
If any of the above factors apply, the appropriate next step is usually a discussion with your GP. Where surgery is the right pathway, a referral can then be made.
Matching the Operation to the Presentation
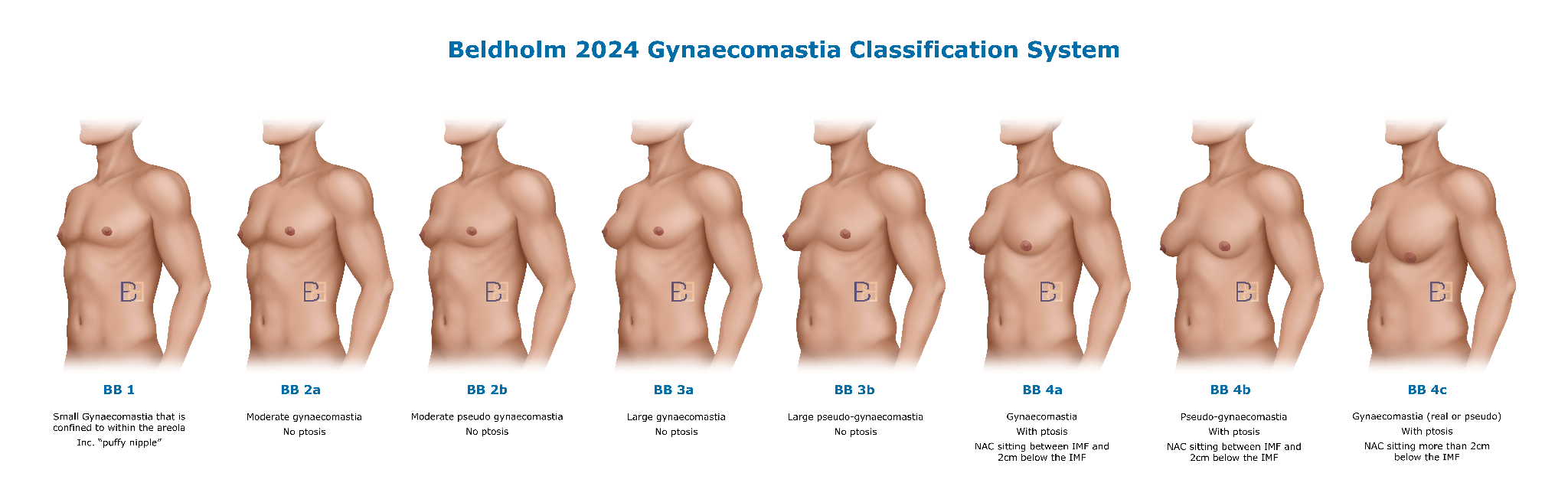
Three things determine which operation is appropriate: whether the enlargement is glandular, fatty, or both; the volume of tissue involved; and whether there is associated skin laxity.
