Comprehensive Body Contouring After Significant Weight Loss
Surgical planning matched to your pattern of loose skin, not the other way around. One coordinated plan across the regions that need it.
After significant weight loss, loose skin rarely sits in one region only. It runs across the abdomen, extends around to the flanks and lower back, and often involves the arms, thighs, or breast as well. Each region has its own pattern, and the operations that address one region are not interchangeable with those that address another.
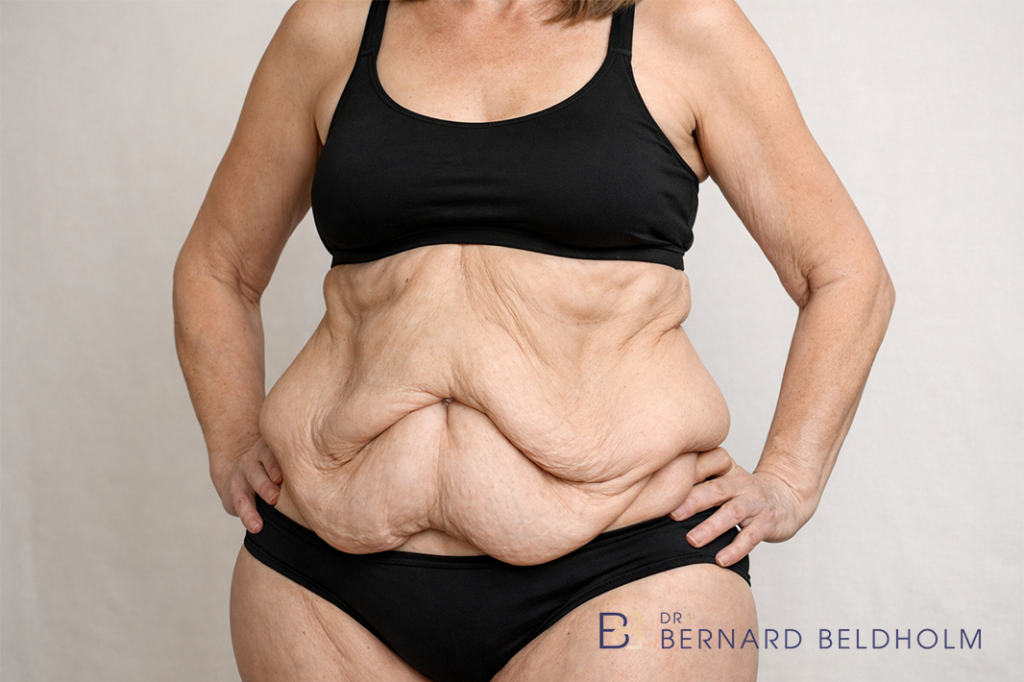
For patients in this position, the question is not which single procedure to choose. It is how to plan a sequence of operations across the regions that need them. A comprehensive approach starts by mapping the full pattern, then deciding which operations belong together in one stage and which are best spaced apart.
Dr Bernard Beldholm FRACS is a Specialist Surgeon focused on post-weight-loss body contouring, with more than fifteen years of experience planning and performing this kind of multi-region work.
My Approach

I start with the pattern, not the procedure
Many patients arrive having already settled on a single procedure, often an abdominoplasty (tummy tuck), wanting to know whether that one operation will address everything. For some patients, the answer is yes. For those with multi-region laxity, a single-procedure plan leaves residual skin in the regions the procedure was never designed to reach.
My approach starts at the other end. The first task at consultation is to map the full pattern of loose skin across every region affected, then work out which operations match that pattern and how they fit together.
Why pattern-matching matters

Each pattern of loose skin has its own surgical anatomy. Vertical excess on the abdomen calls for a different operation to horizontal excess across the midline. Skin that extends around the flanks and lower back cannot be reached through an abdominal-only incision. These anatomical realities determine which procedure matches which pattern.
One surgeon through every stage
For multi-region work, I believe the surgeon who plans the pathway should be the surgeon who performs every stage. Scar healing in one region affects the timing of the next. Blood-test results from the first stage inform the supplementation plan for the second. And when a patient returns six months after the first operation, the same surgeon who assessed them at the start is the one reviewing the result.
Pre-operative preparation matters more here

Pre-operative preparation matters more for this kind of surgery than for procedures performed on a healthier physiological baseline. Post-weight-loss patients, particularly post-bariatric patients, often have nutritional vulnerabilities that increase complication risk if not corrected before surgery. The preparation protocol I use, detailed further down this page, is built around that reality.
Is this the right approach for me?
For patients with significant loose skin after major weight loss, surgery is what removes it. Skin that has been stretched for years rarely retracts further once weight has stabilised, and non-surgical methods do not meaningfully change redundant skin. Whether surgery is right at this point in time, and at what scale, depends on a few specific factors.
Is surgery the right answer?
Several factors determine whether surgery should proceed at all, or whether it should be deferred.
Has your weight been stable? A minimum of six months at a stable weight is recommended before any body contouring operation. For patients who have undergone bariatric surgery, twelve to eighteen months of weight stability is standard. Operating on weight that is still changing can compromise the result and require revision.
Is your BMI in a workable range? A BMI above 35 generally warrants deferring surgery. The complication risk profile shifts at higher BMI, and skin removal procedures performed at higher BMI tend to leave more residual laxity. For some patients, further weight loss before surgery, supported by GP or bariatric input, produces a better surgical outcome.
Are you planning further pregnancies? If so, surgery is best deferred until family is complete. A subsequent pregnancy can stretch the abdominal wall and skin envelope again, undoing the surgical correction.
Are you a current smoker? Smoking and nicotine in any form, including vaping and nicotine replacement products, increase complication risk significantly: wound breakdown, skin necrosis, and impaired healing. Cessation for at least six weeks pre-operatively is required, and longer is better.
Do you have uncontrolled health conditions? Conditions such as poorly controlled diabetes, untreated sleep apnoea, anaemia, or active inflammatory disease need to be optimised before elective body contouring. The consultation will identify these and outline what needs to be in place before surgery proceeds.
Are you expecting your skin to tighten on its own? After significant weight loss, skin elasticity has usually been compromised by long-term stretching. Skin that is loose at twelve months post-weight-loss is unlikely to retract further. Creams, exercise, massage, and non-surgical “skin tightening” treatments do not produce meaningful change in this situation.
Single procedure or comprehensive plan?
The second question is about scale.
A comprehensive approach is the right scale when:
- Loose skin extends across more than one region, for example abdomen plus flanks plus lower back, or torso plus arms or thighs
- Skin laxity crosses the abdominal midline horizontally as well as hanging vertically
- The full pattern of loose skin cannot be addressed through a single standard operation
- The total volume of work warrants planned sequencing rather than ad-hoc procedure choice
A single-procedure approach may be more suitable when:
- Loose skin is limited to one region, for example lower abdomen only
- The pattern is straightforward, such as post-pregnancy lower abdominal laxity with mild muscle separation
- Weight loss has been modest, a few kilograms rather than tens of kilograms
- A standard abdominoplasty or similar single procedure can address the entire concern
Patients whose situation matches the second group are usually better served by a surgeon whose practice centres on standard abdominoplasty for post-pregnancy or moderate-laxity patients. The remainder of this page describes the comprehensive multi-region approach, suited to patients with significant loose skin spanning multiple regions after major weight loss.
Matching the Procedure to your Pattern
Several procedures sit under the general description of body contouring after weight loss, sometimes also called skin removal surgery. They are not interchangeable. Each is designed for a specific pattern of loose skin, and the operation that suits one pattern leaves residual skin in another. The right procedure depends on where the loose skin sits, how it sits, and how far it extends.
