Breast Lift (Mastopexy) After Pregnancy or Weight Loss
A breast lift (mastopexy) repositions the nipple-areola complex and reshapes breast tissue to address breast ptosis (drooping) after pregnancy, breastfeeding, weight loss, or changes over time.
My Approach to a Breast Lift (Mastopexy)

When you come to me considering a breast lift (mastopexy), the first thing I want to understand is what you have noticed and what you would like to address.
Some patients are most concerned about the position of the nipple-areola complex. Others are bothered more by skin laxity or the shape of the lower pole. Some want both, with added fullness in the upper pole as well.
The right operation depends on which of these matters most to you, and on what your anatomy will allow.
There is no single breast lift (mastopexy) technique that suits every patient. The incision pattern is chosen to fit your anatomy:
- Doughnut (peri-areolar): where the skin excess is small and the nipple-areola complex requires only modest repositioning
- Lollipop (vertical): where there is moderate skin excess
- Inverted-T (anchor): where there is significant excess
The choice follows from your pattern, not the other way around.
I am clear about what a breast lift (mastopexy) will and will not do. The operation repositions and reshapes. It does not create upper pole fullness in a breast that has lost volume.
Where added fullness matters to you, we discuss whether your own tissue can be reshaped to achieve it (auto-augmentation), or whether an implant-based approach would suit you better. These options are explored at consultation and in the patient guide.
A breast lift (mastopexy) is a personal decision. I encourage you to take your time, ask questions, and seek a second opinion if it would help.
Is a Breast Lift (Mastopexy) Right for me?

Suitability for a breast lift (mastopexy) depends on several factors: what you have noticed, your anatomy, your overall health, and your goals. The information below is a useful starting point for your own thinking. A clinical assessment at consultation is what determines whether a breast lift (mastopexy) is appropriate for you.
Common reasons women consider a breast lift (mastopexy)

Patients commonly seek a consultation when they notice:
- The nipple-areola complex sitting at or below the inframammary fold (the natural crease where the breast meets the chest)
- Stretched skin and a less full breast shape after pregnancy and breastfeeding
- Loss of volume and a flatter upper pole after significant weight loss
- Gradual changes in breast position over time
- Asymmetry between the two sides
An at-home indicator sometimes referred to as the pencil or ruler test can be useful. If your nipple sits at or below the level of your inframammary fold, this is consistent with some degree of breast ptosis (drooping). It is an indicator only. It does not determine which surgical approach is appropriate, or whether surgery is suitable for you at all. Those questions are answered at consultation.
When a breast lift (mastopexy) may not be the right answer

A breast lift (mastopexy) is not appropriate for every patient who experiences breast ptosis. Considerations that may delay or change the surgical plan include:
- Future pregnancy plans. Subsequent pregnancies will affect breast shape and may reverse the results of surgery
- Plans to breastfeed in future. Some breast lift (mastopexy) techniques can affect breastfeeding capacity, and this is discussed before any decision is made
- Active smoking. Smoking significantly increases the risk of wound healing problems and skin or nipple-areola complex tissue loss. Smokers are asked to stop for at least six weeks before and after surgery
- Weight not yet stable. Further weight changes after surgery will affect the result. Patients are generally asked to be at a stable weight for around six months
- Pseudoptosis. In some cases the nipple-areola complex sits in a normal position but the lower pole appears full or sagging. This presents differently, and a standard breast lift (mastopexy) may not be the most appropriate approach
- Minimal ptosis where added volume is the main concern. Augmentation alone may achieve the goal in some patients, without the additional incisions of a breast lift (mastopexy)
- Active breast disease or recent breast cancer treatment. Surgical planning differs in these situations and is coordinated with your treating breast specialist
A consultation provides an individualised assessment and clarifies which of these considerations apply to you.
