Brachioplasty (Arm Lift): Upper Arm Skin Removal Surgery
Brachioplasty, also known as arm lift surgery or arm tightening surgery, is a procedure that removes excess skin from the upper arm.
It is most commonly performed for patients with loose upper arm skin following significant weight loss. Ageing and genetic factors can also contribute to skin laxity that does not improve with weight stability or exercise.
Several surgical approaches are available. These range from suction-assisted lipectomy (liposuction) alone through to limited, full, and extended brachioplasty.
The appropriate technique depends on the amount of excess skin, how far the skin extends, and the distribution of fat in the upper arm. This is assessed at consultation by Dr Bernard Beldholm FRACS, Specialist Surgeon, at his practice in the Hunter Valley, NSW.
Results vary between patients. All surgery carries risks. A GP referral is required for consultation.
The Beldholm Approach to Brachioplasty

Most patients I see for brachioplasty (also referred to as arm lift, arm tightening, or arm reduction surgery) have already lost significant weight, whether through lifestyle changes, bariatric surgery, or other medical weight-loss programs. The upper arm is one of the areas where skin does not reliably retract after that kind of weight change. By the time someone comes to me, the skin has usually been loose for at least a year, and exercise has not changed it.
Matching the operation to your pattern
My approach is to let the pattern on the arm determine the operation. The right technique depends on:
- How much excess skin is present
- Where the skin extends: armpit only, down the inner arm, or continuing into the chest wall
- The distribution of fat in the upper arm
- Whether the presentation is predominantly skin, predominantly fat, or a mix of both
In practice these factors combine. A patient with moderate inner-arm laxity and some fat may have a full brachioplasty with liposuction in the same operation. A patient with skin excess continuing to the chest wall may have an extended brachioplasty, with or without liposuction depending on what fat is present.
The four-option framework in the downloadable guide is a starting point. The actual surgical plan is decided at examination.
Standalone, or combined with another procedure
Most brachioplasty in my practice is a standalone operation. In some post-weight-loss patients, however, several contouring patterns are present at once. Combining procedures in one operation can be clinically appropriate when that is the case.
Examples of combinations I sometimes perform:
- Brachioplasty combined with bra-line lipectomy, when loose skin also extends across the upper back
- Brachioplasty combined with torsoplasty, when upper body skin laxity is also present
These combinations are decided clinically, based on what is present at examination. If combining is not clinically appropriate, the procedures are staged separately.
Preparing for surgery (full and extended brachioplasty)
If you are having a full or extended brachioplasty after significant weight loss, there is preparation work before we operate. The arm wound sits under tension as it heals. Patients who have lost a lot of weight often have nutritional gaps that directly affect healing.
Everyone in this group starts on a pre-operative nutrition pathway at their first consultation, before we have surgical dates. The pathway is covered in full below.
Whether brachioplasty is appropriate for you, and which variant is right for your pattern, is determined at consultation.
Is Brachioplasty the Right Procedure for Me?
Not every patient with loose upper arm skin is a candidate for surgical arm skin removal. Some patients benefit from brachioplasty. Others are better served by addressing weight stability, fat distribution, or an underlying medical factor first.
Signs that surgical skin removal may be appropriate
Patients who consider brachioplasty typically present with one or more of the following physical signs:
- Loose or excess skin along the upper arm that has persisted for at least 6 months despite stable body weight and exercise
- Folds of skin in the inner arm that cause irritation, rash, or hygiene difficulty
- Skin excess that extends from the armpit along the inner arm toward the elbow
- In some patients, skin that continues from the upper arm into the chest wall
- Difficulty with clothing fit that is caused specifically by excess upper arm skin
The amount of skin, where it extends, and the underlying fat distribution are all assessed at the consultation. These factors determine whether brachioplasty is appropriate and, if so, which surgical variant matches the pattern.
When brachioplasty may not be the first step
Brachioplasty may be deferred, or not recommended, in several circumstances:
- Weight not yet stable. Significant ongoing weight loss or weight gain can affect the surgical outcome. A minimum of 6 months of stable body weight is generally expected. For post-bariatric patients, 12 to 18 months after reaching target weight is preferred.
- Skin still retracting. In some cases, skin continues to retract for up to a year after significant weight loss. Surgery too early can remove skin that would otherwise have returned naturally.
- Fat excess without true skin excess. Patients whose upper arm concern is predominantly fat rather than skin may be better served by suction-assisted lipectomy (liposuction) alone, rather than skin excision.
- Current or planned pregnancy. Surgery is deferred in patients who are currently pregnant.
- Current smoking. Smoking significantly affects wound healing in brachioplasty. Smoking cessation for a defined period before and after surgery is required.
- Uncontrolled diabetes or other medical conditions. Patients with a raised HbA1c, active infection, or other uncontrolled systemic conditions require medical optimisation before surgery can be considered.
