Brachioplasty (Arm Lift Surgery)
Surgical options for loose or excess skin of the upper arms, including after significant weight loss. Performed by Dr Bernard Beldholm FRACS, Specialist Surgeon.
Brachioplasty is not one operation. Four options exist, and the appropriate one depends on the pattern of skin laxity and the distribution of fat within the upper arm. Which option is right for you is determined at consultation through physical assessment.
The Beldholm Approach

When a patient comes to me with concerns about loose or excess upper arm skin, the question is which brachioplasty technique fits their anatomy. Brachioplasty is not a single procedure. The clinical work sits in matching the technique to the pattern, preparing the patient properly, and doing the operation well in one well-planned admission.
Three principles guide how I approach brachioplasty.
1. The procedure matches the pattern
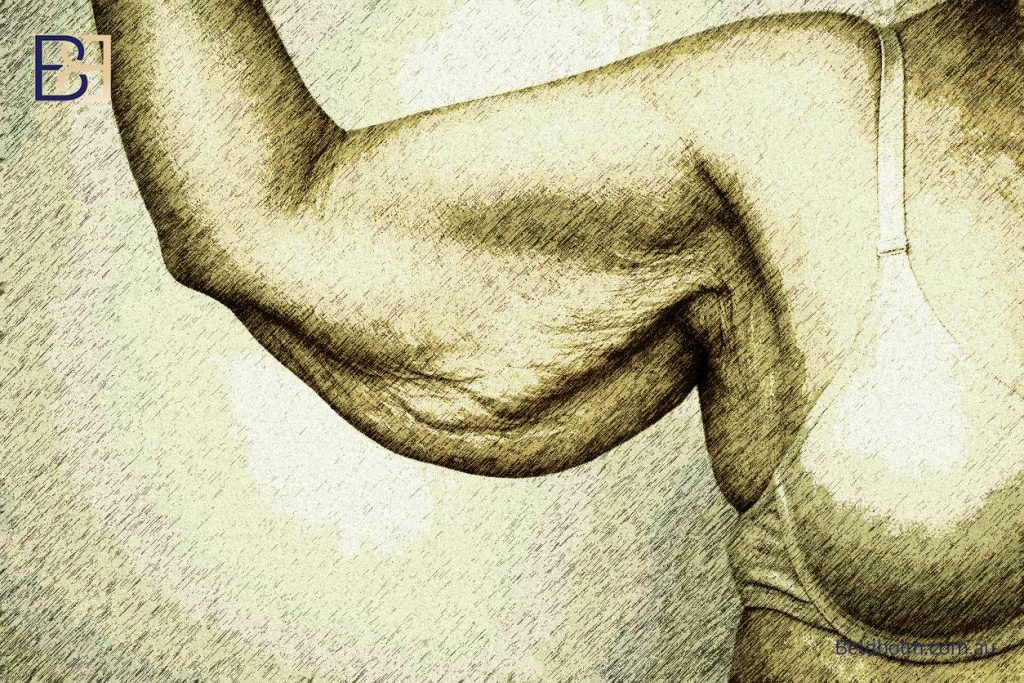
Not every arm needs the same incision. A patient with mild laxity confined to the axilla needs a different operation from a patient whose excess skin extends from armpit to elbow, and both are different from the post-massive-weight-loss patient whose skin laxity continues onto the lateral chest wall. The four options set out later on this page exist because upper-arm anatomy after weight change is not uniform.
I assess each arm individually at consultation. Which option is appropriate is determined by the pattern of skin laxity, the distribution of fat within the arm, and skin quality. The answer is sometimes a smaller operation than the patient expected, and sometimes a larger one.
2. One operation, well planned
Where the anatomy allows it, I prefer one well-planned operation over staged procedures. Bilateral brachioplasty (both arms operated on together) is the standard approach. The real clinical decision is what to include in that one operation. Where skin laxity extends onto the lateral chest wall, I perform the chest extension in the same operation as the arm work, not as a second admission.
Brachioplasty can also form part of a wider post-weight-loss body contouring plan. Whether it is combined with other procedures or staged depends on medical factors, overall operative time, and what is clinically appropriate for the individual patient. That is a discussion I have with each patient based on their full clinical picture.
