Augmentation Mastopexy (Breast Lift with Implants)
A combined breast lift (Mastopexy) and implant procedure for women who want both the lift and added upper-pole fullness, performed as one operation where clinically suitable.
My Approach to Combined Breast Lift (Mastopexy) and Implants

Most patients who come to me for a breast lift (Mastopexy) with implants ask the same thing first: can it be done in one operation? Where it is clinically suitable, my preferred path is yes. Combined Augmentation Mastopexy means one anaesthetic, one recovery period, and one set of fees. For most patients I see, this is the right approach.
There are situations where a staged plan is safer. The risk of complications rises with the size of the lift required. Patients with grade 3 ptosis, and many post-weight-loss patients with substantial loose skin requiring large excisions, may be better suited to a staged approach: Mastopexy first, then implant placement approximately six months later, once the tissues have settled.
Is This Combination Likely to Apply to you?
Augmentation Mastopexy is most often considered by women who notice both a change in breast position and a loss of breast tissue volume. Common pathways include:
- After pregnancy and breastfeeding, where breast tissue volume has decreased and the nipple-areola complex now sits lower on the breast mound
- After significant weight loss, where breast tissue volume has reduced and the skin envelope has loosened
- With age, where breast tissue volume has gradually changed and skin elasticity has reduced
This combination is for patients who want both elements addressed: a lift to re-position the breast, and an implant to add upper-pole fullness beyond what their own tissue provides. Women who want only the lift, or only added volume, may be better suited to a different procedure. The four main paths are covered in the patient guide.