- Body Mass Index above 35. A BMI above 35 is associated with increased surgical risk. Surgery may be deferred while further weight management is pursued.
What the consultation determines
Whether brachioplasty is appropriate for a particular patient, and which variant matches the pattern present, is determined at the initial consultation with Dr Beldholm. A GP referral is required before that consultation can be booked.
Matching Brachioplasty Technique to Your Pattern
The right brachioplasty technique depends on what is actually present on the arm. Four core surgical approaches sit along a spectrum, from fat removal alone through to removal of skin and fat extending into the chest wall. In practice, these can be combined (for example, a full brachioplasty performed together with liposuction in the same operation) based on the skin and fat pattern at examination.
A short glossary
A few terms appear repeatedly below:
- Brachioplasty is the medical term for arm lift surgery. It removes excess skin (and sometimes fat) from the upper arm.
- Suction-assisted lipectomy (SAL) is the medical term for liposuction. It removes fat through small incisions but does not remove skin.
- Axilla is the medical term for the armpit.
- Scar placement varies by procedure. Brachioplasty scars are generally placed in the underarm area. They are typically not visible when the arm is viewed from the front, but can be visible when viewed from behind.
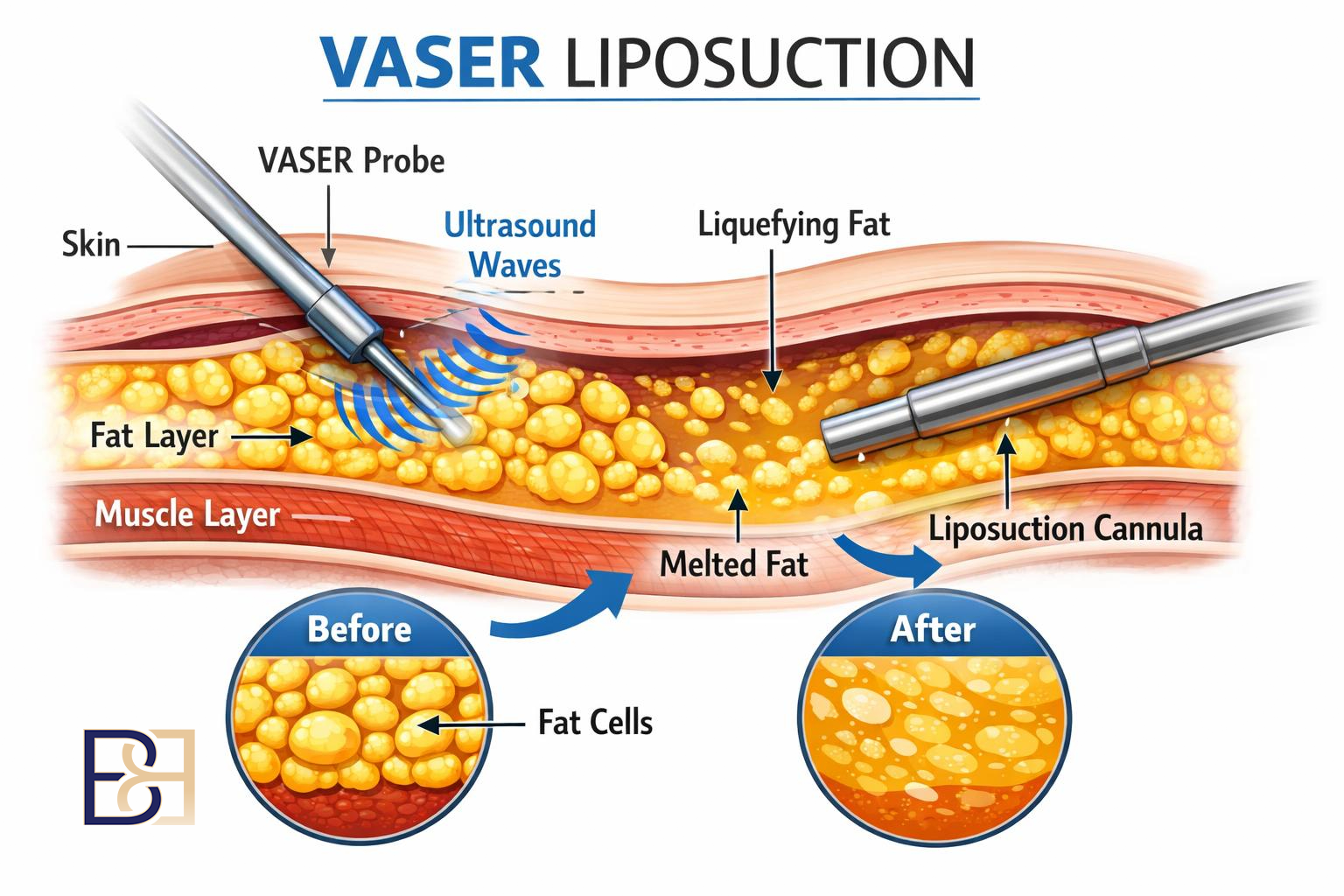
Option 1: Suction-assisted lipectomy (liposuction) alone
Who this suits. Patients whose upper arm concern is predominantly excess fat, with minimal loose skin. Skin quality and elasticity must be adequate to retract after fat removal.
