Abdominoplasty After Weight Loss – Surgery for Excess Abdominal Skin
When loose skin remains after significant weight loss, surgery is usually the next question.
After major weight loss, whether through bariatric surgery, medical weight-loss programs, or lifestyle change, many patients are left with excess abdominal skin that does not retract with time, exercise, or further weight change. For patients researching abdominoplasty after weight loss, the common questions are:
- Which procedure matches my situation?
- Am I a suitable candidate?
- What does the consultation and recovery process actually involve?
This page is written for patients who have already identified loose abdominal skin as their concern and are now looking at their surgical options. It covers the main types of abdominoplasty (standard, extended, Fleur-de-Lis, and circumferential), how each one matches a different pattern of excess skin, who is typically a candidate, and how the consultation process works with Dr Bernard Beldholm, a Specialist Surgeon (FRACS) based in the Hunter Valley, NSW. A GP referral is required for all consultations.
Dr Beldholm’s Approach

I have focused my practice on body contouring after significant weight loss for more than 15 years. In that time, the pattern I see in every consultation is the same: the right operation depends on the patient’s specific pattern of loose skin, not on a menu of procedures the patient chooses between.
Matching the procedure to the pattern
When a patient sits down in my clinic after significant weight loss, my first task is to look at where the loose skin actually sits. The questions I am working through are:
- Is the excess skin concentrated on the lower abdomen, or does it extend around to the flanks?
- Is the looseness vertical (hanging downward) or horizontal (draping across the midline)?
- Are the abdominal muscles separated, and is there a hernia in the abdominal wall?
These answers determine which abdominoplasty matches the pattern. A standard operation is right for some patients; an extended, Fleur-de-Lis, or circumferential operation is right for others.
One operation where possible
Where the pattern allows, my preference is to treat everything in a single comprehensive operation rather than stage multiple smaller ones. One anaesthetic, one recovery, one period off work is usually easier on the patient than two or three separate surgeries spaced months apart. Staging is still the right call when medical factors require it, but the default starting point is a single well-planned operation.
Preparation before surgery
Because a single comprehensive operation places more physiological demand on the body, the preparation before surgery matters. Nutritional optimisation, weight stability, and medical preparation are not optional extras. They are part of the operation.
Who is a candidate for abdominoplasty after weight loss?
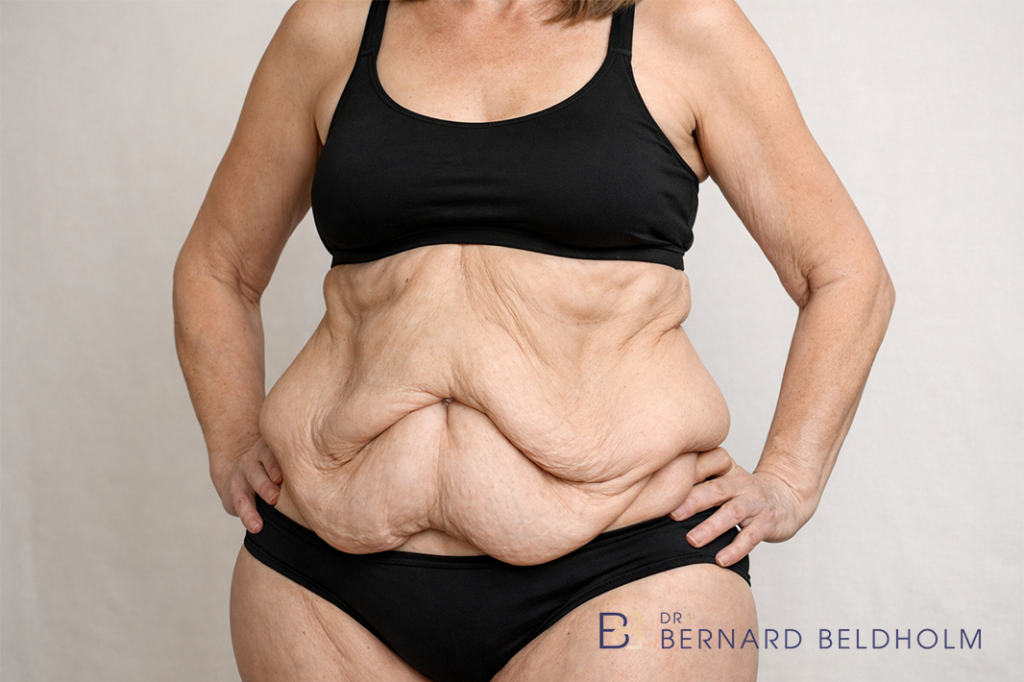
Candidacy for abdominoplasty after weight loss depends on several factors, not just the presence of loose skin. The following is a general guide to the situations in which surgery is usually considered, and the situations in which it is usually deferred.
If your weight has stabilised and you are in good general health
Patients typically considered candidates for abdominoplasty after weight loss share the following characteristics:
- Significant weight loss, whether through bariatric surgery, medical weight-loss programs, or lifestyle change. Medicare defines significant weight loss as a reduction of at least 5 BMI units, though in practice most patients who come to consultation have lost substantially more.
- Weight stable for at least 6 months, ideally 12 months. Operating while the weight is still changing can compromise the long-term result.