Factors that may defer surgery
Several physical factors may mean surgery is not appropriate at this time. These are discussed at consultation, and may include:
- Weight stability. For patients who have lost significant weight, or who are post-pregnancy, weight should be stable for approximately six months before surgery. Ongoing weight change after surgery affects the result.
- Smoking. Smoking impairs wound healing and increases complication rates. A period of cessation before and after surgery is required.
- General health. Conditions such as poorly controlled diabetes, anaemia, or uncontrolled blood pressure are addressed before surgery is considered.
- Family planning. Future pregnancy and breastfeeding can affect breast position and volume after surgery. Patients who plan further pregnancies may prefer to defer.
- Breastfeeding. A period of approximately six months from the cessation of breastfeeding is recommended before breast surgery.
Suitability is assessed individually at consultation following physical examination and discussion of medical history.
Matching the Procedure to your Pattern
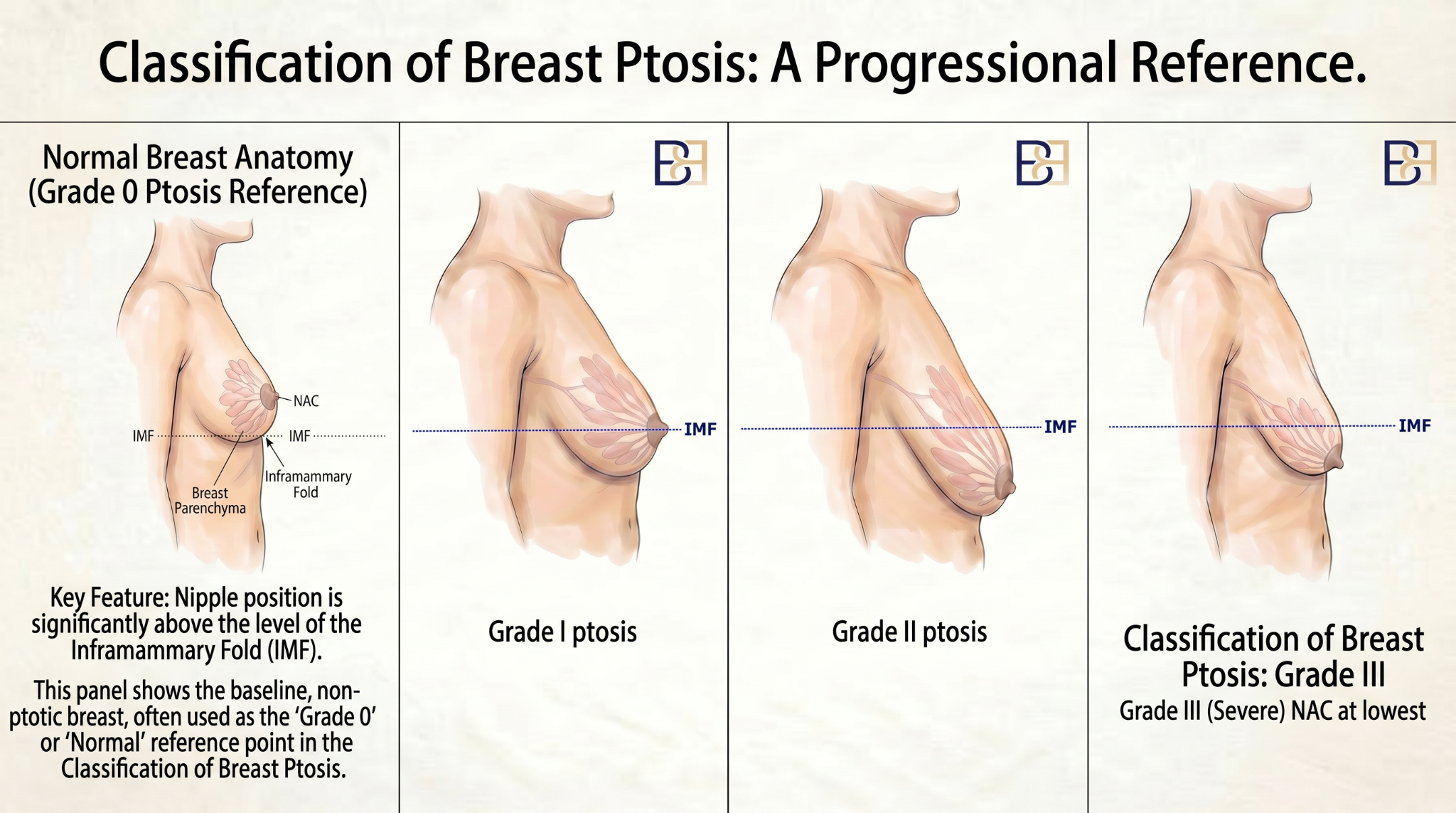
The right path through Augmentation Mastopexy depends on four clinical factors. These are assessed at consultation and shape both the technique used and whether the procedure is performed in one operation or two.
Degree of breast ptosis. Breast ptosis is graded by where the nipple-areola complex sits relative to the inframammary fold. Higher grades indicate a larger lift, with more tissue re-positioning and a longer incision pattern.
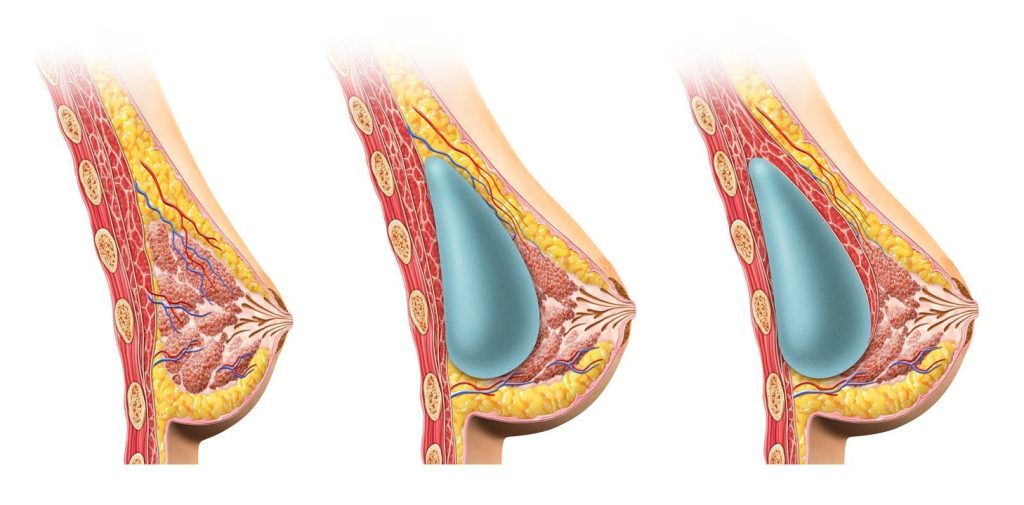
Breast tissue volume. The amount of native breast tissue present. Where volume is reduced and additional upper-pole fullness is wanted, an implant is added. Where volume is adequate, an implant may not be needed.
