Reduction Mammoplasty (Breast Reduction): Symptoms, Surgical Options & What to Expect
For some women, persistent neck and shoulder pain, bra-strap grooving, skin irritation under the breast crease, and exercise limitation are linked to breast size. Reduction Mammoplasty (Breast Reduction) is a surgical procedure that removes excess breast tissue, glandular tissue, and fat, with the aim of reducing the physical symptoms associated with heavy or symptomatic breasts.
The procedure is performed by a Specialist Surgeon. A GP referral is required for all consultations.
This page covers the symptoms and patterns that commonly lead women to consider surgery, the questions worth thinking through before booking, the main surgical approaches, and what is involved at consultation, in hospital, and during recovery.
All surgery carries risks. Individual results vary. Consultation required to determine suitability.
The Beldholm Approach

Three principles guide how I approach reduction mammoplasty (breast reduction).
This section also addresses breast reduction performed with liposuction (suction assisted lipectomy) alone, which patients sometimes ask about as an alternative.
My usual approach to breast reduction (reduction mammoplasty)
Pattern-matching, not procedure-matching.
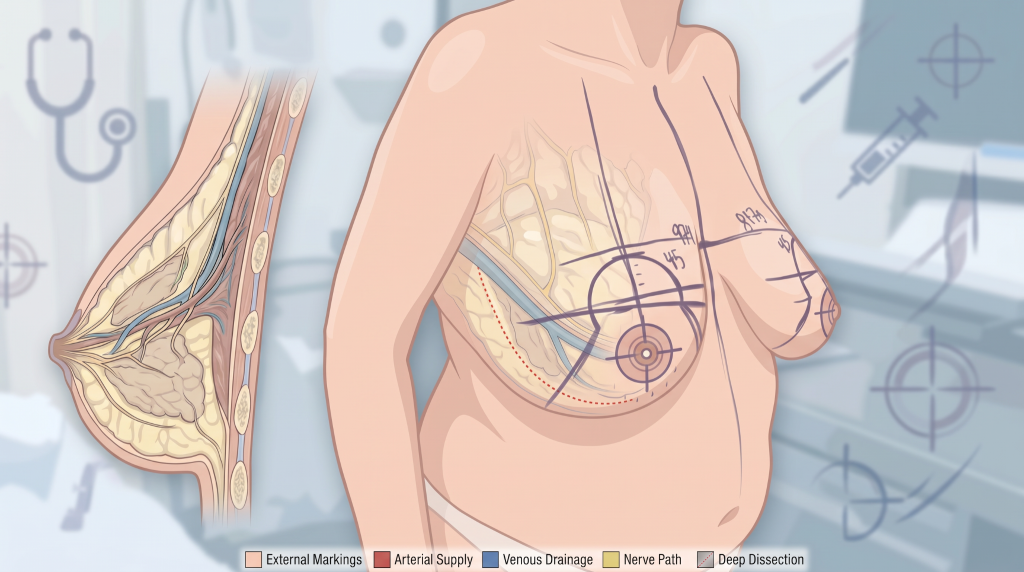
The technique should match the breast pattern, not the other way around. The amount of tissue to be removed, the position of the nipple-areolar complex, and the quality of the skin all influence which incision pattern is appropriate.
Your anatomy and symptoms determine the technique. There is no default approach I apply to everyone.
One operation where possible.
Where it makes sense clinically, I prefer to address breast volume and chest-wall contour in a single operation rather than staging them.
Reduction mammoplasty (breast reduction) addresses excess breast tissue, glandular tissue, and fat within the breast. It does not always treat the lateral breast fold or the axillary tail (the area of breast tissue that extends toward the armpit), which can contribute to chest-wall fullness adjacent to the breast.
In selected cases, I combine VASER liposuction (ultrasonic suction assisted lipectomy) with reduction mammoplasty to address these adjacent areas at the same operation.
Whether VASER liposuction (ultrasonic suction assisted lipectomy) is appropriate depends on what your physical examination shows at consultation. This is different to using liposuction (suction assisted lipectomy) as an alternative to surgical reduction, which is covered in the next section.
Pre-operative optimisation.

Reduction mammoplasty is performed under general anaesthesia. How a patient is prepared in the weeks beforehand affects healing and risk.
Smoking cessation, weight stability, and general fitness all matter. The detail of what I ask patients to do is covered further down this page under Preparing for Surgery.
Liposuction (suction assisted lipectomy) as an approach to breast reduction
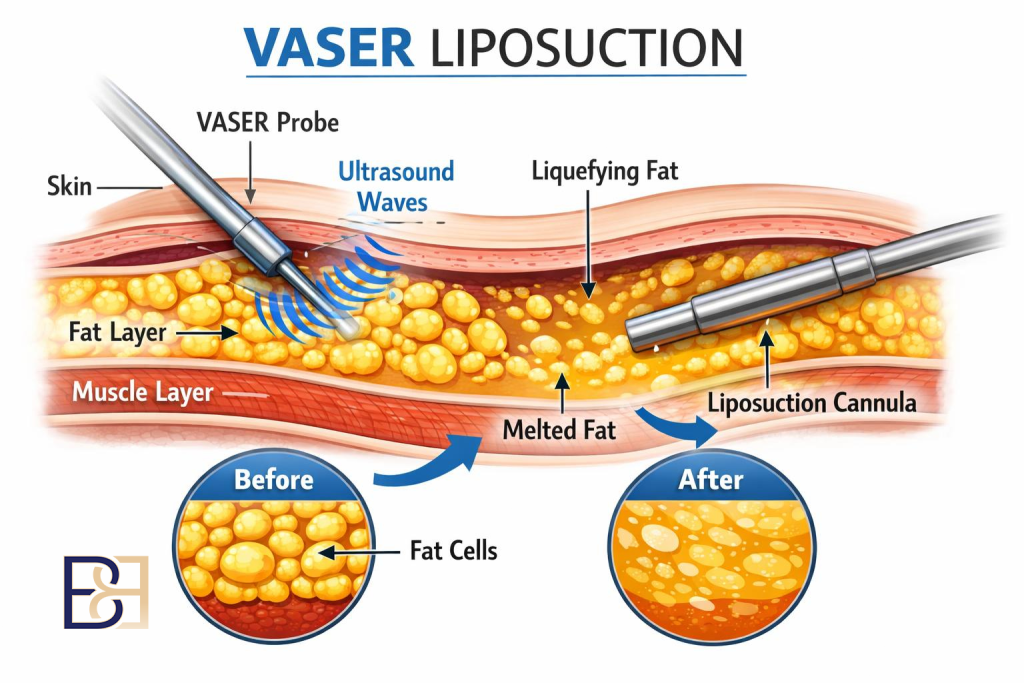
Some patients ask about reducing breast size using liposuction (suction-assisted lipectomy) alone.