- A BMI in a workable range. Lower BMIs generally produce more predictable results, with BMIs between 18 and 30 preferred where possible. Higher BMIs are not an automatic exclusion but may limit how much skin can be safely removed in a single operation.
- No active smoking or nicotine use, including nicotine replacement therapy and vape products containing nicotine. Smoking impairs wound healing and increases the risk of serious complications.
- Chronic medical conditions such as diabetes, high blood pressure, or heart disease are well controlled.
- Realistic expectations about what the operation can and cannot do. Abdominoplasty removes excess skin and repairs separated muscles. It is not a weight-loss procedure.
Age is not usually the deciding factor when general health is good. Many patients considering abdominoplasty after weight loss are in their 50s, 60s, or beyond. What matters more than a number is fitness for general anaesthetic and the absence of uncontrolled medical conditions.
If your weight or health needs attention first

In the following situations, surgery is usually deferred until the underlying factor is addressed:
- Ongoing weight loss or weight fluctuation greater than 1 to 2 kg per month. Further weight loss after surgery can produce new loose skin.
- Uncontrolled diabetes, elevated HbA1c, or other metabolic issues that substantially increase surgical risk.
- Active smoking or recent nicotine use. A minimum of 4 weeks nicotine-free before and after surgery is required.
- Very high BMI where a single operation would not produce a reasonable result or would carry excessive risk.
- Nutritional deficiencies, which are common after bariatric surgery. Low iron, protein, vitamin D, or B12 levels need to be corrected before surgery to support wound healing.
Most of these factors are addressable in the months leading up to surgery. Candidacy is assessed individually at consultation.
Matching the Procedure to your Pattern
The procedure that may be appropriate for abdominal loose skin after weight loss depends on where the excess sits, how much there is, and what the underlying abdominal wall looks like.
Loose skin after significant weight loss generally shows up in one of two directions, sometimes both:
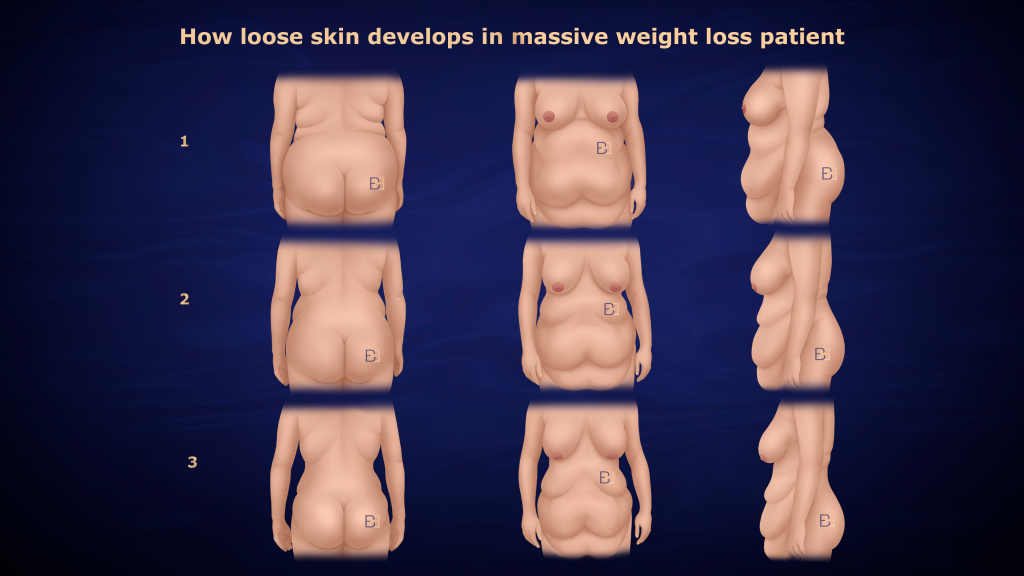
Most patients come to the consultation with a general term in mind, whether that’s abdominoplasty (tummy tuck), extended abdominoplasty (extended tummy tuck), or stomach skin removal surgery. The specific procedure that suits each patient depends on where the loose skin sits. A procedure for a patient whose looseness is mainly across the lower abdomen is different from a procedure for a patient whose looseness extends around the flanks, or runs both vertically and horizontally.
The main procedures used to remove excess abdominal skin are grouped below by the pattern they address. A consultation is required to determine which operation matches your specific anatomy.
Three terms used to describe loose skin patterns
After significant weight loss, three terms describe where the loose skin sits:
- Vertical excess. The skin hangs downward from the upper abdomen toward the pubic area. Usually addressed by removing a horizontal strip across the lower abdomen.
- Horizontal excess. The skin is loose across the midline, bunching from side to side. Usually addressed by removing a vertical strip along the midline.
- Circumferential excess. The looseness wraps around the lower trunk, including the abdomen, flanks, lower back, and upper buttocks. Addressed by an incision that goes right around the waist.
Most patients have a combination of these patterns rather than a single one.