Skin envelope quality and laxity. Looser, less elastic skin (common after pregnancy or significant weight loss) requires more excision and changes how the closure heals.
Scar position and quality. The patient’s individual healing pattern influences technique selection and scar planning.
Two patterns most commonly apply for combined breast lift (Mastopexy) and implants:
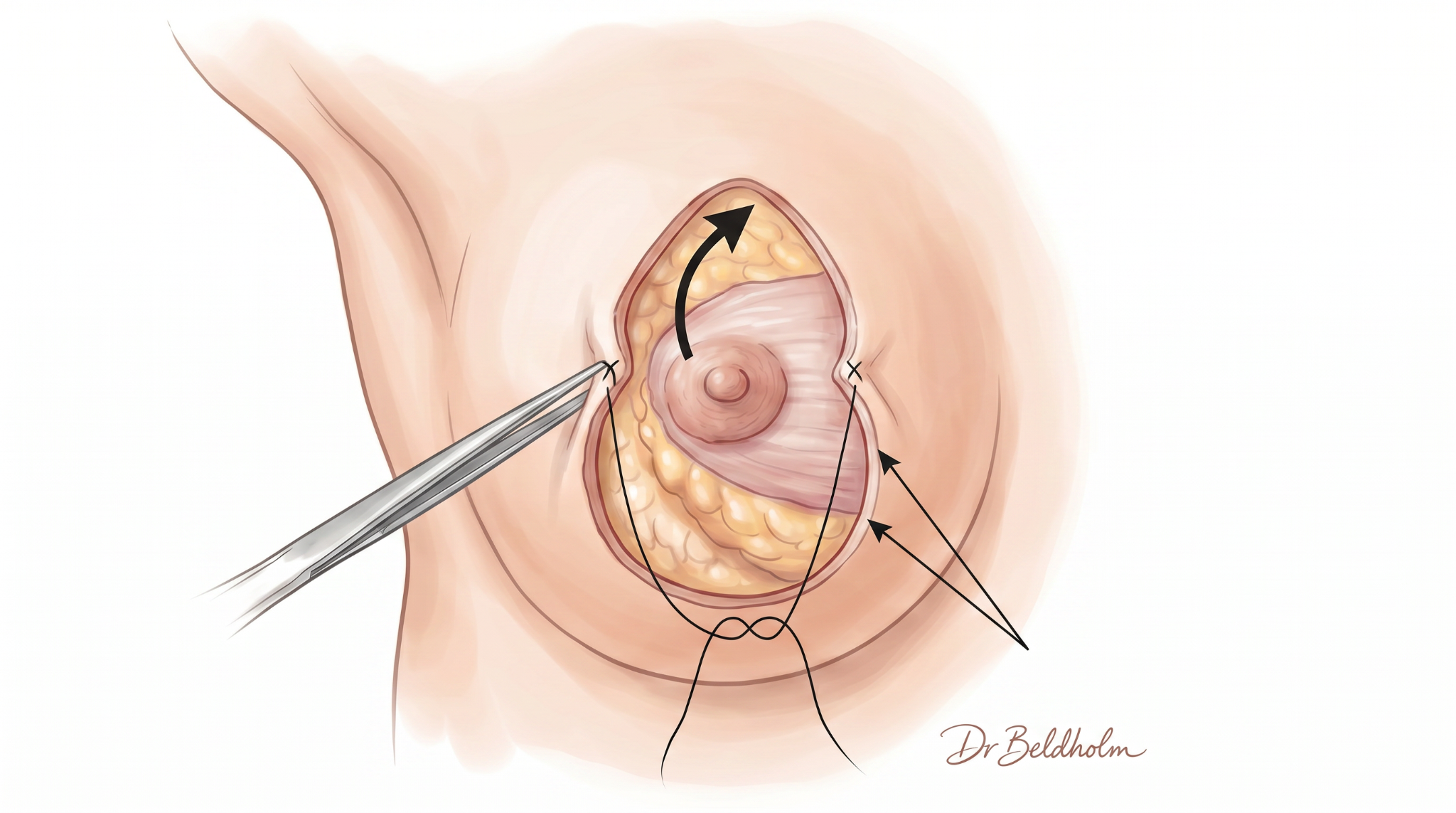
Pattern A: Combined Augmentation Mastopexy in one operation
For patients with grade 1 or grade 2 ptosis, adequate but reduced breast tissue volume, and a wish for upper-pole fullness beyond what their own tissue provides. The lift and the implant are performed in the same operation, through the same incisions, with no additional scars required for the implant placement.