This is a different technique to the VASER liposuction (ultrasonic suction-assisted lipectomy) adjunct described above. In an approach using liposuction (suction-assisted lipectomy) alone, fat is removed from the breast itself with the goal of reducing breast volume, without surgical excision of skin or repositioning of the nipple-areolar complex.
I rarely recommend this approach, for two main reasons.
First, most patients with heavy breasts have a significant component of firm glandular tissue. Glandular tissue does not respond well to liposuction (suction assisted lipectomy).
Second, when significant breast volume is removed without surgical repositioning of the nipple-areolar complex, the breast commonly develops significant ptosis afterward. Ptosis is itself a cosmetic concern and can cause new functional issues such as skin irritation under the breast crease.
There is a narrow group of patients for whom liposuction (suction assisted lipectomy) may be appropriate as a standalone approach to breast reduction. The combination is unusual, and typically requires all of the following:
- A small reduction, in the range of 1 to 2 cup sizes at most
- Good elastic skin
- No significant ptosis already present
- Breasts that are fat-predominant rather than glandular-predominant (more fat tissue than gland tissue)
Whether you fall into this group is determined at consultation, after physical examination.
Are Your Symptoms Severe Enough to Consider Surgery?

Reduction mammoplasty (breast reduction) is a significant operation. Not everyone with large breasts needs surgery, and there are reasons it may not be the right step at a particular time.
The questions below are not a substitute for clinical assessment. They are a way of thinking through whether a consultation with a Specialist Surgeon is worth booking.
Symptoms commonly associated with breast hypertrophy
The following are physical symptoms patients commonly describe at consultation:
- Neck pain, upper back pain, or shoulder pain that worsens through the day
- Bra-strap grooving, with visible indentation in the skin over the shoulder
- Skin irritation, rash, or maceration in the crease underneath the breast
- Postural change, including forward shoulder roll and mid-back ache
- Difficulty exercising or limitation in physical activity
- Difficulty fitting clothing or finding supportive bras
- Asymmetry between the two breasts that causes functional difficulty
If several of these are familiar, and they have been present for an extended period rather than a recent change, a consultation can help determine whether reduction mammoplasty is appropriate.
Reasons surgery may not be the right step right now

Some circumstances mean reduction mammoplasty is better deferred to a later time, or that other steps should be tried first. These include:
- Active weight change. If your weight is currently increasing or decreasing, breast size and shape will change with it. Surgery is generally better timed when weight has been stable for at least six months.
- Plans for pregnancy in the next 12 to 24 months. Pregnancy and breastfeeding change breast size, shape, and skin quality. Reduction mammoplasty may also affect breastfeeding ability (covered in the Risks section below). Many patients prefer to complete their family before considering surgery.
- Currently breastfeeding. Surgery is generally deferred until breastfeeding has finished and the breasts have settled, which can take several months after weaning.
- Active smoking. Smoking significantly affects wound healing and increases the risk of complications. Cessation for a defined period before and after surgery is required.
- Uncontrolled medical conditions. Diabetes, cardiovascular disease, anaemia, and other conditions need to be stable and managed before surgery is considered.
A GP referral is required for a surgical consultation. Your GP is well placed to help you decide whether the timing is right.
Book your appointment online now
Matching the Procedure to Your Pattern

There is no single technique that suits every patient. The right approach to reduction mammoplasty (breast reduction) depends on three things: how much tissue needs to be removed, where the nipple-areolar complex sits in relation to the breast crease, and the quality of the skin.
This section walks through the three main surgical techniques and the role of VASER liposuction (ultrasonic suction assisted lipectomy) as an adjunct. Which combination is appropriate for you is determined at consultation, after physical examination.