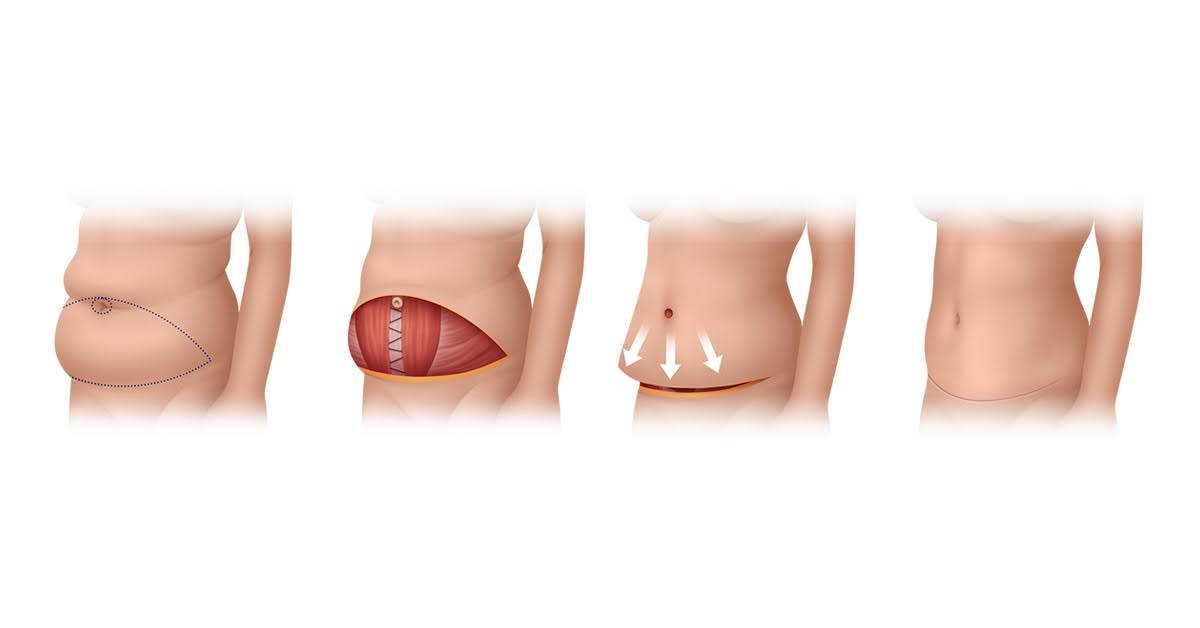
Pattern 1: Excess skin mainly on the lower abdomen
Many patients after moderate weight loss, and patients after pregnancy, have loose skin concentrated below the navel, often accompanied by separated abdominal muscles (diastasis recti).
Standard abdominoplasty (tummy tuck). The lower-abdominal skin is removed through a horizontal incision placed low, typically from hip to hip. The belly button (umbilicus) is repositioned and any separated muscles are repaired. The scar sits low enough to be covered by underwear.
Pattern 2: Excess skin extending to the flanks
After significant weight loss, the loose skin often extends past the hips to include the flanks and sides. A standard abdominoplasty does not reach far enough to treat this.
Extended abdominoplasty (extended tummy tuck). The horizontal incision is carried further around each side, allowing removal of excess skin from the flanks as well as the lower abdomen. Addresses the flank-roll pattern that a standard abdominoplasty leaves behind.
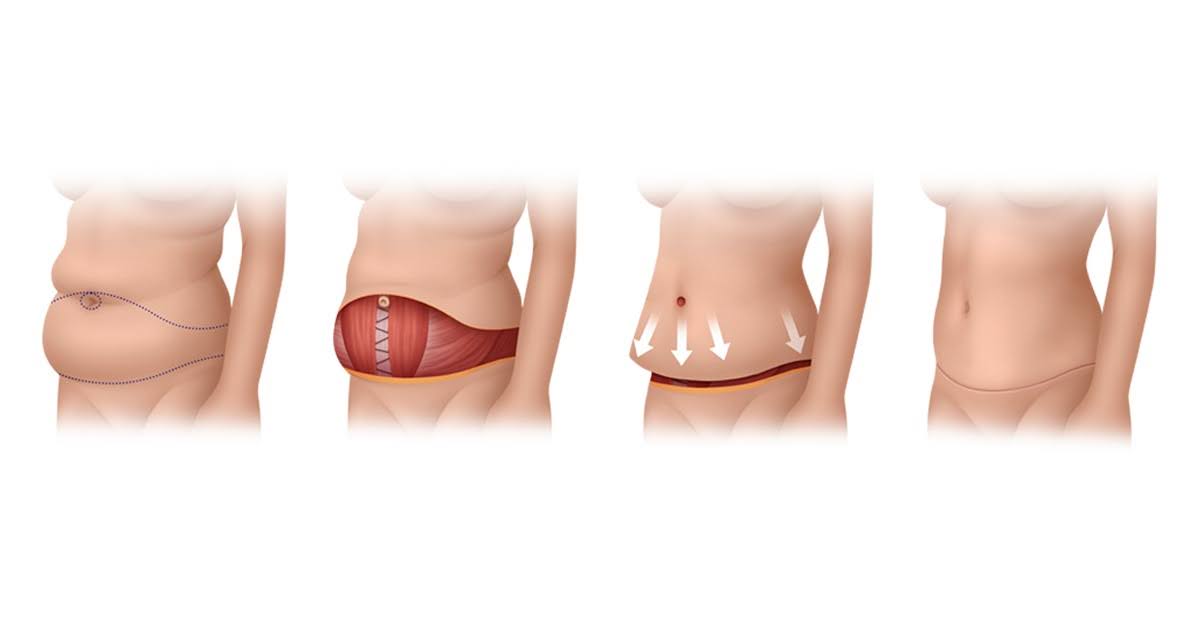
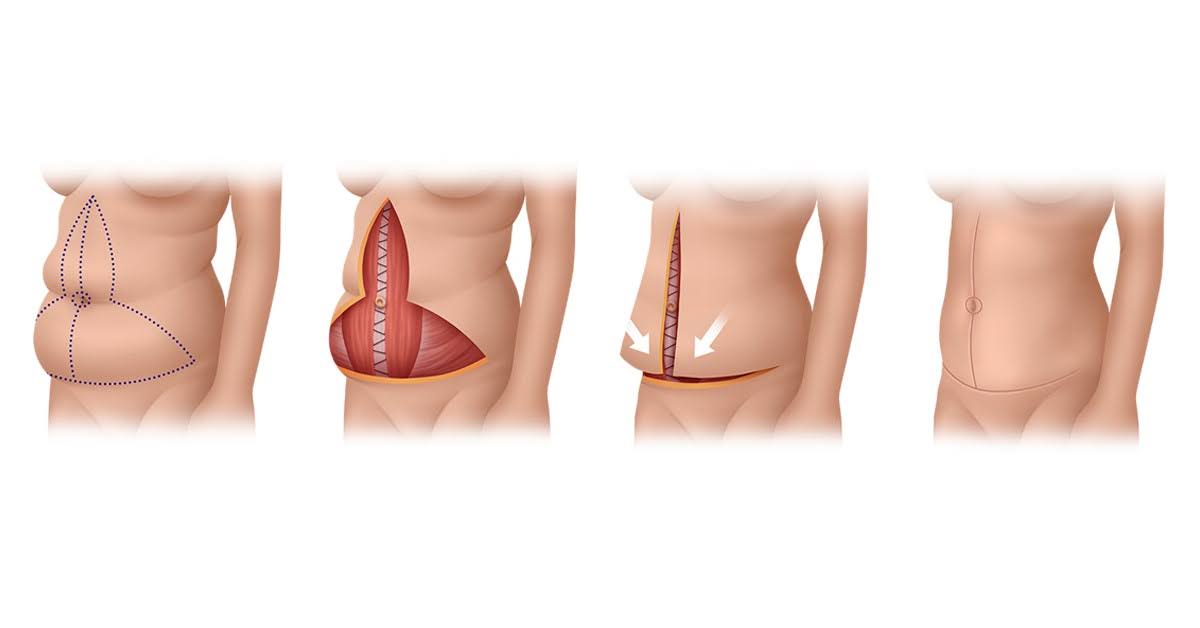
Pattern 3: Excess skin in both vertical and horizontal directions
After massive weight loss, many patients have significant looseness running both vertically (hanging downward) and horizontally (bunching across the midline), often involving the upper abdomen as well as the lower.