This is the preferred path when clinically suitable. One anaesthetic, one recovery period, one set of fees.
Pattern B: Staged Mastopexy and Augmentation
For patients where the lift component is large and combining the procedures in one operation carries a higher risk of complications. This typically applies to patients with grade 3 ptosis, and many post-weight-loss patients with substantial loose skin requiring large excisions.
Mastopexy is performed first as a standalone operation. Implant placement is performed approximately six months later, once the tissues have settled. Two operations, two recovery periods, two sets of fees. The trade-off is a lower complication risk profile for patients where the lift component is large.

A note on cost classification
Augmentation is always classified as cosmetic surgery. The implant component of any Augmentation Mastopexy does not attract a Medicare rebate.
A standalone Mastopexy may attract a Medicare item number where it meets specific clinical criteria, assessed individually at consultation. This means the cost picture differs between the two approaches:
- Single-stage combined. The Medicare item number for Mastopexy specifically excludes operations performed with implants. The combined operation is classified as cosmetic in full.
- Staged. The first-stage standalone Mastopexy may attract a Medicare item number where it qualifies. The second-stage implant placement is cosmetic.
Full detail on Medicare and private health fund implications is provided in the FAQ.
Other Mastopexy paths
Some patients who consider lift with implants are, on assessment, better suited to Mastopexy alone, or to Mastopexy with Auto-Augmentation, where existing breast tissue is reshaped to a higher position without an implant. The four main Mastopexy paths are covered in the patient guide.
Free Patient Guide: 4 Mastopexy (Breast Lift) Options After Pregnancy or Weight Loss
Most patients arriving at this page are weighing the same question: which Mastopexy path matches my situation, and is adding implants the right choice for me?
This guide covers the four main Mastopexy approaches in detail, including the two that involve implants:
- Standard Mastopexy
- Mastopexy with Auto-Augmentation (using your own tissue, no implant)
- Combined Augmentation Mastopexy in one operation
- Staged Mastopexy and Augmentation
It also explains how Reduction Mammoplasty (Breast Reduction) is a different procedure, and where Medicare may apply.
Your details will not be shared. Unsubscribe anytime.
About Dr Beldholm

Dr Bernard Beldholm is a FRACS Specialist Surgeon with over 15 years of surgical experience. His clinical focus is post-pregnancy and post-weight-loss body contouring, and breast surgery.
Dr Beldholm operates at Maitland Private Hospital, which provides 24-hour doctor cover and on-site ICU. A GP referral is required to attend a consultation.
“Combined breast lift (Mastopexy) and implants is the right operation for many patients. For others, staging is safer. The most important part of consultation is working out which path applies to you.”
Dr Bernard Beldholm
Dr Bernard Beldholm M.B.B.S, B.Sc (Med), FRACS, Specialist General Surgeon. AHPRA Medical Registration number: MED0001186274.
Preparing for Surgery

Combined Augmentation Mastopexy is a longer, more complex operation than either Mastopexy alone or Breast Augmentation alone. The preparation that I ask of patients reflects that.
Several factors are addressed before I confirm a surgery date:
Weight stability. For post-pregnancy and post-weight-loss patients, weight should be stable for approximately six months. Ongoing weight change after surgery affects breast position and volume. Patients still losing weight are advised to reach a stable weight before booking.
Smoking and nicotine. Smoking impairs wound healing and increases the risk of complications. Patients are asked to stop smoking and using nicotine products for a period before and after surgery.
General health. Conditions such as diabetes, anaemia, and high blood pressure are reviewed and optimised before surgery. Blood work is ordered where indicated. Patients on blood-thinning medication are managed in consultation with their prescribing doctor.
Implant decisions. Choice of implant shape, size, and projection is made at consultation, after physical examination and discussion of your goals. 3D imaging is part of the consultation, alongside physical sizing with implants in a sports bra. Patients can return to try selected implants again before finalising their choice.