A note on terminology before the techniques
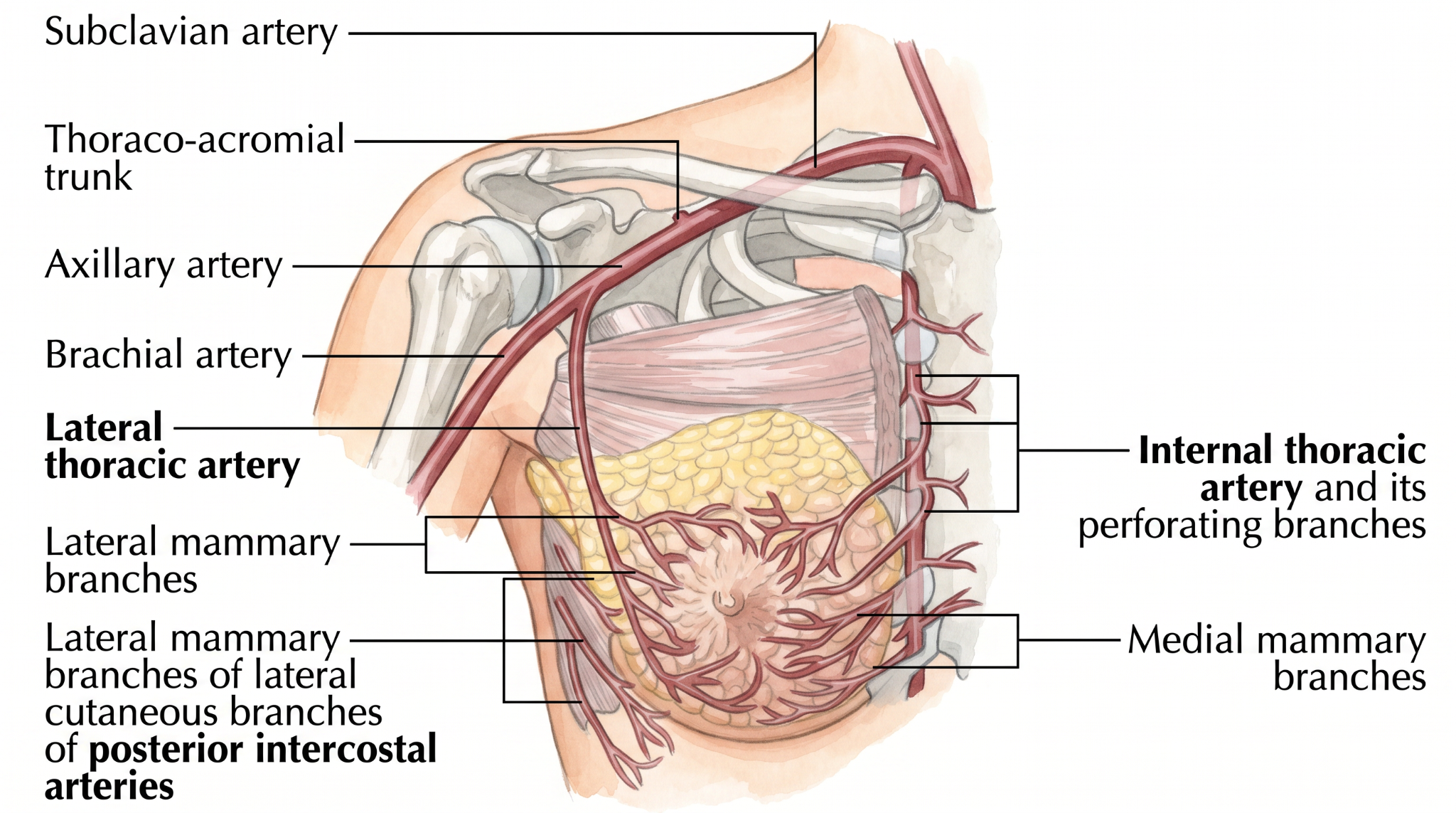
A few terms appear throughout this section.
Pedicle is the tissue connection that maintains blood and nerve supply to the nipple-areolar complex when the breast is reshaped. Different pedicle techniques (inferior, superomedial, and others) preserve this connection in different ways.
Pattern refers to the shape of the skin excision and the resulting scar (vertical, Wise, or free nipple graft).
In short, a reduction is a combination of how much tissue is removed, which scar pattern allows that volume to be removed, and which pedicle keeps the nipple-areolar complex viable.
Reduction or lift? A note before the techniques
Every surgical reduction mammoplasty (breast reduction) includes repositioning of the nipple-areolar complex, so a lift component is built into the operation. The exception is breast reduction performed using liposuction (suction assisted lipectomy) alone, which is covered earlier under The Beldholm Approach. That technique does not reposition the nipple-areolar complex.
A standalone breast lift (mastopexy) is a different operation. It lifts and reshapes the breast without the goal of reducing volume.
If a lift rather than a reduction is what is clinically appropriate for your pattern, that is determined at consultation.