3. Preparation before the operation

Post-weight-loss patients come to consultation with nutritional gaps that most of them do not know they have. Low levels of protein stores, iron, vitamin D, B12, and zinc are the norm rather than the exception after significant weight loss or bariatric surgery. These gaps affect wound healing, infection risk, and recovery.
I address preparation before surgery, not after. For patients having Full or Extended Brachioplasty after significant weight loss, that means starting a core supplement routine at planning, blood testing to identify specific deficiencies, and correcting what needs correcting before the operation is booked. For smaller operations the preparation is lighter, but the principle is the same: a well-prepared patient heals better.
Is Brachioplasty Right for You?
Whether brachioplasty is appropriate for you, and when to have it, depends on individual factors. The points below are general guides. Final suitability and timing are determined at consultation.
When brachioplasty may be appropriate
Brachioplasty is commonly considered when:
- weight has been stable for at least six months
- there is loose or hanging upper arm skin that does not improve with exercise or weight training
- excess skin causes skin irritation or rubbing within folds
- fitted or short-sleeved clothing is limited by arm contour
- there are concerns about upper arm shape after significant weight loss or bariatric surgery
- the arms appear out of proportion with the rest of the body after weight loss
Loose skin of the upper arms is a physical consequence of reduced skin elasticity. Toning exercises build muscle beneath the skin but do not remove excess skin itself. Non-surgical skin tightening has a limited role in true excess-skin patterns. Where excess skin is the concern, surgical removal is the main option.