How a Breast Lift (Mastopexy) is Matched to your Pattern
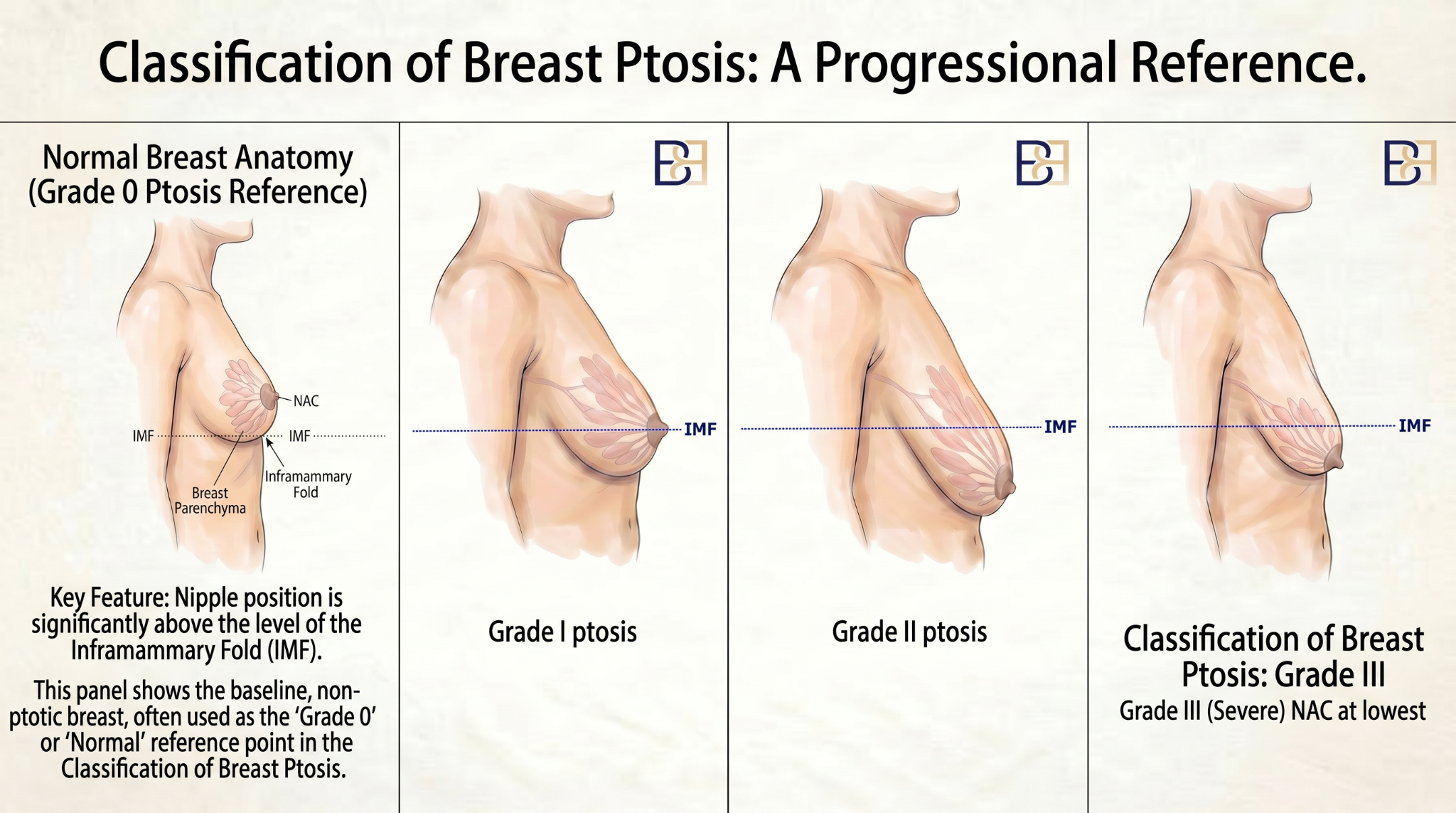
A breast lift (mastopexy) is not one operation. The technique chosen depends on the pattern of breast ptosis, the position of the nipple-areola complex, the amount of skin excess, and whether breast volume has changed.
Some terms that appear below:
- Ptosis: drooping. Breast ptosis is commonly graded as mild, moderate, or severe (the Regnault classification).