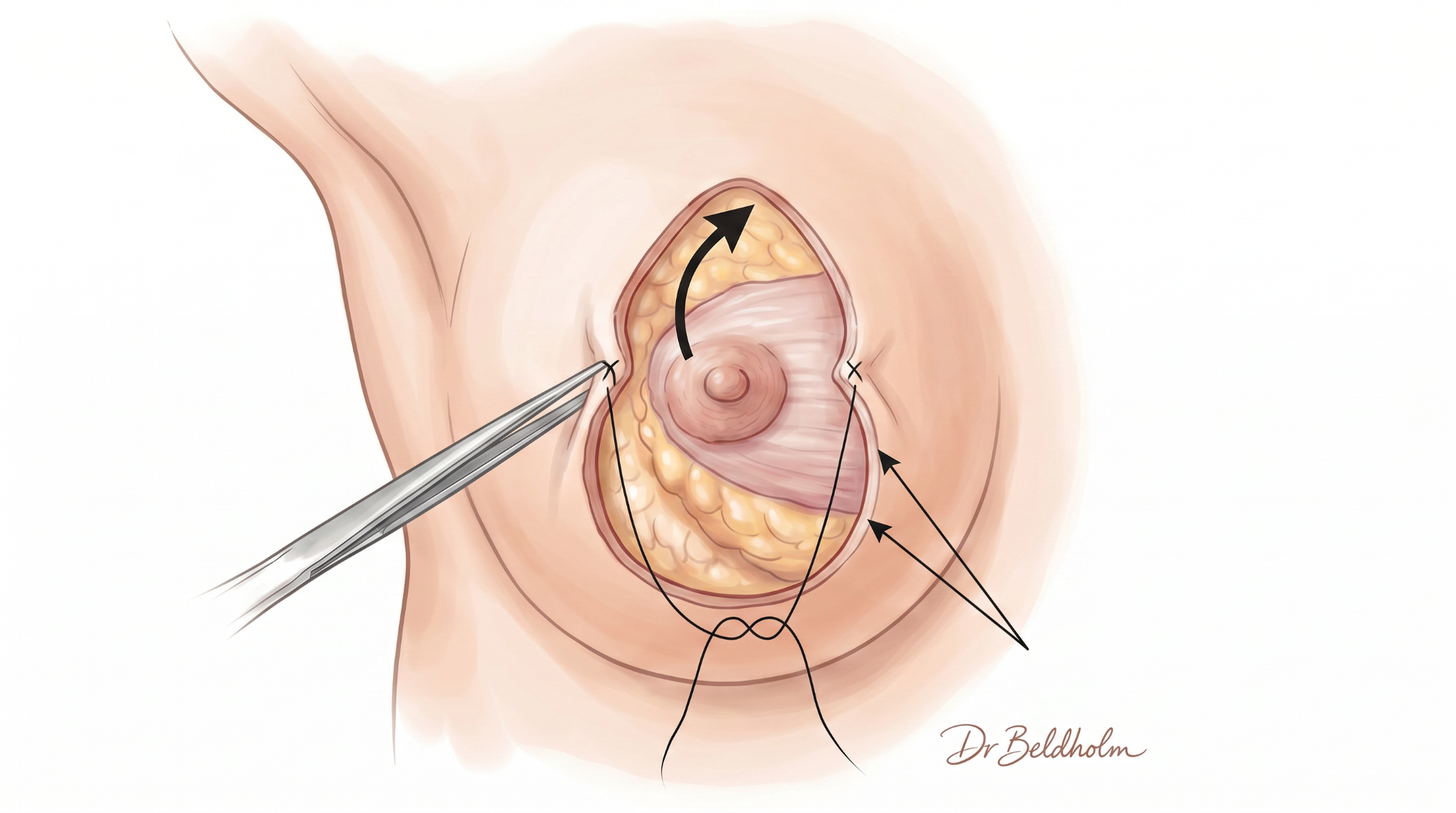
Vertical Pattern Reduction
Best for: small to moderate reductions where skin elasticity is good.
Incisions: around the areola and a vertical line down to the breast crease. Sometimes called a lollipop pattern.
Scar: circular scar around the areola, plus a vertical line below.
Limitations: less suitable for very large reductions, or where significant skin laxity is present.
Wise Pattern Reduction (Inverted-T)
Best for: moderate to larger reductions, or where significant skin laxity is present.
Incisions: around the areola, vertically down to the crease, and along the inframammary fold. Sometimes called an anchor or inverted-T pattern.
Scar: longer overall scar than the vertical pattern; allows more skin and tissue to be removed.
Limitations: longer scar, including a horizontal component along the breast crease.
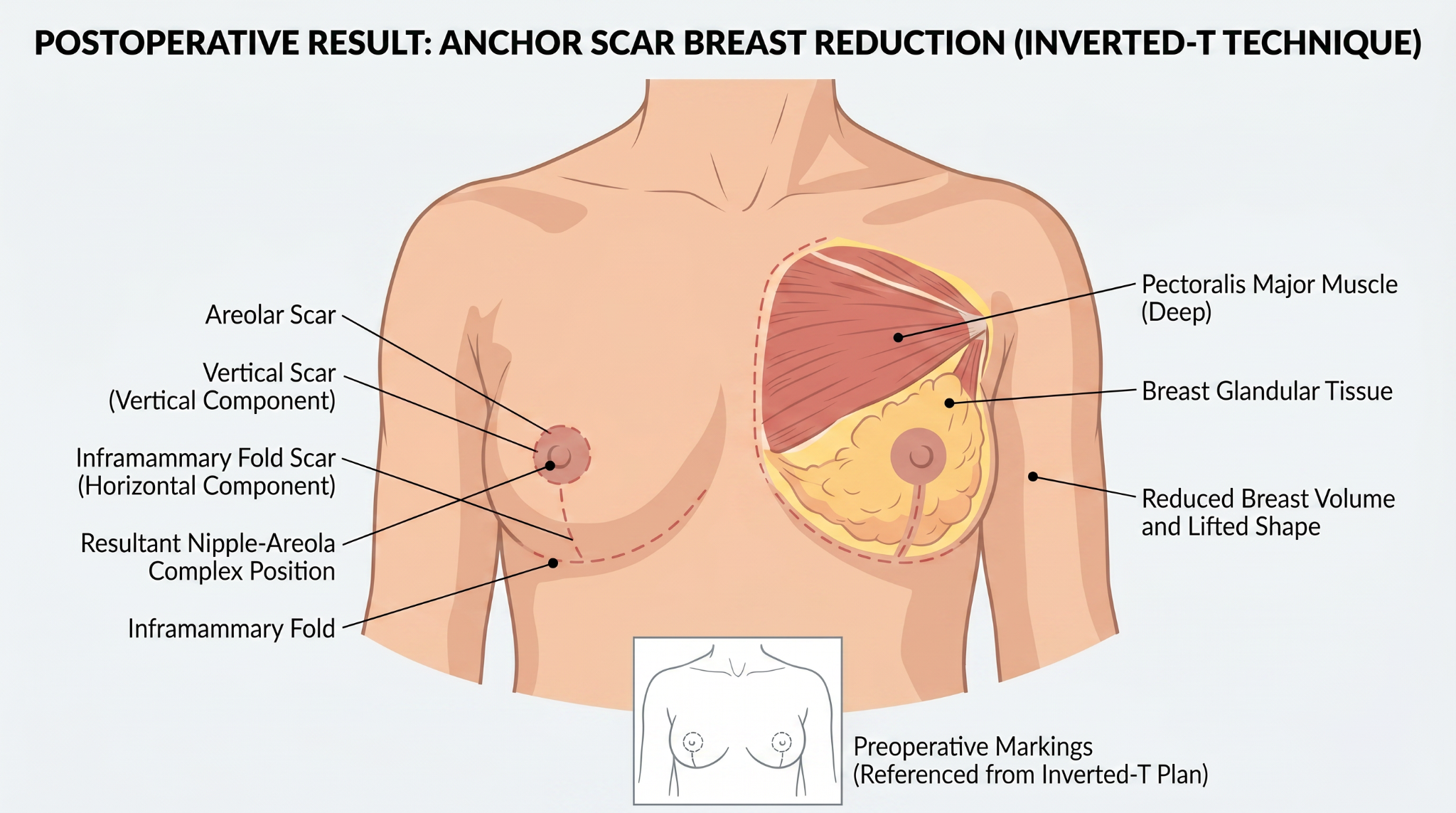
Free Nipple Graft Reduction
Best for: rarely performed. The graft has a high rate of failure, and nipple sensation is not preserved. The technique is not the default for most patients. It is only considered when a standard pedicle technique already carries a high risk of losing the nipple-areolar complex. For example, when the pedicle length required is excessive, or when significant medical issues mean a shorter operation is necessary.