Reasons to wait
Brachioplasty is generally deferred when:
- weight is still fluctuating by more than one to two kilograms per month, or an active weight-loss program is continuing
- bariatric surgery was performed less than twelve to eighteen months ago
- pregnancy is current or planned in the near future
- smoking has not been stopped before surgery (smoking significantly increases wound-healing risks)
- diabetes is not well controlled
- an underlying health condition affecting healing is not yet stable
Deferral does not mean surgery is ruled out. It means timing matters. In most of these situations, brachioplasty can still be appropriate once the underlying factor is addressed.
Matching the Procedure to Your Pattern
Four brachioplasty options cover the range of upper arm skin and fat presentations. The option that applies to you is determined at consultation through physical assessment of each arm.
A short vocabulary
- Brachioplasty: surgical removal of excess upper arm skin
- Suction-assisted lipectomy (SAL): removal of fat through small incisions, also called liposuction
- Axilla: the armpit area
- Lateral chest wall: the side of the chest beneath the armpit, extending toward the lateral breast
The four options
Each option addresses a different pattern of excess skin, excess fat, or both. The options are set out from least to most extensive.
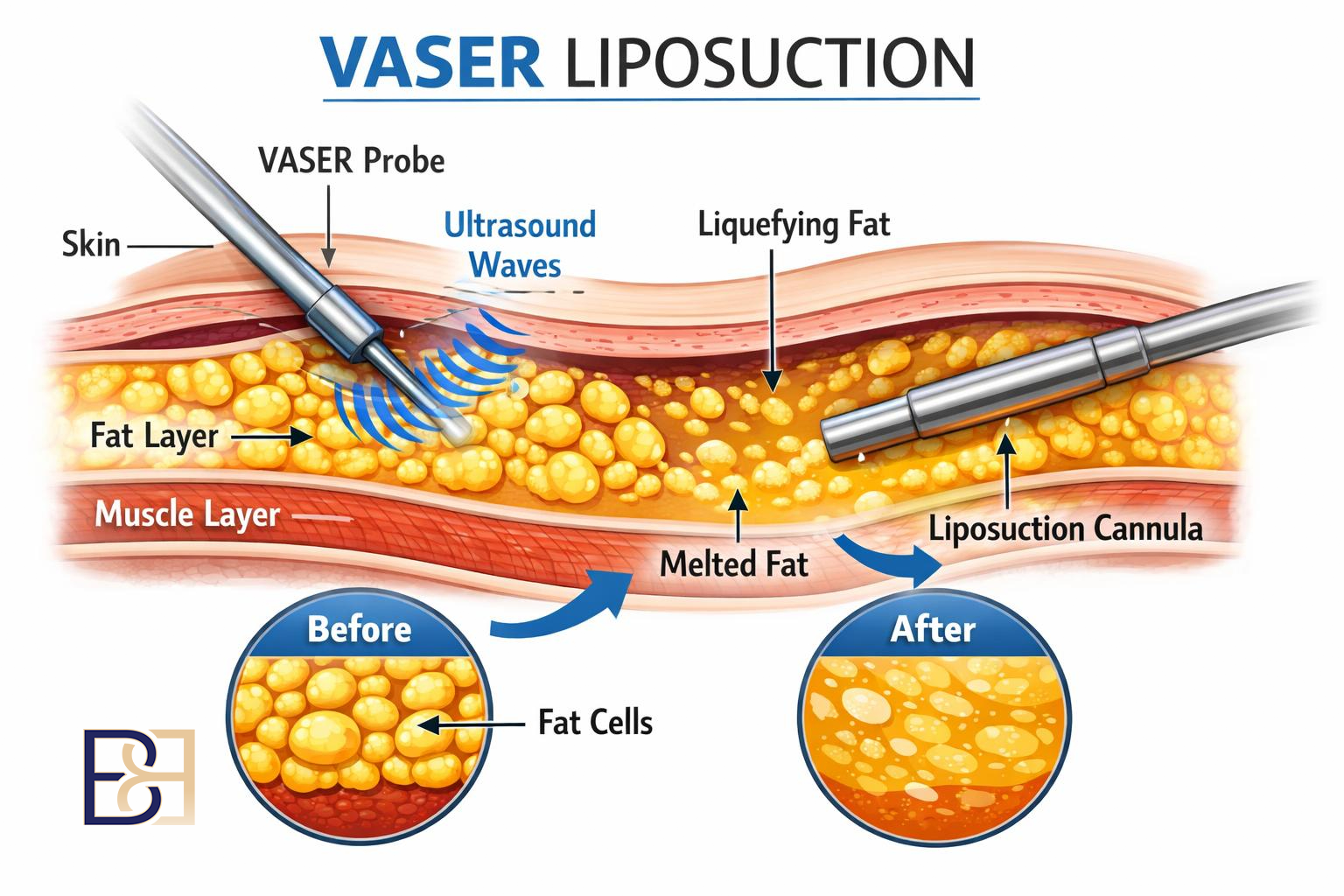
1. Liposuction only (suction-assisted lipectomy)
Best for: excess upper arm fat where skin quality is good and skin laxity is minimal. This pattern is uncommon in post-weight-loss patients and more typical in patients without significant weight change.