- Nipple-areola complex (NAC): the nipple and the surrounding pigmented skin (areola).
- Inframammary fold (IMF): the natural crease where the lower edge of the breast meets the chest wall.
- Lower pole: the lower half of the breast, from the nipple to the inframammary fold.
The patterns below describe typical presentations and the techniques generally appropriate for each. Suitability is assessed at consultation.
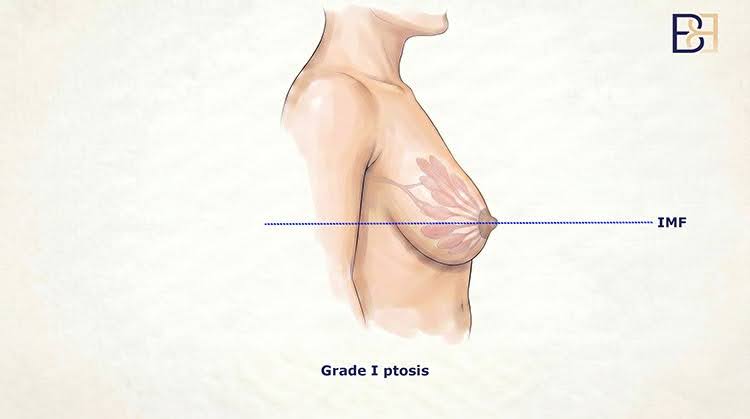
Mild ptosis (Grade 1)
The nipple-areola complex sits at the level of the inframammary fold. Skin excess is small. Breast volume is generally adequate.
Technique generally appropriate: Doughnut (peri-areolar) incision. The incision sits around the edge of the areola only. The skin envelope is tightened a small amount and the nipple-areola complex is repositioned slightly higher.
What this looks like: a single circular scar around the areola.
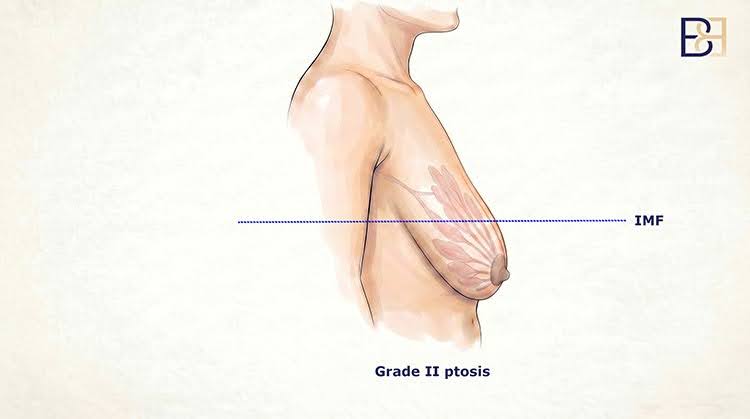
Moderate ptosis (Grade 2)
The nipple-areola complex sits below the inframammary fold but above the most dependent (lowest) part of the breast contour. Skin excess is moderate. The lower pole has stretched.
Technique generally appropriate: Lollipop (vertical) incision. The incision goes around the areola and continues vertically down to the inframammary fold. The skin envelope is tightened, the lower pole is reshaped, and the nipple-areola complex is repositioned higher.
What this looks like: a scar around the areola plus a vertical scar from the areola down to the inframammary fold.
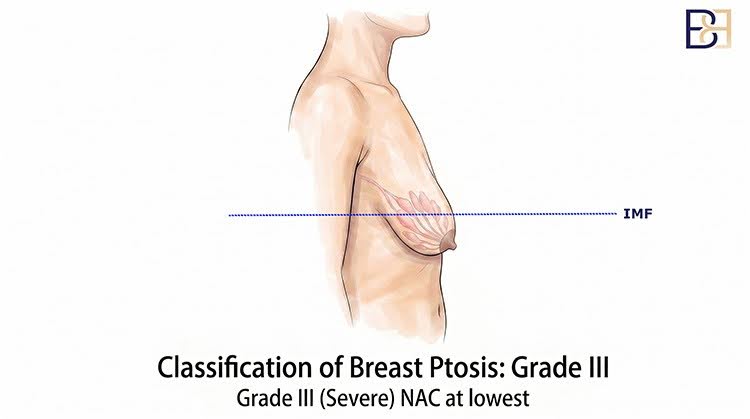
Severe ptosis (Grade 3)
The nipple-areola complex sits at the most dependent (lowest) part of the breast, with two-thirds or more of the breast tissue below the inframammary fold. Skin excess is significant.