A brief note on terminology
A few terms appear in the procedure descriptions below. Vertical excess refers to skin that hangs downward under gravity. Horizontal excess refers to skin that gathers across the midline, often forming a fold above the umbilicus. Circumferential excess extends around the flanks and lower back. Most patients after significant weight loss show a combination of these patterns, not just one.
Vertical excess (lower abdomen)
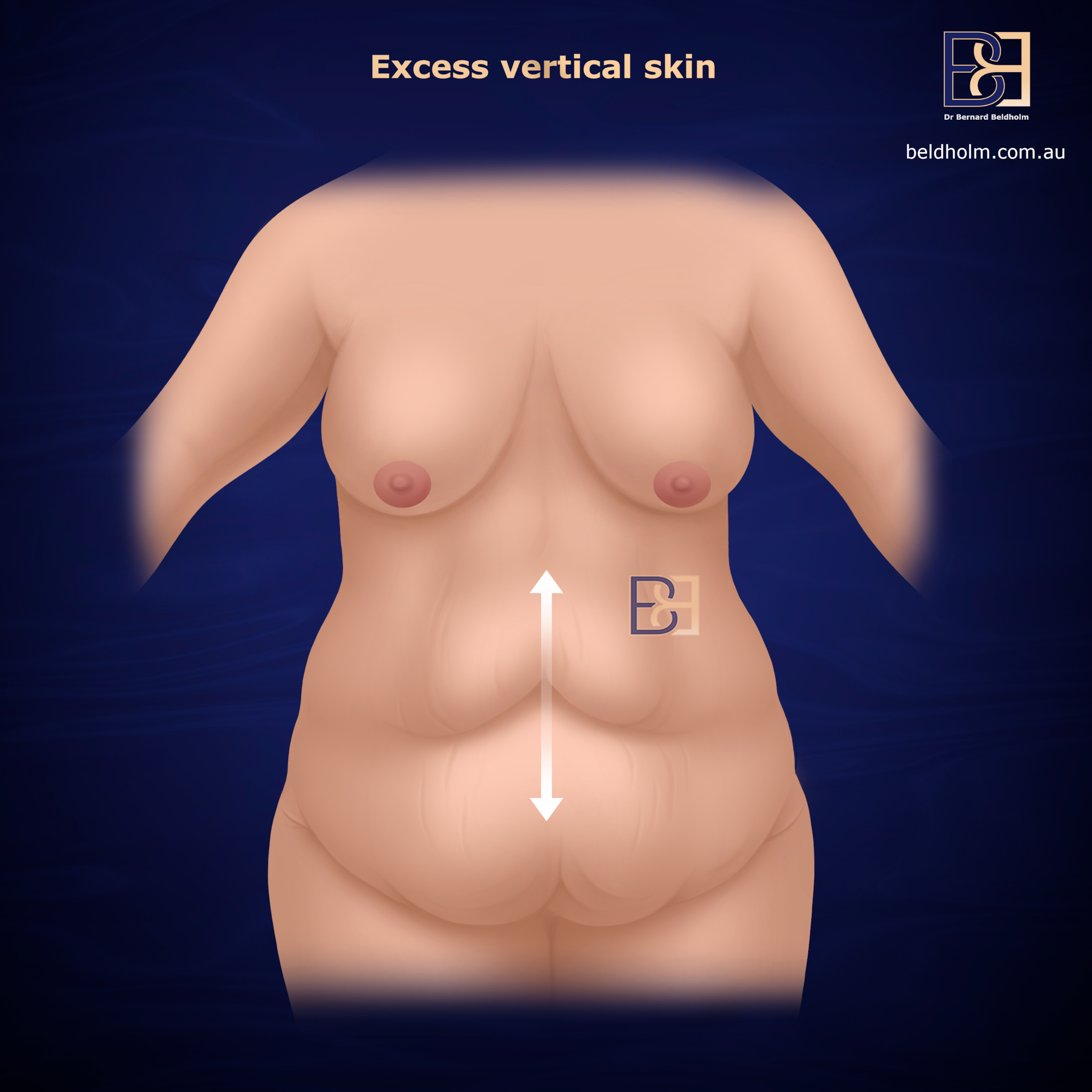
When excess skin hangs downward from below the umbilicus and the upper abdomen is largely unaffected, the procedures that address this pattern remove skin through a horizontal incision across the lower abdomen.
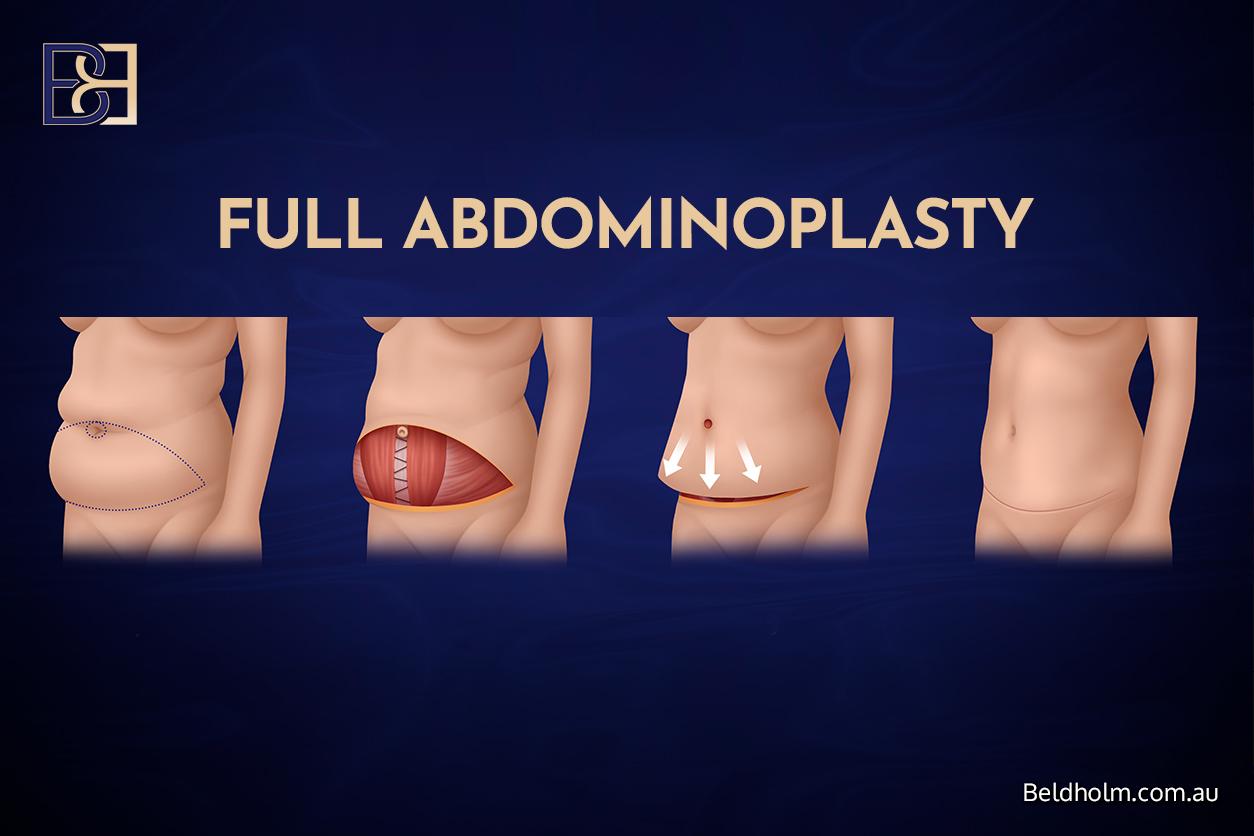
Standard abdominoplasty (tummy tuck)
Removes excess skin and fat from below the umbilicus through a horizontal hip-to-hip incision low on the abdominal wall. The umbilicus is repositioned. The abdominal muscles can be tightened where separation (diastasis recti) is present. The scar sits low enough to be covered by underwear.