Incisions: small entry points, usually a few millimetres in length.
Scar: minimal, placed in hidden skin creases where possible.
Limitation: liposuction removes fat but does not remove excess skin. Where skin laxity is present, skin will not retract sufficiently after fat removal alone.
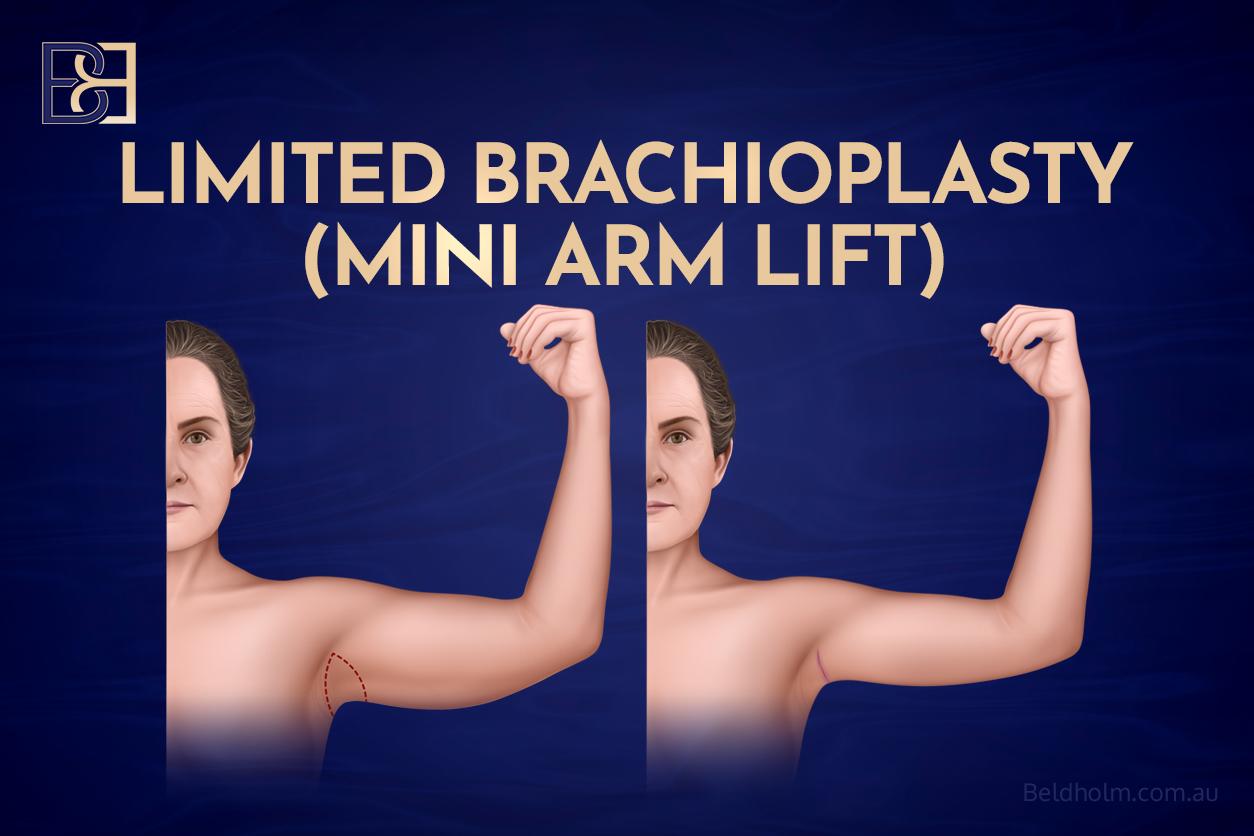
2. Limited Brachioplasty
Best for: mild skin laxity confined to the upper inner arm near the axilla. This suits patients whose skin excess does not extend far down the arm toward the elbow.
Incisions: placed within or close to the axilla, positioned to fall within the natural creases of the armpit.
Scar: shorter than Full Brachioplasty and positioned to be less visible in everyday clothing.
Limitation: the amount of skin that can be removed is restricted by the shorter incision. Limited Brachioplasty is not suitable for patients with skin laxity extending along the length of the upper arm.

3. Full Brachioplasty (or standard brachioplasty)
Best for: moderate to severe loose or hanging skin along the length of the upper arm, extending from the axilla toward the elbow. This is the most common pattern after significant weight loss.
Incisions: run from the axilla along the inner aspect of the upper arm toward the elbow. Incision placement is planned so the resulting scar sits along the inner arm rather than the more visible outer arm.
Scar: longer than Limited Brachioplasty. The scar is visible but placed in the least conspicuous position on the arm. Scar quality matures over twelve to eighteen months.
Limitation: the scar is the trade-off for the amount of skin that can be removed. Patients choosing Full Brachioplasty accept a longer scar in exchange for a meaningful reduction in arm skin excess.