A few terms used below:
- Subcutaneous mastectomy: surgical removal of the glandular breast tissue under the nipple
- VASER suction-assisted lipectomy: liposuction performed using ultrasonic energy to break down fat before it is suctioned out
- Infra-areolar incision: a small scar placed within the lower border of the areola
- Supra-areolar incision: an incision at the upper border of the areola, where the pigmented areolar skin meets normal skin, used in larger cases where additional skin needs to be removed
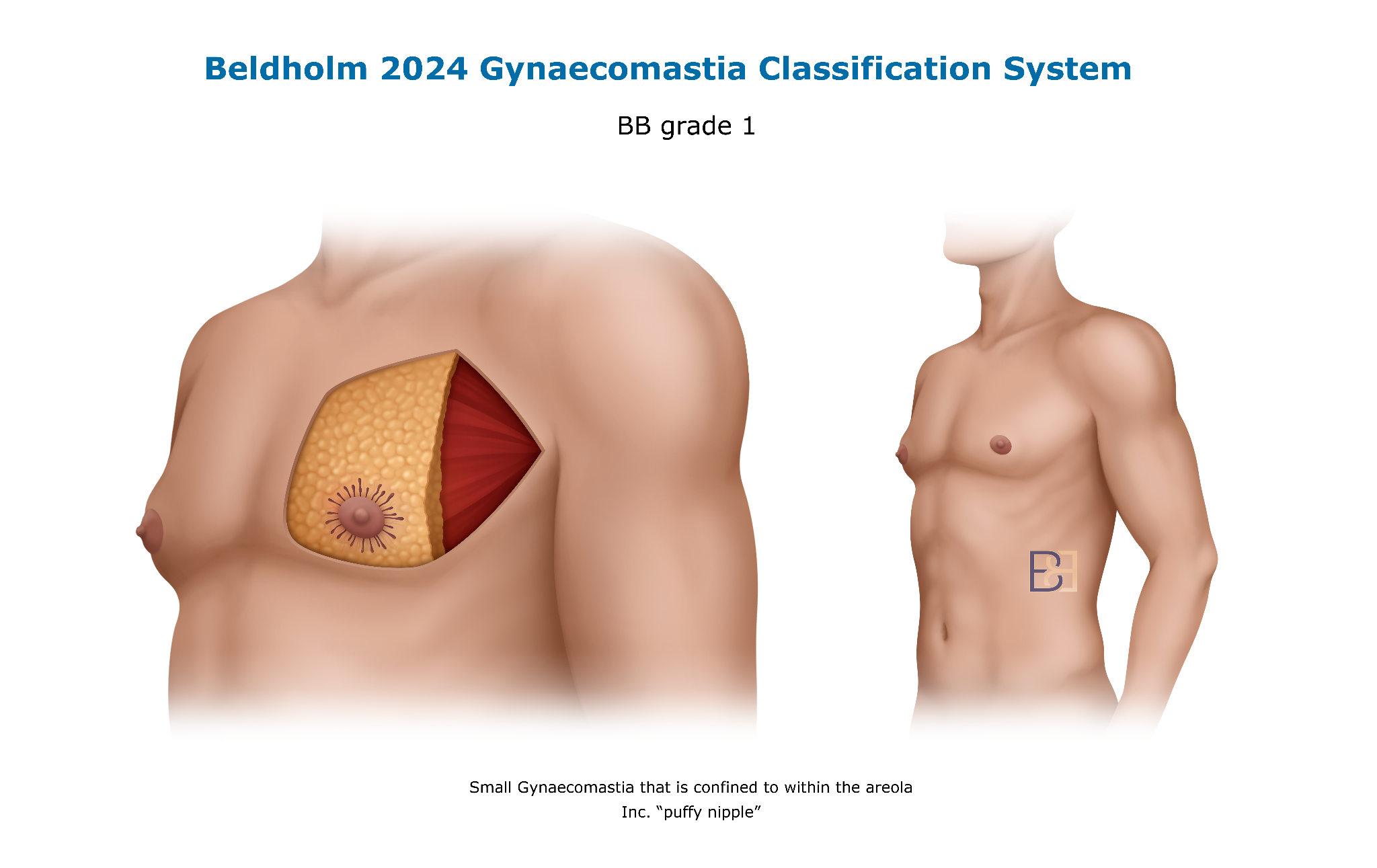
Pattern A: Firm tissue confined to the areola
This presentation involves a small area of firm, palpable tissue confined within the area of the areola, with little to no surrounding fat. The cause is glandular enlargement.
Operation: Subcutaneous mastectomy through an infra-areolar incision. The scar sits within the lower border of the areola.
This pattern corresponds to BB Grade 1 in the Beldholm 2024 framework.
Pattern B: Soft, fatty enlargement (pseudo-gynaecomastia)
The chest feels soft to the touch, without a firm gland under the nipple. The volume comes from fatty tissue rather than glandular tissue. The condition is sometimes referred to as pseudo-gynaecomastia.