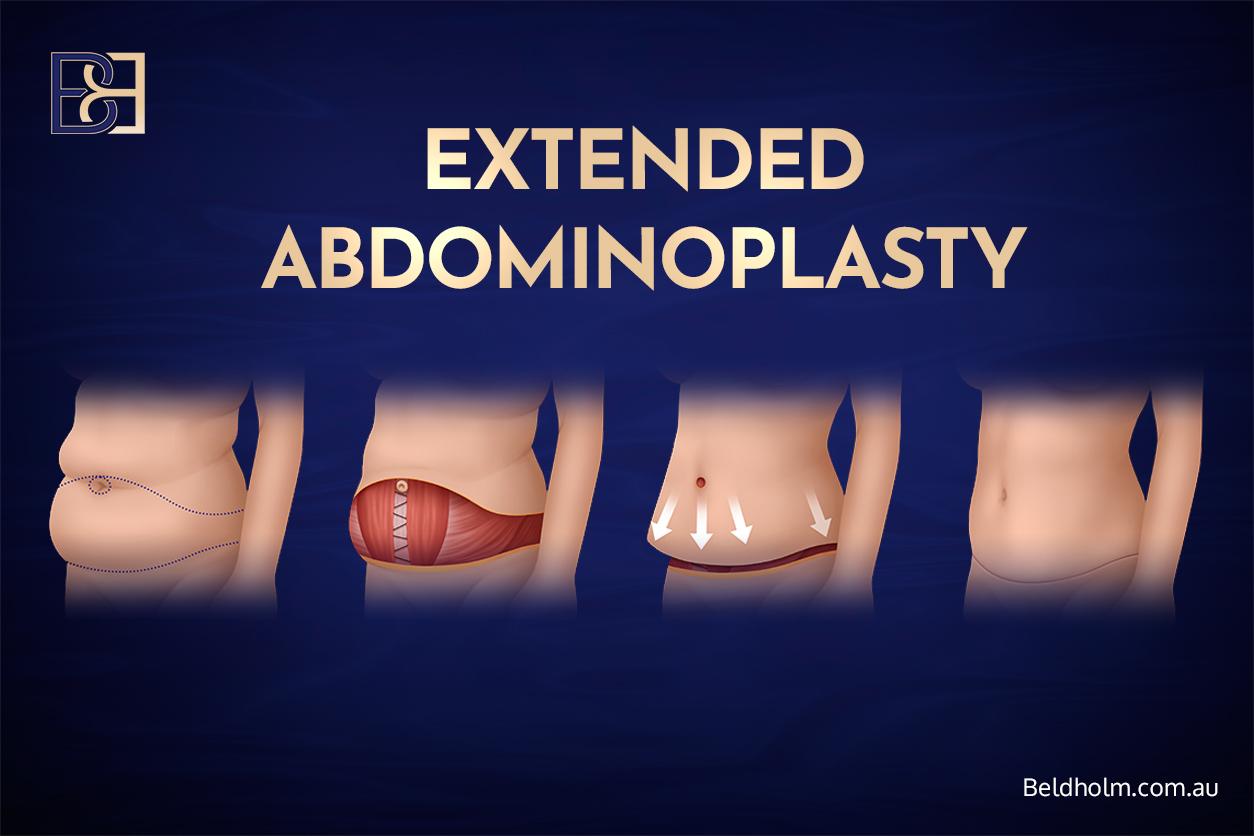
Extended abdominoplasty
A standard abdominoplasty with the horizontal incision extended laterally toward the flanks. Removes excess from the lower abdomen and the adjacent flank/hip area. Considered when vertical laxity continues laterally onto the flanks but does not extend around to the lower back. Patients with laxity that extends fully around to the lower back are usually candidates for a belt lipectomy instead (see below).
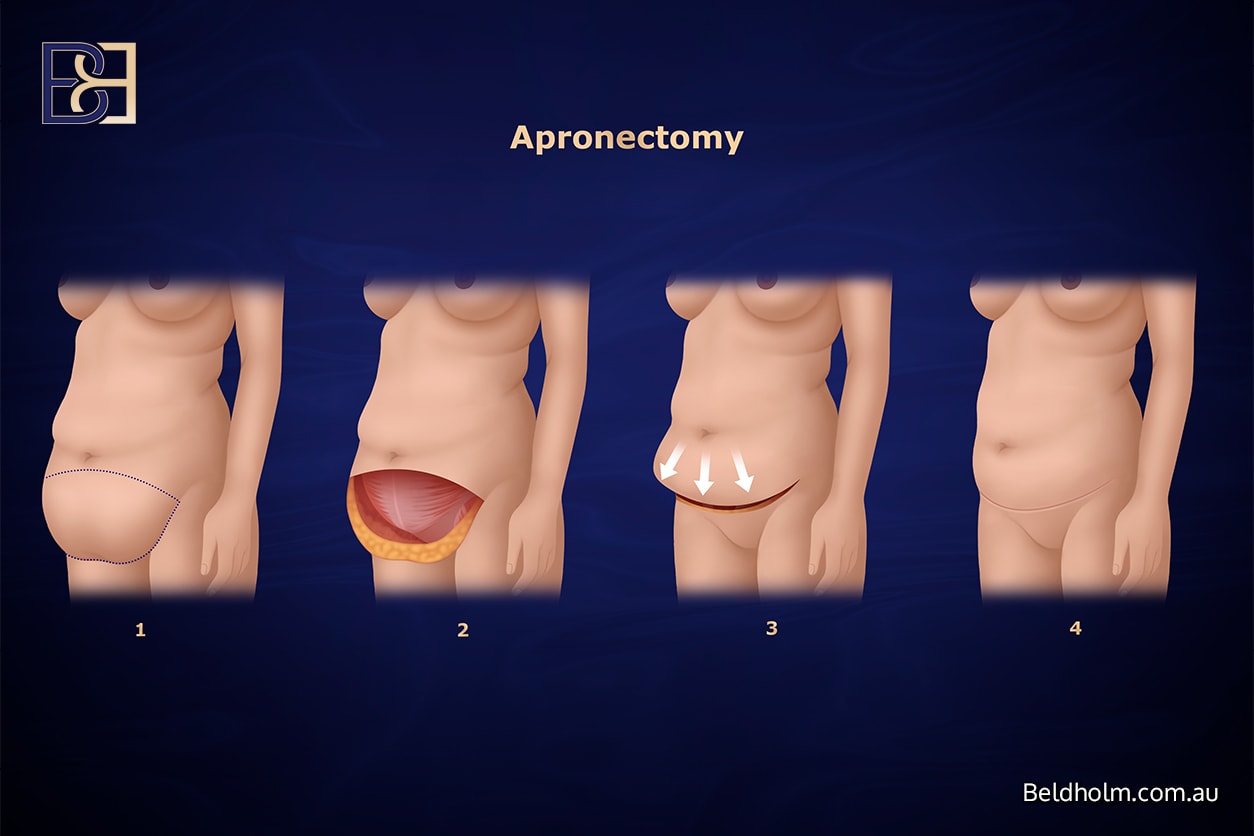
Apronectomy (panniculectomy)
Removes the lower abdominal apron through the same horizontal incision but does not tighten the abdominal muscles or reposition the umbilicus. Considered for patients whose comorbidities limit a fuller operation, or where the priority is removal of a heavy apron causing functional symptoms such as rashes, hygiene difficulties, or mobility limits. Medicare eligibility may apply where criteria are met, assessed individually at consultation.