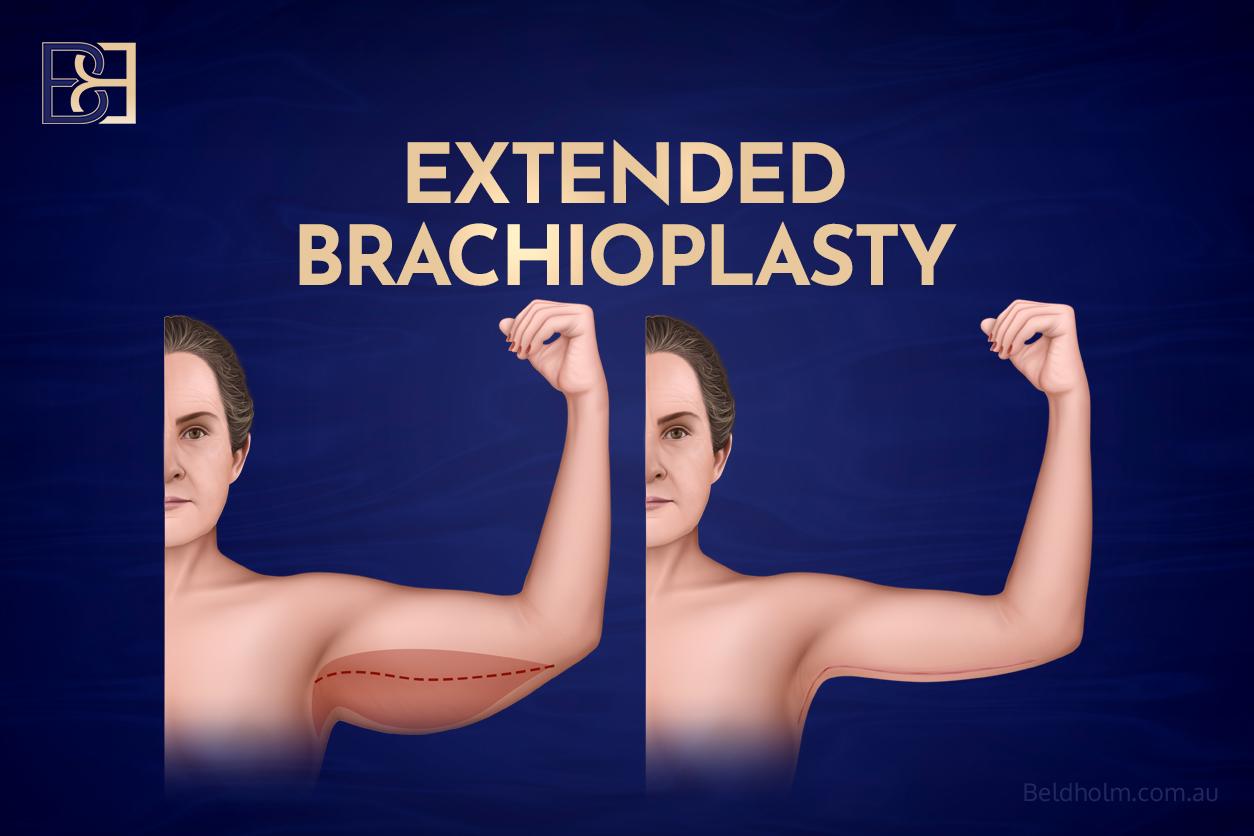
4. Extended Brachioplasty
Best for: skin laxity that does not stop at the armpit. In patients after major weight loss, excess skin often continues from the upper arm onto the lateral chest wall and toward the lateral breast. Extended Brachioplasty addresses both areas in one operation.
Incisions: continue from the arm incision across the axilla and onto the lateral chest wall. The exact extent is planned based on the pattern of skin laxity.
Scar: longer again than Full Brachioplasty, extending onto the chest. Placement is planned to sit beneath everyday clothing where possible.
Limitation: the longer incision means longer healing time and a larger area of scar. It is reserved for patients whose pattern genuinely extends onto the chest wall, as shorter options cannot address chest laxity.
Where fat is also present
Where upper arm fat is present alongside skin laxity, suction-assisted lipectomy can be combined with Limited, Full, or Extended Brachioplasty in the same operation. Combined brachioplasty with SAL is a common approach for post-weight-loss patients who have residual fat in the upper arm as well as loose skin.
Which option, or combination, is appropriate for your arms is determined at consultation.
Before Your Consultation
Reading through the options in more detail before your consultation means you arrive with specific questions rather than general ones. Dr Beldholm’s patient guide covers the four brachioplasty options in the same structure used above, with illustrations of each technique and a short comparison of incision length, scar location, and the patterns each option addresses.
4 Brachioplasty (Arm Lift) Options You Need to Know if You Have Loose Underarm Skin
A patient guide covering:
- Liposuction only (suction-assisted lipectomy)
- Limited Brachioplasty
- Full Brachioplasty
- Extended Brachioplasty
For each option: who it suits, where the incisions sit, what the scar looks like, and the main limitations to be aware of.
Educational content only. Not a substitute for medical advice. Consultation required to determine suitability for surgery.
Book your appointment online now
About Dr Bernard Beldholm

I am a Specialist Surgeon with more than fifteen years of surgical practice. My work focuses on body contouring surgery after significant weight loss and after pregnancy, alongside breast surgery and facial surgery. Brachioplasty forms a regular part of my operative practice, both as a standalone procedure and as part of wider post-weight-loss body contouring plans.