Fleur-de-Lis abdominoplasty. Combines a low horizontal incision with a vertical incision running up the midline, forming an inverted T shape. Removes more skin in both directions than any single-incision operation. Involves a visible vertical scar that does not hide under most clothing. Often the right choice after substantial weight loss.
Dual-vector abdominoplasty. When upper abdominal laxity is significant enough that a Fleur-de-Lis alone cannot adequately treat it, the Fleur-de-Lis can be combined with an upper abdominal lipectomy. This adds a further incision in the upper abdomen to remove skin in that zone. Reserved for the most extensive patterns of upper, lower, and horizontal laxity.
Pattern 4: Circumferential looseness around the lower trunk
Patients with 360-degree skin laxity, most commonly post-bariatric patients, have loose skin not only on the abdomen but also on the flanks, lower back, and upper buttocks.
Circumferential abdominoplasty (belt lipectomy). The incision runs completely around the waist, allowing simultaneous removal of excess skin from the abdomen, flanks, hips, and lower back in a single operation. Requires a longer hospital stay and a more structured recovery program.
Circumferential hybrid abdominoplasty. When a patient with circumferential laxity also has significant vertical and horizontal excess on the anterior abdomen, the belt lipectomy can be combined with a Fleur-de-Lis. This adds a vertical midline incision to the 360-degree incision, treating the full circumferential pattern and the anterior vertical and horizontal laxity in the same operation. Reserved for patients with the most extensive post-weight-loss skin excess.