Operation: VASER suction-assisted lipectomy. The fat is broken down using ultrasonic energy and removed through small access incisions. There is no need for gland excision because no gland is involved.
For larger presentations where the skin has stretched, a small excision of skin above the areola may also be performed in the same operation to address skin redundancy. This pattern spans BB Grades 2b and 3b.
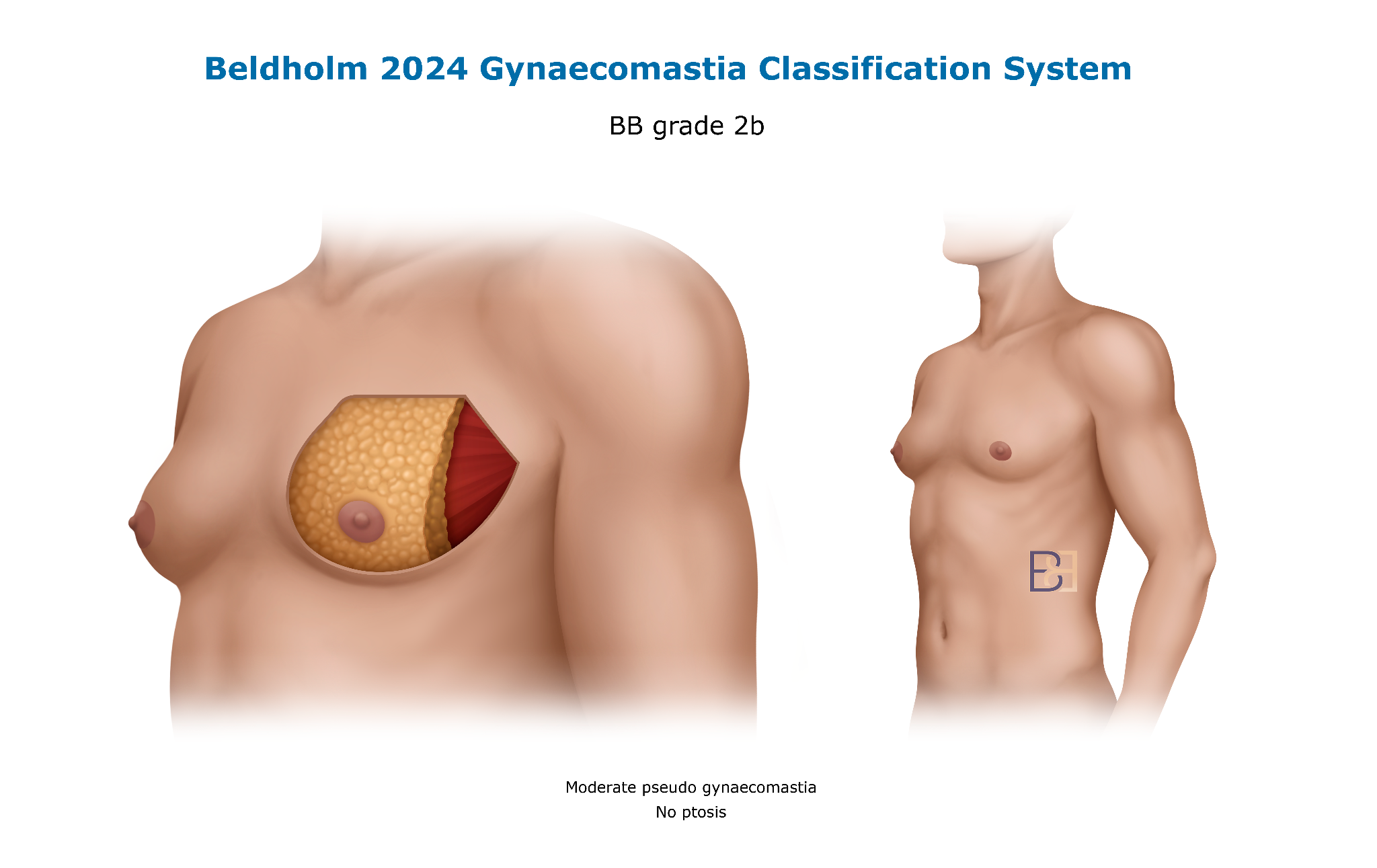

Pattern C: Combined gland and fat
This is the most common presentation: a firm gland under the nipple with surrounding fatty fullness across the chest. Both components contribute to the appearance and both need to be addressed.