- What is removed. Fat only. Skin is not excised.
- Incisions. Small entry points (a few millimetres each) for the liposuction cannula.
- Scar. Minimal and generally well-concealed.
- Main limitation. This option does not address loose skin. Patients with significant skin excess are not candidates for liposuction alone.
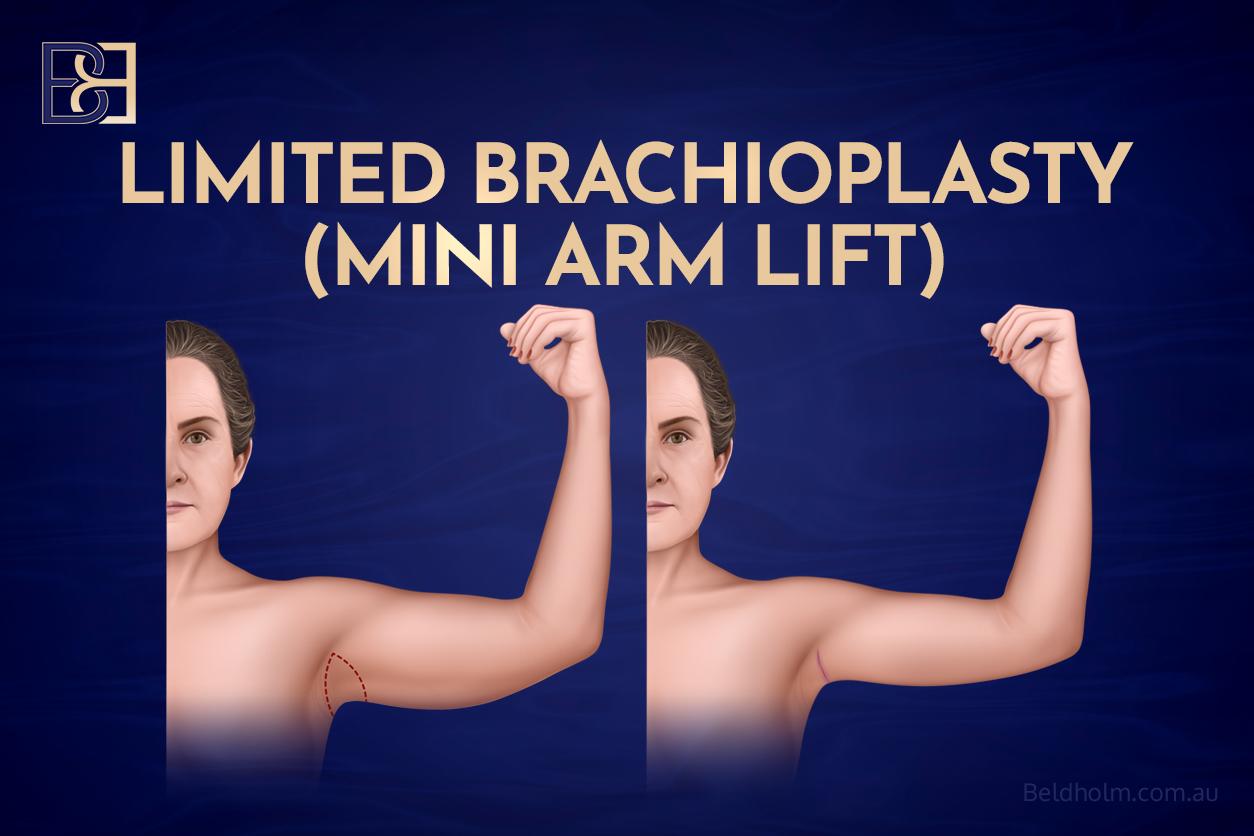
Option 2: Limited brachioplasty
Who this suits. Patients with mild loose skin concentrated near the axilla (armpit), without significant extension down the inner upper arm.
- What is removed. A smaller crescent of skin in the axilla region, with or without a small amount of fat.
- Incisions. Placed within or close to the axilla so that the scar is concealed by the arm at rest.
- Scar. Shorter than full brachioplasty, and generally hidden within the natural crease of the armpit.
- Main limitation. Limited brachioplasty removes less skin than full brachioplasty. Patients with moderate or severe laxity extending down the inner arm are not suitable candidates for a limited operation.