I operate at Maitland Private Hospital in the Hunter Valley, NSW. The hospital provides 24-hour medical cover and has an on-site intensive care unit, which matters for the patients I look after, particularly those having larger body contouring operations after weight loss.
A GP referral is required before your first consultation with me. Referrals are standard practice in Australia for specialist surgical consultations, and an independent referral from your GP supports your clinical assessment.
Alongside clinical practice, I contribute to the professional community through conference presentations and peer-reviewed publication on body contouring topics. I also work closely with bariatric surgeons and GP networks who refer patients to me for surgical management of post-weight-loss skin concerns.
Dr Bernard Beldholm M.B.B.S, B.Sc (Med), FRACS, Specialist General Surgeon. AHPRA Medical Registration number: MED0001186274.
Preparing for Surgery

How much preparation your surgery needs depends on which operation you are having and whether you have had significant weight loss.
For patients having Limited Brachioplasty or liposuction only, preparation is straightforward. Standard pre-operative checks apply, including stopping fish oil and certain other supplements before surgery, and confirming weight stability. The detail is discussed at consultation.
For patients having Full Brachioplasty or Extended Brachioplasty after significant weight loss, preparation is more detailed and starts weeks before the operation. The rest of this section covers that group.
Why preparation matters after significant weight loss
Post-weight-loss patients come to consultation with nutritional gaps that most of them do not know they have. Low protein stores, iron, vitamin D, B12, zinc, and other micronutrients are common after significant weight loss and near-universal after bariatric surgery. These gaps affect wound healing, infection risk, and recovery.
A larger operation on a nutritionally depleted patient carries higher risk than the same operation on a well-prepared patient. That is the reason I address preparation before the operation rather than after.
Weight stability

Before I book a Full or Extended Brachioplasty, I want to see weight stability for at least six months. For patients who have had bariatric surgery, I prefer to wait at least twelve to eighteen months from the bariatric operation before body contouring. Operating on a patient whose weight is still changing produces a result that also changes over the following year, which defeats the purpose of the surgery.
Nutrition protocol

The nutrition protocol has two tiers.
Tier 1 (universal) for Full and Extended Brachioplasty post-weight-loss patients. These supplements are started at surgical planning, and at a minimum four weeks before surgery:
- whey protein isolate
- a complete multivitamin
- vitamin D3 with K2
- vitamin C
- zinc
Tier 2 (blood-guided). Pre-operative blood tests check levels of iron, vitamin B12, folate, vitamins A and B1, calcium, selenium, and magnesium. Where blood results confirm a deficiency, I add the relevant supplement before surgery and recheck where necessary.
Fish oil, vitamin E, and several herbal supplements increase bleeding risk and are stopped one week before surgery. Post-operative bloods are repeated at six to eight weeks.
You will leave your first consultation with a nutrition guide, a blood test request form, and the Tier 1 supplements to start. The detail of your specific protocol is finalised at the second consultation once blood results are back.
Consultation Process

My standard is at least two consultations before surgery. This gives both of us time to plan properly, review blood results, and answer questions without pressure. It is also aligned with current practice guidelines for surgical consultation in Australia.
Before your first consultation
A GP referral is required. Your GP assesses your general suitability for surgical consultation and provides an independent medical view that supports my clinical assessment.
First consultation
The first consultation takes about an hour. I will take your history and examine you, and standardised clinical photographs are taken with disposable garments in a private setting. We discuss the options set out on this page in the context of your specific anatomy, work through risks and recovery, and answer your initial questions.
You will leave the first consultation with:
- a nutrition guide specific to body contouring surgery
- a blood test request form (for post-weight-loss patients having Full or Extended Brachioplasty)
- the Tier 1 supplements to start
- clear direction on pathology collection
- an introduction to my surgical coordinator, who manages the non-clinical side of your booking
Second consultation
The second consultation happens two to four weeks after the first. We review your blood results and add any Tier 2 supplements that your pathology indicates. We confirm the surgical plan, answer any remaining questions, and my coordinator finalises your written quote at this point.
Telehealth for patients from afar
Patients travelling from outside the Hunter Valley can have their first consultation by phone or video. An in-person consultation is required before surgery, which is usually booked to coincide with pathology collection or on the day before the operation. The second consultation can also be conducted by phone or video depending on geography.