Operation: Subcutaneous mastectomy combined with VASER suction-assisted lipectomy in a single operation. VASER liposuction is performed first to address the fatty component, and the gland is then removed through an infra-areolar incision.
For larger presentations, the incision is placed at the upper border of the areola (supra-areolar) and a small section of skin above the areola is excised to address skin redundancy. This pattern spans BB Grades 2a and 3a.
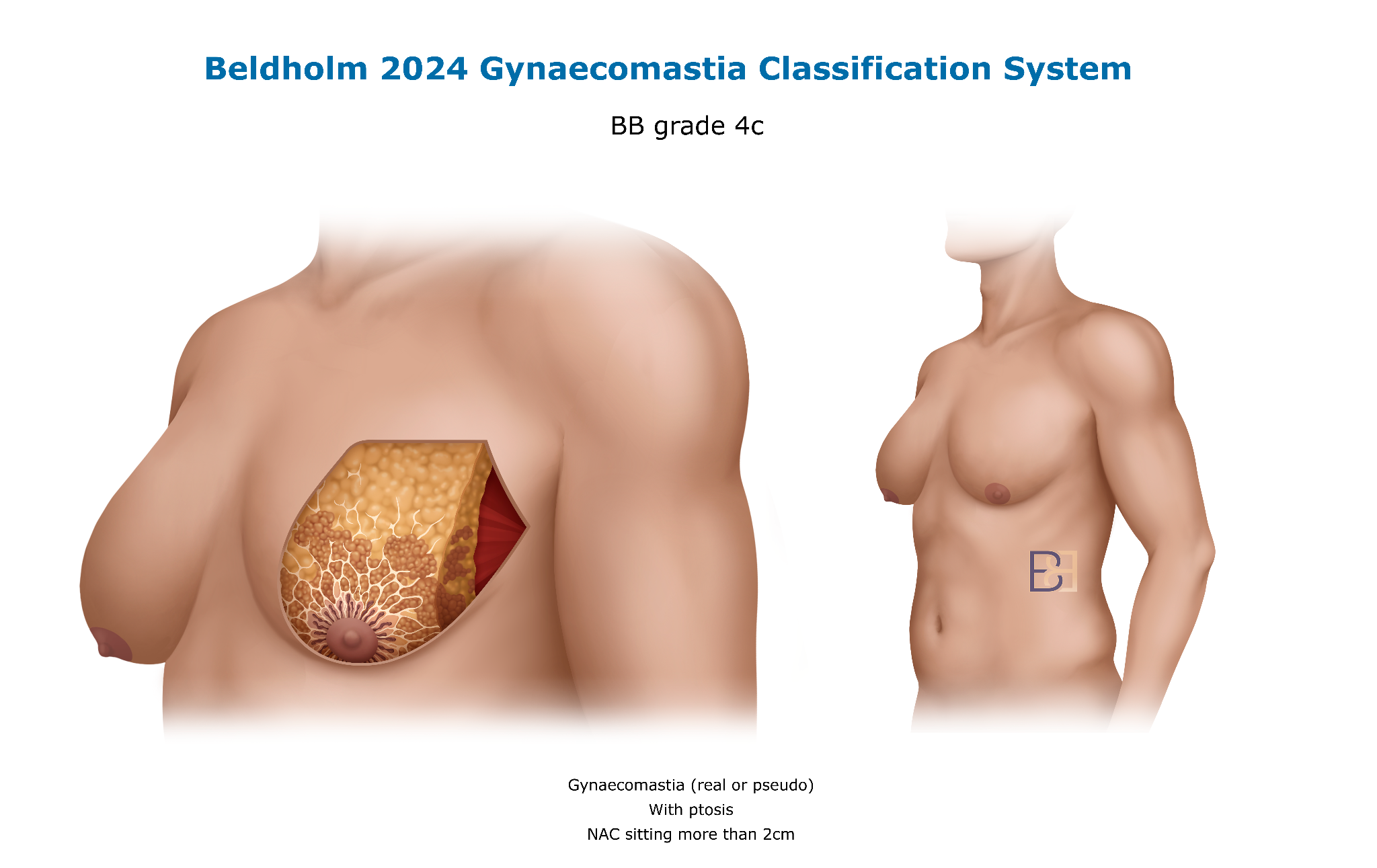
Pattern D: Significant skin excess after substantial weight loss
A separate pathway exists for patients with marked skin laxity or ptosis (the nipple sitting below the inframammary fold). This is most often seen after substantial weight loss and falls outside day-case surgery. Patients with this presentation are addressed through Dr Beldholm’s post-weight-loss surgical pathway, with assessment at consultation.
The full Beldholm 2024 framework covering all eight grades, from BB 1 through BB 4c, is set out in the patient guide below.
Download the Patient Guide
The Beldholm 2024 Gynaecomastia Grading System sets out eight grades of gynaecomastia, from BB 1 through BB 4c, with the recommended operation for each. The patient guide is a structured reference that organises this in one place.
Inside the guide:
- A diagram of each of the eight grades with anatomical reference
- A grade-by-grade table covering description and recommended operation
- Clinical terminology used in the recommendations, including subcutaneous mastectomy, VASER suction-assisted lipectomy, and skin excision techniques
It is designed to help patients identify which grade may apply to their presentation and to discuss surgical options at consultation.
The 8 Grades of Gynaecomastia and the Recommended Surgery for Each. Educational content only. Not a substitute for medical advice. Consultation required to determine suitability.
About Dr Bernard Beldholm

I am a Specialist General Surgeon based in the Hunter Valley, operating at Maitland Private Hospital. My clinical focus is body contouring, including post-weight-loss surgery, breast surgery, and gynaecomastia (male breast reduction).