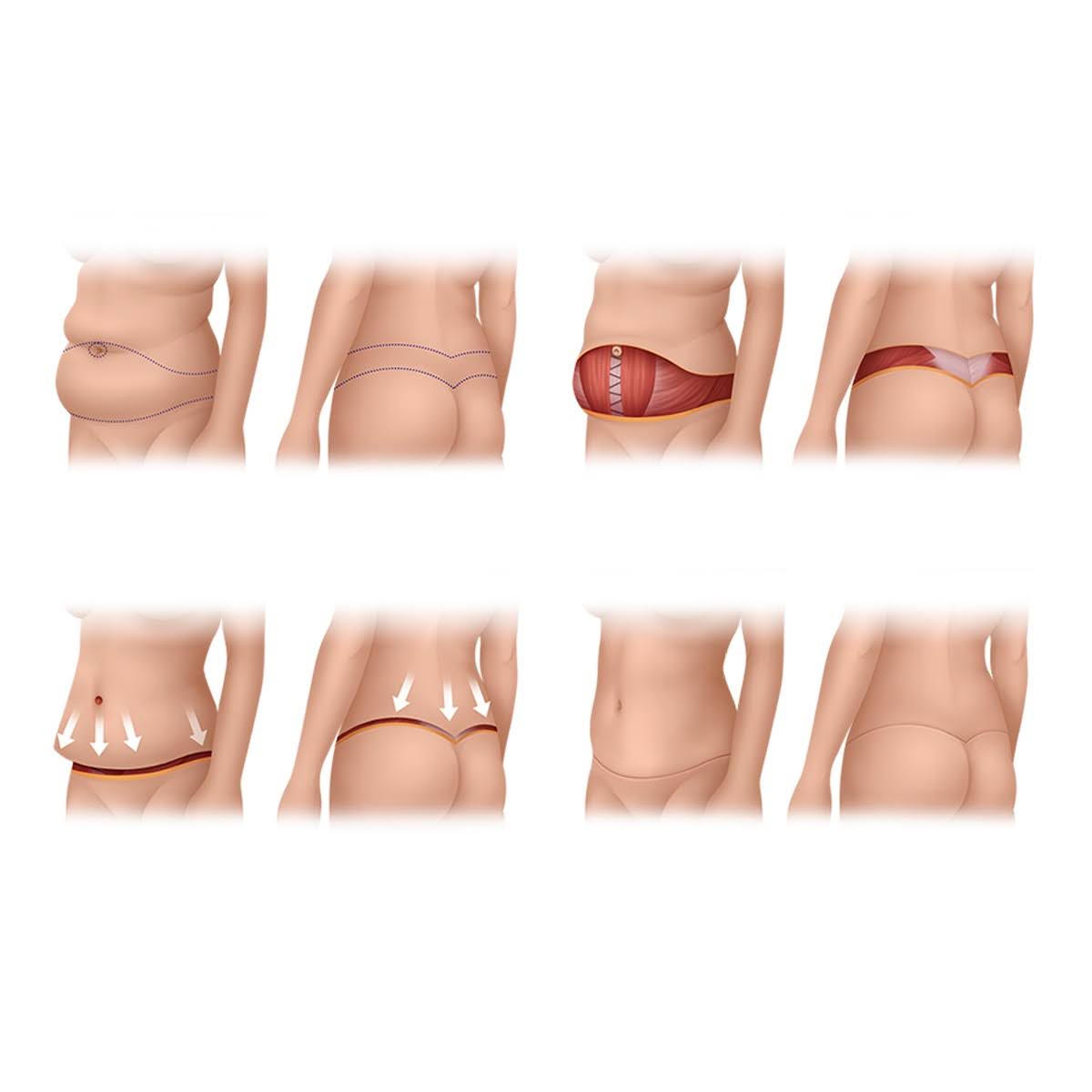
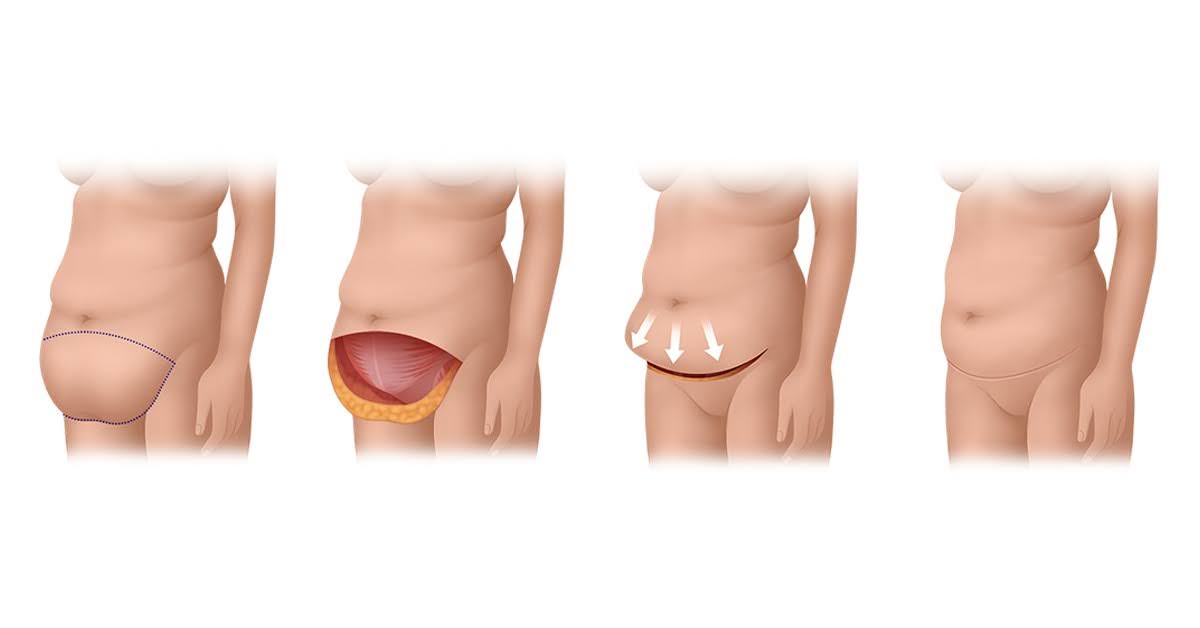
Pattern 5: Significant hanging apron with medical constraints
Some patients have a large overhanging skin apron but are not medically suitable for a long operation, or have not yet reached their goal weight. In these cases, a more limited operation may be used as an interim step.