Incisions: Wise pattern incisions, with the nipple-areolar complex removed and repositioned as a graft.
Scar: Wise pattern scar around the areola, vertically to the crease, and along the breast crease.
Limitations: specific implications for nipple sensation and breastfeeding ability. These are discussed in detail when this approach is being considered.
VASER Liposuction (Ultrasonic Suction Assisted Lipectomy) as an Adjunct
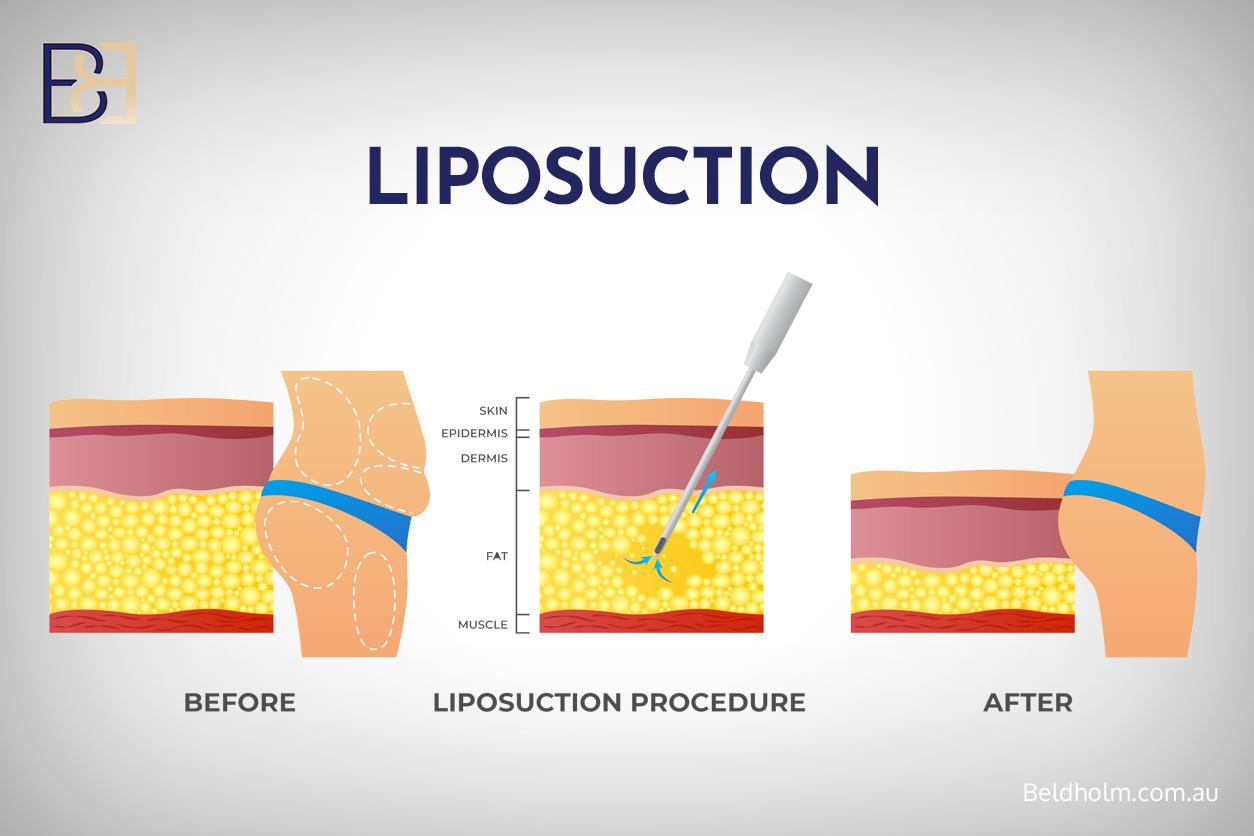
VASER liposuction (ultrasonic suction assisted lipectomy) may be combined with any of the three reduction techniques above, performed at the same operation.
The aim is to address the lateral breast fold and the axillary tail (the area of breast tissue that extends toward the armpit). These adjacent areas of fullness are not always treated by reduction alone, and addressing them at the same operation can affect the overall contour across the chest wall.
Whether VASER liposuction (ultrasonic suction assisted lipectomy) is appropriate is determined at consultation.