Technique generally appropriate: Inverted-T (anchor, or Wise pattern) incision. The incision goes around the areola, vertically down to the inframammary fold, and along the inframammary fold itself. This allows the largest amount of skin to be removed where the nipple-areola complex needs to be moved a significant distance higher.
What this looks like: a scar around the areola, a vertical scar to the inframammary fold, and a horizontal scar along the inframammary fold.
This pattern is common in patients after significant weight loss, and in some patients after multiple pregnancies.
Ptosis with volume loss
Some patients, particularly after significant weight loss, present with ptosis combined with reduced breast tissue volume. A standard breast lift (mastopexy) repositions and reshapes the existing tissue, but does not restore upper pole fullness where volume has been lost.
Techniques generally discussed:
- Auto-augmentation breast lift (mastopexy). The patient’s own breast tissue is dissected from the skin envelope, reshaped, and secured in a higher position on the chest wall. The skin is then re-draped over the new tissue position. This gives upper pole fullness using the patient’s own tissue, without an implant. It is a longer and more technically demanding operation than a standard breast lift (mastopexy).
- Combined breast lift (mastopexy) with implants. Where added volume beyond what the patient’s own tissue provides is desired, implants may be combined with the breast lift (mastopexy) in one operation, or in a staged approach. This is a separate clinical decision and is covered in detail in the patient guide.
A note on lower pole tightening
All breast lift (mastopexy) techniques involve some lower pole tightening, which results in a mild reduction in lower pole volume. This is intrinsic to the operation and is part of how breast shape is restored. The breast is not made smaller in the way a Reduction Mammoplasty (breast reduction) would do. Reduction Mammoplasty is a different operation and is discussed at consultation if it may apply to your situation.
Patient Guide: 4 Breast Lift (Mastopexy) Options
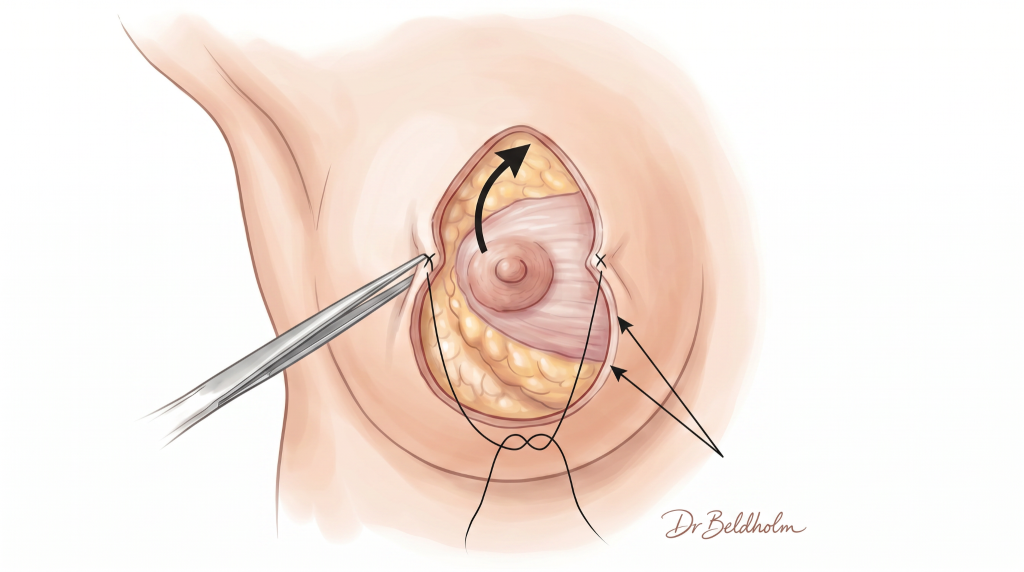
The patient guide expands on the four main breast lift (mastopexy) approaches in depth: how they differ, who each is generally suited to, and the trade-offs involved.