Apronectomy (panniculectomy). Removes the hanging lower-abdominal skin and fat without undermining surrounding tissue, repairing muscles, or repositioning the belly button. A shorter operation with a shorter recovery, but a more limited result. Often performed as a staging operation before a more comprehensive procedure, once the patient is medically optimised or has reached goal weight.
Free guide: 7 Surgical Options for Loose Skin After Weight Loss
A companion guide written by Dr Beldholm for patients considering surgery for loose skin after significant weight loss. Covers the seven procedures most often used to treat the abdomen, flanks, and back.
What’s inside:
- Seven procedures explained, with the pattern of loose skin each one addresses
- Factors Dr Beldholm considers when recommending a specific procedure
- Typical hospital stay and recovery for each procedure
- Questions worth raising at consultation
- What a GP referral involves and how to obtain one
About Dr Beldholm

I am Dr Bernard Beldholm, a Specialist Surgeon with Fellowship of the Royal Australasian College of Surgeons (FRACS). My practice is based at Lorn in the Hunter Valley, NSW, and my AHPRA medical registration number is MED0001186274.
For more than 15 years, my practice has focused on body contouring surgery after significant weight loss and after pregnancy. This focus means that the patients I see, the consultations I run, and the operations I perform are largely the same kinds of cases every week. Abdominoplasty after weight loss is one of the most common procedures I perform.
Where I operate
All surgery is performed at Maitland Private Hospital, which has 24-hour doctor cover and an on-site intensive care unit. I do daily rounds while patients are admitted, and my team provides in-hospital care from admission through to discharge.
The patients I see
My patient population includes:
- Patients who have had bariatric surgery (gastric sleeve, gastric bypass, and related procedures) and have reached a stable weight
- Patients who have lost significant weight through medical weight-loss programs or lifestyle change
- Patients after one or more pregnancies with loose abdominal skin and abdominal wall changes
- Patients who have previously had abdominal surgery and are returning for revision procedures
Where patients come from
Patients travel to see me from across New South Wales, including Sydney, the Central Coast, Newcastle, and the Hunter, and occasionally from interstate. The practical arrangements for patients travelling longer distances are covered later on this page.
Preparing for Surgery

Whether your operation is a standard abdominoplasty or a more extensive circumferential or Fleur-de-Lis procedure, the preparation beforehand is a substantial part of the process. For patients having a single comprehensive operation, the preparation matters even more, because the demands on the body during a longer operation are greater.
Preparation happens across several areas at once: nutrition, weight stability, medical optimisation, and smoking. These are discussed in detail at the first consultation and revisited at the second consultation before surgery is booked.
Nutrition
Many patients who come to my clinic after significant weight loss, particularly after bariatric surgery, have nutritional deficiencies that are not obvious without blood tests. Low protein, iron, vitamin D, vitamin B12, and zinc are common. These deficiencies affect wound healing, scar quality, and recovery.
At the first consultation I arrange a pre-operative blood test and provide a nutrition guide. The results guide two things:
- Tier 1 supplements: a baseline set that most post-weight-loss patients start on immediately.
- Tier 2 supplements: additional supplements added for specific deficiencies identified on blood tests.
A dietitian review is also arranged for bariatric-history patients during the inpatient phase.
Weight stability

I ask patients to maintain a stable weight for at least 6 months, and ideally 12 months, before surgery. Weight fluctuations greater than 1 to 2 kg per month are a reason to defer. There are two reasons:
- Surgery on still-changing tissue can compromise the long-term result.
- Further weight loss after surgery tends to produce new loose skin, undoing some of what the operation achieved.
Most post-bariatric patients reach a stable weight 12 to 18 months after their bariatric procedure. Some patients take longer, which is fine; the right time is when the weight stops changing.
What preparation looks like in practice
Between the first consultation and surgery, patients typically work through:
- Pre-operative blood tests
- Starting Tier 1 supplements immediately
- Adding Tier 2 supplements where indicated
- Stopping nicotine in all forms (cigarettes, e-cigarettes containing nicotine, and nicotine replacement) for a minimum of 4 weeks before and after surgery
- Optimising chronic conditions with their GP, such as blood pressure and diabetes control
- A phone consultation with the anaesthetist before surgery
- Stopping specific supplements (fish oil, vitamin E, ginkgo biloba, high-dose vitamin C) in the week before surgery
- Fasting per ANZCA guidelines on the day of surgery
Most patients go from first consultation to surgery in 1 to 3 months, depending on the pace at which these steps are worked through.
Consultation Process

Before surgery is booked, most patients meet with me at least twice. The first consultation focuses on assessment and planning. The second reviews blood test results and confirms readiness to proceed. Patients who want more time or have additional questions can book a third consultation at no extra cost. Most patients go from first consultation to booked surgery in 1 to 3 months, depending on the pace of the workup and the surgical schedule at Maitland Private Hospital.
Getting a GP referral

A GP referral is required for all consultations. Your GP should include a brief summary of your weight-loss history, current medical conditions and medications, and any specific concerns about the abdominal skin or wall. If you are considering a Medicare rebate, ask your GP to note the functional symptoms of excess skin (rashes, irritation, skin infections) in the referral letter.