Anaesthetic consultation
For post-weight-loss patients having larger body contouring surgery, a routine pre-operative anaesthetic consultation is arranged by phone. The anaesthetist reviews your medical history, any medications, and any relevant medical weight-loss treatments you may be on. An in-person anaesthetic review takes place at the hospital on the day of admission.
Booking lead time
Typical booking lead time is one to three months from the second consultation to surgery. Longer operations and combined body contouring plans may need additional scheduling time.
GP referral required. Consultation required to determine suitability.
Hospital and Recovery
I operate exclusively at Maitland Private Hospital. The hospital provides 24-hour medical cover and has an on-site intensive care unit. For larger body contouring operations after weight loss, that infrastructure matters. I do daily ward rounds while my patients are admitted.
Hospital stay

Length of stay varies with the operation:
- Liposuction only (suction-assisted lipectomy): day procedure
- Limited Brachioplasty: day procedure
- Full Brachioplasty: day procedure or one night, depending on the extent of skin removed and your overall recovery on the day
- Extended Brachioplasty: typically one night, occasionally two depending on the extent of the operation
All operations are performed under general anaesthesia.
Early recovery
The first two weeks after surgery are the period of most active recovery. Dressings are in place, upper-body activity is restricted, and most patients take one to two weeks away from work depending on the type of work they do. Driving is restricted while you are not able to safely control a vehicle.
I review my patients intensively in the first two weeks. You can expect two to three nurse or doctor visits per week for wound checks, dressing changes, and any post-operative concerns.
Routine follow-up
Routine follow-up appointments are scheduled at one, three, six, and twelve months after surgery. All follow-up is included in the surgical fee. The twelve-month review covers final scar assessment.
Patients from afar
For patients travelling to the Hunter Valley for surgery, I recommend a local stay of seven to ten days for the initial recovery period. Beyond that, ongoing follow-up can be coordinated with your GP and supplemented with telehealth appointments.
Returning to exercise
Return to strenuous upper-body exercise is delayed until healing has progressed sufficiently. The exact timing depends on which operation you have had and how your individual recovery is going. Lighter activity (walking, lower-body cardio) usually resumes earlier. Specific guidance is given at your follow-up appointments.
Risks and Complications

All surgery carries risks. Brachioplasty is no exception. Risks must be understood and weighed against potential benefits before any decision to proceed.
The information below is a general summary. Risks specific to your individual circumstances are discussed in detail at consultation, where your medical history, the option you are considering, and your overall risk profile are reviewed together. Informed consent for surgery is a process that takes place over both pre-operative consultations.
General surgical risks
The following risks apply to most surgical procedures performed under general anaesthesia:
- bleeding during or after the operation
- haematoma (collection of blood under the skin) requiring further intervention
- infection at the surgical site
- adverse reaction to anaesthetic agents
- deep vein thrombosis and pulmonary embolism
- wound healing problems
- need for further surgery to address a complication
Risks specific to brachioplasty
Brachioplasty involves an incision on the upper arm, dissection of skin and subcutaneous tissue, and closure under tension. The following risks are particularly relevant:
- seroma (collection of fluid under the skin) requiring drainage
- numbness or altered sensation along the inner aspect of the arm
- delayed wound healing along the length of the incision
- widening or thickening of the scar over time
- hypertrophic or keloid scarring in patients prone to these scar types
- asymmetry between the two arms
- contour irregularity along the inner arm
- dog-ear formation at the ends of the incision, occasionally requiring revision
- temporary or longer-lasting swelling of the forearm and hand
- injury to nerves or vessels in the upper arm
For Extended Brachioplasty, the same risks apply along the chest extension, with the additional consideration of a longer incision and a larger area of dissection.
Where suction-assisted lipectomy is included
Where SAL is combined with brachioplasty, additional risks specific to liposuction may occur, including contour irregularity, prolonged swelling, and seroma at the liposuction sites.
Risks more relevant to post-weight-loss patients
Post-weight-loss patients may have reduced skin quality, lower nutritional reserves, and a higher overall risk of wound healing problems compared with non-weight-loss patients. Pre-operative nutritional optimisation, as set out in section seven, is one part of how this risk is addressed. Even with optimisation, complication rates in this group are higher than in patients without significant weight history.