Putting it together
The table below summarises the three reduction techniques. The right combination of pattern, pedicle, and adjunct is determined at consultation, after physical examination and clinical photography.
| Technique | Best for | Best for |
|---|---|---|
| Vertical pattern | Small to moderate reductions, good skin elasticity | Around areola plus vertical line |
| Wise pattern | Moderate to larger reductions, or significant skin laxity | Around areola, vertical, and along breast crease (anchor) |
| Free nipple graft | Rarely indicated; very large reductions or specific medical circumstances | Wise pattern scar |
A Patient Guide for Those Still Deciding
For women who are still working through whether reduction mammoplasty (breast reduction) is the right step, a written patient guide can help.
The guide below covers the symptoms commonly associated with heavy breasts, a self-assessment to help think through your own situation, when surgery is generally considered, an overview of the main surgical techniques, and what to bring to your GP referral conversation.
About Dr Bernard Beldholm

I am a Specialist General Surgeon based at Maitland Private Hospital in the Hunter Valley, NSW.
For more than 15 years my practice has focused on body contouring and breast surgery, including reduction mammoplasty (breast reduction), abdominoplasty, brachioplasty, and related procedures. I trained in general surgery and completed Fellowship of the Royal Australasian College of Surgeons (FRACS).
How I work
The principles outlined earlier on this page reflect how I approach every reduction mammoplasty patient: matching the technique to the breast pattern, where appropriate addressing breast volume and chest-wall contour in the same operation, and preparing patients carefully in the weeks before surgery.
I see every patient at consultation myself. I perform the operation myself. I review every patient post-operatively until they have settled. Continuity matters in reduction mammoplasty because the operation is technical, the recovery has stages, and the final result takes months to mature.
Hospital and practice

I operate at Maitland Private Hospital, which has 24-hour medical cover and an on-site intensive care unit. My consulting rooms are at 30 Belmore Road, Lorn, a short drive from the hospital.
The Hunter Valley region means many of my patients come from Maitland, Newcastle, the Upper Hunter, the Central Coast, and surrounding areas. Some travel from further afield in NSW where the procedure or technique they are seeking is what they are looking for.
Preparing for Surgery

How well a patient is prepared in the weeks before surgery affects healing, recovery, and risk. This is true for any operation, and reduction mammoplasty (breast reduction) is no exception.
The preparation I recommend is not the same as the more involved nutritional preparation I use for larger post-weight-loss body contouring patients. For most reduction patients the preparation is more focused, and centres on the items below.
Smoking
Smoking significantly affects wound healing and increases the risk of complications, including poor scar formation and tissue loss.
I ask patients to be nicotine-free for at least six weeks before surgery, and at least six weeks after. This includes cigarettes, vaping, and nicotine replacement products. Where smoking has been long-standing, your GP can help with cessation support.
Weight stability

If your weight is currently changing, breast size and shape will change with it. I recommend a period of weight stability before surgery, generally at least six months at your current weight.
For patients whose weight is not currently stable, surgery is better deferred until it is, so the operation can be planned around your settled anatomy.
General fitness
Patients who are physically active before surgery generally tolerate the anaesthetic better, recover faster from the immediate post-operative period, and return to normal activity sooner.
Walking, swimming, and similar low-impact activity in the weeks before surgery is helpful. Heavy upper-body exercise close to surgery is not necessary and may cause discomfort.
Pre-operative bloods and medical assessment
Before surgery I arrange a set of standard pre-operative blood tests through your GP or pathology provider. These confirm that haemoglobin, kidney function, and other relevant markers are within range for surgery.
If you take regular medications, particularly blood thinners, hormonal medications, or anti-inflammatories, we will discuss which need to be paused and for how long.
Anaesthetic consultation
Reduction mammoplasty is performed under general anaesthesia. A separate consultation with the anaesthetist is part of the preparation. This is usually done by phone in the week before surgery, with an in-person review on the morning of admission.
Supportive bra
A supportive surgical bra is worn after the operation. My practice provides guidance on the type to source before surgery, so it is ready when you are discharged from hospital.
A note on post-weight-loss patients
If you have had significant weight loss and are also seeking reduction mammoplasty (breast reduction), the preparation may need to include more than what is outlined above. Where this applies, we discuss it at consultation and adjust the preparation accordingly.
A GP referral is required for all surgical consultations.
The Consultation Process

The consultation process for reduction mammoplasty (breast reduction) is structured around two consultations rather than one. This is my clinical standard. It gives patients time between visits to consider what has been discussed, ask further questions, and make a decision without pressure.
Before the first consultation
A GP referral is required for all surgical consultations. Your GP will provide a referral letter, which I review before we meet.
If you have had relevant imaging (breast ultrasound, mammogram, or other) within the past 12 months, please bring those results. They are not always required for surgical planning, but they are useful context.
The first consultation
The first consultation covers your symptoms, your medical history, your goals for surgery, and a physical examination of the breasts.
The examination is conducted in private and is necessary to assess breast size, skin quality, the position of the nipple-areolar complex, and the pattern of any asymmetry.
Standardised clinical photographs are taken at this visit. Photographs are essential for surgical planning and form part of your medical record. They are stored confidentially and are not used for any other purpose without your written permission.
I then explain the surgical options that are appropriate for your pattern, including the relevant scar pattern, what is being addressed at the operation, and the realistic outcomes and limitations. We also discuss the risks specific to your situation.
You will leave the first consultation with the information needed to consider whether to proceed.
Between consultations
There is generally a gap of two to four weeks between the first and second consultation. This gap is intentional. It allows time to think through what has been discussed, raise the discussion with family or your GP, and decide whether to proceed.
The second consultation
If you decide to proceed, the second consultation covers the surgical plan in detail, the written quote, the date of surgery, and the practical steps in the lead-up.
By the end of the second consultation, the surgical plan is finalised, the consent process is complete, and the date is in the diary.
Telehealth
At least one of the two consultations must be in person, so the physical examination and clinical photography can be carried out properly. Where it is clinically appropriate, the second consultation may be conducted by telehealth, particularly for patients travelling from outside the Hunter region.