Your first consultation
The first consultation takes about one hour. It covers:
- Your medical history, weight-loss history, current health, and any previous surgery
- A physical examination of the abdominal wall, including the pattern of loose skin, any muscle separation, and any hernias
- Standardised clinical photographs taken in a private changing facility
- A discussion of which abdominoplasty procedure best matches your pattern, with the risks, recovery, and hospital stay explained
- A blood test form, a copy of the pre-surgery nutrition guide, and instructions to start Tier 1 supplements immediately
Your second consultation
The second consultation is usually scheduled 2 to 4 weeks after the first. It covers:
- Review of your blood test results
- Any Tier 2 supplements to add for identified deficiencies
- Further discussion of the surgical plan, with any additional questions answered
- Confirmation of your readiness to proceed with booking a surgery date
Anaesthetic consultation
The anaesthetic consultation is conducted by phone with one of the anaesthetists at Maitland Private Hospital. It covers your medical history, current medications, and any specific concerns regarding anaesthesia. A final in-person examination by the anaesthetist takes place on the day of surgery.
Fees and quotes
A written quote is prepared in two stages:
- My patient coordinator prepares the surgical fees within 1 to 2 days of your decision to proceed, including MBS item numbers where your surgery meets the criteria and GST where the procedure is cosmetic.
- Hospital and anaesthetist estimates are added over the following 1 to 2 weeks.
The hospital team handles the private health insurance check. Patients with appropriate private cover usually do not pay the hospital portion out of pocket.
Telehealth for patients outside the Hunter
For patients who do not live in the Hunter Valley or nearby regions, the initial consultation can be conducted by telehealth. The examination is a key part of surgical planning, however, so an in-person consultation is required before surgery can be booked. Telehealth follow-ups after surgery are available where clinically appropriate.
Hospital Stay and Recovery
Every abdominoplasty after weight loss is performed at Maitland Private Hospital and followed by a structured recovery program. Recovery has two phases: the inpatient stay immediately after surgery, and the first several months afterward with regular follow-up at my Lorn clinic.
Hospital stay
The length of hospital stay depends on the procedure. A standard abdominoplasty typically requires 1 to 3 nights. A circumferential abdominoplasty (belt lipectomy) requires approximately 2 to 3 nights. The most extensive procedure, a circumferential hybrid abdominoplasty, requires 5 to 7 nights. Extended abdominoplasty and Fleur-de-Lis operations typically fall within this range, depending on the individual case. The expected stay is confirmed at pre-operative planning.
I see patients daily while they are admitted. A dietitian review is arranged during the inpatient phase for patients with a bariatric surgery history. The hospital has 24-hour doctor cover and an on-site intensive care unit.
The first two weeks after discharge
The first two weeks are the most intensive phase of recovery. Patients attend my Lorn clinic 2 to 3 times per week during this period for:
- Nurse and doctor review of wound healing
- LED light therapy to reduce inflammation
- Dressing changes, including replacement of the PICO negative-pressure dressing with Hypafix tape around day 7
- Adjustment of the compression garment as swelling reduces
Most patients are moving around the house on day one and taking short walks by the end of the first week. Return to work depends on the procedure, the patient’s job, and healing. Desk-based work is usually possible at 2 to 4 weeks; physical work and heavy lifting usually require 6 to 8 weeks or longer.
Longer-term follow-up
After the initial two-week period, I review patients at approximately 1, 3, 6, and 12 months post-operatively. All routine follow-up is included in the procedure fee. The compression garment is typically worn for around 6 weeks, depending on the procedure. Scars continue to settle and soften over 12 to 18 months.
Patients travelling from outside the Hunter
Patients travelling from Sydney, regional NSW, or interstate are advised to stay locally for 7 to 10 days after surgery. This covers the most intensive follow-up period and allows any early concerns to be addressed in person. After this initial local stay, ongoing follow-up can continue through a combination of in-person visits and telehealth review, with the 1, 3, 6, and 12 month check-ins coordinated around the patient’s travel schedule.
Risks of abdominoplasty after weight loss

All surgery carries risks. Abdominoplasty after weight loss is major surgery. The following risks are discussed in detail at consultation, and the decision to proceed is made only once the patient has had enough information and time to consider them.
Potential risks and complications
Risks that may occur with any abdominoplasty after weight loss include:
- Bleeding. Small amounts during and after surgery are expected; larger bleeds can require return to the operating theatre or blood transfusion.
- Haematoma. A collection of blood beneath the skin flap, sometimes requiring drainage.
- Infection. Wound or deeper infection, treated with antibiotics and sometimes additional procedures.
- Seroma. A collection of clear fluid beneath the skin flap, sometimes requiring drainage in the clinic.
- Delayed wound healing. Particularly at the midline, at incision junctions, and around the belly button. May require prolonged dressing care.
- Wound breakdown (dehiscence). Part of the incision may separate during healing, requiring ongoing wound care and sometimes further surgery.
- Skin flap complications. Reduced blood flow to the skin flap can cause partial skin loss; more extensive skin loss can occur and may require further surgery.
- Deep vein thrombosis (DVT) and pulmonary embolism (PE). Blood clots in the leg veins that may travel to the lungs. These are potentially life-threatening and require immediate treatment.