Horizontal excess (mid-abdominal)
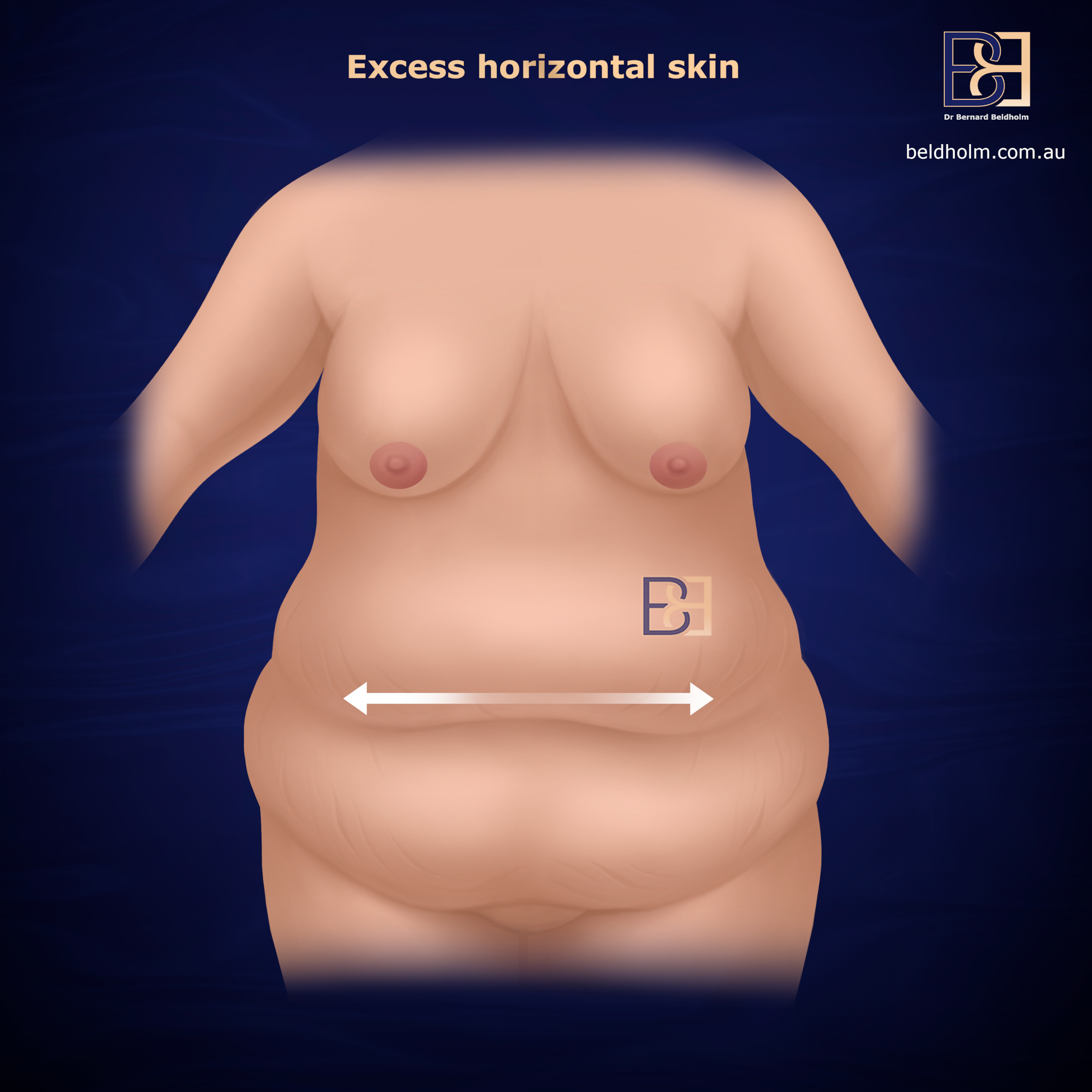
Some patients have skin that gathers horizontally across the midline of the abdomen, particularly above the umbilicus, in addition to any vertical hanging. A standard abdominoplasty removes vertical excess only and leaves this horizontal excess in place.
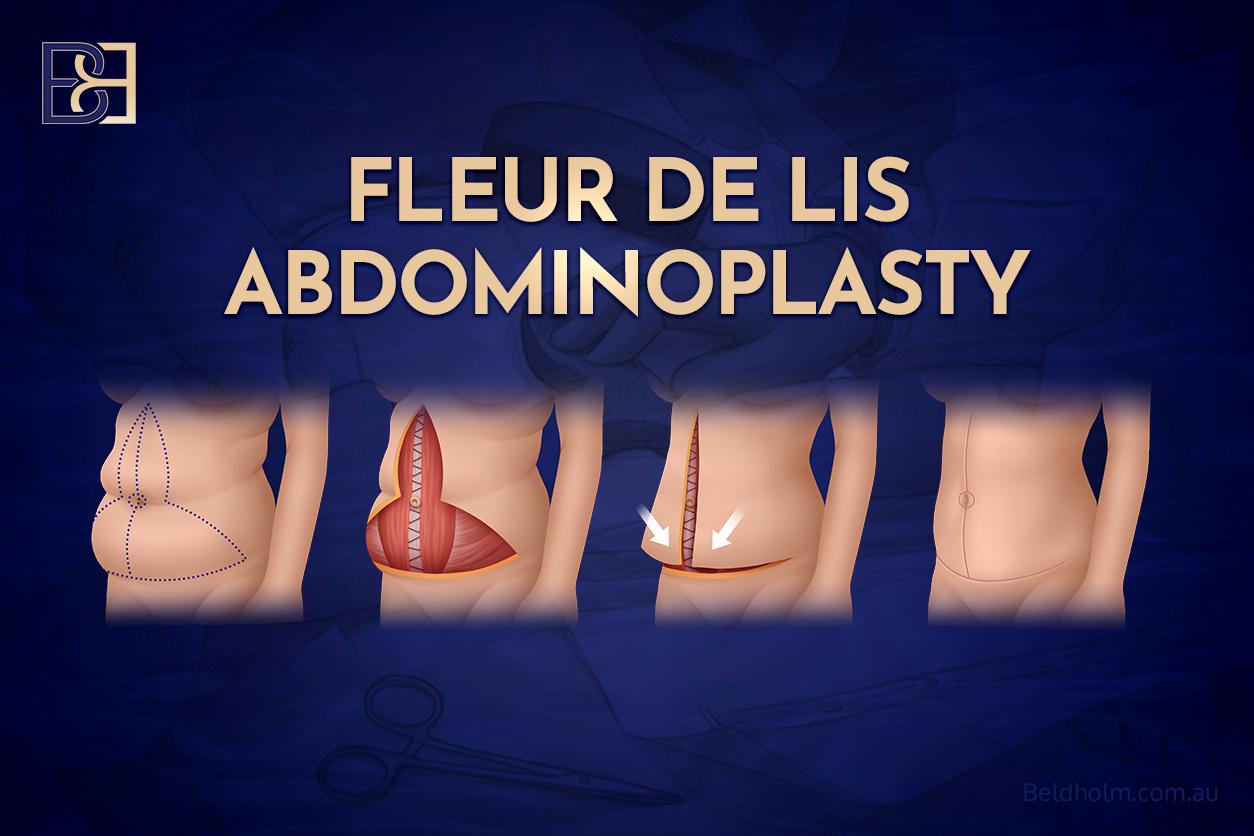
Fleur-de-Lis abdominoplasty (Fleur-de-Lis tummy tuck)
Adds a vertical midline incision to the standard horizontal incision, forming an inverted T-shape. This combination removes skin in two directions: vertically through the lower-abdomen excision, and horizontally through the midline excision. The trade-off is a more extensive scar than a standard abdominoplasty, including a permanent vertical midline scar.
Combined vertical, horizontal, and upper-abdominal excess
After major weight loss, the most common pattern involves vertical excess in the lower abdomen, horizontal excess across the midline, and additional laxity in the upper abdomen above the umbilicus. A Fleur-de-Lis alone leaves the upper abdomen untouched.