Inside:
- Standard breast lift (mastopexy): what is involved, who it is generally suited to, and the incision options
- Auto-augmentation breast lift (mastopexy): using your own tissue for upper pole fullness without an implant, particularly relevant after weight loss
- Combined breast lift (mastopexy) with implants: when a single operation is medically suitable, and the trade-offs involved
- Staged breast lift (mastopexy) and breast augmentation: when separating the two operations may be the more appropriate clinical choice
- How Reduction Mammoplasty (breast reduction) differs from a breast lift (mastopexy), and when it may apply
About Dr Beldholm

I am Dr Bernard Beldholm, M.B.B.S, B.Sc (Med), FRACS, a Specialist General Surgeon based in the Hunter Valley. My AHPRA Medical Registration number is MED0001186274.
I have more than 15 years of operative experience. My clinical focus is on breast surgery and on body contouring after pregnancy and significant weight loss. The breast lift (mastopexy) is one of the procedures I perform regularly.
I operate at Maitland Private Hospital, where there is 24-hour medical cover and an on-site intensive care unit. For body contouring patients where surgery may be more involved, I prefer this level of perioperative cover.
For more about my background, please see my full profile.
Preparing for Breast Lift (Mastopexy) Surgery
Good preparation improves your experience of surgery and your recovery. The points below are the ones I discuss with most patients before a breast lift (mastopexy). Your individual preparation is finalised at consultation, taking your medical history into account.
Health and lifestyle

If you have other medical conditions such as diabetes or hypertension, I want these to be well-controlled before surgery. Pre-operative blood tests are arranged to check anaemia, kidney function, and other relevant markers. Your GP and I work together where needed.
Smoking and nicotine products significantly increase the risk of wound healing complications, skin loss, and nipple-areola complex tissue loss after a breast lift (mastopexy). I ask patients to stop smoking and using nicotine products, including vapes and patches, for at least six weeks before and after surgery.
Future weight changes will affect the result of a breast lift (mastopexy). I generally ask patients to be at a stable weight for around six months before surgery, which means within a few kilograms either way.
Future pregnancy and breastfeeding
If you are planning a pregnancy in the near future, surgery is generally deferred. Pregnancy will affect breast shape and may reverse the results.
If you are planning to breastfeed in the future, this is discussed before any decision is made. Some breast lift (mastopexy) techniques can affect breastfeeding capacity. The technique chosen and the timing of surgery take this into account.
Medications and pre-operative investigations
Some medications and supplements affect bleeding risk and need to be paused before surgery. These include aspirin, anti-inflammatory medications, fish oil, and certain herbal supplements. I provide a written list of what to stop and when at consultation. Other regular medications are reviewed and continued or paused as appropriate.
Depending on your age and breast history, breast imaging such as a mammogram or ultrasound may also be arranged before surgery.
Practical preparations
In the days before surgery, you may wish to:
- Arrange transport home from hospital
- Have someone available to help at home for the first 24 to 48 hours
- Prepare loose, front-opening clothing that does not need to go over your head
- Set up a comfortable resting area at home
A detailed pre-admission checklist is provided after your consultation.
What to Expect at Consultation

A consultation is required before any surgical decision. A current GP referral is needed to attend.
Booking your first consultation
You can book online, or by telephoning the practice to speak with a receptionist. The first consultation can be in-person at Lorn in the Hunter Valley, or by Zoom. At least one in-person consultation is required before surgery.
The first consultation
The first consultation is one hour. We cover:
- Your medical and breast history, including pregnancies, breastfeeding, family history, and any prior breast surgery
- What you have noticed and what you would like to address
- Your goals and any concerns
I perform a physical examination. Clinical photographs are taken with your consent, including anterior and lateral views, which form part of the surgical planning. I routinely use 3D imaging during the consultation as a visual aid for discussion. Simulated images are illustrative only.