Some resources call this procedure “mini brachioplasty”. The clinical operation is the same.

Option 3: Full brachioplasty
Who this suits. Patients with moderate to severe loose skin extending along the inner upper arm, from the axilla toward the elbow. This is the most commonly performed brachioplasty variant in post-weight-loss patients.
- What is removed. A longer ellipse of excess skin along the inner upper arm, with or without liposuction of underlying fat in the same operation.
- Incisions. Run through the underarm area from the axilla along the upper arm. Incision placement is chosen so that the resulting scar sits in the underarm region, where it is generally not visible when the arm is viewed from the front.
- Scar. Located in the underarm area, generally not visible from the front, but can be visible when the arm is viewed from behind. Scar maturation takes 12 months or more. Scar quality depends on individual healing, wound tension, and post-operative care.
- Main benefit. Removes a significant amount of excess skin and addresses inner upper arm contour.
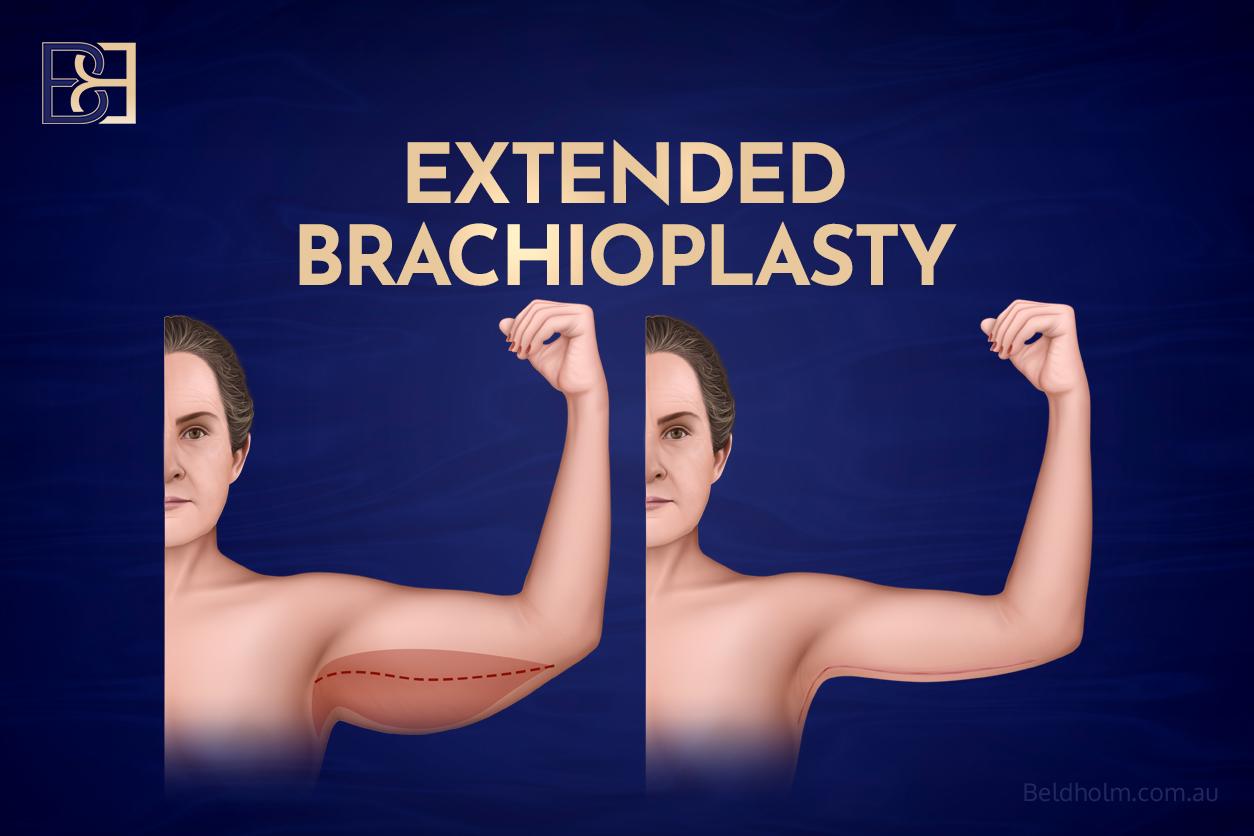
Option 4: Extended brachioplasty
Who this suits. Patients whose loose skin continues from the upper arm into the lateral chest wall or axillary roll area. This pattern is common after major weight loss and cannot be addressed by a full brachioplasty alone.
- What is removed. Excess skin from the inner upper arm, continuing across the axilla and onto the lateral chest wall. Liposuction may or may not be performed in the same operation, depending on fat distribution.
- Incisions. Extend from the inner arm across the axilla and onto the side of the chest. The exact incision length depends on how far the skin laxity extends.