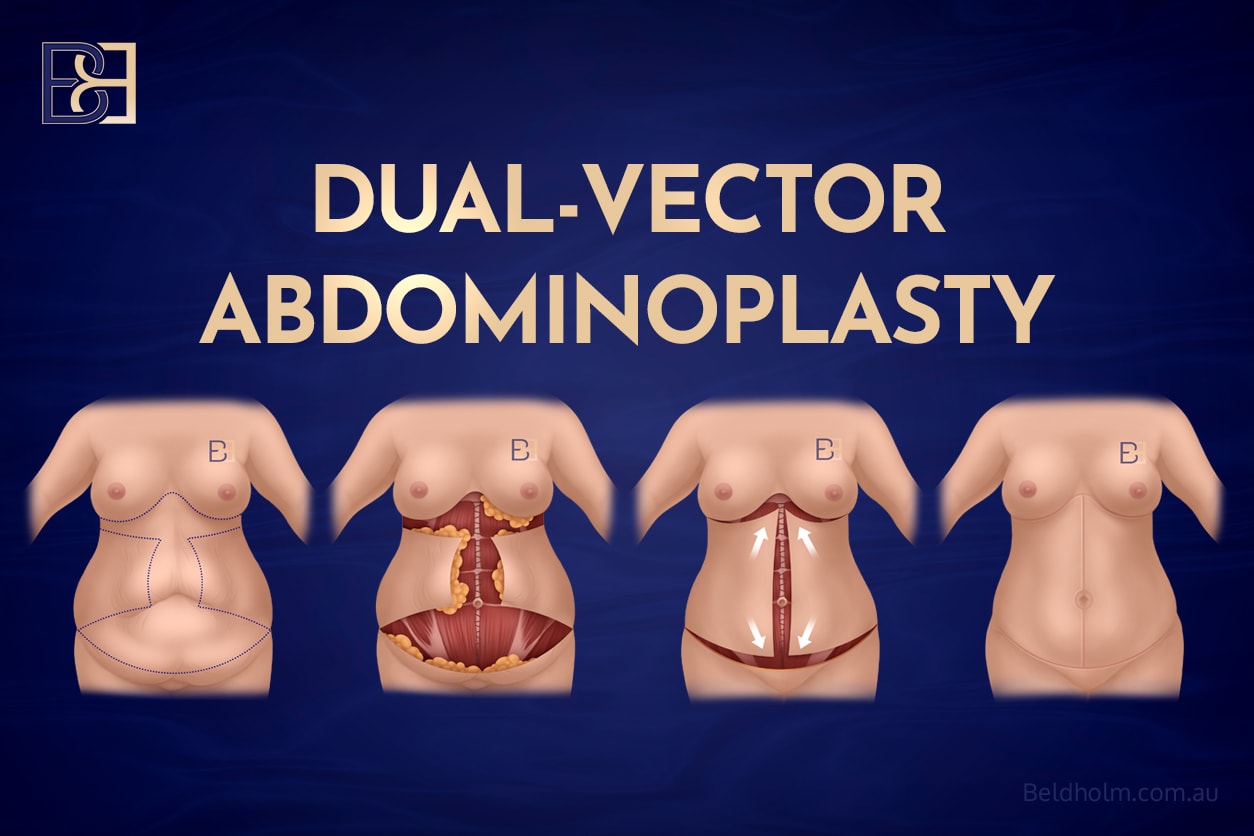
Dual-vector abdominoplasty
A three-zone operation that addresses the lower abdomen, mid-abdomen, and upper abdomen in a single procedure. The Fleur-de-Lis component removes vertical and horizontal excess from the lower and mid-abdomen. An additional incision beneath the breast crease removes excess from the upper abdomen. Appropriate when upper-abdominal laxity is significant and a Fleur-de-Lis alone would leave skin in that zone.
Torso-spanning excess (flanks and lower back)
When loose skin extends around the flanks and lower back, an abdominal-only operation cannot reach it. The pattern requires an incision that continues circumferentially around the body.
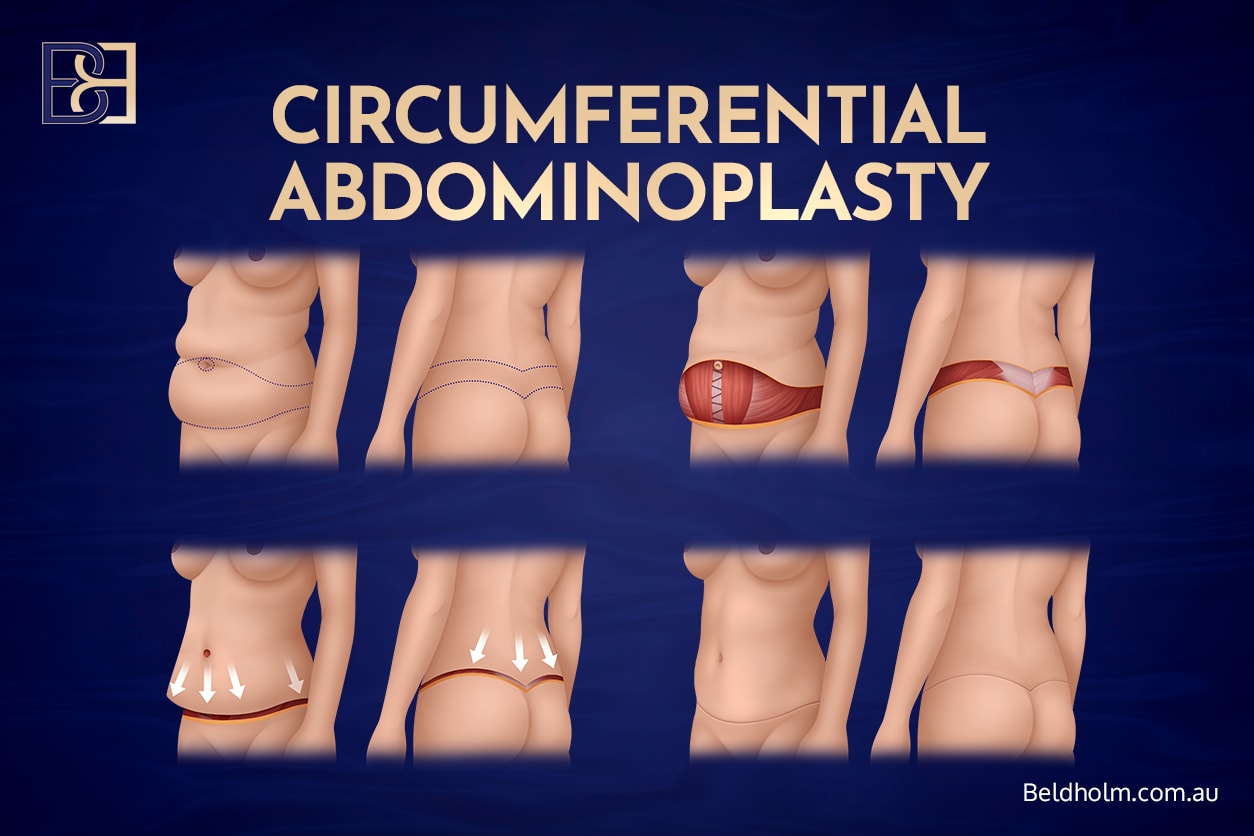
Belt lipectomy (circumferential body lift, lower body lift)
Removes skin and fat from the lower abdomen, flanks, and lower back through a continuous incision around the waist. The same operation also lifts the buttocks and outer thighs as the skin is closed. Hospital stay is typically three to five days.