We then discuss the techniques that suit your pattern. The patient guide outlines the main approaches in detail; consultation is where the discussion is individualised to you. If pre-operative investigations are needed, such as breast imaging or blood tests, these are arranged.
You leave the first consultation with information to consider. There is no expectation to make a decision on the day.
The follow-up consultation
A second consultation is part of my clinical standard for breast lift (mastopexy) patients. This may be in-person or by Zoom, depending on circumstances. We review any investigation results, refine the surgical plan, and answer further questions.
The surgical coordinator provides a detailed written quote covering the surgeon’s fees, anaesthetist’s fees, hospital fees, and any other relevant costs. Surgery is scheduled if you decide to proceed.
Between consultations
I encourage every patient to take time between consultations to consider the information, ask further questions, and seek a second opinion if it would help. There is no rush to proceed before you feel ready.
Book your appointment online now
Hospital and Recovery

A breast lift (mastopexy) is performed at Maitland Private Hospital under general anaesthetic. The hospital provides 24-hour medical cover and an on-site intensive care unit.
Day of surgery
The operation is typically performed as a day-stay procedure, which means most patients are discharged the same day. You arrive in the morning, the surgery is performed, and you go home in the afternoon or early evening. A responsible adult is required to drive you home and stay with you for the first 24 hours.
You go home in a compression garment. A second garment is provided so you can rotate them while one is being washed. Drains are not routinely used after a breast lift (mastopexy).
The first week

Pain after a breast lift (mastopexy) is generally manageable with regular paracetamol and an anti-inflammatory medication. A short course of stronger analgesia is provided in case it is needed.
You can shower the day after surgery in most cases. Detailed wound and dressing care instructions are provided on discharge.
I ask patients to:
- Sleep on their back, propped up on pillows
- Avoid lifting anything heavier than a kettle for the first week
- Avoid raising arms above shoulder height for the first two weeks
- Take regular short walks each day
Returning to normal activity

Most patients return to a desk-based job within 3 to 5 days. Physical jobs require longer time off, discussed individually at consultation.
Walking can be increased over the first 2 to 3 weeks. Full exercise, including running, weights, and chest workouts, is generally resumed at around 4 weeks.
Most of the early swelling settles by around 4 weeks. The final shape continues to settle over the following 3 to 6 months as the tissues soften and the scars mature.
Recovery experience varies between patients. Individual timelines are discussed at consultation.
Follow-up schedule
In the first two weeks after surgery, the practice nurse and I see patients 2 to 3 times per week to monitor healing and address any concerns.
After this period, follow-up appointments are at:
- 1 month
- 3 months
- 6 months
- 12 months
Further follow-up is arranged as needed.
Risks of Breast Lift (Mastopexy) Surgery

All surgery carries risks. A breast lift (mastopexy) is no exception. The information below is a summary of the main risks. Each risk is discussed in detail at consultation, and the discussion is documented as part of informed consent.
Risks specific to a breast lift (mastopexy)
- Bleeding and haematoma. A collection of blood may form under the skin, sometimes requiring further surgery to drain.
- Infection. Wound infections may occur and may require antibiotics or, less commonly, further surgical intervention.
- Seroma. A collection of clear fluid that may need to be drained.
- Delayed wound healing. Healing can be slower at the junction of incisions, particularly where the vertical and horizontal incisions meet in an inverted-T pattern.
- Wound dehiscence. Wounds may separate after surgery, particularly if there is excessive tension on the closure or other healing factors are present.
- Sensation changes. Sensation in the nipple or breast skin may be reduced, increased, or absent. These changes are sometimes permanent.
- Asymmetry. Some asymmetry between the two breasts is common and may be more noticeable than expected. Revision surgery is sometimes required.
- Unfavourable scarring. Scars may become thickened (hypertrophic), raised (keloid), widened, or pigmented. Scar maturation takes 12 to 18 months.