- Scar. Longer than full brachioplasty, extending from the underarm area onto the lateral chest. Careful placement keeps the scar as concealed as possible under the arm and within the natural contour of the torso.
Main benefit. Addresses arm and upper torso laxity in a single operation where both patterns are present.
Combining brachioplasty with other procedures
In some post-weight-loss patients, skin laxity is present in more than one area at once. Brachioplasty is most commonly performed as a standalone operation. Where clinically appropriate, it may also be performed in the same operative episode with:
- Bra-line lipectomy, when loose skin extends across the upper back
- Torsoplasty, when upper body skin laxity is also present
Whether to combine, or to stage the procedures separately, is a clinical decision based on the patient’s overall medical status, the size of the combined operation, and what is on the body at examination.
Which variant is right for me?
The selection is made by Dr Beldholm at the initial consultation, based on physical examination of the arm and any other areas of concern. A GP referral is required for consultation.
Download the Free Guide
4 Brachioplasty (Arm Lift) Options You Need to Know If You Have Loose Underarm Skin
Covering liposuction alone, limited brachioplasty, full brachioplasty, and extended brachioplasty.
This short guide explains the four core surgical approaches to loose upper arm skin. For each option, it outlines who the procedure typically suits, how the operation is performed, where the incisions are placed, and the main limitations and benefits.
The guide is written for patients considering brachioplasty and is intended to support the information on this page, not to replace a consultation.
Educational content only. Not a substitute for medical advice. A consultation with Dr Beldholm is required to determine whether brachioplasty is appropriate for a particular patient.
About Dr Bernard Beldholm

I am Dr Bernard Beldholm, a Specialist Surgeon based in the Hunter Valley, NSW. I have been in specialist practice for more than 15 years, with a clinical focus on body contouring surgery for patients who have lost significant weight.
Clinical focus
My practice concentrates on:
- Post-weight-loss body contouring, including abdominoplasty, brachioplasty, thighplasty, and torsoplasty
- Post-pregnancy body contouring
- Breast surgery, including mastopexy, reduction, and augmentation
- Facial rejuvenation surgery
Brachioplasty forms a regular part of my weekly operating list, particularly for patients who have lost weight through bariatric surgery, medical weight-loss programs, or sustained lifestyle change.
Where I operate
All procedures are performed at Maitland Private Hospital, a fully accredited private hospital with 24-hour medical cover and on-site intensive care support. Performing surgery in an accredited private hospital environment (rather than a day-surgery facility) means that, if extended post-operative observation is ever required, it is available in the same building.
Consultations take place at my rooms in the Hunter Valley. A telehealth option is available for the initial consultation for patients travelling from further afield within New South Wales.
GP referral

A GP referral is required before an initial consultation can be booked. This applies to every new patient and is part of the standard pathway for specialist care in Australia.
Book your appointment online now
Preparing for Brachioplasty

Who this preparation pathway applies to
The pathway described below applies to patients having full or extended brachioplasty after significant weight loss. These operations involve longer incisions under greater wound tension, and the post-weight-loss population more frequently has nutritional deficiencies that directly affect wound healing.
For patients having liposuction alone or a limited brachioplasty, and for patients whose arm skin laxity is not weight-loss related, pre-operative preparation is straightforward and covered at the consultation. The intensive nutrition pathway described here is not required.
Why pre-operative nutrition matters for arm wounds
A full or extended brachioplasty leaves a long inner-arm incision that bears constant tension as the arm moves. Wound tension, combined with the reduced protein, iron, vitamin D, zinc, and B-vitamin levels commonly seen after significant weight loss, increases the risk of:
- Wound separation or delayed healing along the incision
- Seroma formation (fluid collection under the skin)
- Slower scar maturation and wider scar formation
- Longer overall recovery
Correcting these deficiencies before surgery means the body has what it needs to heal when wound tension is at its highest in the first few weeks after the operation.
The two-tier nutrition framework

I use a two-tier pre-operative nutrition framework with post-weight-loss patients:
Tier 1: universal baseline (started from the first consultation)
Every patient in this group starts on the same Tier 1 baseline at the first consultation, before blood results are reviewed. Tier 1 covers the most common deficiencies in the post-weight-loss population:
- Whey protein isolate, titrated to daily protein intake
- A complete multivitamin
- Vitamin D3 with vitamin K2
- Vitamin C
- Zinc
Tier 2: blood-guided additions (added at the second consultation)
At the first consultation I provide a blood test request form so bloods are taken before the second consultation. Common Tier 2 additions, when bloods indicate they are needed, include:
- Iron
- Vitamin B12
- Folate
- Vitamin A
- Vitamin B1 (thiamine)
- Calcium citrate
- Selenium
- Magnesium
Tier 2 additions are patient-specific. Not every patient needs every item.