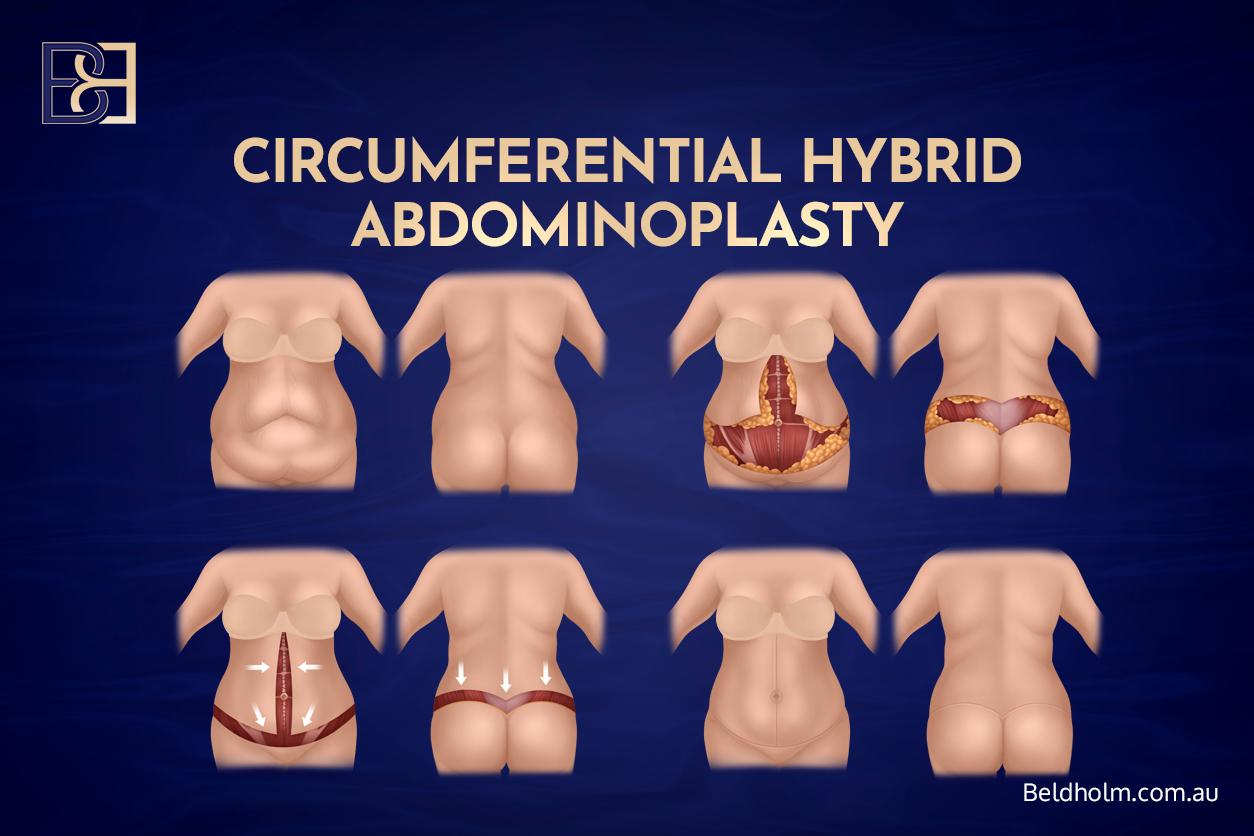
Hybrid circumferential abdominoplasty
A Fleur-de-Lis abdominoplasty combined with a belt lipectomy in a single operation. Addresses vertical, horizontal, and circumferential excess together when the pattern spans all three. Operative time is longer and hospital stay is typically five to seven days. Reserved for patients whose pattern warrants it and whose physiology supports the operative load.
Multi-region: beyond the torso
Loose skin after significant weight loss often extends beyond the torso. These regions require their own procedures:
- Arms. Brachioplasty (limited, full, or extended) addresses upper-arm and adjacent torso laxity.
- Thighs. Thighplasty (limited, vertical, full, or J-pattern) addresses inner-thigh and groin laxity.
- Breast. Mastopexy (breast lift), or mastopexy with augmentation, addresses breast deflation and skin-envelope laxity.
Each region is covered in detail on its own page. The question of how multiple regions are sequenced into single or staged operations is addressed in the next section.
Adjuncts
Some patients have residual fat deposits alongside loose skin that the excisional procedure alone does not fully address. In selected cases:
- Suction-assisted lipectomy (liposuction) is performed alongside the main operation to remove fat and improve contour.
- VASER (ultrasound-assisted lipectomy) uses ultrasound to liquefy fat before extraction; useful for fibrous fat that does not respond well to standard liposuction.
Book your appointment online now
Single operation or staged plan?
After significant weight loss across multiple regions, planning the surgery involves a question that single-procedure patients do not need to answer: how many operations, in what order, with what spacing between them. The aim is to plan the smallest number of operations that is medically sensible for the patient. For some patients that is a single comprehensive operation. For others it is two or more stages. The decision depends on the pattern of loose skin, physiology, comorbidities, and recovery support.
The case for combining where appropriate
Where physiology and operative time allow, combining procedures into a single operation has practical advantages:
- One anaesthetic exposure rather than two or three across separate operations
- One recovery window rather than repeated periods off work and family responsibilities
- One hospital admission and one set of perioperative risks, rather than these stacked across stages
- Continuity of healing across regions that share blood supply or anatomic relationships, such as the abdomen, flanks, and lower back addressed together through a hybrid circumferential approach
- Reduced cumulative scar revision risk compared with multiple separate operations on adjacent areas
In practice, most procedures can be combined for patients whose operative time and physiological reserve allow it. Combinations performed in suitable cases include hybrid circumferential abdominoplasty addressing the entire torso, belt lipectomy combined with brachioplasty, and circumferential abdominoplasty combined with thighplasty. The constraint is operative time and physiological reserve rather than fixed rules about which procedures pair with which.
The case for staging
Several factors can shift the decision toward staging:
- Operative time and physiological reserve. This is usually the limiting factor. Each additional procedure adds operative time, blood loss, and physiological stress on the body. Beyond a threshold that varies between patients, combining further procedures introduces more risk than is medically justified.
- BMI, anaemia, and comorbidities. A patient at the upper end of the workable BMI range, or with diabetes, sleep apnoea, or anaemia identified on pre-operative bloods, may be better served by staged operations even where the procedures could anatomically be combined.
- Scar healing in adjacent regions. When a procedure leaves a scar that runs close to where the next procedure’s incision will sit, allowing the first scar to settle reduces the risk of complications at the second operation.
- Recovery support availability. A patient travelling from interstate or further afield, with limited support at home, may opt to space operations to manage recovery practically.
How the decision is made
The decision is reached during the two-consultation process described later on this page, with input from blood results and medical history.
The factors weighed at that point include:
- The total pattern of loose skin and which regions are involved
- Estimated operative time for each combination being considered
- Pre-operative bloods, BMI, and any comorbidity profile
- Smoking status and nutritional baseline
- Recovery support and time available off work
- Patient preference for fewer larger operations versus more numerous shorter ones
Whichever pathway is recommended, the same surgeon plans and performs every stage. Continuity matters most when staging is required: the surgeon who assessed the original pattern is the one mapping the next operation onto the result of the first.
Free guide: 7 Surgical Options for Loose Skin on the Abdomen, Flanks & Back
For patients who want a more detailed reference to read at home or share with family, the practice provides a free patient guide titled “7 Surgical Options for Loose Skin on the Abdomen, Flanks & Back Every Post-Weight-Loss Patient Should Know.”
The guide describes each of the seven excisional procedures: what pattern of loose skin it addresses, how it combines with adjacent operations, scar position and length, and the role of pre-operative nutritional preparation. The format is designed to be read at home, shared with a partner or family member, and brought to the consultation as a reference for the discussion.