Dr Bernard Beldholm M.B.B.S, B.Sc (Med), FRACS, Specialist General Surgeon. AHPRA Medical Registration number: MED0001186274.
Over more than 15 years working in body contouring surgery, I developed the Beldholm 2024 Gynaecomastia Grading System to organise the clinical decision-making for this procedure. The system sets out eight grades from BB 1 through BB 4c, each with a recommended operation. The grading system is the structure behind the patient guide above, and it is the framework I use when assessing patients at consultation.
At consultation, your presentation is assessed against the same framework you can read about in the guide, and the operation is matched to the pattern present rather than the reverse. The intent is a clear path from examination to treatment plan, with the discussion focused on what is appropriate for your circumstances.
Preparing for Surgery
Even for a day-case operation, some preparation in the weeks leading up to surgery makes a meaningful difference to wound healing and recovery. The points below are a starting framework; specific instructions are provided at consultation and ahead of surgery.
Weight stability. Surgery is performed once weight has been stable for at least six months. This applies whether weight has been recently lost or recently gained.
Smoking cessation. Smoking and vaping reduce blood flow to the skin and slow wound healing. I ask patients to stop at least four weeks before surgery and to remain off them through the early recovery period.
Alcohol moderation. Alcohol affects bleeding and bruising, and is reduced in the two weeks before surgery.
Medications and supplements. Some medications and supplements affect bleeding. I review your medication list at consultation and provide specific guidance on which to stop and when, taking into account any other medical conditions.
General fitness. Maintaining your usual level of activity and a balanced diet in the weeks before surgery supports recovery. Significant new exercise programs or restrictive eating patterns are best deferred until after the operation.