Practical preparation. Patients are given written pre-operative instructions covering medications to pause, fasting, what to bring on the day, and arrangements for support during the first week of recovery.
These are general points. I tailor preparation to the individual at consultation.
What Happens at Consultation

A GP referral is required to attend a consultation. Consultations are booked online, or by telephoning the practice to speak with a receptionist.
My clinical standard for Augmentation Mastopexy is two or more consultations before surgery. The decision to proceed is made over time, not in a single appointment.
Consultation 1: assessment. Approximately one hour. Medical history, examination, clinical photography (with consent), 3D imaging, and physical sizing with implants. Discussion of suitability for the combined or staged approach, and a review of risks. Telehealth is available for patients at a distance, but at least one in-person consultation is required before surgery. A detailed written quote covering surgeon, anaesthetist, hospital, and follow-up care is provided after this consultation.
Consultation 2: review and decisions. Review of options, finalising implant shape and size, and answering remaining questions. The quote and scheduling can be discussed with the patient coordinator at this visit. Patients are encouraged to take time, ask questions, and seek a second opinion.
Anaesthetic consultation. A separate consultation with the anaesthetist is arranged before surgery, usually by telephone, with an in-person review on the day of admission.
For cosmetic surgery in Australia, informed consent is obtained at a consultation at least seven days before the day of surgery. My consultation pattern is built around that requirement, and around giving patients time to consider their decision.
Book your appointment online now
Hospital and Recovery

Surgery is performed at Maitland Private Hospital, in the Hunter Valley NSW. The hospital provides 24-hour medical cover and an on-site intensive care unit.
Hospital stay. Combined Augmentation Mastopexy is most often performed as a day-stay procedure, with discharge later the same day. An overnight stay is available where preferred, or where clinically indicated. Patients who stay overnight are seen during admission. Most patients are home on the day of surgery.

Early recovery. A general recovery timeline:
- Discomfort for the first few days, varying from patient to patient. Most patients manage with paracetamol and a short course of stronger pain relief
- Compression garments are provided and worn during the early healing period
- Showering the day after surgery is usually possible
- Drains are not routinely required
- Most patients with a desk-based job return to work within one to two weeks
- Driving is resumed when the patient can safely perform an emergency stop, usually around two weeks
- Light activity is gradually reintroduced. Full exercise without restriction is generally appropriate from approximately six weeks

Wound care and scar management. Standard post-operative care includes a course of LED light therapy and silicone scar strips. Care continues during the first months as the wound matures.
Follow-up. Patients are seen the day after surgery and again at one month, three months, and six months. These appointments are part of the surgical fee.
Final result. Breast position and shape continue to settle for several months after surgery. Final position and feel are typically reached at approximately twelve months.
Recovery varies between patients. Individual timelines depend on the technique used, the size of the lift, the implant placement, and how each patient heals.
Risks

All surgery carries risks. Combined Augmentation Mastopexy involves both the risks of Mastopexy and the risks of breast implants, in a single, longer operation. The risk of complications is greater for combined operations than for either component performed alone, and rises further with the size of the lift required.
The list below is not exhaustive. The full risks are discussed at consultation, and patients are given written information to take home and consider.
General surgical risks
- Bleeding, including the possibility of haematoma requiring return to theatre
- Infection
- Adverse reactions to the anaesthetic
- Blood clots in the legs or lungs (deep vein thrombosis and pulmonary embolism)
- Slow wound healing or wound breakdown
- Scarring, including hypertrophic or keloid scars in patients prone to them
- Asymmetry between the two sides
- Persistent or unsatisfactory result requiring revision surgery
Risks specific to Mastopexy
- Loss or change of nipple sensation, which may be temporary or permanent
- Loss of blood supply to the nipple-areola complex, in rare cases requiring further surgery
- Healing problems at the T-junction of the incision, where the vertical and horizontal scar lines meet
- Breast shape changes over time as tissues continue to settle
- Visible scarring that does not fade as hoped
- Inability to breastfeed, or reduced ability to breastfeed, after surgery
Risks specific to breast implants
- Capsular contracture, where scar tissue around the implant tightens and can change breast shape or cause discomfort
- Implant rupture or leakage, which may not be immediately noticeable and may require imaging to detect
- Implant malposition, including movement of the implant from its original position
- Rippling or palpability of the implant edge, particularly in patients with thinner soft tissue cover
- Need for further surgery during a patient’s lifetime. Implants are foreign material in the body, and the majority of patients will need revision surgery at some stage. The revision rate at ten years is approximately thirty percent
- Breast Implant Associated Anaplastic Large Cell Lymphoma (BIA-ALCL), a rare type of immune system cancer associated with certain breast implants. Ongoing surveillance is recommended
Combined-operation considerations
Performing Mastopexy and Breast Augmentation in the same operation increases the risk of complications compared to either procedure alone. For patients with grade 3 ptosis, or post-weight-loss patients with substantial loose skin, a staged approach often carries a lower complication risk profile.