Educational content only. Not a substitute for medical advice. Each patient’s circumstances and pattern of loose skin are assessed individually at consultation.
About Dr Bernard Beldholm

My background and training
My full credentials are: Dr Bernard Beldholm M.B.B.S, B.Sc (Med), FRACS, Specialist General Surgeon. AHPRA Medical Registration number: MED0001186274.
After completing my surgical training and Fellowship of the Royal Australasian College of Surgeons (FRACS), I focused my practice on body contouring after major weight loss. That has been the principal focus of my work for more than fifteen years.
Why post-weight-loss body contouring
This kind of surgery is different from body contouring performed on a healthier physiological baseline. Patients come to me after losing significant weight through bariatric surgery, medical weight-loss programs, or sustained lifestyle change. The physiology, nutritional baseline, and skin elasticity in this group differ from patients without a history of major weight loss.
The volume of skin to remove is greater. The pre-operative preparation matters more. The decision about combining or staging procedures is more complex. Over the years, focusing on this specific patient group has allowed me to develop a structured way of working through each of those questions.
Where I operate

I operate at Maitland Private Hospital in the Hunter Valley, NSW. The hospital provides 24-hour doctor cover and on-site intensive care, which I consider clinically important for the larger operations this patient group often requires.
Patients travel to me from across NSW including Sydney, and from interstate. The consultation process described below is structured to accommodate distant patients, with at least one in-person consultation and additional consultations conducted by telehealth where clinically appropriate.
Book your appointment online now
Preparing for Surgery: Pre-operative Optimisation

For most patients in my practice, surgery is six weeks to three months away from the first consultation. That gap is not waiting time. It is preparation time.
Why preparation matters more for this kind of surgery
Body contouring after major weight loss takes place on a different physiological baseline than body contouring on patients without prior major weight loss. Post-bariatric patients commonly carry nutritional deficiencies including low iron, low vitamin B12, low vitamin D, and sometimes low protein. Bariatric procedures themselves alter how nutrients are absorbed. Patients who have lost weight through medical weight-loss programs or sustained lifestyle change can also have suboptimal nutritional baselines, particularly when weight loss has occurred over a short period.
These deficiencies, if uncorrected, increase surgical risk. Wound healing depends on protein, vitamin C, zinc, and adequate iron. Skin and tissue strength depend on the same. Blood loss tolerance is reduced when haemoglobin is borderline. The complication risk is meaningfully higher when nutritional baseline has not been corrected before surgery.
Pre-operative optimisation is therefore not a wellness add-on. It is part of the surgical plan.
Which operations the protocol applies to
The full protocol applies to the larger body contouring operations: abdominoplasty in any pattern (standard, Fleur-de-Lis, dual-vector, extended), apronectomy, belt lipectomy, hybrid circumferential abdominoplasty, full or extended brachioplasty, and thighplasty in any pattern. The protocol does not apply to limited brachioplasty alone, suction-assisted lipectomy alone, or to patients without a history of major weight loss; nutrition for those patients is discussed individually at consultation.
For comprehensive single-stage operations, where multiple regions are addressed in one session, the same protocol applies but the demand on physiology is higher. The nutritional baseline that needs to be in place before such an operation is correspondingly higher.
Tier 1: universal post-weight-loss supplementation

Every post-weight-loss patient undergoing a major operation starts Tier 1 from the time of consultation, ideally a minimum of four weeks pre-operatively:
- A complete multivitamin
- Vitamin D3, 3000 to 6000 IU daily, with vitamin K2
- Vitamin C, 1 to 2 grams daily during the perioperative period
- Zinc, 8 to 11 milligrams daily
- Whey protein isolate (WPI), 80 to 100 grams daily, for patients whose dietary protein intake is inadequate. This is very common after bariatric surgery, where altered absorption and reduced food volume often make it difficult to reach daily protein targets through diet alone.
Tier 2: individualised additions based on blood tests
Tier 2 is added at the second consultation, after pre-operative blood test results have been reviewed. Depending on what the blood tests show, Tier 2 may include any combination of: iron, vitamin B12, folate, vitamin A, vitamin B1 (thiamine), calcium citrate, selenium, and magnesium. Specific dosing is individualised.
Timing: fish oil and post-operative bloods
Two additional timing points are part of the protocol:
- Fish oil and omega-3 supplements should be ceased one week before surgery to reduce the risk of bleeding during and after the operation. They can be resumed one to two weeks after surgery once the highest-risk bleeding window has passed.
- Post-operative blood tests are taken six to eight weeks after surgery to confirm nutritional status remains stable through the recovery period and to identify any deficiencies that have emerged.
The Consultation Process
I see all surgical patients across at least two consultations, sometimes more, before booking surgery. The two-consultation structure is my clinical standard for this kind of work. It allows time for blood results, nutrition setup, and a considered decision before any commitment.
Booking and what is required

A GP referral is required for all surgical consultations. Bookings can be made online through the practice website or by telephoning the practice receptionist. Once booked, the typical lead time from initial consultation to surgery is one to three months, depending on operative scheduling and how preparation progresses.
Consultation 1: initial assessment
The first consultation covers the clinical assessment: medical history, examination of the regions concerned, and a discussion of which procedures match your pattern of loose skin. By the end of the first consultation, patients leave with:
- A nutrition guide and the Tier 1 supplement protocol to start immediately
- A pathology blood form to take to a collection centre at a time that suits
- A list of any additional tests, investigations, or specialist reviews that may be required before surgery proceeds
- A clear sense of which procedures are likely to be considered, with the final surgical plan to be decided at the second consultation
Consultation 2: blood results and surgical planning
The second consultation takes place two to four weeks after the first, once blood results are available. At this consultation:
- Blood test results are reviewed; Tier 2 supplements are added where indicated
- The surgical plan is finalised, including which procedure or combination of procedures will be performed and whether the work will be staged
- Risks are discussed in detail, including specific risks relevant to the procedures being considered
- The practice coordinator joins the consultation to provide a written quote covering surgical fees, anaesthetic fees, hospital fees, and any associated costs
Telehealth for distant patients
Patients travelling from Sydney, interstate, or rural areas can usually conduct one of the two consultations by telehealth, with the other in person. The decision about which consultation suits which format is made on a case-by-case basis.
For most distant patients, the first consultation is conducted by telehealth and the second is conducted in person at Maitland. This allows the in-person assessment to take place close to the surgical decision point, when blood results are also available. For some patients, the in-person component is consolidated on the day before surgery, with the assessment, the blood-results review, and the procedure-confirmation review all completed at that point.
At least one consultation must take place in person before surgery is booked.
Anaesthetic consultation
A separate anaesthetic consultation is part of the pre-operative pathway for all surgical patients. This is usually conducted by phone in the weeks before surgery, with an in-person review by the anaesthetist on the morning of admission to hospital.
Photography
All surgical patients are photographed at consultation as part of the medical record. These photographs are kept confidentially within the practice and are not used for any other purpose without specific written permission from the patient.
Costs and Medicare

The practice provides a written quote at the second consultation, covering surgical fees, anaesthetic fees, hospital fees, and any associated costs.
Medicare eligibility for body contouring procedures is assessed individually at consultation and depends on specific clinical criteria. Some patients qualify for partial Medicare rebates; others do not. The eligibility position for a given case is confirmed during the consultation pathway.
The Hospital and Recovery
Maitland Private Hospital

I perform all surgical procedures at Maitland Private Hospital in the Hunter Valley, NSW. The hospital provides 24-hour doctor cover and on-site intensive care.
For this kind of surgery, the on-site ICU matters. Hybrid circumferential abdominoplasty, Fleur-de-Lis, belt lipectomy, and the longer combined operations are physiologically demanding procedures, particularly for post-bariatric patients. Operating at a hospital where intensive care is available on site, rather than transferred from another facility, is part of how I manage the operative risk profile for this cohort.