Booking a consultation
Consultations can be booked online through the practice website, or by telephoning the rooms. The receptionist will ask for your GP referral details and arrange a time that suits.
Book your appointment online now
Hospital Stay and Recovery
Reduction mammoplasty (breast reduction) is performed at Maitland Private Hospital. The hospital has 24-hour medical cover and an on-site intensive care unit.
On the day of surgery
You will be admitted to hospital on the morning of surgery. The anaesthetist will see you on the ward and answer any final questions before the operation.
The operation itself takes several hours, depending on the technique and the volume of reduction.
After surgery, you are transferred to the recovery unit, then to your room. Pain relief is provided through the first 24 hours and adjusted to keep you comfortable.
Length of stay
For most patients I prefer an overnight stay. This allows pain relief, drains if used, and any immediate post-operative concerns to be managed in hospital, and lets me see you the morning after.
For some patients reduction mammoplasty (breast reduction) can be performed as a day procedure, where it is clinically appropriate and where there is suitable support at home. The decision is made at the second consultation.
The first two weeks

Most patients are reviewed in the first week, then again at around the two-week mark. These reviews check the wounds, assess healing, and adjust dressings as needed.
Pain in the first few days is managed with prescribed analgesia. By the end of the first week most patients are comfortable on over-the-counter pain relief.
The supportive surgical bra is worn full time for the first four weeks. After four weeks it can be worn part of the day, generally for several more weeks, until I confirm at follow-up that ongoing support is no longer needed.
Returning to normal activities
Recovery times vary with the size and extent of the operation. The guide below describes what most patients can expect.
- Driving: generally five to seven days, once you are off opioid pain medication and able to perform an emergency stop comfortably.
- Work from home: generally five to seven days for most patients.
- Desk-based work in the office: generally seven to fourteen days.
- Heavy lifting and upper-body exertion: avoided for two to three weeks. Returning to this too soon increases the risk of bleeding and wound complications.
- Exercise: light walking from the first week. Heavier exercise, including running and upper-body strength work, gradually re-introduced from around the three-week mark.
These are general timelines. Your own recovery is influenced by the technique used, the volume of reduction, your overall health, and how your body responds to surgery.
Longer-term recovery
Initial swelling settles over the first six to twelve weeks. The breasts continue to settle into their final shape over several months. Scar maturation takes twelve to eighteen months, during which time scars typically fade.
I see patients again at three months, six months, and twelve months after surgery, with longer-term follow-up as needed.
Risks of Reduction Mammoplasty

All surgery carries risks. Reduction mammoplasty (breast reduction) is a major operation, and the risks below are drawn from standard surgical practice and from the published literature on reduction mammoplasty outcomes. The risks specific to an individual patient depend on their anatomy, their medical history, the technique used, and the volume of reduction. These are discussed in detail at consultation.
The list below is not exhaustive. It is intended to give patients a realistic picture of what reduction mammoplasty involves, and what can go wrong.
General surgical and anaesthetic risks
These risks apply to most major operations performed under general anaesthesia.
- Anaesthetic complications. Reactions to anaesthetic agents are uncommon but possible. The anaesthetist will discuss specific risks based on individual medical history.
- Bleeding. Significant bleeding during or after surgery may require return to theatre.
- Haematoma. A collection of blood under the skin, which may require drainage.
- Seroma. A collection of fluid under the skin, which may resolve on its own or require drainage.
- Infection. Wound infection or, less commonly, deeper infection. Infection may require antibiotics, dressings, or further surgery.
- Deep vein thrombosis and pulmonary embolism. A clot forming in the leg veins (DVT) which can travel to the lungs (PE). Steps are taken before, during, and after surgery to reduce this risk, including compression stockings and early mobilisation.
- Wound healing problems. Slow healing, delayed wound closure, or wound separation, particularly at the junction of incisions in Wise pattern reductions.
- Need for revision surgery. A second operation may be needed to address asymmetry, scar issues, or other concerns. Revision is not common but is not rare.
Risks specific to reduction mammoplasty
These risks are particular to reduction surgery.
Scarring
Scars from reduction mammoplasty are permanent. The position depends on the technique used (vertical, Wise, or free nipple graft).
Scars typically fade and flatten over twelve to eighteen months, but the final appearance varies between patients. Some patients form thicker scars (hypertrophic scars) or, less commonly, keloid scars. Skin type, ethnicity, and individual healing all influence scar quality.
Asymmetry
The breasts are never perfectly symmetrical before surgery, and they will not be perfectly symmetrical after. Reduction mammoplasty aims for improved symmetry, not identical breasts. In some cases, residual asymmetry is significant enough that a revision is considered.
Changes to nipple sensation
Sensation in the nipple-areolar complex may be reduced, altered, or lost. This may be temporary, but in some patients it is permanent. Pedicle techniques aim to preserve nerve supply to the nipple, but this cannot be guaranteed.
Effects on breastfeeding
Reduction mammoplasty may affect the ability to breastfeed. Some patients breastfeed successfully after reduction; others cannot. The likelihood of preserved breastfeeding ability depends on the technique used, the volume of reduction, and individual anatomy.
In free nipple graft reduction, the loss of breastfeeding ability is expected, because the duct connections between the nipple and the underlying breast tissue are divided.
Patients who plan future pregnancies are advised to consider this carefully when discussing whether to proceed.
Fat necrosis
Areas of fat tissue may not survive the operation and can form firm lumps within the breast. Fat necrosis is more common in larger reductions. The lumps usually settle over time, but in some cases require imaging investigation or further surgery.
Pigmentation changes
The skin around the scars or the areola may change colour, becoming lighter or darker than the surrounding skin. This is more common in patients with darker skin types.