- Post-operative pain. Abdominoplasty is a major operation and post-operative pain is expected. Pain management is provided throughout the hospital stay and after discharge; some patients experience ongoing discomfort for weeks after surgery.
- Changes in skin sensation. Numbness and altered sensation in the lower abdomen are expected after abdominoplasty. Some areas of altered sensation may be permanent.
- Asymmetry. Small differences between the two sides of the abdomen or waistline may be present after healing.
- Fat necrosis. Areas of fatty tissue beneath the skin may lose blood supply, causing firm lumps that usually resolve over months but sometimes require treatment.
- Complications involving the belly button (umbilicus). These include altered position, altered shape, or partial or complete loss.
- Need for revision surgery. Further surgery may be required to address complications, asymmetry, or unsatisfactory healing.
- Anaesthetic complications. Reactions to anaesthesia, airway complications, and other serious anaesthetic events.
- Dissatisfaction with the aesthetic outcome. The shape, contour, or scar appearance may not meet every patient’s expectations.
Circumferential procedures, Fleur-de-Lis, dual-vector, and circumferential hybrid abdominoplasty involve longer operating times and more extensive incisions, which increase the likelihood of several of the above complications. Your specific risk profile is discussed at consultation based on the procedure recommended for your pattern.
Scar permanence
Every abdominoplasty after weight loss leaves a permanent scar. The location, length, and visibility of the scar depend on the procedure:
- A standard or extended abdominoplasty leaves a low horizontal scar that can be covered by underwear.
- A Fleur-de-Lis or dual-vector abdominoplasty adds a vertical scar running up the midline, and in the case of dual-vector, a further upper-abdominal scar. These vertical and upper scars do not hide under most clothing.
- A circumferential abdominoplasty leaves a horizontal scar that extends right around the waist.
- A circumferential hybrid abdominoplasty combines the circumferential scar with a vertical midline scar.
Scar appearance continues to change over 12 to 18 months, generally becoming paler and flatter with time. Factors that affect final scar quality include genetic skin type, smoking status, nutrition, adherence to scar care, and the tension on the wound during healing. Some scars become wider, thicker, or more pigmented than others, and these outcomes cannot be predicted in advance for any given patient.
Individual variation
The risk profile for each patient is different. It depends on the procedure performed, general health, any chronic conditions, nicotine history, nutritional status, and other factors. Part of the purpose of the consultation process is to identify and address modifiable risk factors before surgery is booked, and to ensure that each patient proceeds with a clear understanding of what can go wrong as well as what the operation is intended to achieve.
Frequently Asked Questions
What is abdominoplasty after weight loss?
Abdominoplasty after weight loss, also called a post-weight-loss tummy tuck, is a surgical procedure that removes excess skin and, in most cases, fatty tissue from the abdomen, and repairs separated abdominal muscles (diastasis recti) where present. It is commonly used to treat the loose abdominal skin that remains after significant weight loss, whether through bariatric surgery, medical weight-loss programs, or lifestyle change. It is not a weight-loss procedure in itself.
Which type of abdominoplasty is right for me?
There is no single answer without an examination. Standard abdominoplasty suits patients whose loose skin is concentrated on the lower abdomen. Extended abdominoplasty extends the incision to treat the flanks. Fleur-de-Lis abdominoplasty addresses both vertical and horizontal skin laxity. Circumferential abdominoplasty (belt lipectomy) treats 360-degree skin laxity around the lower trunk. The matching procedure depends on the pattern of loose skin, which is assessed at consultation.
Can loose abdominal skin after weight loss be treated without surgery?
Non-surgical treatments such as creams, radiofrequency devices, and compression garments do not remove loose skin. After significant weight loss, stretched skin does not retract to its previous state because the underlying collagen and elastin fibres have been disrupted. For patients with substantial loose skin, surgery is usually the only effective option.
Where is surgery performed?
All abdominoplasty surgery is performed at Maitland Private Hospital in the Hunter Valley, NSW. The hospital has 24-hour doctor cover and an on-site intensive care unit. Consultations take place at Dr Beldholm’s clinic in Lorn, NSW.
Does Medicare cover abdominoplasty after weight loss?
A Medicare rebate may apply under MBS item 30177 where specific criteria are met. These include documented weight loss of at least 5 BMI units, weight stable for a minimum of 6 months, and functional symptoms attributable to the excess skin, such as recurrent rashes, skin irritation, or infections that have not responded to non-surgical management. Eligibility is assessed individually at consultation. Abdominoplasty performed for purely cosmetic reasons does not qualify for a Medicare rebate.
How soon after reaching goal weight can I have surgery?
A minimum of 6 months at stable weight is recommended before abdominoplasty, with 12 months preferred. Most patients who have had bariatric surgery reach a stable weight 12 to 18 months after their procedure. Operating while weight is still changing can compromise the long-term result and may produce new loose skin once further weight is lost.
Book a consultation
The next step is a consultation. In-person consultations are held at Dr Beldholm’s Lorn clinic in the Hunter Valley. Telehealth consultations are available for patients outside the region.
Or call the clinic on (02) 4934 5700.
Dr Beldholm’s companion guide, 7 Surgical Options for Loose Skin After Weight Loss, covers the seven procedures most often considered after significant weight loss. It explains how to identify your pattern of loose skin, what each procedure involves, and what to expect from recovery.