Fish oil timing
Fish oil is commonly used by patients in this group. It needs to be paused in the week before surgery to reduce bleeding risk, and can be resumed one to two weeks after the operation once initial wound healing is established.
Post-operative bloods
A follow-up set of bloods is taken 6 to 8 weeks after surgery to confirm that nutritional status has been maintained during the early healing phase.
Bringing it together
The nutrition pathway runs alongside the surgical planning. By the time we set operating dates, Tier 1 has been in place for several weeks and any Tier 2 additions have been started based on blood results. The goal is straightforward: when the operation happens, the body is in the best condition reasonably achievable to support wound healing.
The pathway is introduced in full at the consultation. A GP referral is required before that consultation can be booked.
The Consultation Process

Brachioplasty is not booked from a single appointment in my practice. Patients work through two consultations before surgical dates are set. This gives time for proper assessment, blood results to come back, and any questions to be worked through without pressure.
Before the first consultation
Two things need to be in place before a consultation can be booked:
- A referral from your GP. This is a standard requirement for specialist surgical care in Australia.
- Any previous relevant records, including weight history, bariatric surgery records (if applicable), and recent blood results. These can be brought to the first consultation or forwarded in advance.
First consultation
The first consultation is the clinical assessment. Typical length is 45 to 60 minutes. What happens:
- Full medical history, including weight history and any previous surgery
- Physical examination of the upper arms, and of any other areas where skin laxity may be relevant (chest wall, back, torso)
- Discussion of which brachioplasty variant matches the pattern (liposuction alone, limited, full, or extended; with or without additional procedures)
- Clinical photography for your medical file. All patients are photographed as part of the standard clinical record. These photographs are kept confidentially in your medical file and are not used for any other purpose without your written permission.
- A blood test request form (for post-weight-loss patients having full or extended brachioplasty)
- Tier 1 supplements introduced, together with the pre-surgery nutrition guide
- Direction to pathology collection near your home
Patients leave the first consultation with a clear understanding of the surgical options, a written request for blood tests, and the nutrition pathway already underway.
Between consultations
Two to four weeks typically pass between the first and second consultations. During that time:
- Blood tests are taken at a pathology collection centre
- Tier 1 supplements are continued daily
- Any questions arising from the first consultation can be noted for the second
Second consultation
The second consultation confirms surgical planning. Typical length is 30 to 45 minutes. What happens:
- Blood results are reviewed together
- Tier 2 supplements are added, specific to the blood results
- The surgical plan is confirmed in detail, including incision placement, operating time, hospital stay, and expected recovery
- The practice coordinator provides a written quote and assists with scheduling
- Provisional operating dates are set, typically with one to three months lead time
Telehealth options
At least one consultation must take place in person. The other consultation, and any follow-up discussions, can be conducted by telehealth where clinically appropriate. This gives patients travelling from further afield within New South Wales some flexibility while preserving the in-person physical examination that specialist surgical care requires.
Anaesthetic consultation
A separate consultation is arranged with the anaesthetist. For most patients this takes place by phone ahead of surgery, with an in-person review on the morning of the operation at the hospital.
Between booking and surgery
Once operating dates are set, patients continue their nutrition pathway, organise any pre-operative medical clearance required, and receive written pre-operative instructions from my rooms. If Tier 2 additions have been made, those continue through to the day of surgery.
A GP referral is required before the first consultation can be booked.
Hospital Stay & Recovery
Where the operation is performed

All brachioplasty procedures are performed at Maitland Private Hospital, a fully accredited private hospital with 24-hour medical cover and on-site intensive care support. Operating in an accredited private hospital environment means that, if extended post-operative observation is ever required, it is available in the same building.
Hospital stay by procedure type
The length of hospital stay depends on the brachioplasty variant performed:
- Liposuction alone (SAL): day surgery. Home the same day once recovered from the anaesthetic.
- Limited brachioplasty: day surgery. Home the same day once recovered from the anaesthetic.
- Full brachioplasty: overnight stay. Home the following day.
- Extended brachioplasty: overnight stay. Home the following day.
Where brachioplasty is combined with another procedure (for example with torsoplasty or bra-line lipectomy), the length of stay is reviewed during surgical planning at the second consultation.
Immediately after surgery

Expect bandaging across both upper arms. Some bruising, swelling, and discomfort is normal in the first week. Oral pain relief is prescribed for the early recovery period. Drains are not routinely used in most brachioplasty cases, but may be placed if clinically indicated.
Compression garments are part of the post-operative pathway. These are worn over the upper arms, typically for several weeks, to reduce swelling and support the healing tissue. The specific garment and wearing schedule are provided at the pre-operative appointment.