Loss of the nipple-areolar complex
In a small number of cases the blood supply to the nipple-areolar complex is compromised during surgery, and the nipple does not survive. This is uncommon but not zero. The risk is higher in larger reductions, in patients who smoke, and in patients with poor circulation. Free nipple graft is sometimes recommended in advance precisely because the standard pedicle approach would carry a high risk of this.
Persistent post-operative pain
A small number of patients experience pain in the breast or chest wall that continues beyond the expected recovery period. This is uncommon.
Risks particular to free nipple graft reduction
In addition to the risks above, free nipple graft reduction carries the following:
- Loss of nipple erectile function. The nipple is unlikely to respond to temperature or touch in the way it did before surgery.
- Loss of breastfeeding ability. As noted above, this is expected with this technique.
- Loss of nipple sensation. Because the nipple-areolar complex is removed and replaced as a graft, the nerve supply is divided. Sensation in the nipple is not preserved with this technique.
- Graft failure. Free nipple graft has a high rate of failure. This is one of the principal reasons it is not the technique of choice for most patients. If the graft fails, further surgery is required, and the appearance of the nipple-areolar complex is significantly affected.
Risks particular to liposuction (suction assisted lipectomy) used in breast surgery
Where VASER liposuction (ultrasonic suction assisted lipectomy) is used as an adjunct to surgical reduction, or where liposuction (suction assisted lipectomy) is used as a standalone approach, the following additional risks apply.
- Contour irregularity. Areas of the chest wall may heal with visible irregularity, dimpling, or asymmetry.
- Skin laxity. Removing fat without skin excision may leave skin loose, particularly where elasticity is reduced.
- Burns. Ultrasonic energy used in VASER carries a low risk of thermal injury to overlying skin or surrounding tissue.
- Persistent ptosis. Where liposuction (suction assisted lipectomy) is used without surgical repositioning of the nipple-areolar complex, ptosis may develop or persist after the operation.
At consultation
The risks above apply broadly to reduction mammoplasty (breast reduction). The risks specific to an individual patient depend on anatomy, medical history, the technique used, and the volume of reduction. These are discussed in detail at consultation, alongside the surgical plan and consent process.
Frequently Asked Questions
Is reduction mammoplasty (breast reduction) covered by Medicare or private health insurance?

Reduction mammoplasty performed for medical reasons may meet Medicare criteria, depending on whether specific clinical conditions are met. Private health insurance may also apply where medical criteria are satisfied. Eligibility is assessed individually at consultation, and a written quote covering surgeon fees, anaesthetist fees, hospital costs, and any out-of-pocket gap is provided at the second consultation. Cosmetic-only reduction (where there is no medical indication) is not covered by Medicare.
A GP referral is required for the consultation, regardless of how the procedure will be funded.
Will reduction mammoplasty affect my ability to breastfeed?

It may. Some patients breastfeed successfully after reduction; others cannot. The likelihood of preserved breastfeeding ability depends on the technique used, the volume of reduction, and individual anatomy.
Pedicle techniques aim to preserve some of the duct connections between the nipple and the underlying breast tissue, but this cannot be guaranteed. In free nipple graft reduction, the loss of breastfeeding ability is expected, because the duct connections are divided.
Patients who are planning future pregnancies are advised to consider this carefully before deciding whether to proceed.
How visible will the scars be?
Scars from reduction mammoplasty are permanent. Their position depends on the technique used.
In a vertical pattern reduction, the scar runs around the areola and vertically down to the breast crease. In a Wise pattern reduction, the scar adds a horizontal line along the breast crease. In a free nipple graft reduction, the scar follows the Wise pattern, with an additional graft outline around the repositioned nipple-areolar complex.
Scars typically fade and flatten over twelve to eighteen months, but the final appearance varies between patients. Skin type, ethnicity, and individual healing all influence scar quality. Some patients form thicker (hypertrophic) or, less commonly, keloid scars. Risk factors specific to scar quality are reviewed at consultation.
What does recovery typically look like?
Most patients stay in hospital overnight. Pain in the first few days is managed with prescribed analgesia, and most patients are comfortable on over-the-counter pain relief by the end of the first week.
A supportive surgical bra is worn full time for the first four weeks, and part of the day for several more weeks after that.
Driving is generally resumed at five to seven days, working from home at five to seven days, and desk-based work in the office at seven to fourteen days. Heavy lifting and upper-body exertion are avoided for two to three weeks. Light walking can begin in the first week, with heavier exercise gradually re-introduced from around the three-week mark.
Recovery times vary with the size and extent of the operation, the technique used, and individual healing.
When will I see the final result?
Initial swelling settles over the first six to twelve weeks. The breasts continue to settle into their final shape over several months. Scar maturation takes twelve to eighteen months, during which time scars typically fade.
Patients are reviewed at three months, six months, and twelve months after surgery, with longer-term follow-up as needed.
Is there a minimum or maximum age for reduction mammoplasty?
There is no fixed age cut-off for reduction mammoplasty. Surgery is generally considered after breast development has completed, which is typically in the late teens or early twenties. For older patients, suitability depends on overall health rather than age alone.
A GP referral and a consultation are required to determine whether reduction mammoplasty is appropriate for an individual patient.
Booking a Consultation
For women with symptoms of breast hypertrophy who are considering reduction mammoplasty (breast reduction), the next step is a consultation. The consultation establishes whether surgery is appropriate, what technique fits the breast pattern, and how the procedure would be planned.
A GP referral is required. Consultations can be booked online or by telephoning the practice on (02) 4934 5700.
The practice is based in Maitland, in the Hunter Valley, NSW. Patients travel from Maitland, Newcastle, the Upper Hunter, the Central Coast, and surrounding areas. Reduction mammoplasty is performed at Maitland Private Hospital.
GP referral required. Consultation required to determine suitability. Results vary. All surgery carries risks.