Hospital stays by procedure

Length of stay varies by procedure:
- Standard abdominoplasty or similar single procedure: 1 to 3 days
- Belt lipectomy / circumferential body lift: 3 to 5 days
- Hybrid circumferential abdominoplasty: 5 to 7 days
Combined operations involving more than one region typically sit between these markers, depending on the specific combination. I see all surgical patients during daily rounds throughout their admission.
Early recovery: the first two weeks

The first two weeks after surgery are the most intensive period of follow-up. Patients are seen at the practice 2 to 3 times per week during this period for:
- Wound and dressing review by the nurse and doctor
- LED light therapy
- Dressing changes
- Symptom and pain management review
- Adjustment of activity advice as recovery progresses
The PICO negative-pressure dressings used after surgery are typically replaced with Hypafix tape around day 7.
Standard follow-up appointments
After the intensive first two weeks, patients are seen for follow-up review at 1 month, 3 months, 6 months, and 12 months post-surgery. These appointments review scar progression, functional recovery, and any matters the patient wants to discuss.
For patients travelling from a distance
Patients travelling from Sydney, interstate, or rural areas typically plan for a local stay of 7 to 10 days following surgery. This covers the immediate post-operative period and the first round of intensive follow-up at the practice. After this initial period, patients can usually return home with their care coordinated through their GP and supplemented by telehealth review where clinically appropriate.
The 1-month, 3-month, 6-month, and 12-month follow-up appointments can typically be conducted by telehealth for distant patients, with in-person review at the practice arranged where clinically required.
Risks

All surgery carries risk. Body contouring after major weight loss carries a defined set of general surgical risks plus procedure-specific complications, and post-weight-loss patients have specific risk factors that need to be considered when planning surgery. The information below is general; individual risk profile is assessed at consultation.
General surgical risks
Any operation under general anaesthetic carries certain general risks. These include:
- Bleeding during or after the operation
- Infection of the surgical wound or surrounding tissue
- Deep vein thrombosis (DVT) and pulmonary embolism (PE), where blood clots form in the deep veins of the legs and may travel to the lungs
- Anaesthetic complications, including reactions to anaesthetic agents
- Cardiovascular and respiratory complications during or after surgery
These risks are present for any surgical procedure performed under general anaesthetic. Their relative likelihood varies depending on the patient’s medical history, the operation being performed, and the operative time involved.
Procedure-specific risks
Body contouring operations carry their own specific risks beyond the general surgical risks. These include:
- Wound healing complications, including delayed healing or wound breakdown along the incision lines
- Seroma (collection of fluid beneath the skin)
- Haematoma (collection of blood beneath the skin)
- Scar issues, including hypertrophic scarring, keloid formation, scar widening, or scar asymmetry
- Asymmetry of contour between left and right
- Sensory changes in the skin around the surgical area, including temporary or permanent numbness
- Skin necrosis (tissue loss), particularly along incision edges
- Need for revision surgery to address residual loose skin, scar issues, or asymmetry
The likelihood of each of these complications varies depending on the procedure, the volume of tissue removed, and the patient’s individual healing characteristics.
Risk factors specific to post-weight-loss patients
Patients undergoing body contouring after major weight loss have several risk factors that are specific to this group:
- Nutritional vulnerability. Many post-bariatric patients carry undiagnosed nutritional deficiencies that increase wound healing complications and infection risk if uncorrected before surgery.
- Reduced skin elasticity. Skin that has been stretched for years has lower elastic recoil after surgery, which can affect scar position, contour, and the rate of post-operative skin retraction.
- Comorbidity burden. Many patients in this group have associated medical conditions (diabetes, sleep apnoea, hypertension, anaemia) that need to be optimised before elective surgery to reduce complication risk.
- Weight stability. Surgery performed before weight has stabilised may compromise the result and increase the likelihood of revision.
How risk is managed in this practice
Several elements of the consultation and surgical pathway described elsewhere on this page are designed specifically to manage the risk profile of this cohort:
- The two-consultation structure with pre-operative blood tests identifies and corrects nutritional deficiencies before surgery
- The pre-operative supplement protocol (Tier 1 universal, Tier 2 individualised on bloods) addresses the most common deficiencies
- Weight stability requirements (minimum 6 months, 12 to 18 months post-bariatric) reduce the risk of result compromise
- Smoking cessation requirements (minimum 6 weeks pre-operatively) reduce wound healing complication risk
- Operating at a hospital with on-site intensive care provides a margin for managing the rare cases where intensive support is required post-operatively
These measures reduce risk; they do not eliminate it. All surgery carries inherent risk regardless of preparation.
Note on individual variation
Results of surgery vary between patients. The information above is general and educational; specific risks relevant to a given patient and a given procedure are discussed in detail at consultation, where individual risk factors are assessed. The decision to proceed with surgery rests with the patient after this discussion.
Educational content only. Not a substitute for medical advice from a qualified practitioner.
Frequently Asked Questions
Why would a Sydney patient travel to the Hunter Valley for body contouring?
Patients give a range of reasons. Common ones include the practice’s sub-specialty focus on body contouring after major weight loss, the structured pre-operative optimisation protocol (which addresses nutritional deficiencies common in this cohort before surgery), the continuity of having the same surgeon plan and perform every stage of multi-region work, and the on-site intensive care available at Maitland Private Hospital for the more demanding operations. For some patients, travelling away from home for surgery and the early recovery period also offers a degree of privacy from local social and professional networks during recovery.
How does the consultation process work for distant patients?
The standard model is two consultations: one conducted by telehealth (typically the first), and one conducted in person at Maitland Private Hospital (typically the second). The in-person consultation is generally scheduled close to the surgical decision point, when blood test results are also available and the surgical plan is being finalised. For some patients, the in-person component is consolidated onto the day before surgery. The arrangement is decided on a case-by-case basis. At least one consultation must take place in person before surgery is booked.
How long do I need to stay near the hospital after surgery?
A local stay of 7 to 10 days following surgery is typically recommended for distant patients. This covers the hospital admission and the first round of intensive post-operative follow-up at the practice (2 to 3 visits per week during the first two weeks). After this initial period, patients can usually return home, with ongoing care coordinated through their GP and supplemented by telehealth review at the practice where clinically appropriate.
Can my GP coordinate follow-up care closer to home?
Yes. Once the early recovery period is complete and the patient has returned home, ongoing care is typically coordinated with the patient’s GP. The practice provides correspondence to the GP outlining the procedure performed, post-operative findings, and the recommended follow-up schedule. Standard follow-up reviews at 1, 3, 6, and 12 months can usually be conducted by telehealth for distant patients, with in-person review at the practice arranged where clinically required.
What if I need staged surgery: can it be planned around my travel and recovery support?
Yes. For patients undergoing staged surgery, the spacing between stages is decided as part of the surgical plan at the second consultation. Travel logistics, recovery support availability, and time available off work are among the factors considered, alongside the clinical factors (operative time, BMI, blood results, scar healing in adjacent regions). Stages are typically spaced six to twelve months apart, with the specific timing individualised to each patient.
Will I need a GP referral?
Yes. A GP referral is required for all surgical consultations at the practice, including initial telehealth consultations.
Next Steps
The next step for patients considering a comprehensive surgical plan across multiple regions is a consultation. The two-consultation pathway described above is structured to allow time for clinical assessment, blood-guided nutritional preparation, and a considered surgical decision before any commitment.
A GP referral is required for all consultations.
Or call the clinic on (02) 4934 5700.
Dr Beldholm’s companion guide, 7 Surgical Options for Loose Skin After Weight Loss, covers the seven procedures most often considered after significant weight loss. It explains how to identify your pattern of loose skin, what each procedure involves, and what to expect from recovery.