The first two weeks

The first two weeks of recovery are the most important for wound healing. During this period:
- Rest is prioritised over activity
- Arms are kept raised where practical to reduce swelling
- Lifting is avoided, including anything more than light objects
- Driving is avoided until arm movement is comfortable and pain-free
- The wound is kept dry until reviewed
Most patients are seen in my rooms for a wound review at 1 to 2 weeks.
Returning to daily activity
Return to work depends on the type of work. Desk-based work is often resumed from around 2 weeks, provided arm movement is comfortable. Work involving heavy lifting, physical labour, or overhead arm movement generally requires 4 to 6 weeks.
Light walking can begin early. More demanding physical activity, including resistance training and anything placing tension across the inner arm, is reintroduced gradually, usually from around 6 weeks, with full return to gym and upper-body training typically by 8 to 12 weeks.
Follow-up schedule
Routine follow-up after brachioplasty in my practice includes:
- Early wound review at 1 to 2 weeks
- Further reviews at 6 weeks, 3 months, 6 months, and 12 months
A follow-up set of bloods is taken at 6 to 8 weeks in post-weight-loss patients to confirm nutritional status has been maintained through early healing.
Scar maturation
The brachioplasty scar continues to change for 12 months or more after surgery. Early in recovery the scar is typically pink, firm, and slightly raised. Over the following year it gradually softens, fades, and flattens. Final scar appearance varies between patients and is influenced by individual healing, wound tension, genetics, and post-operative care. Scar management strategies are introduced at the wound review appointments.
If you are travelling from further afield
Patients travelling to Maitland from further afield within New South Wales are generally asked to plan for a local stay of 7 to 10 days after surgery. This allows the early wound review to take place in person before returning home. Subsequent follow-up can be by telehealth where clinically appropriate.
Risks & Possible Complications

All surgery carries risk. Brachioplasty is a substantial surgical procedure, and patients considering it should understand both the general risks of surgery and the specific risks associated with arm lift procedures.
This section describes the main risks and possible complications. It is not a complete list. Dr Beldholm discusses risks in detail at consultation in the context of each patient’s individual medical history, body weight history, and the specific brachioplasty variant being planned.
Risks specific to brachioplasty
Scar-related outcomes. Brachioplasty produces a visible scar. Scar placement is chosen carefully, but the scar is not invisible. Scar appearance varies between patients. Possible scar-related complications include:
- Wider or raised scar formation (hypertrophic or keloid scarring)
- Changes in scar pigmentation
- Asymmetry between the two sides
- Scar stretching over time, particularly where wound tension is high
Wound-related complications. Because the inner arm wound sits under tension as the arm moves, wound-related complications are more common in brachioplasty than in some other procedures. These include:
- Wound separation or delayed healing along part of the incision
- Seroma formation (a collection of fluid under the skin), which may require drainage
- Haematoma (a collection of blood under the skin), which occasionally requires surgical drainage
- Wound infection, which may require antibiotics or further intervention
Sensation changes. The inner upper arm contains sensory nerves that may be affected by the surgery. Possible outcomes include:
- Numbness along the inner arm, particularly in the early months after surgery
- Altered sensation or tingling
- In some patients, areas of reduced sensation that persist long term
Asymmetry and contour irregularities. Despite careful planning, the two arms may heal differently. Possible outcomes include visible differences in scar length, scar quality, arm contour, or skin tightness between the two sides. Minor asymmetry is common; significant asymmetry is uncommon but possible.
Outcome variability. Final appearance and scar quality are influenced by individual healing, skin quality, wound tension, genetics, age, smoking status, nutrition, and adherence to post-operative instructions. Outcomes vary between patients. No surgical outcome can be guaranteed.
General surgical risks
As with any major surgery, brachioplasty carries general surgical risks, including:
- Bleeding
- Infection
- Deep vein thrombosis (DVT) and pulmonary embolism (PE)
- Delayed wound healing
- Poor cosmetic outcome requiring revision surgery
- Allergic reaction to suture material, dressings, or other materials used during surgery
Anaesthetic risks
Brachioplasty is performed under general anaesthetic. General anaesthesia carries its own risks, including:
- Reactions to anaesthetic agents
- Nausea and vomiting
- Sore throat or dental injury from airway management
- Cardiac and respiratory complications, which are uncommon but possible
These risks are discussed at the separate anaesthetic consultation, where individual medical factors are reviewed.
Factors that can increase risk
Some factors increase the risk of complications in brachioplasty. These are reviewed at the consultation and, where possible, modified before surgery proceeds:
- Smoking (significantly increases wound healing complications)
- Body Mass Index above 35
- Uncontrolled diabetes
- Certain medications (including blood thinners and some supplements)
- Nutritional deficiencies, particularly protein, iron, vitamin D, zinc, and B-vitamin deficiencies
- Ongoing weight instability
Revision surgery
In some cases, revision surgery may be considered to address scar-related concerns, asymmetry, or contour irregularities. Revision surgery is a separate operation with its own risks and is considered only after initial healing is complete, usually at 12 months or later.