A detailed pre-operative instruction sheet covering medications, fasting, what to bring on the day, and post-operative arrangements is provided ahead of surgery.
Consultation Process

A GP referral is required before booking your first consultation. The referral confirms your eligibility for specialist care and allows me to access your relevant medical history.
I work to a two-consultation standard. Most patients are seen at least twice before surgery is scheduled. The first consultation is in person at the clinic in Maitland; the second can be in person or by phone or video, depending on what is clinically appropriate.
Consultation 1: Assessment. I take a full history and examine the chest. The history covers your medical background, weight changes, any medications or substances that may contribute to the condition, and your reasons for considering surgery. The examination distinguishes between glandular and fatty enlargement, assesses skin laxity, and identifies which of the patterns described above applies. If a recent ultrasound or set of endocrine bloods has not already been arranged by your GP, I provide a request form so these can be done before the second consultation.
Between consultations. Time is left to gather any imaging or blood results, to consider what was discussed, and to put together questions for the second visit.
Consultation 2: Surgical planning. I review the results, confirm which operation is appropriate, and explain what happens before, during, and after surgery. The practice coordinator then prepares a written quote and discusses scheduling.
Anaesthetic review. A separate phone consultation with the anaesthetist takes place before surgery, with an in-person review at the hospital on the day of the operation.
Patients typically book surgery one to three months after the second consultation, depending on practice availability and your circumstances.
You can book your first consultation online, or by telephoning the practice to speak with the receptionist.
Hospital and Recovery
Surgery is performed under general anaesthetic at Maitland Private Hospital, which has 24-hour medical cover and an on-site intensive care unit. For BB Grades 1 to 3, gynaecomastia surgery is a day procedure. Most patients are discharged on the same day as the operation, with a chest compression vest in place.
Compression garment. A fitted compression vest is worn day and night for the first two weeks, then most patients continue to wear it overnight for a further two to four weeks. The vest reduces swelling, supports the chest tissue while it heals, and helps the skin to redrape during healing.
Drains. Small drainage tubes are usually used in cases involving gland excision combined with VASER liposuction (typically BB Grades 2a and 3a). They are not used for Grade 1 cases or for liposuction-only operations. Where used, drains are removed within one to three days.
Wound care and follow-up. I use absorbable sutures for all surgical incisions. Where a drain is placed, a single non-absorbable stitch holds it in position and is removed when the drain comes out. The first follow-up appointment takes place within the week after surgery, with further reviews scheduled across the following weeks and months as healing progresses.
Healite LED therapy. Healite is a non-thermal LED light therapy that may be used after surgery to support wound healing. Sessions are short and are coordinated with your follow-up appointments.
Return to work and activity. Recovery time depends on what you do. Most patients return to desk-based work within a few days. Activities involving moderate physical effort can usually resume within one to two weeks. Heavy lifting and chest-focused exercise are restricted for a longer period, typically four to six weeks, to allow healing of the deeper tissues. I provide a personal recovery plan at consultation based on your work and lifestyle.
Healing timeline. Some swelling and firmness in the operated area is normal in the first weeks and gradually resolves. This typically takes three to six months, depending on the operation performed.
Risks and Complications

All surgery carries risk. Patients considering gynaecomastia (male breast reduction) surgery should understand that complications can occur even when the operation is performed with reasonable care. The risks below are not exhaustive. They are discussed in detail at consultation, alongside the steps taken to reduce them and the management approach if they occur.
General surgical and anaesthetic risks
These apply to any operation under general anaesthetic and include bleeding, haematoma (a collection of blood under the skin), seroma (a collection of fluid), infection, wound healing problems, anaesthetic reactions, and deep vein thrombosis or pulmonary embolism. Patients with other medical conditions or on certain medications may have an increased risk profile, which is reviewed at consultation.