Scarring
Brachioplasty leaves a permanent scar. The length of the scar depends on which option is performed. The final appearance of the scar varies between individuals and depends on factors including genetics, skin type, smoking history, and post-operative care. Scars typically mature over twelve to eighteen months, becoming softer and lighter over that time, though they do not disappear.
Outcomes vary
Individual results from brachioplasty vary, and the outcome experienced by one patient does not predict the outcome for another. Factors influencing the result include the option performed, individual skin and tissue characteristics, post-operative wound healing, scar maturation, and weight stability after surgery.
All surgery carries risks. Results vary. The above is a general summary; risks specific to your situation are discussed in detail at consultation.
Frequently Asked Questions
How much does brachioplasty cost in Australia?
The total cost of brachioplasty depends on which option is performed, the length of operating time, hospital fees, anaesthetist fees, and whether suction-assisted lipectomy is included. Surgical fees, hospital and anaesthetist estimates, and any GST applicable to cosmetic cases are confirmed in a written quote provided after the second consultation. A personalised quote requires assessment, so a meaningful figure cannot be given before consultation.
Is brachioplasty covered by Medicare?
Medicare may contribute to the cost of brachioplasty in patients who meet specific clinical criteria, typically related to skin excess after significant weight loss and associated symptoms such as recurrent skin irritation. Eligibility is assessed individually at consultation, and depends on clinical findings, history, and supporting documentation. Where Medicare criteria are met, private health insurance may also contribute. Item-specific details and out-of-pocket figures are confirmed in your written quote, not on this page.
What is the difference between Limited, Full, and Extended Brachioplasty?
The three brachioplasty options differ in the length of the incision and the area of skin that can be removed.
- Limited Brachioplasty addresses mild skin laxity confined to the area near the axilla. The incision sits within or close to the armpit.
- Full Brachioplasty addresses moderate to severe skin laxity along the length of the upper arm. The incision runs from the axilla toward the elbow.
- Extended Brachioplasty addresses skin laxity that continues from the upper arm onto the lateral chest wall, common after major weight loss. The incision continues from the arm onto the chest.
Which option is appropriate is determined at consultation by physical assessment of the pattern of skin laxity in each arm. The four options are described in detail in section four of this page.
How long is recovery after brachioplasty?
Recovery timelines vary between patients and between the four options. As a general guide, the first one to two weeks involve restricted upper-body activity and time away from work for most patients. Two to three nurse or doctor visits per week take place during this period for wound checks and dressing changes. Lighter activity often resumes from around two to three weeks. Return to strenuous upper-body exercise is delayed until healing has progressed sufficiently, with timing confirmed at follow-up appointments. Routine follow-up continues at one, three, six, and twelve months. Individual recovery varies.
Will I have a visible scar?
Yes. Brachioplasty requires an incision to remove skin, and a scar is unavoidable. The length and location of the scar depend on which option is performed. Incisions are planned to place the resulting scar in the least conspicuous position appropriate to the option being performed, typically along the inner aspect of the arm and within the natural creases of the axilla where possible. Scars mature over twelve to eighteen months and the final appearance varies between individuals.
Can brachioplasty be combined with other body contouring procedures?
In some patients, brachioplasty can be performed in the same operation as other body contouring procedures, including abdominoplasty, breast surgery, or thighplasty. Whether combination is appropriate or whether procedures should be staged depends on overall operating time, the patient’s medical fitness for a longer operation, and the clinical priorities. Combinations are not offered as packaged or discounted bundles. Each procedure is quoted individually, and the surgical plan is agreed at consultation.
Next Steps
Brachioplasty is not a single procedure. The right option for you, whether that is liposuction only, Limited Brachioplasty, Full Brachioplasty, or Extended Brachioplasty, with or without combined SAL, is determined by the pattern of skin laxity and fat in your arms. That assessment happens at consultation.
A GP referral is required before your first consultation. Telehealth first consultations are available for patients travelling from outside the Hunter Valley.
Or call the clinic on (02) 4934 5700.
4 Brachioplasty (Arm Lift) Options You Need to Know if You Have Loose Underarm Skin
GP referral required. Consultation required to determine suitability. Results vary. All surgery carries risks.