A note on individual results
Individual results vary. The descriptions and images patients may see of brachioplasty outcomes in educational materials represent the experience of specific patients and are not predictive of what any particular patient will experience. Surgical outcomes depend on many factors, most of which are individual to the patient.
Whether brachioplasty is appropriate, and the risks relevant to a particular patient’s situation, are discussed in detail at consultation. A GP referral is required before a consultation can be booked.
Frequently Asked Questions
How much does brachioplasty cost with Dr Beldholm?
The cost of brachioplasty depends on which surgical variant is performed, whether it is combined with another procedure, the length of hospital stay required, and the anaesthetist’s fees. There is no single fixed price.
Patients receive a written quote from the practice coordinator at the second consultation, after the surgical plan has been confirmed. The quote covers Dr Beldholm’s surgical fee, anaesthetic fees, hospital fees, and any associated costs.
Eligibility for Medicare rebates is assessed individually at consultation. Criteria apply.
Will the scar be visible?
Brachioplasty scars are placed in the underarm area. They are generally not visible when the arms are viewed from the front, but can be visible when the arms are viewed from behind.
Scar appearance changes considerably during the first 12 months after surgery. The scar is typically pink, firm, and slightly raised in early recovery, gradually softening, fading, and flattening over time. Final scar appearance varies between patients.
Can brachioplasty be combined with other post-weight-loss procedures?
In some cases, yes. Where loose skin is present in more than one area at the same time, and the patient is medically suitable for a longer combined operation, brachioplasty may be performed in the same operating session as torsoplasty or bra-line lipectomy.
Whether to combine procedures or to stage them separately is a clinical decision based on the patient’s overall medical status, the size of the combined operation, and the pattern of skin laxity present at examination.
How much time off work is needed after brachioplasty?
Time off work depends on the type of work performed:
- Desk-based work is often resumed from around 2 weeks, provided arm movement is comfortable
- Work involving heavy lifting, physical labour, or overhead arm movement generally requires 4 to 6 weeks
- Return to upper-body strength training typically follows from around 6 weeks, with full clearance usually by 8 to 12 weeks
These are general guidelines. Individual recovery varies, and return-to-work timing is reviewed at the post-operative wound review appointments.
Is brachioplasty covered by Medicare?
Some brachioplasty cases meet the criteria for a Medicare item number. Eligibility depends on the clinical circumstances, including the cause of the loose skin (significant weight loss, for example), documentation of related symptoms or functional issues, and the surgical variant being performed.
Eligibility is assessed individually at consultation. Where Medicare criteria are met, this affects out-of-pocket costs but does not cover the full surgical fee. The practice coordinator provides a written quote that includes any applicable Medicare rebate information.
Private health insurance may also contribute toward hospital costs where the patient holds the appropriate level of cover. This is also reviewed at the second consultation.
How long after weight loss should brachioplasty be considered?
Brachioplasty is generally considered after weight has been stable for at least 6 months. For patients who have had bariatric surgery, the typical recommendation is 12 to 18 months after reaching target weight.
Two reasons drive this timing. First, ongoing weight change can affect the surgical outcome and may stretch or distort the result over time. Second, skin continues to retract for some months after weight loss, and operating too early can remove skin that would otherwise have returned naturally.
Whether the timing is right for a particular patient is assessed at consultation, taking into account weight history, current weight stability, and the underlying cause of the skin laxity.
Booking a Consultation
The cost of brachioplasty depends on which surgical variant is performed, whether it is combined with another procedure, the length of hospital stay required, and the anaesthetist’s fees. There is no single fixed price.

What to bring to the first consultation
Patients attending the first consultation are asked to bring:
- The GP referral letter
- A current list of medications and supplements
- Any previous relevant medical records, including weight history and records from bariatric surgery (where applicable)
- Recent blood test results, if any have been taken in the previous 12 months
Bringing these to the first consultation allows surgical planning to begin without delay.
Booking lead time
Typical lead time from initial enquiry to first consultation is 2 to 4 weeks. Once both consultations are complete and operating dates are confirmed, surgery is generally scheduled with 1 to 3 months lead time, depending on individual planning requirements and theatre availability at Maitland Private Hospital.
How to Book
Consultations take place at Dr Beldholm’s rooms in the Hunter Valley, NSW. At least one consultation must take place in person; telehealth options are available for additional consultations where clinically appropriate.
Or call the clinic on (02) 4934 5700.
4 Brachioplasty (Arm Lift) Options You Need to Know if You Have Loose Underarm Skin
GP referral required. Consultation required to determine suitability. Results vary. All surgery carries risks.