- Fat necrosis. Areas of breast tissue may not survive the surgery and can form firm lumps that may require investigation or removal.
- Nipple-areola complex viability. In some cases the blood supply to the nipple-areola complex is compromised. Partial or, rarely, complete loss of the nipple-areola complex can occur. This risk is higher in significant lifts, in smokers, and where prior breast surgery has affected the blood supply.
- Recurrence of ptosis. Breast position changes over time, with future weight changes, or with subsequent pregnancies.
- Need for revisional surgery. Revision may be needed for any of the above complications or for aesthetic refinement.
General surgical and anaesthetic risks
- Anaesthetic risks. These are discussed separately with the anaesthetist before surgery.
- Deep vein thrombosis (DVT) and pulmonary embolism. Blood clots in the leg veins or lungs are uncommon but serious. Steps are taken to reduce this risk before, during, and after surgery.
- Allergic reactions. Reactions to medications, dressings, or other materials used during surgery.
Effects on breastfeeding
A breast lift (mastopexy) may affect future breastfeeding capacity. The extent of any effect depends on the technique used and individual factors. This is discussed in detail at consultation, particularly if you are planning to breastfeed in the future.
The risks above are discussed in detail at consultation as part of the informed consent process. A more comprehensive list is also available on the breast lift (mastopexy) risks page.
Frequently Asked Questions
Do I need a GP referral?
Yes. A current GP referral is required to attend a consultation with Dr Beldholm. The referral allows the consultation to be considered by Medicare and arranges the formal handover of clinical care. If you do not have a GP, the practice can suggest options.
Will I be able to breastfeed after a breast lift (mastopexy)?
A breast lift (mastopexy) may affect future breastfeeding capacity. The extent of any effect depends on the technique used, the amount of tissue rearrangement involved, and individual factors. Some patients breastfeed without difficulty after surgery; others find their supply is reduced; some are unable to breastfeed. If you are planning to breastfeed in the future, this is an important part of the consultation discussion and influences the timing of surgery and the technique chosen.
Will the scars be visible?
A breast lift (mastopexy) leaves permanent scars. The scar pattern depends on the technique used, as outlined earlier on this page. Most scars sit within the bra or swimwear line and are not visible when clothed. Scar maturation takes 12 to 18 months, during which time scars typically fade. Individual scarring varies, and some patients are more prone to thickened or pigmented scars than others.
Can a breast lift (mastopexy) be combined with implants?
A breast lift (mastopexy) can be combined with implants in a single operation, or the two procedures can be staged with the breast lift (mastopexy) performed first and implants placed approximately six months later. The choice between combined and staged depends on individual factors including the size of the lift required, breast tissue quality, and overall complexity. The patient guide covers the four main approaches in detail.
Is a breast lift (mastopexy) covered by Medicare or private health insurance?

Most breast lift (mastopexy) operations are performed for cosmetic reasons and are not covered by Medicare or private health insurance.
A small group of patients with severe breast ptosis meeting strict clinical criteria may have a Medicare item number that applies to the operation. Where Medicare cover applies, private health insurance may also contribute towards hospital costs depending on your level of cover.
Eligibility is assessed individually at consultation following clinical examination. Where a breast lift (mastopexy) is combined with breast augmentation, Medicare considerations differ and are discussed individually.
A detailed written quote covering all costs is provided after the consultation.
How long until I can return to normal activity?
Most patients return to a desk-based job within 3 to 5 days, increase walking over the first 2 to 3 weeks, and resume full exercise at around 4 weeks. Physical jobs require longer time off, discussed individually at consultation. Recovery experience varies between patients.
Book a Consultation
A breast lift (mastopexy) is a personal decision. The first step is a consultation, where your individual situation is assessed and the surgical options most appropriate for you are discussed.
Consultations are available in-person at Lorn in the Hunter Valley, or by Zoom. A current GP referral is required.
If you would prefer to read more first, the patient guide covers the four main breast lift (mastopexy) approaches in detail.
GP referral required. Consultation required to determine suitability. Results vary. All surgery carries risks.