Specific to gynaecomastia surgery
- Asymmetry between sides. A small degree of asymmetry is normal in the male chest, both before and after surgery. Surgery aims to address visible asymmetry, though some degree of asymmetry generally remains.
- Surface irregularities. Rippling, depressions, or raised areas can develop, particularly where VASER liposuction has been used or where skin excision is part of the operation.
- Sensation changes around the nipple and chest skin. Numbness, hypersensitivity, or altered sensation can occur. These changes are usually temporary, but in some cases are permanent.
- Residual or recurring tissue. A small amount of glandular tissue may remain after surgery, or new tissue can develop if the underlying cause continues, including ongoing use of anabolic steroids or certain medications.
- Scarring. Scars are a permanent outcome of any incision. Their appearance varies between patients and depends on factors such as skin type, healing characteristics, and post-operative care.
- Pigmentation changes. The skin around the areola or chest may show changes in colour after surgery, particularly in darker skin types.
- Skin healing problems. Where skin excision is part of the operation, delayed healing or skin necrosis is possible, particularly in patients who smoke, have diabetes, or have other conditions that affect circulation.
- Need for revision surgery. A second operation may be required if a complication develops or if the patient and surgeon agree that an additional procedure would be appropriate.
A complete review of risks, expected recovery, and individual factors that may apply takes place at consultation prior to surgery.
Frequently Asked Questions
Will gynaecomastia come back after surgery?
Recurrence is uncommon when the underlying cause has been addressed. Surgery removes the existing glandular and fatty tissue. If contributing factors continue, including anabolic steroid use, certain medications, or significant weight gain, new tissue can develop and the condition may reappear. Maintaining stable weight and avoiding contributing factors after surgery reduces this risk.
Is gynaecomastia surgery covered by Medicare?
Medicare eligibility for gynaecomastia surgery is assessed individually. Specific clinical criteria apply, and these are reviewed against your medical history and presentation at consultation. Your GP can provide initial guidance during the referral process.
What is the difference between real and pseudo-gynaecomastia?
Real gynaecomastia involves the development of glandular breast tissue beneath the nipple. The tissue feels firm or rubbery on examination. Pseudo-gynaecomastia is fatty tissue alone, without glandular enlargement, and feels softer. The distinction matters because real gynaecomastia generally requires surgical removal of the gland (subcutaneous mastectomy), while pseudo-gynaecomastia can often be addressed with VASER suction-assisted lipectomy alone. Examination at consultation distinguishes the two.
Can I have liposuction alone without removing the gland?
VASER suction-assisted lipectomy alone is appropriate for pseudo-gynaecomastia, where the enlargement is fatty tissue and there is no glandular component to remove. For real gynaecomastia, where glandular tissue is present, liposuction alone will not address the firm tissue beneath the nipple, and a residual prominence is likely to remain. Examination at consultation determines which approach applies.
Do I need a GP referral?
Yes. A GP referral is required before booking a consultation with Dr Beldholm. The referral confirms eligibility for specialist care and supports access to Medicare rebates where applicable. The first consultation cannot be booked without a current referral.
When can I return to gym and exercise?
Light walking can usually resume within a few days of surgery. Moderate cardiovascular exercise is generally introduced at one to two weeks. Heavy lifting and chest-focused exercise are restricted for four to six weeks to allow healing of the deeper tissues. Specific timelines depend on the operation performed and are reviewed at the post-operative appointments.
Take the Next Step
Gynaecomastia (male breast reduction) surgery in BB Grades 1 to 3 is performed as a day procedure under general anaesthetic at Maitland Private Hospital. Each patient is assessed individually at consultation, where the operation is matched to the pattern present and the practical detail of surgery, recovery, and Medicare eligibility is reviewed.
A GP referral is required before the first consultation can be booked. There is no rush to proceed before you feel ready.
The next step is a discussion with your GP to obtain a referral. Once you have the referral, a consultation can be booked online or by telephoning the practice during business hours.