Risks are discussed in detail at consultation. Patients are encouraged to ask questions, take time, and seek a second opinion before deciding.
Frequently Asked Questions
Is this done as one operation or two?
The preferred path, where clinically suitable, is one operation. Combined Augmentation Mastopexy means a single anaesthetic, a single recovery period, and a single set of fees. Some patients are better suited to a staged approach, with Mastopexy performed first and implants placed approximately six months later. The right path depends on the size of the lift required, the amount of breast tissue, and the overall risk profile.
How is suitability for single-stage versus staged decided?
Suitability is assessed at consultation through physical examination, medical history, and discussion of goals. Patients with grade 1 or grade 2 ptosis and adequate but reduced breast tissue volume are most often suitable for the single-stage approach. Patients with grade 3 ptosis, and many post-weight-loss patients with substantial loose skin, are often better served by a staged approach because the risk of complications rises with the size of the lift required.
Will my implants need replacing?
Breast implants are foreign material in the body, and the majority of patients will need revision surgery at some stage. The revision rate at ten years is approximately thirty percent. There is no fixed expiry date, and replacement timing varies between patients. Reasons for revision include capsular contracture, implant rupture, malposition, and changes in breast shape over time.
What is BIA-ALCL?
BIA-ALCL stands for Breast Implant Associated Anaplastic Large Cell Lymphoma. It is a rare type of immune system cancer associated with certain breast implants. The risk varies by implant type and is discussed at consultation. Ongoing surveillance and awareness of changes (such as breast swelling years after surgery) are recommended for all patients with implants.
How long is recovery?
Most patients with a desk-based job return to work within one to two weeks. Driving is usually resumed at approximately two weeks, when the patient can safely perform an emergency stop. Light activity is gradually reintroduced, and full exercise without restriction is generally appropriate from approximately six weeks. Breast position and shape continue to settle for several months, with final position typically reached at approximately twelve months. Recovery varies between patients.
Is this covered by Medicare or private health?

Augmentation is always classified as cosmetic surgery, regardless of the approach. The implant component does not attract a Medicare rebate or private health fund contribution.
A standalone Mastopexy may attract a Medicare item number where it meets specific clinical criteria, assessed individually at consultation. This affects the two approaches differently:
- Single-stage combined. The Medicare item number for Mastopexy specifically excludes operations performed with implants. The combined operation is classified as cosmetic in full. No Medicare rebate, no private health fund contribution, and ten percent GST applies to all fees.
- Staged. The first-stage standalone Mastopexy may attract a Medicare item number where it qualifies. The second-stage implant placement is cosmetic.
A detailed written quote covering all fees (surgeon, anaesthetist, hospital, and follow-up) is provided after the first consultation.
Next Steps
Thighplasty is a considered decision. The right starting point is a clinical assessment of the pattern of skin laxity, the patient’s overall health, and whether the timing is right.
Two ways to proceed
A GP referral is required. Consultations can be booked online or by telephoning the practice on (02) 4934 5700.
Combined Augmentation Mastopexy is classified as cosmetic surgery. Medicare and private health funds do not contribute to the implant component. Where Mastopexy is performed as a standalone procedure, it may attract a Medicare item number under specific clinical criteria. A detailed written quote is provided after the first consultation.
Augmentation Mastopexy is a permanent surgical change with risks that vary between patients. The information on this page is general and educational. Suitability is assessed individually at consultation following physical examination and discussion of medical history.
GP referral required. Consultation required to determine suitability. Results vary. All surgery carries risks.

